Clear Sky Science · en
Proline/serine-rich coiled-coil 1 alleviates atherosclerosis via remodeling tryptophan metabolism mediated by Akkermansia muciniphila
How Gut Bugs and a Hidden Gene Shape Heart Health
Atherosclerosis—the slow clogging and scarring of our arteries—is usually blamed on high cholesterol and inflammation. This study reveals a surprising new player: a little-studied human gene called PSRC1 that protects arteries by working hand-in-hand with a mucus-loving gut microbe and a molecule made from dietary protein. Together, they form a chain of events stretching from the colon to immune cells inside artery walls, and may open the door to precision treatments for people at high risk of heart disease.
A Gene That Guards the Arteries
The researchers focused on PSRC1, a gene previously flagged in large genetic studies as linked to coronary artery disease. Earlier work in mice suggested that losing PSRC1 worsens atherosclerosis, in part by disturbing the gut microbiome. Here, the team confirmed that mice lacking PSRC1 developed larger, more fragile plaques in their arteries despite being on the same high-fat diet as control mice. Their artery walls showed bigger fatty deposits, larger dead zones inside the plaques and less supportive collagen, all hallmarks of dangerous, rupture-prone lesions that can trigger heart attacks and strokes.
When the Mucus Wall and a Key Microbe Disappear
To see how a gene in the host could affect microbes in the gut, the scientists examined the intestines of PSRC1-deficient mice. They found that the protective mucus layer coating the colon was thinner, with fewer mucus-producing goblet cells and weakened junctions between intestinal cells. This damaged barrier favors the loss of beneficial bacteria. One microbe in particular, Akkermansia muciniphila, which normally thrives by feeding on mucus while helping to maintain it, was strongly depleted. Because Akkermansia has been tied to protection against obesity, inflammation and atherosclerosis, its disappearance offered a plausible link between PSRC1 loss and worsening artery disease. 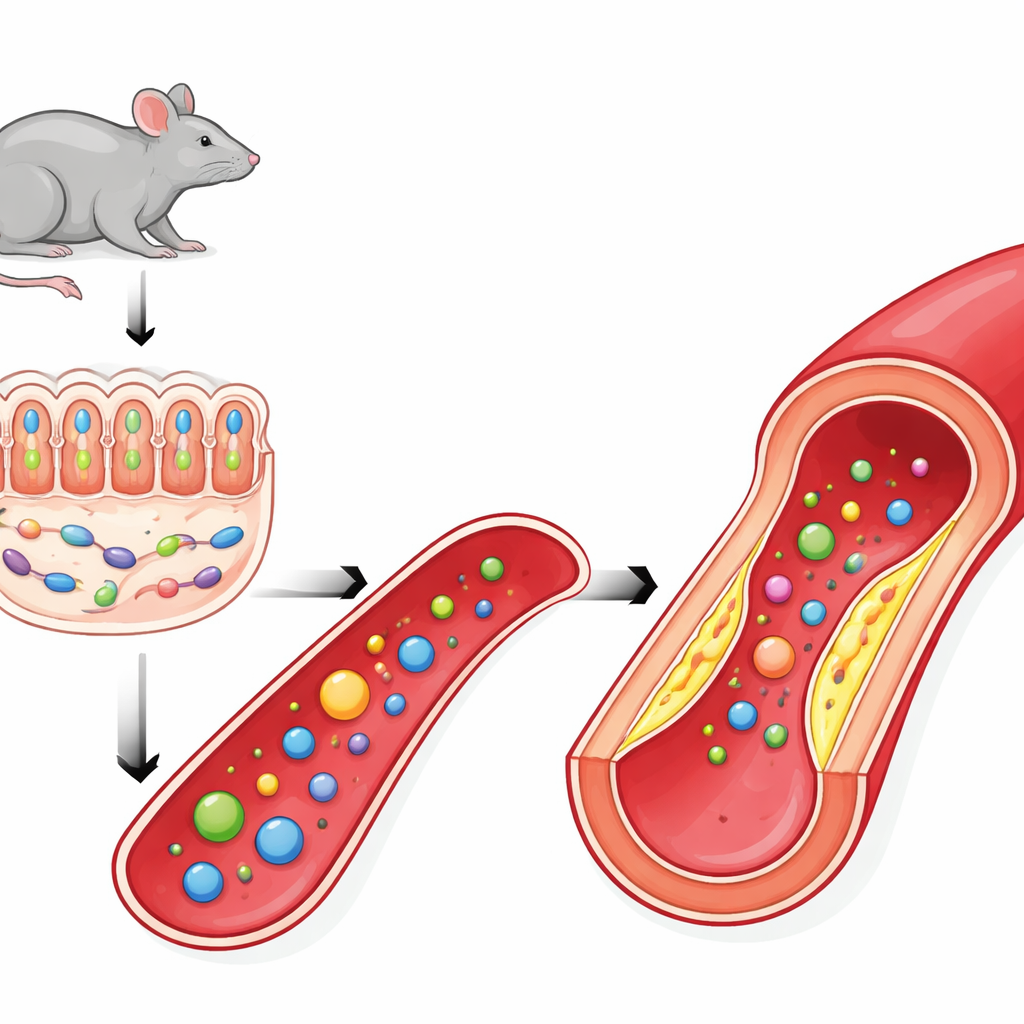
From Dietary Protein to a Protective Signal
The team then zeroed in on tryptophan, an essential amino acid from food that gut bacteria can turn into a variety of chemical messengers. In PSRC1-deficient mice, several tryptophan-derived compounds fell in the blood, especially indole-3-acetic acid (IAA), a product known to dampen inflammation and oxidative stress in experimental models. IAA can activate a sensor inside immune cells called the aryl hydrocarbon receptor (AHR), which in turn controls genes that help keep inflammation and cell death in check. In the mutant mice, AHR activity and its downstream markers were reduced in the liver, colon and, crucially, in plaque-resident macrophages—the immune cells that engulf fats and can either stabilize or destabilize plaques depending on how they behave.
A Microbe–Molecule Lifeline for Immune Cells
To test whether restoring Akkermansia or IAA could rescue the damaged system, the researchers treated PSRC1-deficient mice with live or heat-killed Akkermansia after clearing their native gut flora with antibiotics. Only live bacteria significantly shrank plaque size, improved plaque structure and raised blood IAA levels, while also restoring AHR activity in macrophages. Directly feeding mice IAA likewise reduced plaque burden and made plaques more stable, with fewer dying macrophages and more smooth muscle and collagen. In cell culture, boosting PSRC1 in macrophages increased AHR protein by slowing its breakdown through a de-tagging enzyme called UCHL3, while knocking down PSRC1 made cells more prone to die under stress. Adding IAA reversed this pro-death signal, but only if AHR was active, indicating that the protective effect of IAA runs through this receptor.
Clues from Human Patients
The researchers also looked at blood samples from people undergoing heart evaluation. Compared with individuals without significant coronary blockages, patients with coronary artery disease had lower circulating IAA and lower expression of PSRC1 and an AHR-responsive gene in their blood immune cells. Statistical analysis suggested that higher PSRC1 expression went hand-in-hand with higher IAA and stronger AHR signaling, echoing the mouse findings and supporting the idea of a shared PSRC1–Akkermansia–IAA–AHR axis in humans.
New Paths Toward Tailored Heart Therapies
Taken together, the work sketches a gut-to-artery circuit: PSRC1 helps maintain a healthy mucus barrier and supports Akkermansia, which in turn produces IAA from dietary tryptophan. IAA activates AHR in macrophages, limiting their death and helping keep arterial plaques smaller and more stable. When PSRC1 is lost, this chain weakens—Akkermansia dwindles, IAA drops, AHR signaling fades and macrophages die more readily, expanding the dangerous core of plaques. 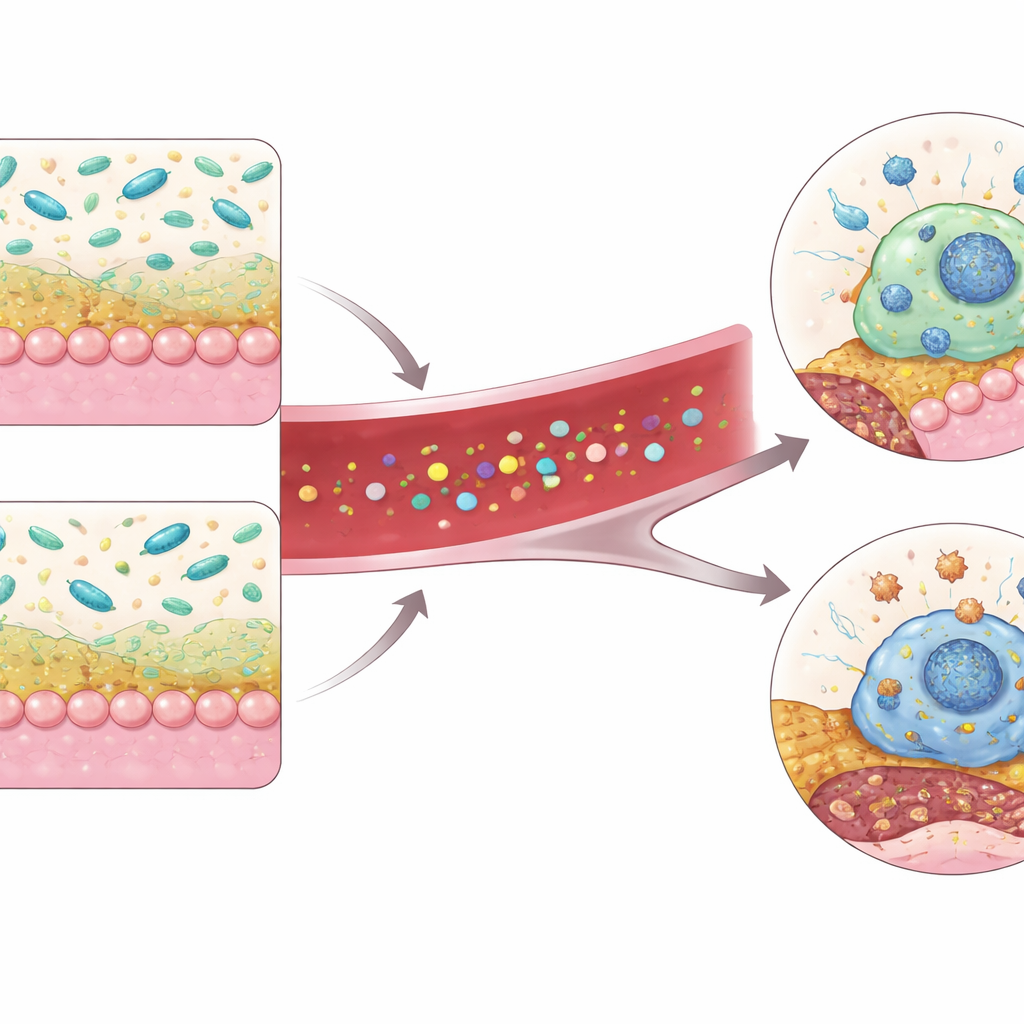
Citation: Wu, Q., Hu, K., Wang, Q. et al. Proline/serine-rich coiled-coil 1 alleviates atherosclerosis via remodeling tryptophan metabolism mediated by Akkermansia muciniphila. Exp Mol Med 58, 848–863 (2026). https://doi.org/10.1038/s12276-026-01668-5
Keywords: atherosclerosis, gut microbiome, tryptophan metabolism, Akkermansia muciniphila, indole-3-acetic acid