Clear Sky Science · en
Development and field evaluation of a rapid detection method for Babesia microti using fluorescent recombinase polymerase amplification(RPA) technology
Why a Hidden Tick Parasite Matters
Many people think of tick bites as a nuisance, but some ticks carry Babesia microti, a microscopic parasite that quietly invades red blood cells. In healthy people it can cause flu-like illness; in vulnerable patients, especially those receiving blood transfusions, it can be life-threatening. Detecting this parasite early is difficult because it often lurks at very low levels in the blood. This study describes a new rapid test that aims to spot B. microti quickly, accurately, and even outside of advanced laboratories, helping protect both patients and the blood supply.
A Stealth Infection in the Blood
Babesiosis, the disease caused by Babesia parasites, is a growing concern in several parts of the world, including China and the United States. Ticks transmit the parasite from wild and domestic animals to humans, where it hides inside red blood cells. Early symptoms, such as fever, tiredness, and anemia, can easily be mistaken for malaria or other common infections. Because the parasite can circulate at extremely low levels, standard blood-smear microscopy or even some molecular tests often miss early or mild infections. This is especially worrisome for blood banks, since apparently healthy donors can unknowingly pass the parasite to transfusion recipients.
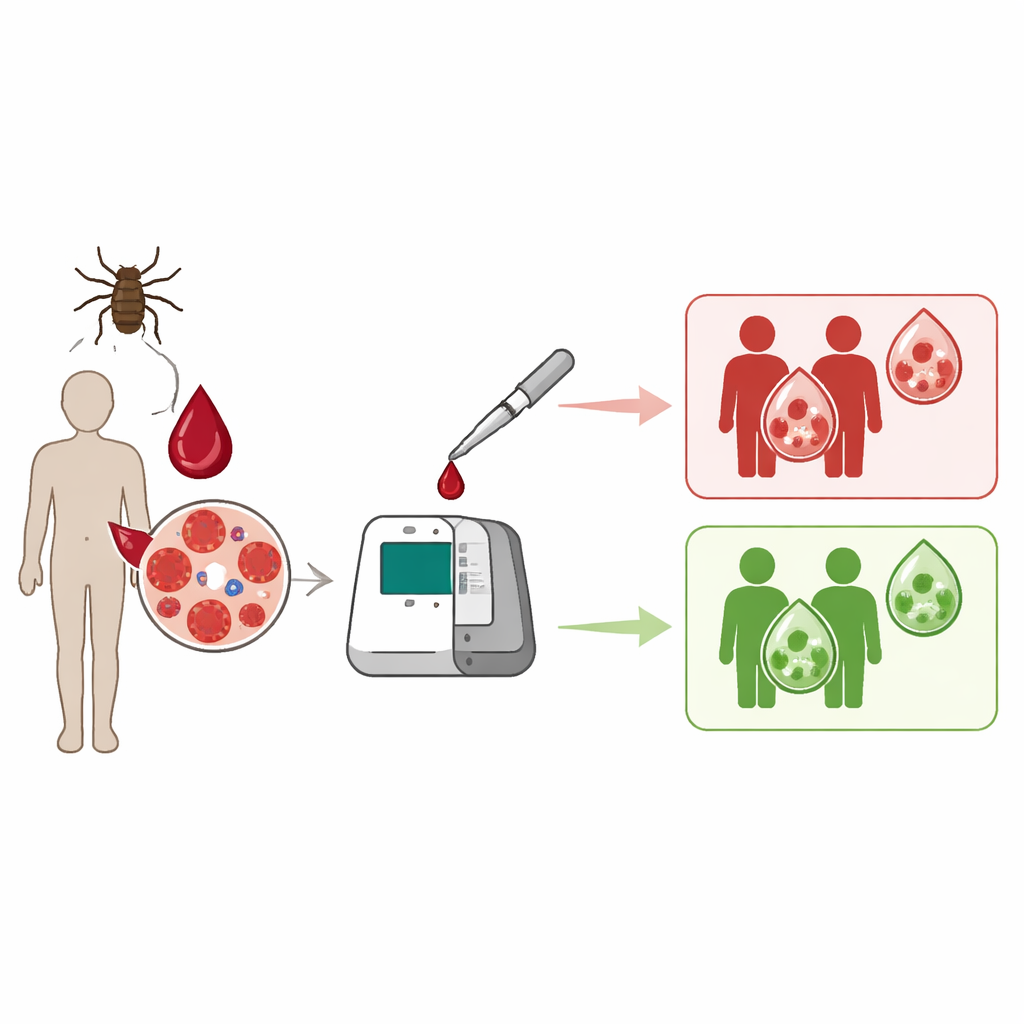
A Faster Way to Spot the Parasite
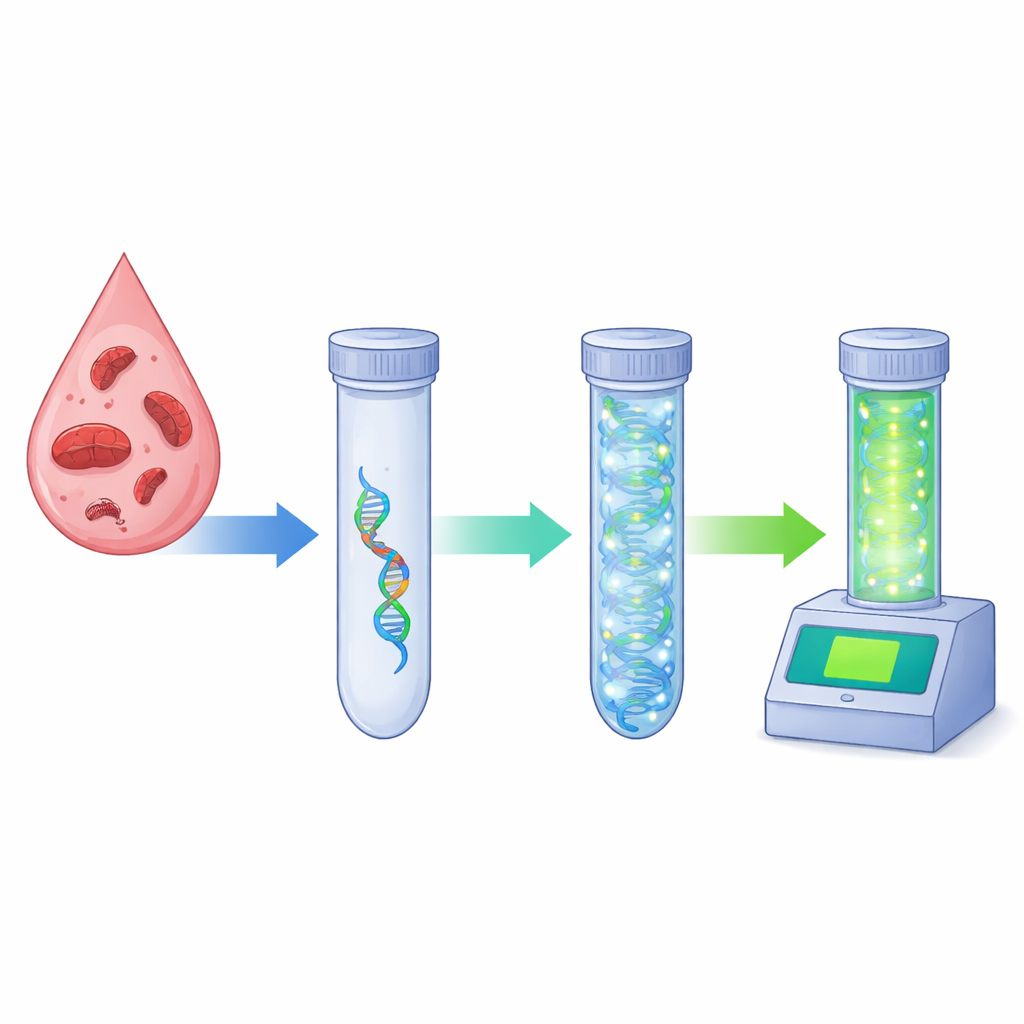
The researchers focused on a technique called recombinase polymerase amplification, or RPA, which can copy specific pieces of DNA at a constant, mild temperature. Unlike conventional PCR, which needs precise heating and cooling cycles and specialized machines, RPA can run at around body temperature in about 20 minutes, making it promising for use in clinics or field settings. The team designed RPA reagents that target a highly conserved genetic region of B. microti known as 18S rRNA, carefully screening and optimizing primer and probe sequences to ensure they recognized B. microti but not related organisms such as malaria parasites.
Testing Sensitivity, Specificity, and Speed
After building the assay, the scientists asked three key questions: How little parasite DNA can it detect, does it confuse B. microti with other microbes, and how does it perform in real blood samples? In the laboratory, the fluorescent RPA test reliably detected as little as 1 femtogram of B. microti DNA per microliter—roughly equivalent to a handful of parasites in a milliliter of blood—and worked optimally at 39 °C in just 20 minutes. When they compared it to a standard nested PCR method, the new test was about ten times more sensitive for pure DNA and roughly 600 times more sensitive when they diluted infected mouse blood, finding as few as 0.046 parasites per microliter, far below the reach of many existing clinical methods.
From Mice and Patients to Real-World Clinics
The team then moved beyond purified DNA. In a controlled mouse model, they followed infections over time and compared three approaches: traditional microscopy, nested PCR, and the new RPA test. Microscopy did not detect the parasite until day 15 after infection, nested PCR became positive in some animals by day 9, and RPA detected infections in more animals earlier, with all mice testing positive by day 12. The assay also correctly identified two confirmed human babesiosis cases. Finally, the researchers applied the test to 119 people in China’s Henan Province who had fever and low platelet counts, symptoms that can be caused by several tick-borne diseases. RPA found B. microti in 21 patients, while nested PCR found 20; statistical analysis showed that the two methods agreed closely, but RPA captured one extra positive case. The study also revealed that many patients carried both B. microti and Bunyavirus, underscoring how co-infections complicate diagnosis.
What This Means for Patients and Blood Safety
To a non-specialist, the central message is straightforward: this fluorescent RPA test offers a quick, portable, and very sensitive way to detect a dangerous tick-borne parasite in blood. By finding B. microti at parasite levels far below what microscopes and many standard tests can see, it could help clinicians diagnose patients earlier, guide appropriate treatment instead of confusing babesiosis with malaria, and strengthen screening in areas where the parasite threatens the blood supply. While practical challenges remain before it can be widely deployed, the study shows that simple, field-ready DNA tests can play a powerful role in defending public health against emerging tick-borne infections.
Citation: Cai, Y., Yang, H.Y., Qiang, K. et al. Development and field evaluation of a rapid detection method for Babesia microti using fluorescent recombinase polymerase amplification(RPA) technology. Sci Rep 16, 14188 (2026). https://doi.org/10.1038/s41598-026-42288-3
Keywords: babesiosis, tick-borne disease, blood transfusion safety, rapid DNA testing, Babesia microti