Clear Sky Science · en
STRATEGIC-1: multiple-line, randomized, open-label GERCOR-PRODIGE-39 phase III trial in unresectable RAS/BRAF wild-type metastatic colorectal cancer
Why treatment order matters
For people living with advanced colorectal (bowel) cancer that has spread and cannot be removed by surgery, medicine has come a long way: doctors now have several powerful drug combinations to slow the disease. But one big question remains largely unanswered: does the order in which these drugs are given really matter for how long the cancer stays under control and how long patients live? The STRATEGIC‑1 trial set out to test, in a rigorous way, whether starting with one modern drug combination versus another would lead to clearly better long‑term results.
Two different game plans
In this large international study, researchers focused on a group of patients whose tumors lacked certain common gene changes (in the RAS and BRAF genes). These patients are known to benefit from a class of drugs that block a surface signal on cancer cells (EGFR), as well as from drugs that starve tumors of new blood vessels (anti‑angiogenic therapy). The trial compared two full treatment “game plans,” not just single drugs. One plan (Arm A) started with a chemotherapy backbone called FOLFIRI combined with an EGFR‑blocking antibody, then switched to a different chemotherapy (FOLFOX) paired with a blood‑vessel blocker (bevacizumab). The other plan (Arm B) began with oxaliplatin‑based chemotherapy and bevacizumab, then moved to irinotecan‑based chemotherapy still combined with bevacizumab, and kept EGFR‑blocking therapy in reserve for later. 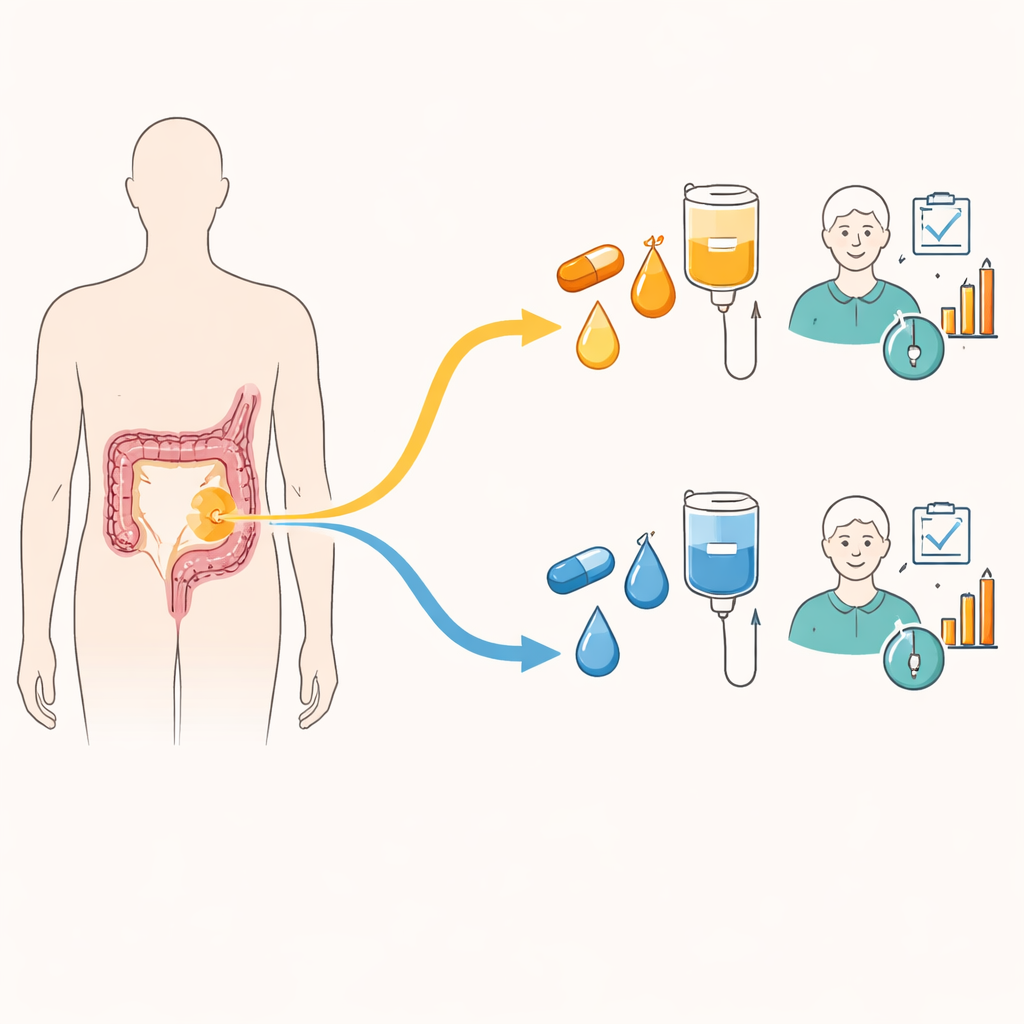
Measuring control over time
Instead of looking only at the first treatment phase, the team used a broader yardstick called “duration of disease control.” This summed up, over several treatment lines, how long each patient’s cancer stayed in check before it clearly worsened. They also tracked overall survival (how long patients lived), how many tumors shrank, whether patients could undergo surgery to remove spots of cancer, side effects, and quality of life. More than 260 people with untreated, inoperable metastatic colorectal cancer entered the study and received one of the two strategies, then were followed for more than five years on average.
Similar long‑term outcomes
The headline result was that the overall time the cancer stayed controlled was almost identical between the two plans—about 23 months in each group. Overall survival was also broadly comparable: around 40 months for those who started with the EGFR‑based plan and about 34 months for those who began with bevacizumab, a difference that did not clearly meet the study’s bar for statistical certainty. Side effects in both groups matched what doctors already know about these drugs, and serious treatment‑related problems occurred at similar rates. Importantly, delaying the start of either targeted drug type (EGFR blocker in one arm, bevacizumab in the other) did not meaningfully change how long patients lived or how long their disease was held in check.
Early responses and tumor location
Where the two strategies did differ was in how often tumors shrank with first‑line treatment. When patients began with the EGFR‑blocking regimen, more than eight out of ten had measurable tumor shrinkage, compared with about two‑thirds in the bevacizumab‑first group. This pattern was even more pronounced in people whose original tumor started on the left side of the colon or rectum, a group already known to respond better to EGFR‑blocking drugs. However, these early differences in shrinkage did not translate into clearly longer disease control or survival across the whole group. When patients moved to second‑ and third‑line treatments, results again looked broadly similar between the two strategies. 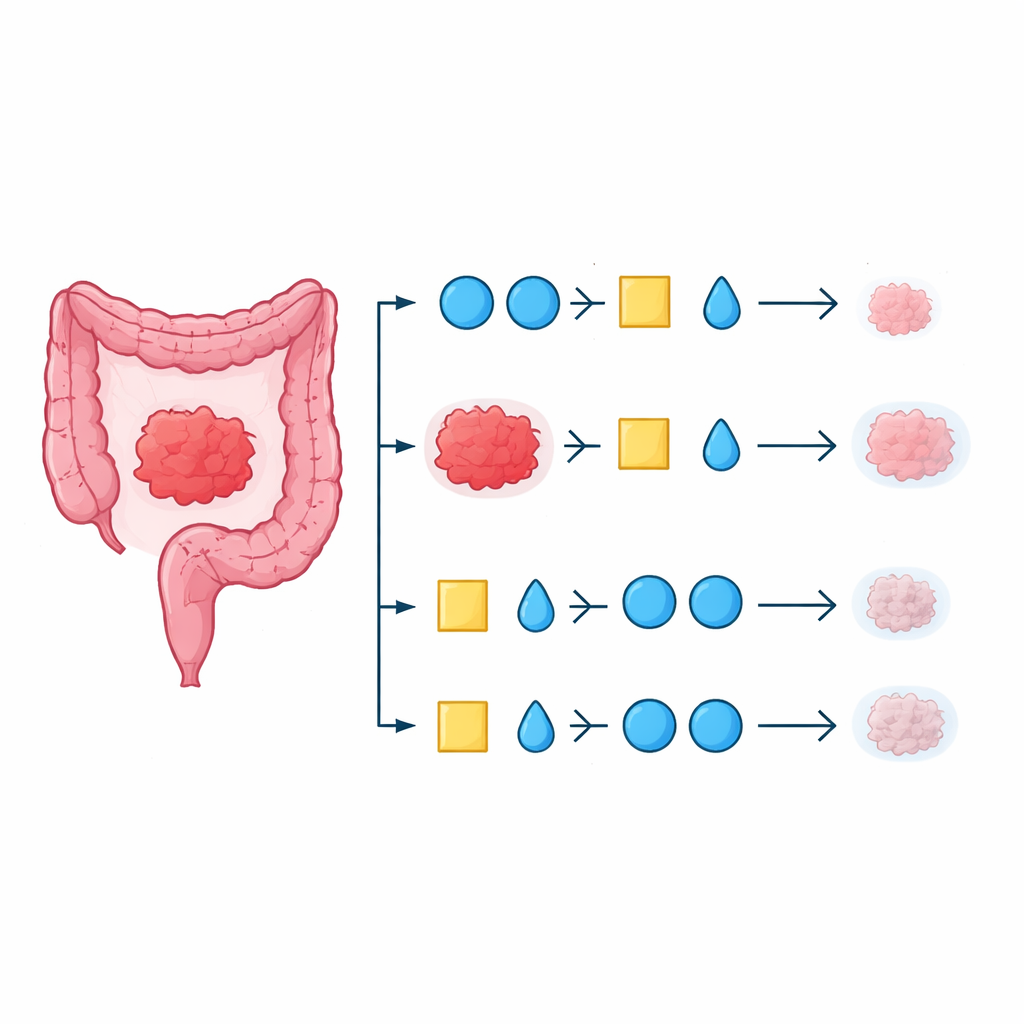
What this means for patients
For patients and clinicians, STRATEGIC‑1 brings both reassurance and nuance. It shows that, within modern standards of care, there is no single “magic” sequence of these two major drug families that dramatically changes how long most patients with this type of metastatic colorectal cancer live. Starting with an EGFR‑blocking regimen may give a higher chance of early tumor shrinkage—useful when rapid reduction is needed—but the overall journey, in terms of total time with the disease under control and overall survival, ends up remarkably similar between the compared strategies. The study also highlights that broad measures of long‑term control may not be the best single guide for choosing a treatment order. Instead, decisions will likely continue to be tailored, considering tumor side, molecular details, patients’ goals, and tolerance, while future research looks for more precise ways to match the right sequence to the right person.
Citation: Chibaudel, B., Dourthe, LM., André, T. et al. STRATEGIC-1: multiple-line, randomized, open-label GERCOR-PRODIGE-39 phase III trial in unresectable RAS/BRAF wild-type metastatic colorectal cancer. Sig Transduct Target Ther 11, 133 (2026). https://doi.org/10.1038/s41392-026-02639-y
Keywords: metastatic colorectal cancer, targeted therapy sequencing, EGFR inhibitors, bevacizumab, treatment strategy trials