Clear Sky Science · en
Machine-learning prediction and risk stratification of 12-month cognitive decline in Alzheimer’s disease using routine clinical and MRI data
Why predicting memory decline matters
Alzheimer’s disease slowly robs people of their memory and thinking, but not everyone declines at the same pace. Some patients lose several points on simple mental tests within a year, while others remain relatively steady. Being able to tell, at the time of diagnosis, who is likely to worsen quickly could help doctors plan visits, support families, and choose patients for clinical trials of new treatments. This study asks whether information that many memory clinics already collect—brief thinking tests and routine brain scans—can be combined with modern computer methods to forecast who will decline over the next 12 months.
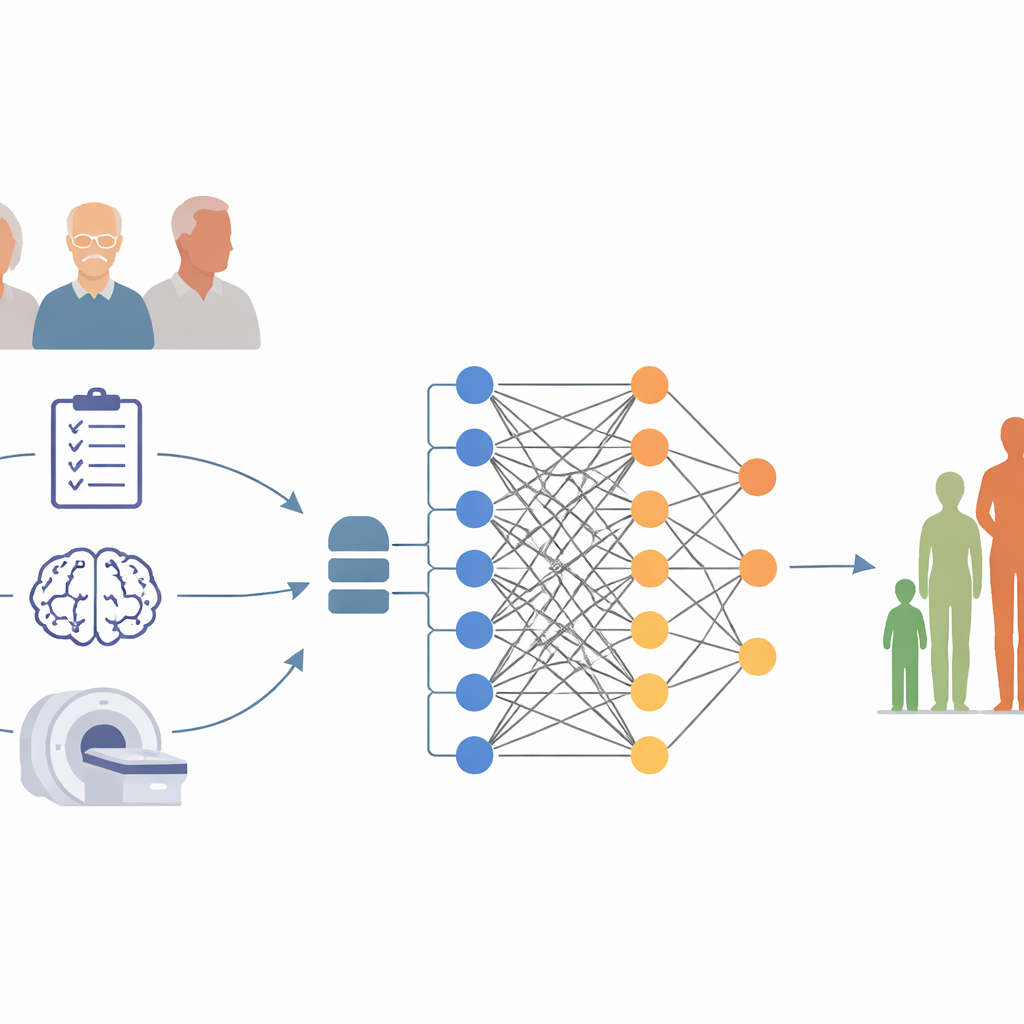
Who was studied and what was measured
The researchers used data from the Alzheimer’s Disease Neuroimaging Initiative, a long-running project that follows people with memory problems using standardized tests and brain imaging. They focused on 306 participants who already had a diagnosis of Alzheimer’s disease and who completed a memory test called the Mini-Mental State Examination, or MMSE, at the start of the study and again one year later. A drop of three or more MMSE points over 12 months was treated as a meaningful decline. At the beginning, each person provided basic information such as age, sex, and years of education, completed several detailed thinking and daily-function questionnaires, and underwent a brain MRI scan that measured the size of key brain regions involved in memory.
How the computer models were built
To see whether near‑term decline could be predicted, the team built and compared two types of forecasting tools. The first was a straightforward statistical formula using just a handful of clinic-friendly measures: age, sex, and scores on two standard thinking tests. The second was a more flexible machine-learning model known as a random forest, which could consider the full set of clinical scores together with MRI measures such as hippocampal volume and the size of the brain’s fluid-filled spaces. The data were repeatedly split into training and testing subsets so that each person’s outcome was predicted by a model that had not yet “seen” that person, mimicking how the tool might behave in new patients.
How well the models predicted decline
About 43% of participants experienced a meaningful MMSE drop over 12 months. Both approaches did better than chance at identifying these individuals. The simple clinical model reached a performance level typically considered “moderate” for medical prediction tools. The random-forest model did slightly better overall and, importantly, showed greater “net benefit” across a wide range of practical risk thresholds. Net benefit is a way of weighing correct and incorrect predictions against the consequences of acting on them—for example, deciding which patients should be monitored more closely or considered for more intensive care. Although the more complex model was not perfect and showed some signs of overfitting, it consistently provided more useful guidance than strategies that either assumed everyone would decline or that nobody would.
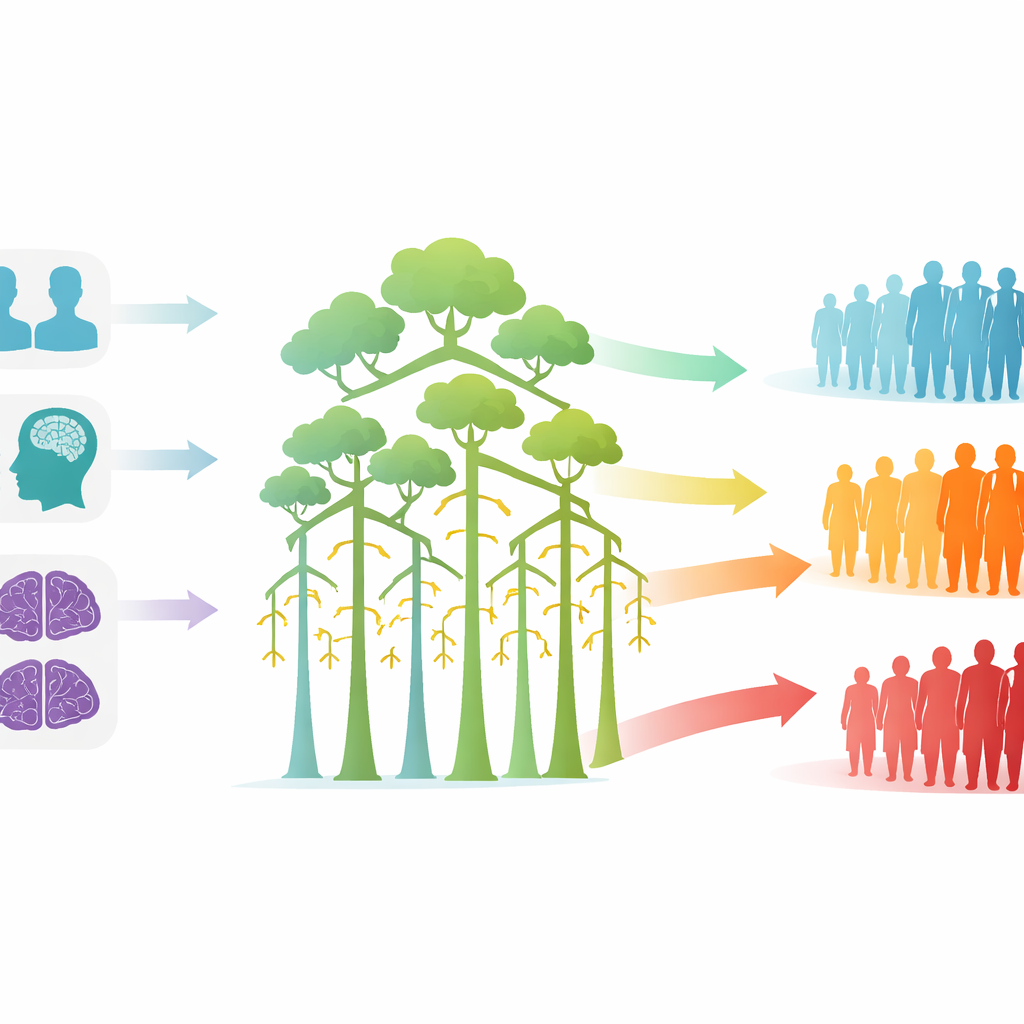
Turning scores into low, medium, and high risk
To make the results easier for clinics to use, the researchers translated the model’s output into three simple risk bands. People whose predicted chance of decline was below one quarter formed a low-risk group; only about one in eight of them actually declined, and their average test scores were almost unchanged after a year. Those in the middle band had roughly a one-in-three chance of decline, and on average lost around one and a half MMSE points. The high-risk group, with predicted chances above one half, saw decline in about two out of three patients and an average loss of more than four MMSE points. This clear stepwise pattern suggests that the model’s probabilities can be turned into practical categories that could guide how often patients are seen and which ones might be prioritized for trials or additional testing.
What this means for patients and clinics
The study shows that by combining routine memory tests with standard MRI scans, and analyzing them with modern computer methods, it is possible to moderately accurately estimate an individual Alzheimer’s patient’s risk of noticeable decline over the next year. While the tool still needs to be checked and adjusted in different hospitals and more diverse populations before being used in everyday care, it points toward a future in which follow-up schedules and trial enrollment are tailored to each person’s likely trajectory, rather than treating all patients as if their disease will progress at the same speed.
Citation: Geng, Y., Zhang, H. Machine-learning prediction and risk stratification of 12-month cognitive decline in Alzheimer’s disease using routine clinical and MRI data. Sci Rep 16, 12227 (2026). https://doi.org/10.1038/s41598-026-43321-1
Keywords: Alzheimer’s disease, cognitive decline, machine learning, brain MRI, risk stratification