Clear Sky Science · en
Multi-modal skin atlas identifies a multicellular immune-stromal community associated with disrupted cornification and specific T cell expansion in atopic dermatitis
Why this itchy skin disease matters
Atopic dermatitis, often called eczema, affects millions of children and adults with red, itchy, easily irritated skin. Doctors know that both the skin’s outer barrier and the immune system are involved, but the exact mix of cells and signals inside a patch of inflamed skin has been hard to see in detail. This study uses cutting-edge single-cell techniques to create a detailed “atlas” of human skin, revealing which cells misbehave in atopic dermatitis and how their conversations may weaken the skin’s protective layer and drive chronic inflammation.
Mapping every cell in healthy and diseased skin
To build this atlas, researchers collected tiny punch biopsies from the skin of adults with and without atopic dermatitis. They analyzed more than 280,000 individual cells from these samples, and then integrated them with over 400,000 cells from earlier studies, yielding a combined map of more than 700,000 skin cells. Using single-cell RNA sequencing, they measured which genes each cell was turning on, and in a subset of T cells they also read out T cell receptor sequences to track which T cells had multiplied in response to triggers. This approach allowed them to distinguish 16 broad cell classes and 86 finer subtypes, including rare populations that are usually missed, such as fully cornified skin cells and specialized fibroblasts.
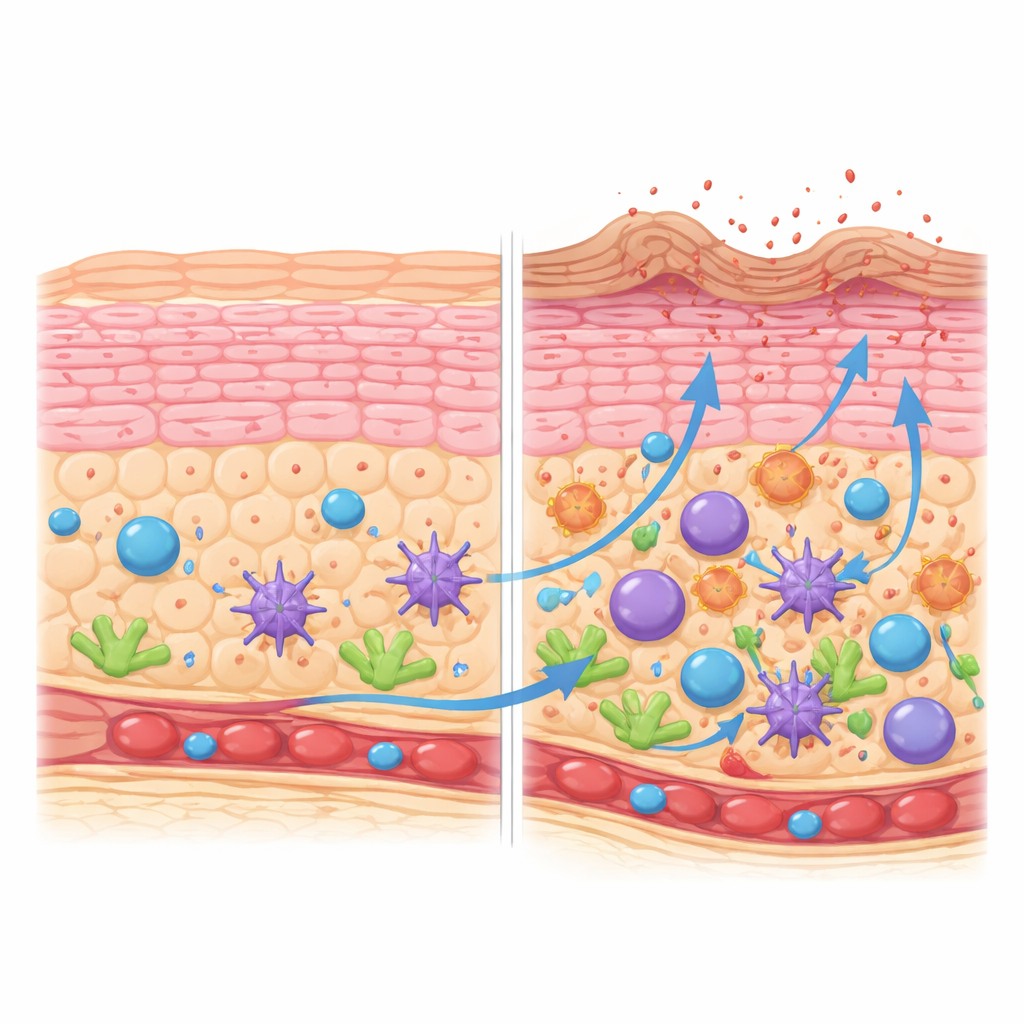
How skin-building cells go off course
The skin’s barrier depends on keratinocytes maturing in an orderly journey from the base layer to a tough, cornified surface. By reconstructing this journey, the team showed that in healthy skin keratinocytes progress smoothly through defined stages, turning on genes that support structure, lipids, and controlled cell death at the right times. In atopic dermatitis lesions, this progression is distorted. There are more dividing keratinocytes and mid-stage cells, but fewer cells that reach a fully mature, cornified state. The top layer is biased toward a less advanced subtype that expresses fewer of the proteins needed to form a strong “brick-and-mortar” barrier, and more small stress-related proteins. These cornified cells also overproduce inflammatory molecules from the interleukin-1 family, tipping the surface toward irritation.
A crowded neighborhood of immune and support cells
Inflamed atopic skin did not just contain more immune cells; it showed a carefully organized shift in who is present. Certain dendritic cells, which pick up and present antigens, accumulated along a maturation path toward a highly activated, migratory state. These cells produced signals that attract and shape T cells and innate lymphoid cells. At the same time, a particular kind of fibroblast, marked by the chemokine CCL19 and enzymes linked to immune regulation, expanded within the skin’s supporting layer. These fibroblasts ramped up genes involved in presenting antigens, guiding immune cells, and remodeling tissue, suggesting that the structural scaffold of the skin actively participates in sustaining inflammation rather than simply holding everything in place.
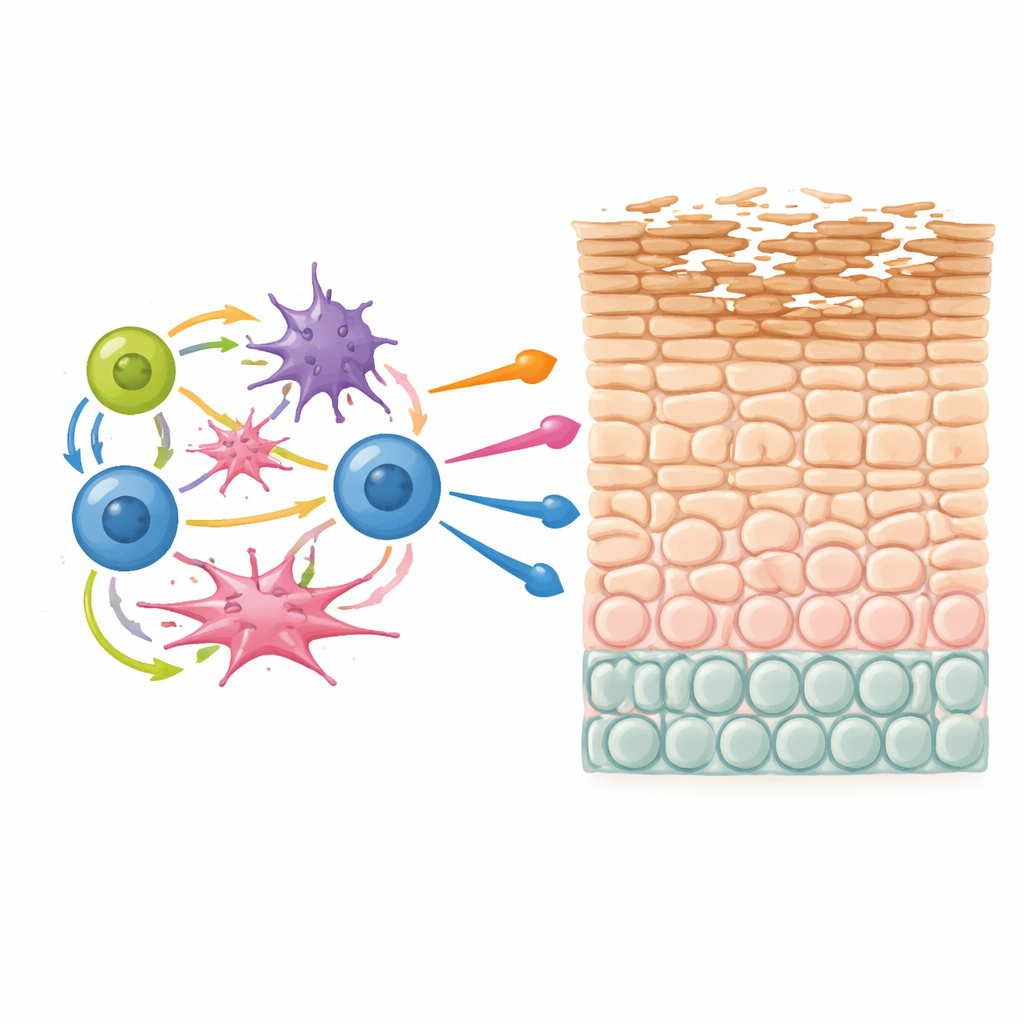
Unique T cells that keep coming back
A striking discovery was a population of T cells found mainly in atopic dermatitis lesions that simultaneously produced three key inflammatory molecules: IL-13, IL-22, and IL-26. These T cells appeared in both helper and killer flavors and shared a common gene program associated with itch, type 2 allergy, and tissue remodeling. By linking gene expression to T cell receptor data, the researchers showed that these triple-producing T cells were often clonally expanded—meaning that a single original T cell had repeatedly encountered its trigger and multiplied. This pattern strongly suggests chronic stimulation, likely by persistent environmental or self-derived antigens in the skin, and identifies these cells as potential key drivers of disease.
A self-reinforcing inflammatory loop tied to genetics
When the team examined how cell types rise and fall together across patients, they identified a multicellular community that repeatedly appeared in lesions. This community included the IL-13/IL-22/IL-26 T cells, activated dendritic cells, cycling innate lymphoid and natural killer-like cells, and CCL19-rich fibroblasts. Computational analysis of ligand–receptor pairs indicated that these cells exchange signals in positive feedback loops—dendritic cells recruit and activate T cells, T cells in turn boost dendritic cells and fibroblasts, and innate cells add further inflammatory cues. Many of the genes highlighted in this network, including well-known risk genes like IL13 and components of the skin barrier such as filaggrin, overlap with regions identified by large genetic studies of atopic dermatitis and related allergic diseases. This suggests that inherited variants may predispose people to form exactly this unstable community, which then disrupts keratinocyte maturation and weakens the barrier.
What this means for people living with eczema
Together, these findings show atopic dermatitis as a problem of a whole neighborhood of cells rather than a single culprit. A specialized group of T cells, dendritic cells, fibroblasts, and innate lymphoid cells appear to lock each other into an inflammatory state that interferes with the skin’s ability to properly cornify and seal itself. Because many current and emerging medicines target the very signals shared within this network, the new atlas helps explain why some treatments work, why others help only subsets of patients, and where new drug targets might lie. For people with eczema, this work points toward future therapies that not only calm immune overactivity but also restore the skin barrier by breaking the harmful cellular conversations that keep the disease going.
Citation: Fiskin, E., Eraslan, G., Alora-Palli, M.B. et al. Multi-modal skin atlas identifies a multicellular immune-stromal community associated with disrupted cornification and specific T cell expansion in atopic dermatitis. Nat Commun 17, 3194 (2026). https://doi.org/10.1038/s41467-026-69587-7
Keywords: atopic dermatitis, skin barrier, single-cell atlas, immune cells, eczema genetics