Clear Sky Science · en
Nitric oxide induces p53-mediated cell death in human nasal epithelial cells
Why your nose’s front line matters
Your nasal passages are more than just air ducts; they form a living shield that helps keep viruses, bacteria, and pollutants out of the body and brain. During infections and chronic inflammation, this shield is bathed in chemical signals that fight germs but can also damage our own cells. One such molecule, nitric oxide, is a well-known defender and troublemaker. This study asks a simple but important question: when nitric oxide lingers at high levels around the nasal lining, does it quietly weaken this first line of defense?
A helpful gas with a dark side
Nitric oxide is a tiny gas molecule that our bodies use to widen blood vessels, aid nerve communication, and power immune defenses. Immune cells release bursts of it to help kill invading microbes, and in normal amounts it supports healthy function. But in strong or prolonged immune reactions, nitric oxide can be produced in excess and react with oxygen to form highly aggressive chemical species. These can damage DNA and other vital cell components, turning a helpful weapon into a source of collateral damage. Because the nasal lining is directly exposed to the outside world and is a major entry point for respiratory viruses such as SARS-CoV-2, understanding how long-lasting nitric oxide exposure affects these cells is crucial.
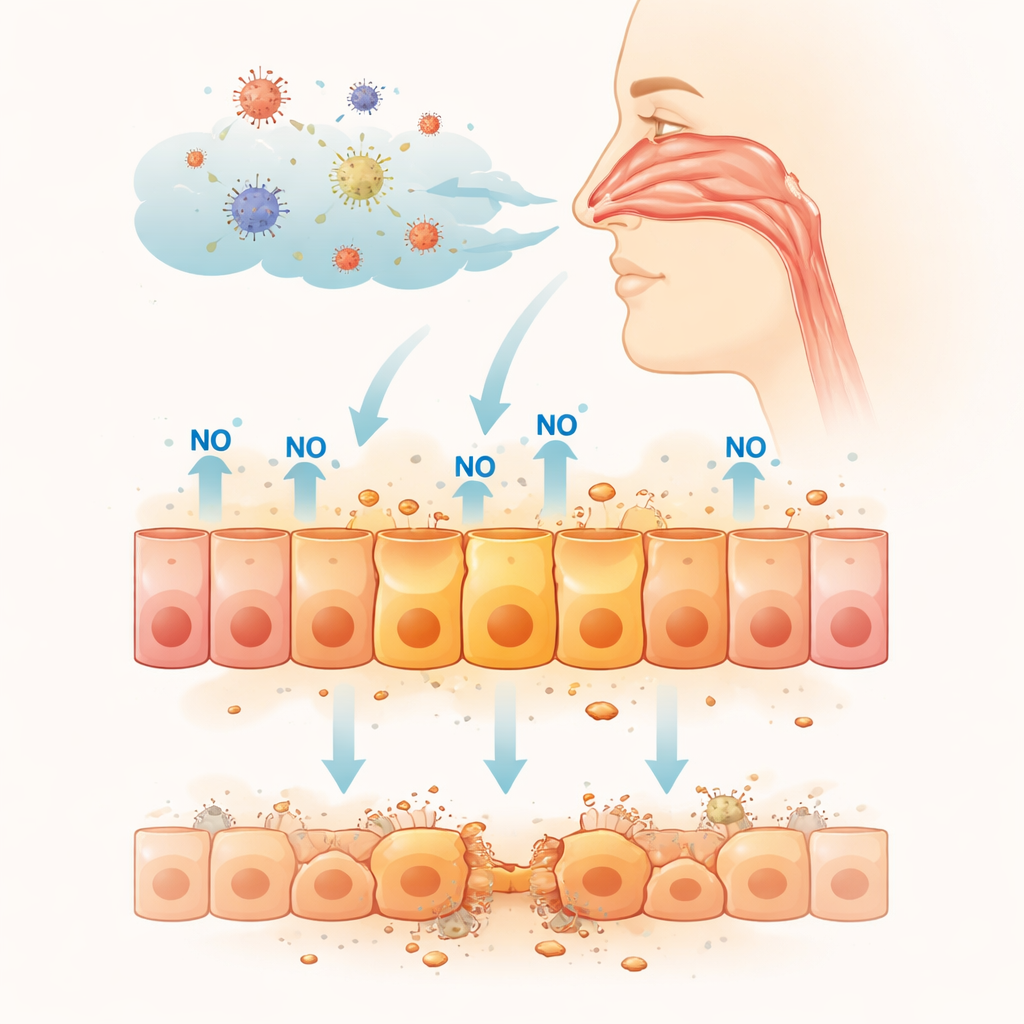
Testing long-term exposure in nasal cells
To explore this, the researchers used a human nasal epithelial cell line grown in the laboratory, a widely used stand-in for the nasal barrier. They exposed these cells for up to three days to a nitric oxide–releasing compound at levels similar to those reported in inflamed tissues. Over time, cell growth slowed and more cells died, indicating that sustained nitric oxide is toxic to this nasal model. To uncover what was happening inside the cells, the team analyzed which genes were switched on or off after 48 hours of exposure. Hundreds of genes changed their activity, and many of the most strongly activated ones turned out to be connected to a central cellular guardian protein called p53, which monitors DNA damage and controls whether cells repair themselves, stop dividing, or self-destruct.
How the cell’s guardian turns against damaged cells
Follow-up experiments confirmed that nitric oxide causes p53 protein to accumulate in nasal cells within just a few hours, a hallmark of its activation. As p53 levels rose, so did the activity of several of its target genes that push cells toward programmed cell death and halt the cell cycle. Markers of apoptosis, the tidy self-destruct program that breaks cells into small, disposable fragments, increased over time. When the scientists used a drug that specifically blocks p53’s ability to control genes, both the surge in p53 target genes and the amount of cell death were significantly reduced. This showed that p53 is a major driver of nitric-oxide-induced loss of nasal epithelial cells, even though other pathways likely contribute as well.
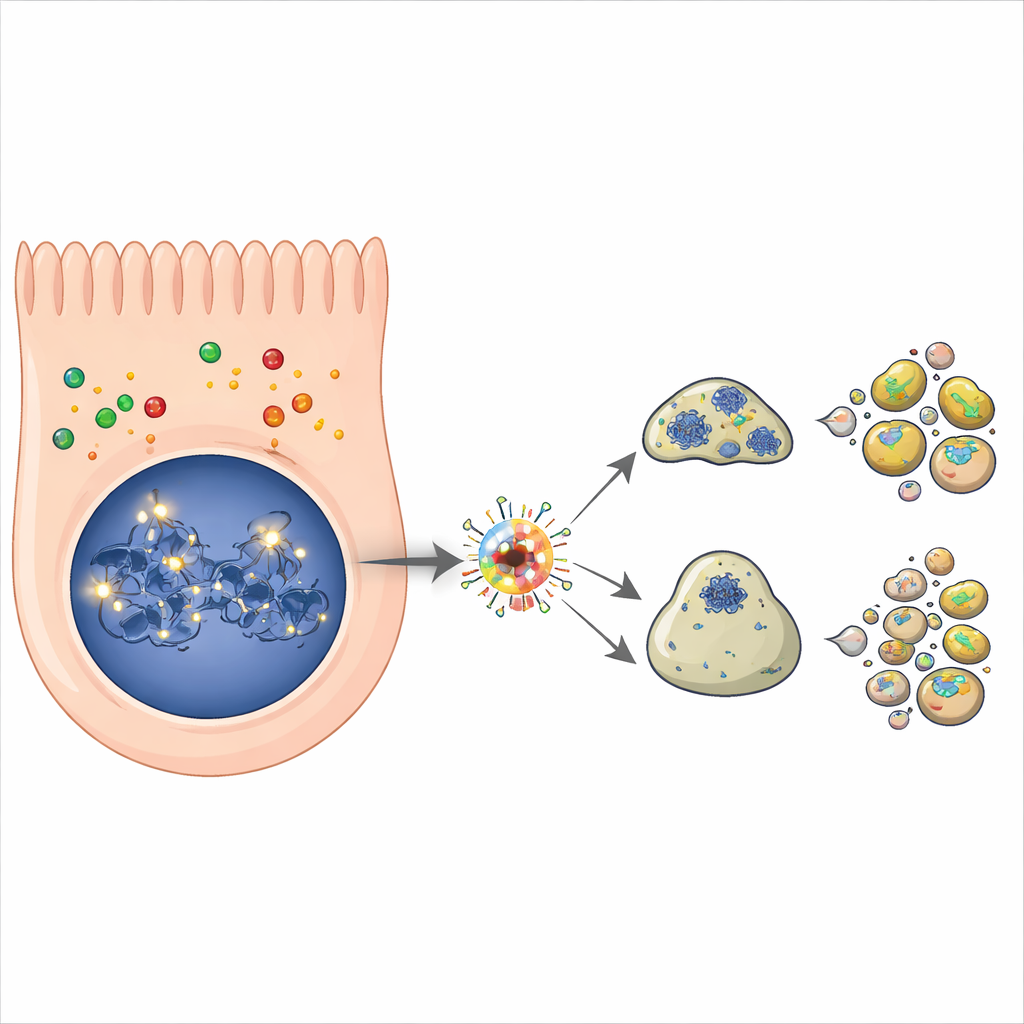
Links to inflammation, smell loss, and chronic disease
The findings fit into a larger picture in which nitric oxide and p53 together shape how tissues respond to stress and inflammation. In conditions such as COVID-19, nasal inflammation and nitric oxide–producing enzymes are elevated, and p53 activity is thought to rise during intense immune reactions. The study suggests a plausible chain of events: during an inflammatory surge, sustained nitric oxide could damage DNA in nasal cells, activate p53, and trigger their death. Over time, this may thin or disrupt the nasal barrier, making it easier for viruses, pollutants, and inflammatory signals to penetrate deeper into the respiratory tract or even reach the brain. Such damage could contribute to persistent problems like long-lasting loss of smell or chronic nasal and airway disease.
What this means for protecting the nasal barrier
In plain terms, the study shows that when nitric oxide sticks around at high levels, it can push nasal lining cells to activate their internal “self-destruct” switch through p53, reducing cell numbers and potentially weakening the barrier inside the nose. While the work was done in a simplified cell system and not in living humans, it underscores that the body’s own defense chemicals must be carefully balanced. Too little nitric oxide can impair immune protection, but too much for too long may erode the very tissues that protect us. A better understanding of this balance could eventually inform strategies to preserve nasal barrier health during severe infections and chronic inflammation.
Citation: Kamiuezono, S., Kubota, S., Tsuchida, T. et al. Nitric oxide induces p53-mediated cell death in human nasal epithelial cells. Sci Rep 16, 10055 (2026). https://doi.org/10.1038/s41598-026-40908-6
Keywords: nitric oxide, nasal epithelium, p53, apoptosis, inflammation