Clear Sky Science · en
Ultrasound-guided percutaneous electrolysis versus dry needling in patients with chronic low back pain a double-blind randomized clinical trial
Why Your Aching Back Matters
Chronic low back pain is one of the most common reasons adults visit a doctor, miss work, or give up favorite activities. Many people live for years with pain that has no clear cause on scans, and standard treatments—pills, exercise, or manual therapy—do not always bring enough relief. This study looked at a newer needle-based technique, called ultrasound-guided percutaneous electrolysis, and compared it with a more established approach, electrical dry needling, to see which one better reduces pain and improves daily life for people with long-standing, non-specific low back pain.
Two Needle Paths to the Same Goal
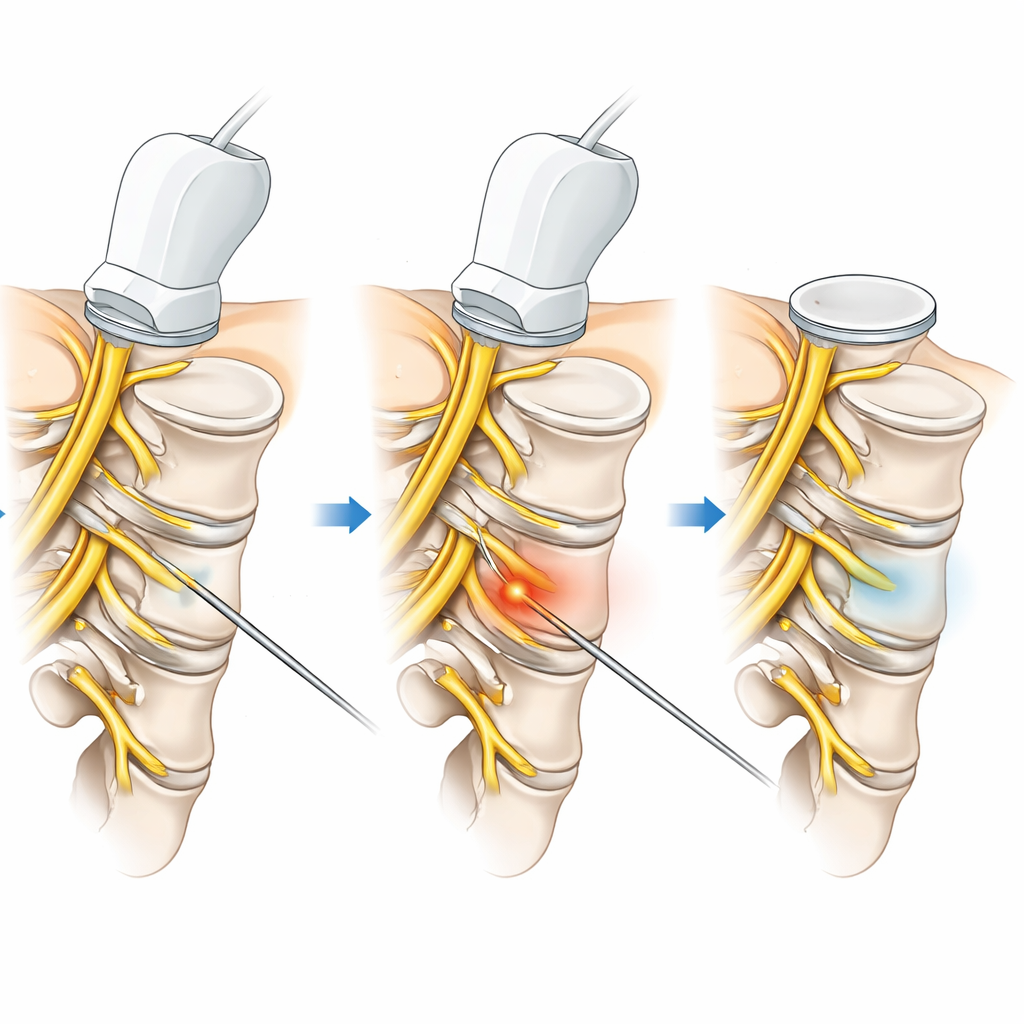
The researchers recruited 70 adults between 30 and 67 years old who had been living with non-specific low back pain for at least three months and had meaningful limits in daily activities. After screening, 64 participants completed the trial. They were randomly assigned, like flipping a coin, to one of two groups. One group received ultrasound-guided percutaneous electrolysis: a very thin needle was guided near the nerve roots in the lower spine (levels L3 to L5) while a small direct electrical current was applied for a few seconds. The other group received electrical dry needling, where needles were placed directly into painful muscle knots in the lower back muscles and then connected to a low-frequency current for 30 minutes. Both groups had one treatment session per week for six weeks.
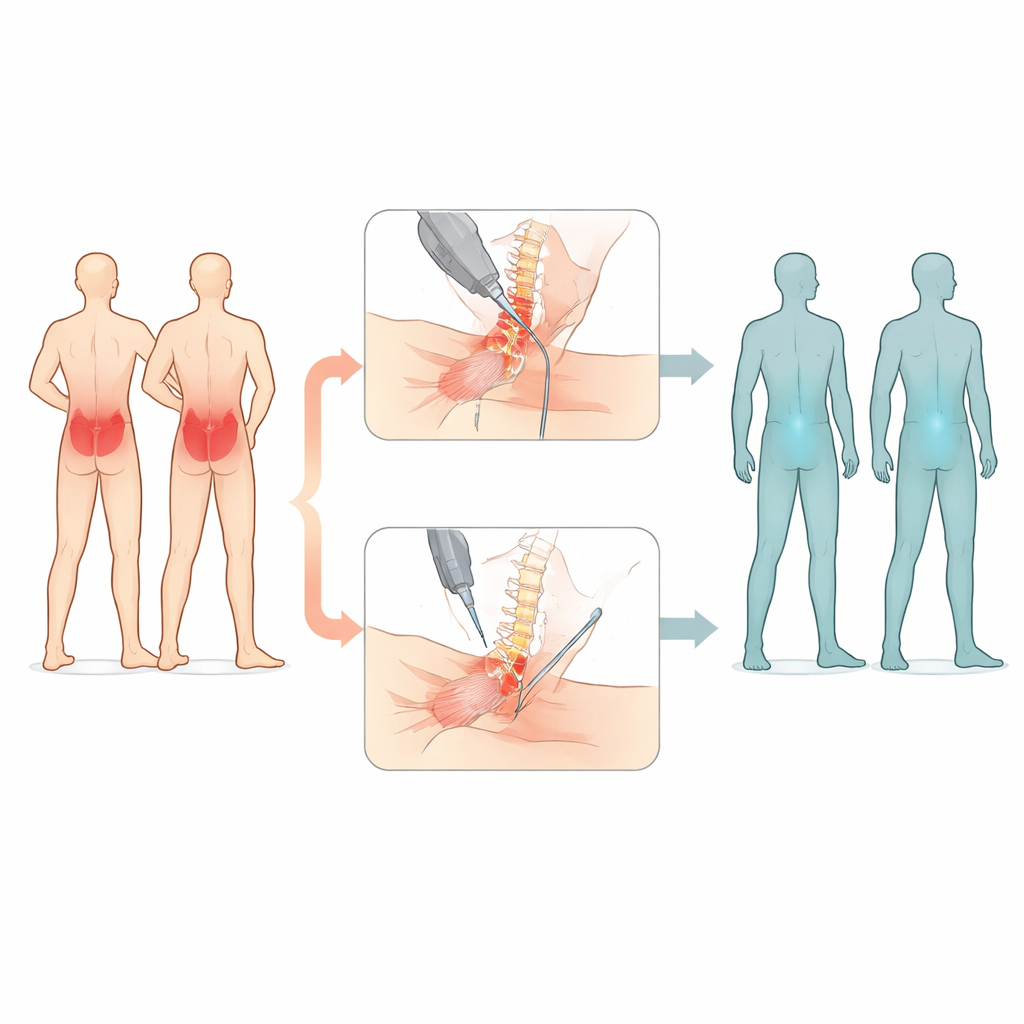
How the Study Was Carried Out
To judge which treatment worked better, the team used several types of tests. They measured how sensitive painful spots in the back muscles were by gently pressing with a handheld device, and they asked participants to rate their pain on a simple line scale. They also used standard questionnaires to assess how much back pain interfered with daily tasks, how afraid people were to move because of pain, and how they felt about their overall health, sleep, and mood. Physical tests looked at endurance of the abdominal muscles and how far people could reach toward the floor while bending forward. These measures were taken before treatment began, halfway through, right after the six-week course, and again one month later.
What Changed in Pain and Movement
Both treatments helped, but the ultrasound-guided electrolysis generally performed better on key measures. Participants in this group developed higher tolerance to pressure on painful muscle spots, meaning those areas became less tender. Over time, people receiving electrolysis reported a larger drop in pain intensity, and by the one-month follow-up the pain reduction was big enough to be considered clearly meaningful in daily life. They also showed greater improvement in disability scores—how much pain limited their activities—although the size of this change did not always reach the threshold researchers use to label it a strong clinical shift. Fear of movement also fell more in the electrolysis group, suggesting that patients felt more confident bending and using their backs. Simple movement tests, such as how close they could get their fingers to the floor, also tended to improve more with electrolysis.
Effects on Sleep, Everyday Life, and Mood
Beyond pain and movement, the team explored how each treatment touched broader aspects of life. People treated with electrolysis reported improvements in certain parts of a general health survey, especially in bodily pain and social functioning, meaning they felt more able to take part in everyday roles and interactions. Some aspects of sleep, particularly daytime sleepiness related to poor nighttime rest, also improved more in the electrolysis group. However, when it came to deeper emotional measures such as anxiety and depression, neither treatment produced large or lasting changes. The procedures were generally safe: the only side effects were short-lived soreness or heaviness in the treated area, which cleared within a few days.
What This Means for People With Back Pain
Put simply, this study suggests that guiding a needle near key nerves in the lower spine and delivering a brief electrical dose may ease chronic low back pain more than treating painful muscle knots alone. People receiving ultrasound-guided percutaneous electrolysis tended to hurt less, move a bit better, and feel more able to participate in daily life, at least in the short term. The technique did not appear to be a cure-all and did not strongly shift mood problems linked to chronic pain, but it looks like a promising addition to exercise and other conservative care. Longer studies in larger and more varied groups will be needed to see how long these benefits last and whether the extra equipment and training required are worth the added cost.
Citation: Saavedra-Hernández, M., Lara-Palomo, I.C., Sánchez-Ferre, C. et al. Ultrasound-guided percutaneous electrolysis versus dry needling in patients with chronic low back pain a double-blind randomized clinical trial. Sci Rep 16, 10649 (2026). https://doi.org/10.1038/s41598-026-45876-5
Keywords: chronic low back pain, percutaneous electrolysis, dry needling, musculoskeletal rehabilitation, pain management