Clear Sky Science · en
Spatial optimisation strategies for tertiary hospitals to promote health equity in Tianjin, China
Why Hospital Location Shapes Fair Access to Care
When you or a family member faces a medical emergency, how quickly you can reach a high-level hospital can be a matter of life and death. Yet in many cities, top hospitals are packed into downtown districts, leaving people in outer neighborhoods with longer travel times and fewer choices. This study looks at Tianjin, a major city in northern China, to ask a simple but powerful question: how can we rearrange where the biggest hospitals are, and how large they are, so that everyone has a fair chance to get timely, high-quality care?
Taking a Close Look at One Big City
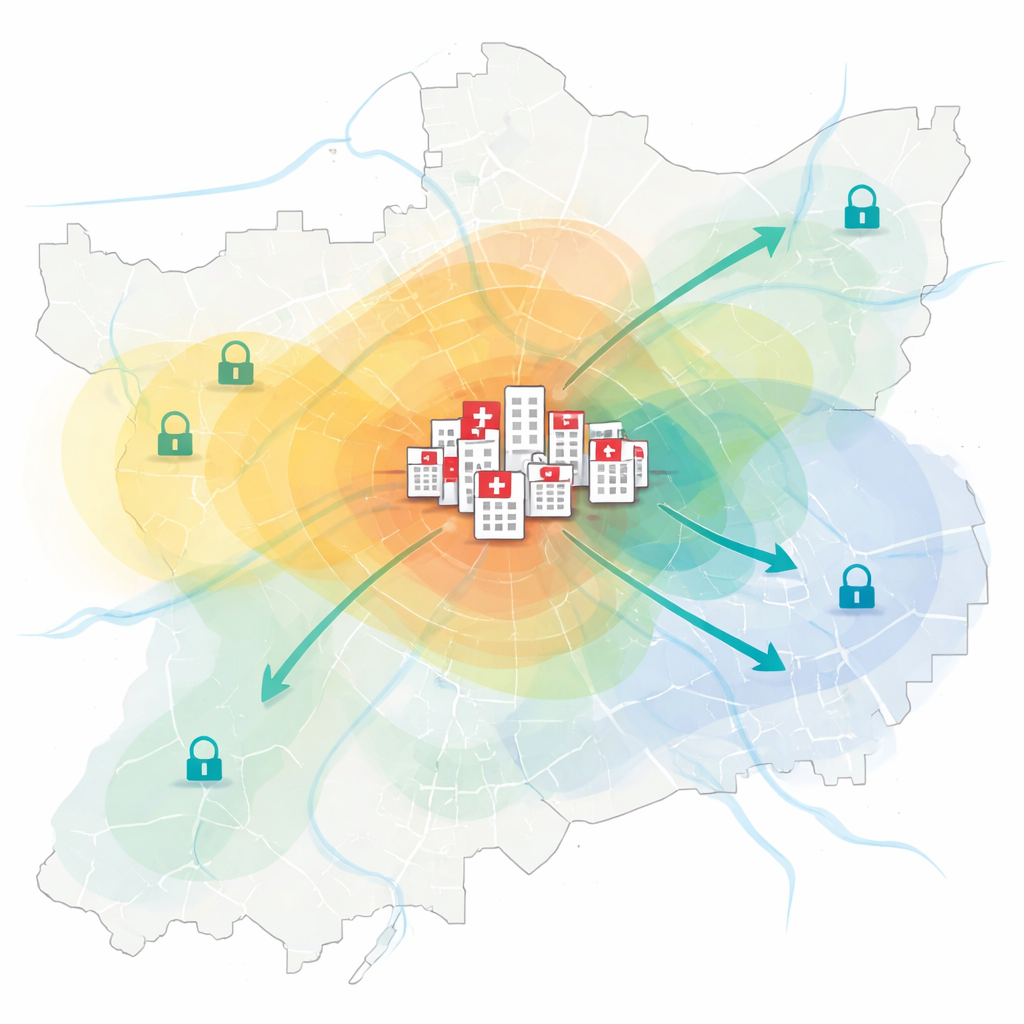
The researchers focus on Tianjin, a rapidly growing city that serves not only its own residents but also patients arriving from surrounding regions. China’s hospital system is tiered, and “tertiary” hospitals sit at the top: they handle complex illnesses, advanced surgery, and serious emergencies. Because these institutions concentrate the best doctors and equipment, their locations strongly influence who gets high-level care, and how fast. The team gathered detailed data on every public tertiary hospital in Tianjin, including where each hospital sits, how many beds it has, how people are distributed across the city, and how roads connect neighborhoods to hospitals.
Mapping People, Hospitals, and Gaps
To understand how well hospitals match people’s needs, the authors built fine-grained maps of population and hospital coverage. Instead of assuming that people are spread evenly within each district, they used “points of interest” for residential buildings and housing areas, combined with land-use data, to estimate where people actually live block by block. They then used digital road networks to simulate how far an ambulance could drive in ten minutes under realistic traffic-speed assumptions. This allowed them to draw service zones around each tertiary hospital and to see which parts of the built-up city area fell outside any hospital’s quick-reach zone.
Unequal Clusters and Strained Hospitals
The maps reveal a clear pattern: tertiary hospitals in Tianjin are heavily clustered in the central urban districts, while the outer districts have few such facilities. Only about 39% of the built-up urban area lies within the ten-minute service range of a tertiary hospital, leaving large “blind spots,” especially between the main city and the coastal Binhai New District. The researchers also compared the number of hospital beds with the number of people living in each hospital’s catchment area. Nearly half of the tertiary hospitals lacked enough beds to meet expected demand, and several were judged severely short. When such hospitals overflow, patients are referred elsewhere. Using network analysis, the team calculated that transfers from outlying districts to better-equipped central hospitals often take 30 to 60 minutes, and the average transfer time citywide is over 21 minutes—far from ideal in emergencies.
A Plan to Spread Capacity and Shorten Trips
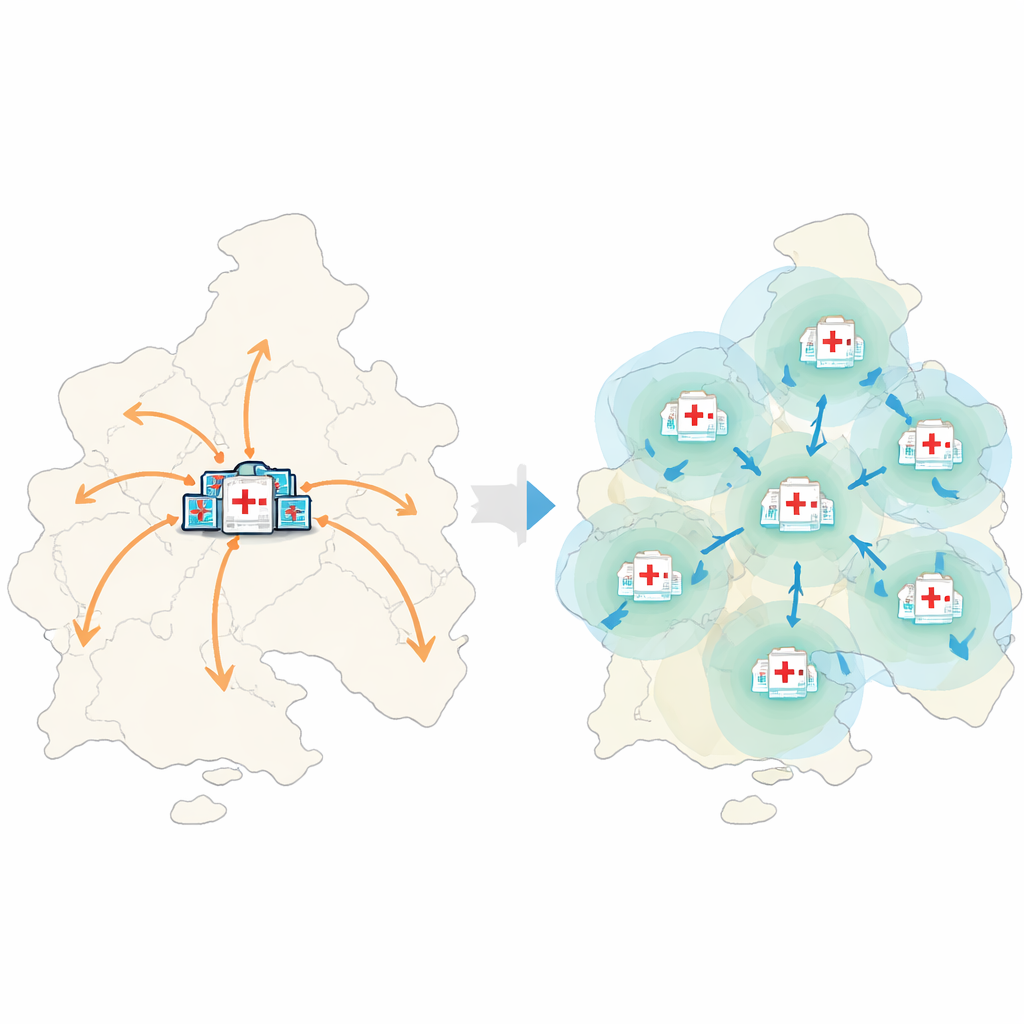
To fix these imbalances, the authors tested a set of planning strategies. First, they identified underserved high-population zones with poor hospital access and proposed building 15 new tertiary hospitals there, each with about 1,000 beds, in three construction phases. Second, they recommended upgrading existing tertiary hospitals that are too small—raising those with fewer than 800 beds up to that level where possible. When they re-ran their models with this optimized layout, the share of the built-up area covered by tertiary hospitals within ten minutes jumped to about 56%. Bed shortages sharply declined, with no hospitals remaining in the most severely strained category. Most strikingly, the average inter-hospital transfer time dropped to under five minutes, suggesting much faster patient routing during surges or disasters.
What This Means for Everyday Patients
For ordinary residents, the study’s message is straightforward: where big hospitals are placed—and how many beds they hold—has a powerful impact on fairness in health care. In Tianjin’s current layout, people living in downtown districts enjoy quick access to advanced care and fast transfers between hospitals, while those in outer districts face longer travel times and fewer options. The authors show that by strategically adding and enlarging hospitals in specific neighborhoods, the city could bring high-level care closer to more people, reduce dangerous delays in emergencies, and move toward a more equitable, resilient health system. Although the work is centered on Tianjin, the approach—combining detailed population maps, road networks, and hospital capacity data—offers a blueprint any growing city can use to plan for healthier, fairer access to care.
Citation: Li, Y., Zhang, R., Feng, Z. et al. Spatial optimisation strategies for tertiary hospitals to promote health equity in Tianjin, China. Humanit Soc Sci Commun 13, 519 (2026). https://doi.org/10.1057/s41599-026-06905-w
Keywords: hospital accessibility, health equity, urban planning, Tianjin, tertiary hospitals