Clear Sky Science · en
Electromyography of the stapedius muscle via a retrofacial approach and electrically evoked stapedius reflex during cochlear implant surgery: a prospective bicentric study
Why tuning hearing implants matters
Cochlear implants can give back a sense of sound to people who are profoundly deaf, but getting the tiny electrical pulses “just right” is still a challenge. Today, surgeons and audiologists often rely on patients’ own descriptions of loudness to adjust these devices, which is hard for very young children, tired patients, or anyone who struggles to communicate. This study explores whether a natural reflex deep in the middle ear can be measured directly during surgery to offer a more objective way to fine tune cochlear implants.
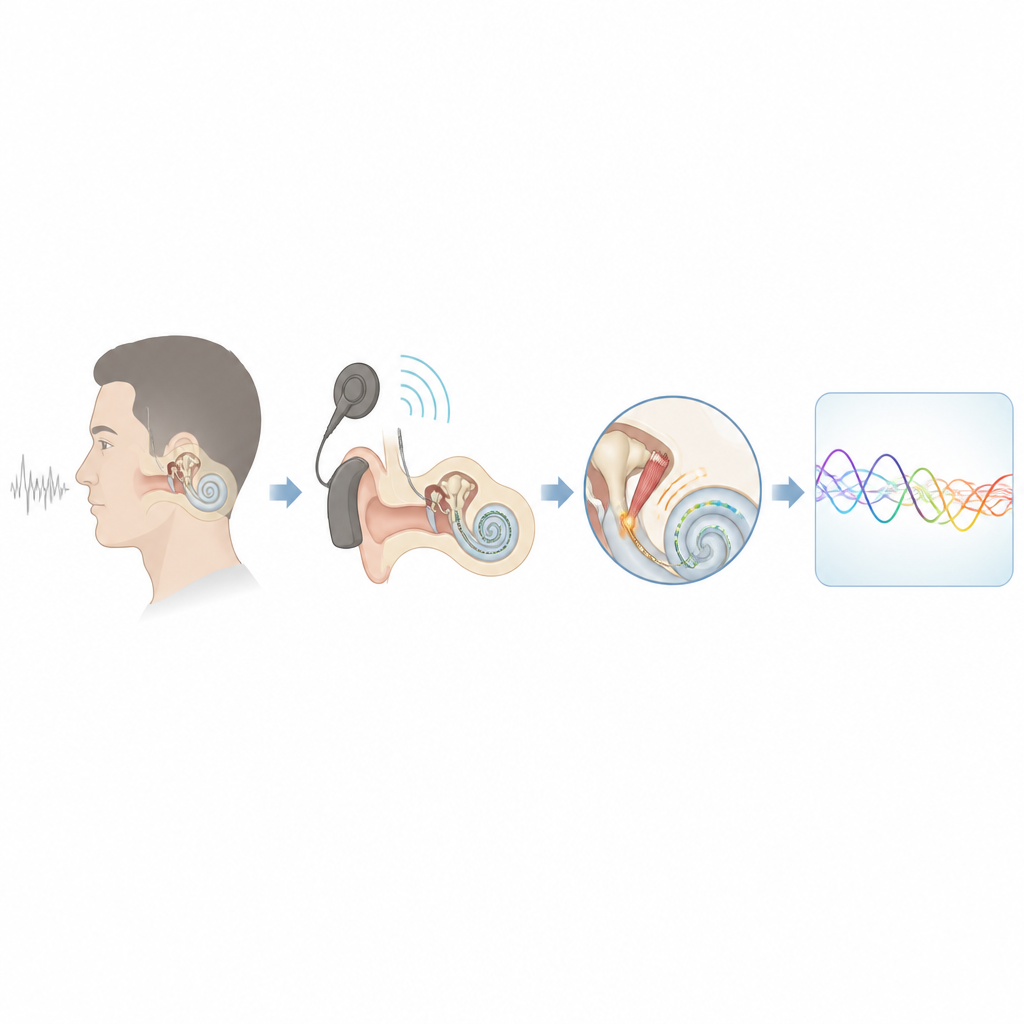
A tiny ear muscle with a big job
Inside the middle ear sits the stapedius muscle, the smallest skeletal muscle in the human body. When we hear sounds that are too loud, this muscle automatically tightens, stiffening the chain of tiny ear bones and helping to protect the inner ear. In people with cochlear implants, the same reflex can be triggered not by sound in the ear canal but by electrical stimulation from the implant inside the cochlea. The point at which the muscle first reacts is called the stapedius reflex threshold, and earlier work has shown that this threshold often lines up with the level that patients describe as comfortably loud. That makes the reflex an attractive “built in meter” for setting implant levels.
Limitations of current reflex checks
Clinically, doctors usually monitor this reflex in an indirect way, by placing a probe in the outer ear canal and watching how sound energy bounces off the eardrum as the middle ear stiffens. This works only when the delicate mechanics of the middle ear are intact. If the tiny tendon that connects the stapedius muscle to the ear bones is missing, or the middle ear is malformed, the indirect method may fail even if the muscle itself is responding. It is also not practical as a permanent sensor that could feed information directly back to the implant. These limitations have led researchers to ask whether they can measure the muscle’s own electrical activity instead, right where it sits, during cochlear implant surgery.
A new route to reach and record the muscle
In this study, surgeons in two German hospitals operated on 14 adults with hearing in one ear and profound deafness in the other ear who were receiving a cochlear implant. Before surgery, high resolution scans were used to map each patient’s middle ear and plan the safest path to reach the stapedius muscle. In most patients, the team used a so called retrofacial approach, carefully drilling behind the facial nerve to expose the full belly of the muscle and insert fine paired electrodes. In three patients whose anatomy made this route unsafe, the surgeons placed electrodes from the front along the stapedius tendon instead. Throughout, facial nerve monitoring and detailed planning were used to avoid nerve injury, and no surgery related complications were reported.
Listening in on the muscle during stimulation
With the electrodes in place, the researchers first triggered the reflex with loud sound in the opposite ear and recorded the stapedius muscle’s electrical activity, free of any implant related interference. Next, after the cochlear implant electrode was inserted, they used the implant itself to deliver short bursts of electrical stimulation on different contacts. At the same time, they watched the stapedius tendon under the microscope and recorded the muscle’s electrical signals. Careful offline processing allowed them to strip away electrical “noise” from the implant and reveal the underlying muscle response. In eight of the fourteen patients, clear stapedius activity could be captured during implant stimulation, especially when the muscle was reached via the retrofacial route and using the optimized recording setup.
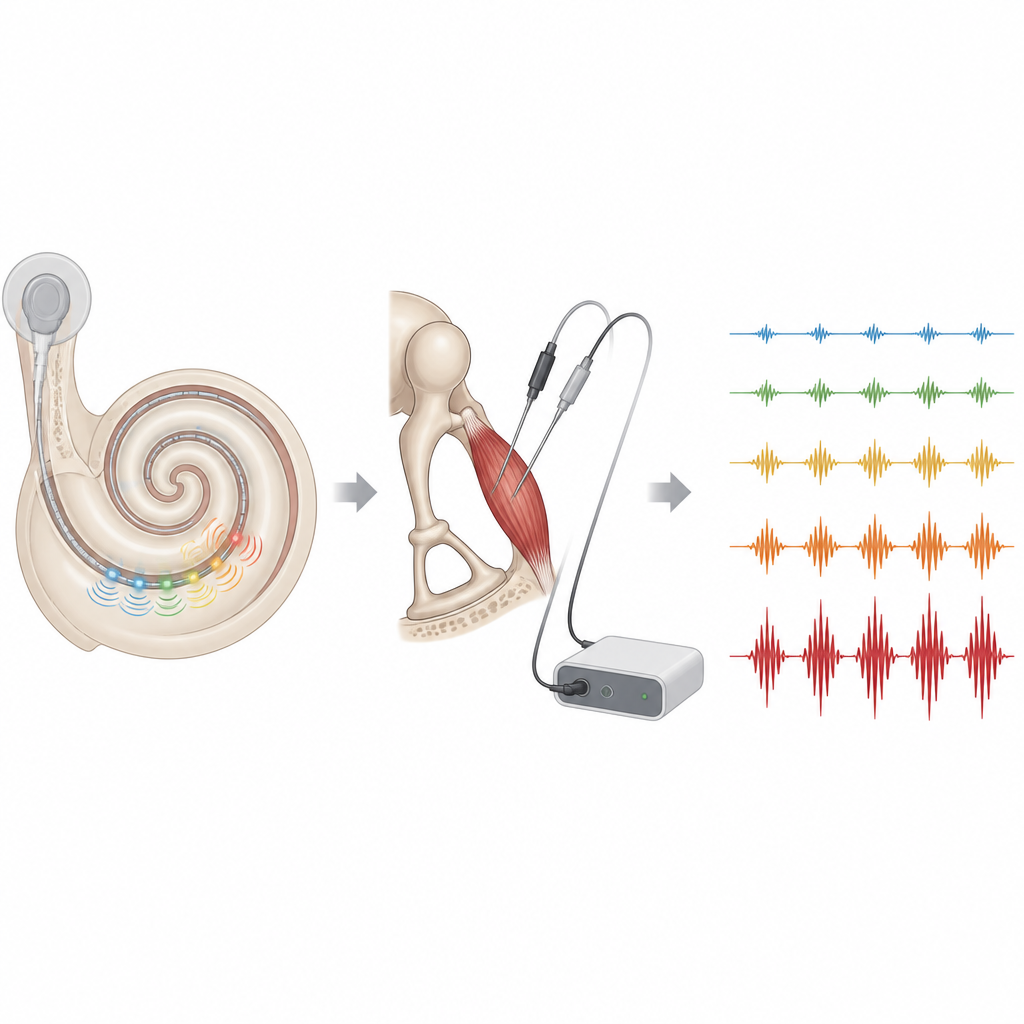
How the new measure compared with the surgeon’s eye
For the patients with the cleanest recordings, the team compared two ways of finding the reflex threshold on each implant contact: the surgeon’s visual judgment of when the tendon first twitched, and the point at which the electrical signal from the muscle clearly rose above baseline. Across 26 such contact by contact comparisons, the electromyography based thresholds were the same as or slightly lower than the visually judged thresholds in the great majority of cases. This pattern fits what is known about muscle physiology, since electrical activity in the muscle always appears before the resulting movement becomes visible. The differences were small, suggesting that the new method and the current visual standard are broadly in agreement.
What this could mean for future implants
For people living with cochlear implants, this work does not change today’s fitting routines yet, but it points toward a future in which the implant could listen to the ear’s own protective reflex while it stimulates. The study shows that, with careful planning and a retrofacial route, surgeons can safely reach the stapedius muscle and record its electrical activity in many adult patients. It also shows that the reflex thresholds derived from these direct measurements closely track what experienced surgeons already judge by eye. Larger studies will be needed to link these intraoperative readings to the loudness levels that patients actually find comfortable after surgery, and to adapt the technique for children and for long term use. If those steps succeed, the stapedius muscle could become a built in sensor that helps future “smart” cochlear implants adjust themselves more objectively and more reliably over time.
Citation: Guntinas-Lichius, O., Arnold, D., Volk, G.F. et al. Electromyography of the stapedius muscle via a retrofacial approach and electrically evoked stapedius reflex during cochlear implant surgery: a prospective bicentric study. Sci Rep 16, 15065 (2026). https://doi.org/10.1038/s41598-026-53093-3
Keywords: cochlear implant, stapedius reflex, electromyography, hearing loss, ear surgery