Clear Sky Science · en
Disruption of metabolic licensing by JAK inhibitors constrains CD8 T cell activation and effector function
Why these immune cells matter to everyday health
Drugs that calm an overactive immune system have transformed life for people with rheumatoid arthritis and other autoimmune diseases. But many of these medicines, called JAK inhibitors, also make some patients more likely to get infections such as shingles or tuberculosis. This study asks a simple but important question: what exactly do these drugs do to our infection-fighting T cells, especially the CD8 T cells that hunt down virus‑infected cells?
Medicines that switch signals off
JAK inhibitors block a family of enzymes that carry signals from immune‑system messenger molecules inside cells. Different drugs in this class target different JAK enzymes, but all aim to dial down inflammation. The authors studied three widely used JAK inhibitors, plus one drug that blocks a related enzyme, using blood cells from healthy volunteers. They focused on naive CD8 T cells, which have not yet seen infection, and memory CD8 T cells, which normally respond quickly to microbes they have encountered before. When these cells were stimulated in the lab to mimic an infection, the team added clinically realistic doses of the drugs and measured how well the cells became activated, multiplied, and armed themselves to kill.
Cells that look awake but lack energy
At first glance, drug‑treated CD8 T cells still showed some signs of waking up: they turned on common activation flags on their surface. But under the hood, they behaved very differently. Normally, an activated T cell rapidly imports sugar from its surroundings and burns it through a high‑gear form of metabolism to fuel division and the production of toxic proteins and alarm‑raising cytokines. With JAK inhibitors present, glucose uptake dropped, the main glucose transporter on the cell surface was reduced, and less lactate—an end‑product of fast sugar burning—built up in the culture dishes. Even among the cells that had clearly switched on activation markers, this “metabolic shift” failed to occur properly. The same pattern appeared in CD4 T cells, suggesting a broader effect across T‑cell types.
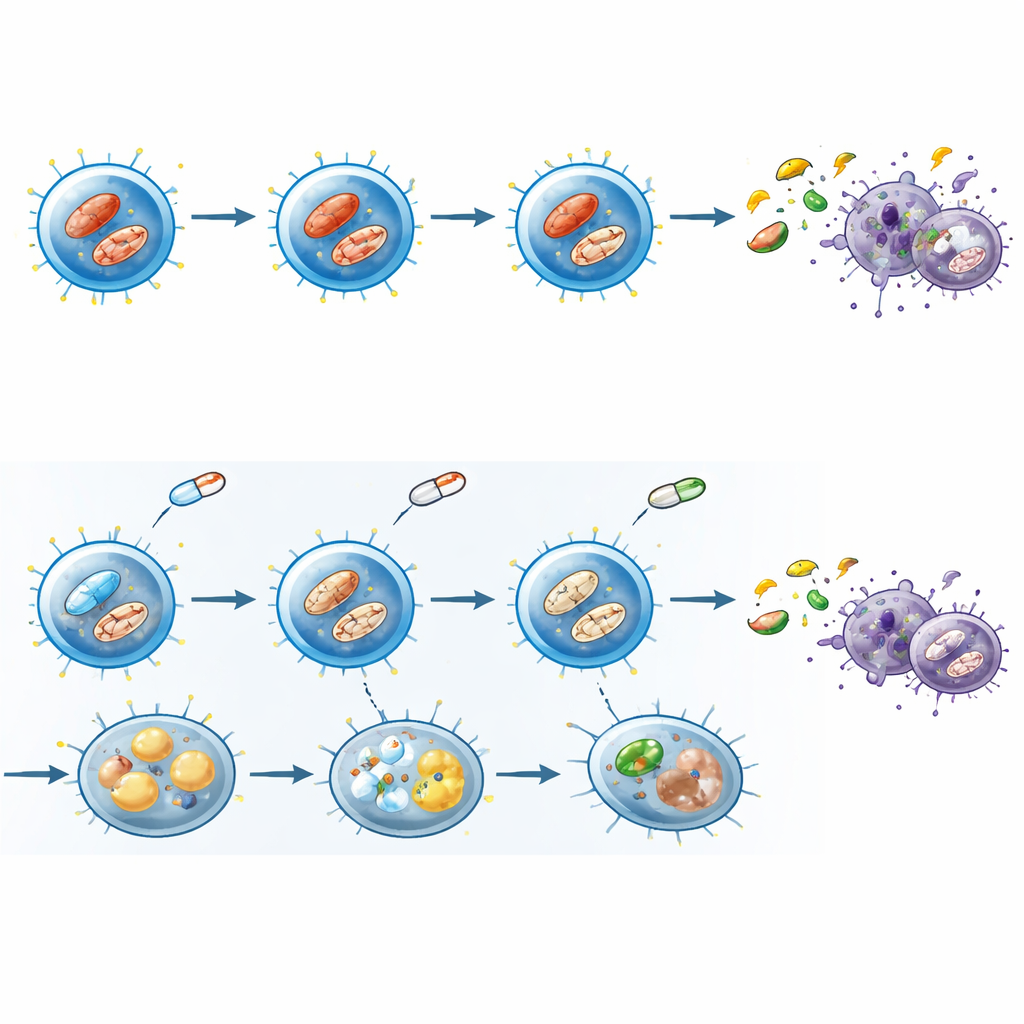
Strained power plants and stored fat
The team then examined the cells’ internal power plants, the mitochondria. Healthy, activated T cells usually show many tightly structured, highly charged mitochondria that help supply energy and important chemical signals. Under JAK inhibition, fewer CD8 T cells had strongly polarized mitochondria, the mitochondrial membrane charge was lower, and detailed electron microscopy revealed swollen, damaged structures with disrupted internal folds. At the same time, the cells accumulated fat droplets, hinting that they were storing rather than efficiently burning lipids. Measurements of mitochondrial‑derived reactive oxygen species also shifted in a way that depended on whether cells were activated, pointing to a disturbed balance of helpful and harmful mitochondrial signals.
Stress programs that curb growth and effort
To understand how these changes are wired at the genetic level, the researchers sequenced RNA from activated memory CD8 T cells exposed to a representative JAK inhibitor. Gene activity linked to fast sugar use and amino‑acid metabolism was dialed down, while programs associated with mitochondrial respiration and cellular starvation were dialed up. At the same time, genes driven by mTOR and MYC—master controllers of growth and biosynthesis—were suppressed, and genes governed by the stress‑response protein p53 were increased. Functional tests confirmed that global protein production slowed and that cells shifted away from relying on glucose toward depending more on mitochondria, despite their compromised state. Altogether, these changes resembled a senescence‑like state: cells not dead, but metabolically stressed, sluggish, and less able to carry out their duties.
Evidence from patients in the clinic
Laboratory results can be misleading if they do not hold up in real people, so the investigators examined blood from patients with rheumatoid arthritis taking JAK inhibitors and compared them with patients on methotrexate, a different immune‑modulating drug, and with healthy volunteers. After mild stimulation, memory CD8 T cells from JAK inhibitor–treated patients were less likely to reach a fully activated state, showed lower activity of the mTOR pathway, and expressed less of the glucose transporter linked to high metabolic demand. Using a single‑cell metabolic assay, these patient cells displayed reduced protein synthesis, decreased dependence on glucose, and increased reliance on mitochondrial pathways, closely mirroring the patterns seen in the laboratory experiments.
What this means for infection risk
For a layperson, the core message is that JAK inhibitors do more than dim inflammatory signals: they also cut the energy supply and growth capacity of key killer T cells. The drugs allow these cells to put on the outward “uniform” of activation, but block the metabolic licensing that lets them run, divide, and destroy infected targets effectively. This constrained, stress‑biased state helps explain why people taking JAK inhibitors can be more vulnerable to certain infections, and suggests that monitoring or supporting T‑cell metabolism might one day help tailor treatment and reduce those risks.
Citation: Onofrio, L.I., Abrate, C., Strusberg, I. et al. Disruption of metabolic licensing by JAK inhibitors constrains CD8 T cell activation and effector function. Cell Death Dis 17, 355 (2026). https://doi.org/10.1038/s41419-026-08610-7
Keywords: JAK inhibitors, CD8 T cells, immune metabolism, autoimmune therapy, infection risk