Clear Sky Science · en
The use of electroencephalography in neurodegenerative disease and its utility in dementia
Listening to the brain’s quiet warnings
Dementia often seems to appear out of nowhere, when memory lapses and thinking problems finally become impossible to ignore. This review explains how electroencephalography, or EEG, can pick up subtle changes in brain activity years before daily life is affected. For readers, it offers a glimpse of how a simple cap of sensors on the scalp might one day help doctors spot neurodegenerative disease early, tell different dementias apart, and track whether treatments are working.
A simple test with a deep view into the brain
EEG records tiny electrical signals from the scalp, providing a fast and relatively low cost way to monitor how large groups of brain cells fire together. The authors describe how dementia, including Alzheimer’s, Parkinson’s dementia, dementia with Lewy bodies, frontotemporal dementia, and Huntington’s disease, all disturb the brain’s normal rhythms. These rhythms are often altered before obvious memory or movement problems appear. Modern computing tools and machine learning can now detect patterns in EEG data that human eyes easily miss, turning a long-used test into a powerful probe of early brain change.

Different ways to watch the brain at work and at rest
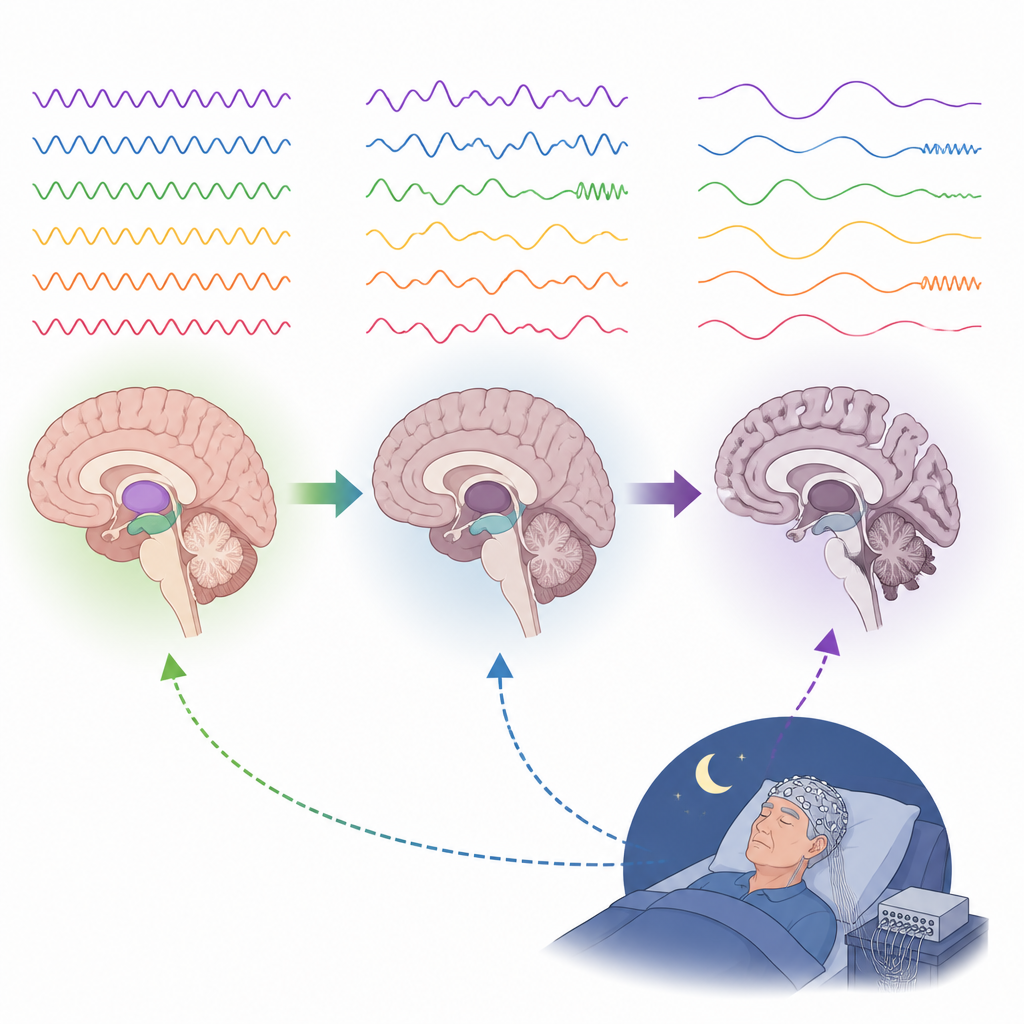
The paper outlines several major ways EEG is used in this field. Routine EEG captures resting brain activity or responses to simple sounds or images, often in sessions lasting under an hour. Event-related responses, such as the P300 wave that appears when the brain detects something important or unexpected, tend to become smaller and slower as dementia progresses. Sleep EEG, usually recorded overnight, reveals how deeply and smoothly a person sleeps. In many dementias, deep slow-wave sleep and short bursts called spindles weaken, and rapid eye movement sleep becomes fragmented or abnormal. In some people with Alzheimer’s and related diseases, brief, silent seizure-like bursts appear mainly during sleep, hinting that nighttime brain overactivity may further harm memory.
What changing brain rhythms say about different dementias
Across many studies, a broad trend emerges: as dementia advances, fast brain waves that support alert thinking fade, while slower waves become stronger and more widespread. Yet each disease also has its own signature. Alzheimer’s and dementia with Lewy bodies often show the greatest slowing over the back of the head, where visual and memory networks sit. Frontotemporal dementia usually shows changes over the front and side regions involved in behavior and language. Huntington’s disease tends to start with changes over the back of the brain and then spread forward as symptoms worsen. By mapping where and how rhythms change, and by measuring how strongly distant brain regions stay in sync, EEG can help distinguish these conditions and predict which people with mild impairment are most likely to decline.
From early warning to guidance for treatment
The authors emphasize that EEG can do more than flag trouble early. By tracking brain rhythms and connectivity over time, it can offer an objective way to see whether a drug, a sleep intervention, or a brain stimulation approach is stabilizing or worsening network function. Studies already show that certain EEG measures can predict who with mild cognitive impairment will later develop Alzheimer’s or Parkinson’s dementia. However, EEG patterns also change with normal aging, and many rhythm changes are shared across diseases, so results must be interpreted with care and ideally combined with other brain imaging and fluid tests.
What this means for the future of dementia care
In plain terms, this review concludes that EEG is poised to become a practical, widely available tool for understanding and tracking the brain changes that lead to dementia. It cannot yet stand alone as a diagnostic test, but its ability to capture early, subtle disruptions in brain networks makes it a strong partner to more expensive scans and lab assays. With larger, standardized studies and smarter analysis methods, EEG-based markers could help doctors spot problems sooner, sort among different dementia types, and follow how the brain responds as new treatments are tried.
Citation: Guo, J., Lisgaras, C.P. The use of electroencephalography in neurodegenerative disease and its utility in dementia. npj Dement. 2, 36 (2026). https://doi.org/10.1038/s44400-026-00089-5
Keywords: electroencephalography, dementia, Alzheimer’s disease, brain rhythms, sleep EEG