Clear Sky Science · en
High gastrointestinal carriage rates of extended-spectrum-β-lactamase-producing enterobacterales and associated factors among hospitalized and nonhospitalized children in Kenya
Why tiny germs in children’s bellies matter
Across the world, doctors are running out of medicines that can reliably cure infections. One reason is that some gut bacteria in healthy-looking people quietly learn to resist even powerful antibiotics. This study from a busy public hospital in Thika, Kenya, looked at children under five years old to see how often they carry such hard-to-treat bacteria in their intestines, and what everyday factors—like age or how medicines are bought—might be feeding this hidden problem.
Checking the hidden passengers
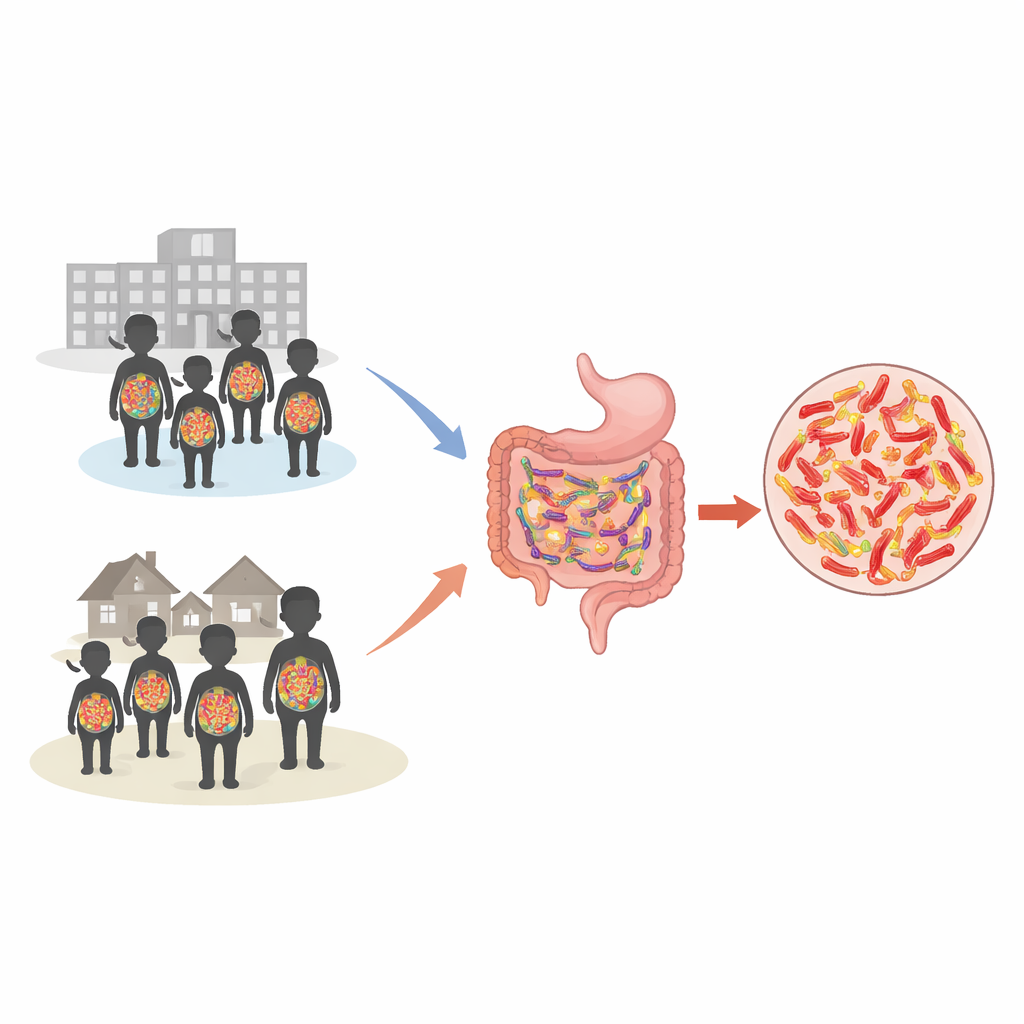
The researchers focused on a family of gut bacteria called Enterobacterales, which normally live harmlessly in human intestines but can cause serious infections when they spread to the blood, lungs, or urinary tract. Some of these bacteria produce special enzymes that break down widely used antibiotics, allowing them to survive treatment. From February to June 2023, the team recruited 540 children, half visiting the outpatient clinic and half admitted to the hospital for at least two days. Parents answered questions about their child’s health, medicine use, and water sources, and each child provided either a stool sample or a rectal swab. These samples were cultured and analyzed with modern laboratory machines to identify which bacteria were present and how resistant they were to different antibiotics.
How common were the tough bacteria?
The findings were striking: more than one in three children carried these resistant bacteria in their intestines. The overall carriage rate was 35.4 percent, and it was actually higher in children coming from home to the clinic (40.4 percent) than in those already in the hospital (30.4 percent). The most frequent culprit by far was Escherichia coli, a common gut resident that can turn dangerous when it carries resistance traits. Many of the resistant strains were not just shielded against one drug family. They often withstood several important antibiotic classes at once, including commonly used drugs such as aminoglycosides, quinolones, and sulfonamides. Only a few medicines, notably piperacillin/tazobactam and colistin, still worked against most of these bacteria.
The rise of last-resort resistance
Even more worrying was that nearly half of the resistant strains were no longer reliably stopped by carbapenems, antibiotics often considered a last resort for severe infections. Some of these carbapenem-resistant strains also produced special enzymes called carbapenemases, which make the bacteria extremely difficult to treat. These highly resistant organisms were found in both hospitalized and nonhospitalized children in similar numbers, underscoring that the problem is not confined to the hospital ward. Again, E. coli dominated among these most threatening bacteria, signaling that an ordinary gut resident is becoming a powerful carrier of resistance genes in very young children.
Who was most at risk?
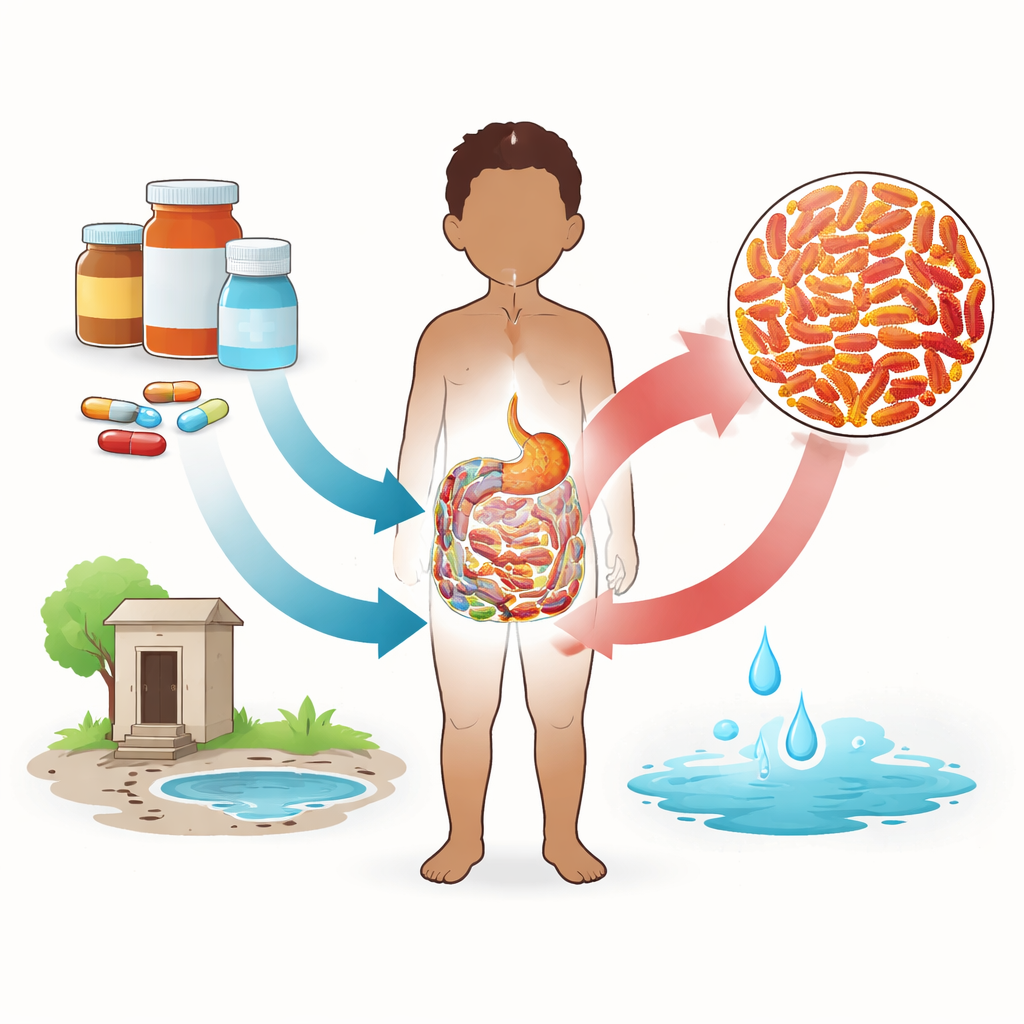
The team looked closely at which children were more likely to harbor resistant bacteria. Age stood out: children younger than two years had significantly higher odds of carrying these strains than older children. This may reflect behaviors like frequent hand-to-mouth contact and greater exposure to contaminated surfaces. Another key factor was how antibiotics were obtained. Among outpatients, children whose caregivers bought antibiotics from retail drug shops without a clinician’s prescription were much more likely to carry resistant bacteria. In contrast, when medicines were obtained from pharmacies with a proper prescription, the likelihood of carriage dropped sharply. Other factors such as type of drinking water did not show a strong independent effect in this study.
What this means for families and communities
For parents, these results highlight that resistance can be building silently in children long before any serious infection appears. The study shows that very young children in Kenya already carry high levels of bacteria that can shrug off multiple drugs, including those used as a last line of defense. It also points to practical steps: improving hygiene in homes, childcare settings, and hospitals, and curbing over-the-counter antibiotic use without medical guidance. By protecting children from contaminated environments and ensuring that powerful medicines are used carefully and only when truly needed, communities can slow the spread of these dangerous gut bacteria and help keep lifesaving treatments effective for the infections that really require them.
Citation: Githii, S., Ndungu, C., Maingi, J.M. et al. High gastrointestinal carriage rates of extended-spectrum-β-lactamase-producing enterobacterales and associated factors among hospitalized and nonhospitalized children in Kenya. Sci Rep 16, 12972 (2026). https://doi.org/10.1038/s41598-026-43265-6
Keywords: antimicrobial resistance, drug-resistant gut bacteria, children in Kenya, hospital and community infections, antibiotic misuse