Clear Sky Science · en
Myeloid HDAC3 deletion protects against traumatic optic injury
Protecting Sight After Head and Eye Injuries
Blunt blows to the head or face can do more than leave a bruise—they can quietly damage the optic nerve that carries visual information from the eye to the brain. This condition, called traumatic optic neuropathy, often leads to permanent vision loss and currently has no reliable treatment. The study summarized here explores a new strategy: reprogramming certain immune cells so they clear away damage more efficiently and help the optic nerve repair itself, potentially preserving sight after injury.
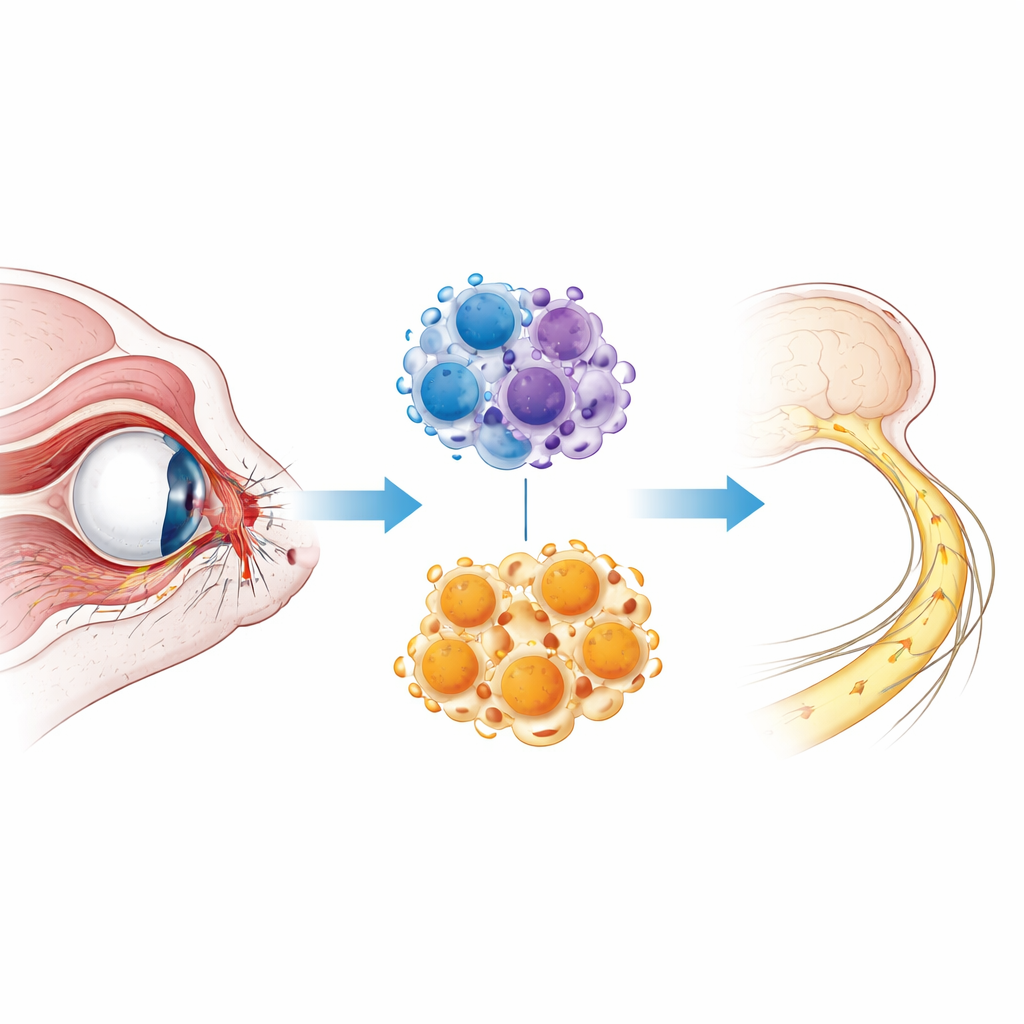
When the Eye’s Wiring Is Hurt
The optic nerve is a tight cable of fibers from retinal ganglion cells, the output neurons of the eye. When this cable is crushed or stretched during trauma, many of these nerve fibers die immediately, while others degenerate slowly over days to weeks. Swelling, inflammation, and a buildup of cellular and myelin debris worsen the injury and make it harder for surviving nerve fibers to regrow. Existing care focuses on stabilizing the patient, because we still lack ways to stop this wave of degeneration. To study these events in detail, scientists often use a mouse model in which the optic nerve is briefly pinched, mimicking the core features of traumatic optic neuropathy.
The Surprising Power of Cleanup Cells
After injury, specialized immune cells called microglia and macrophages rush to the damaged nerve and retina. These “cleanup crews,” collectively known as myeloid cells, can be double-edged swords: they can fuel inflammation, but they can also perform efferocytosis—engulfing and digesting dead cells and debris so that tissue can heal. The researchers focused on a molecular switch inside these cells, an enzyme called HDAC3 that helps control which genes are turned on or off. Previous work showed that blocking HDAC3 directly in nerve cells could reduce cell death. Here, the team asked a different question: what happens if HDAC3 is removed specifically from myeloid cells instead?
Switching Myeloid Cells Into Repair Mode
Using genetically engineered mice, the scientists deleted HDAC3 only in myeloid cells while leaving it intact elsewhere. After optic nerve crush, these mice retained more retinal neurons and showed stronger electrical signals from the retina compared with normal mice, indicating better visual function. They also had more regenerating nerve fibers growing past the injury site. Microscopy revealed that myeloid cells lacking HDAC3 were more active at engulfing dying cells in the retina and clearing myelin debris from the optic nerve. When myelin fragments were offered to macrophages in a dish, cells without HDAC3 swallowed far more of this material, confirming that the enzyme normally restrains their cleanup ability.
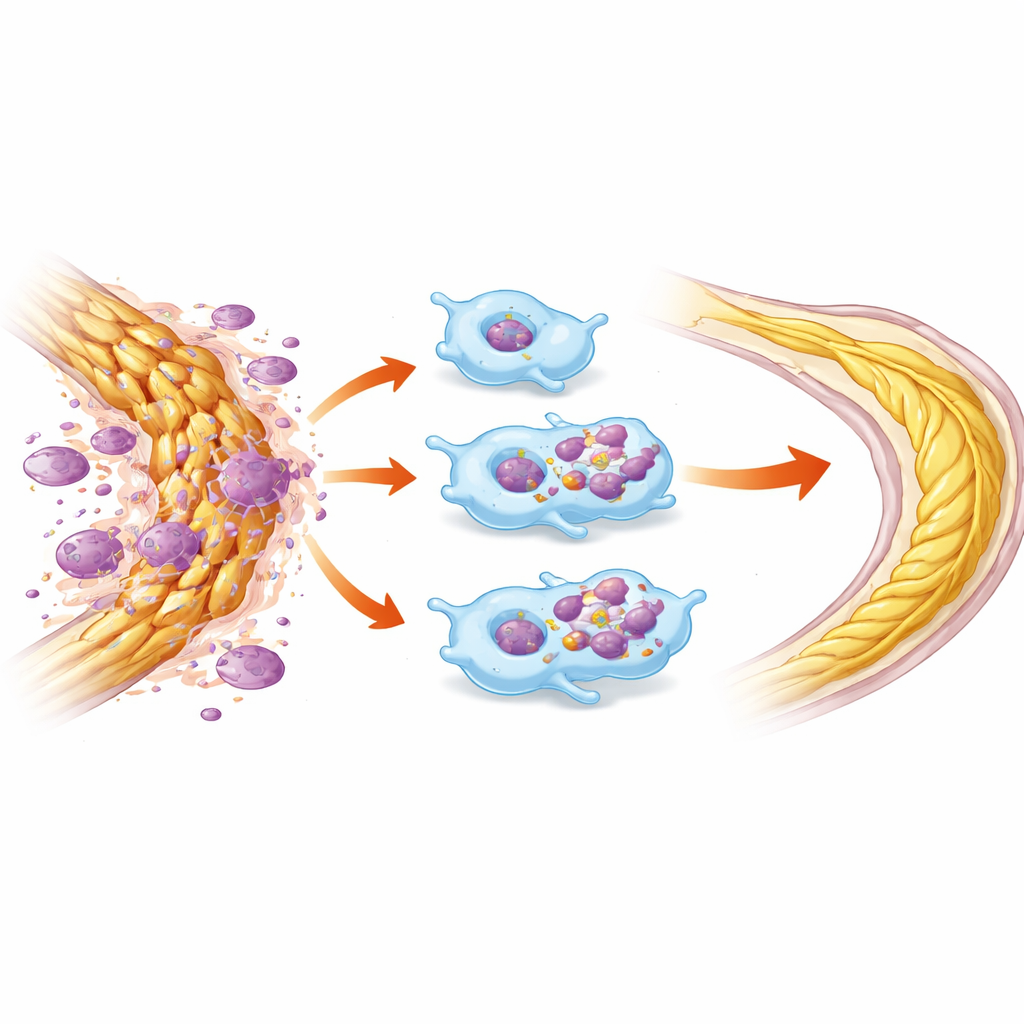
A Key Receptor Helps Drive Debris Clearance
To understand how HDAC3 controls this behavior, the researchers examined molecules involved in efferocytosis. They found that HDAC3-deficient macrophages boosted production of MerTK, a surface receptor known to recognize and ingest dead cells and myelin, along with related factors that promote resolution of inflammation. Blocking MerTK with a small-molecule inhibitor largely erased the advantage in myelin uptake, suggesting that HDAC3 deletion helps by freeing MerTK and its partners to work more strongly. Interestingly, when HDAC3 was removed only from long-lived microglia but not from infiltrating macrophages, the protective effect on retinal cells and function disappeared, pointing to macrophages as the main drivers of this repair program in this injury model.
What This Could Mean for Future Treatments
In simple terms, this work shows that dialing down HDAC3 in certain immune cells turns them into more efficient janitors: they clear away dead cells and nerve insulation faster, calm inflammation, and create a friendlier environment for damaged optic nerve fibers to regrow. Although more research is needed to understand exactly how HDAC3 controls MerTK and to design safe drugs that act selectively on myeloid cells, the concept is clear. By teaching the body’s own cleanup crews to do a better job, we may one day protect vision and promote nerve repair after devastating eye and head injuries.
Citation: Shahror, R.A., Morris, C.A., Cunningham, A. et al. Myeloid HDAC3 deletion protects against traumatic optic injury. Cell Death Discov. 12, 163 (2026). https://doi.org/10.1038/s41420-026-03030-0
Keywords: traumatic optic neuropathy, optic nerve injury, macrophages, HDAC3, efferocytosis