Clear Sky Science · en
Alox8 knockout exacerbates imiquimod-induced psoriasis-like inflammation
Why this skin story matters
Psoriasis is far more than dry, flaky skin. It is a chronic inflammatory disease that can be painful, stigmatizing, and linked to problems such as arthritis and heart disease. This study explores a little-known enzyme in mouse skin, called Alox8, that helps process fats into chemical messengers. By turning this enzyme off, the researchers uncovered how tiny changes in skin lipids can tip the balance between healing and runaway inflammation, offering fresh clues to why psoriasis flares and what might calm it.
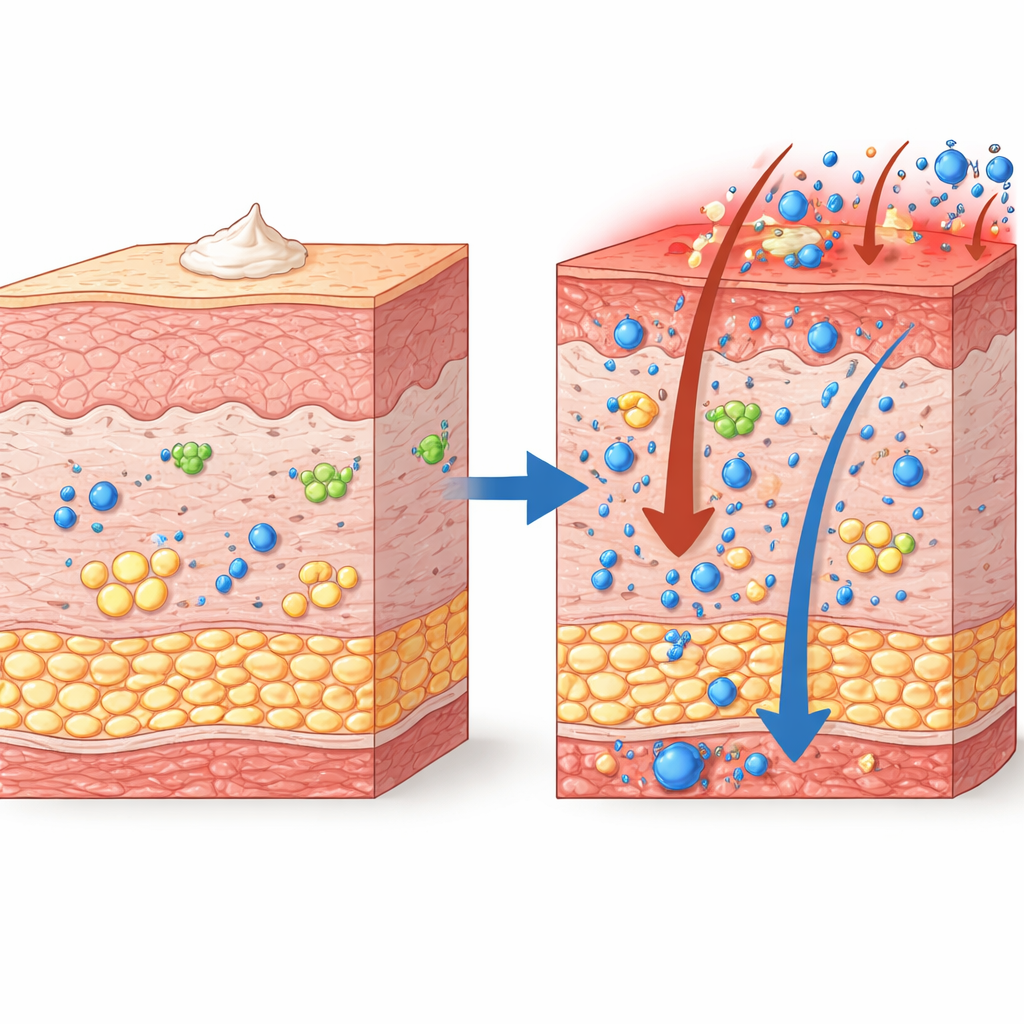
A quiet enzyme with a big job
Our skin is packed with lipids—fats and oils—that not only form a waterproof barrier but also act as signals to immune cells. Enzymes called lipoxygenases turn polyunsaturated fats into short-lived messengers that can either fuel or resolve inflammation. Alox8 is the mouse counterpart of a human enzyme, ALOX15B, which is increased in the skin of people with psoriasis and seems to help switch inflammation off. Before this work, however, the role of Alox8 in living animals and in psoriasis-like disease was unclear, partly because suitable knockout mice did not exist.
Probing psoriasis in mice
The authors engineered mice in which Alox8 was functionally disabled at its active site. They then used a standard model of psoriasis-like skin disease, painting the back skin with imiquimod, an immune-activating cream that triggers redness, thickening, and scaling. First, they mapped where Alox8 is normally active and found strong expression in skin, sebaceous glands, and certain other tissues such as ovary and salivary gland. In healthy animals, Alox8 turned polyunsaturated fats into specific products, but these Alox8-derived lipids were sharply reduced in knockout mice, confirming that the enzyme’s activity was effectively lost.
When the brake is gone, inflammation runs hotter
Compared with normal mice, animals lacking Alox8 developed more severe and longer-lasting psoriasis-like changes after imiquimod. Their skin became thicker and redder, and the outer cell layers showed signs of hyperproliferation rather than orderly maturation. Microscopy revealed increased numbers of dividing cells and fewer cells undergoing DNA-damage–linked death, which together help explain the thickened epidermis. Immune profiling showed heavier infiltration by several immune cell types, especially a subset of T cells called γδ T cells, which are known to produce potent inflammatory cytokines in skin.
At the molecular level, Alox8 deficiency reshaped the skin’s lipid landscape. Untargeted lipidomics showed broad shifts in many lipid classes, including reductions in ceramides and sphingomyelins, molecules important for barrier structure and for restraining cell growth. At the same time, pro-inflammatory pathways revved up. Levels of cyclooxygenase-2 (Cox2), an enzyme that makes prostaglandins, rose earlier and higher in knockout mice, accompanied by increased production of prostaglandin E2. This lipid messenger is known to boost interleukin-17 production by γδ T cells, and in line with that, the knockout mice displayed elevated levels of interleukin-17 and interleukin-22, as well as chemokines that call additional immune cells into the skin.
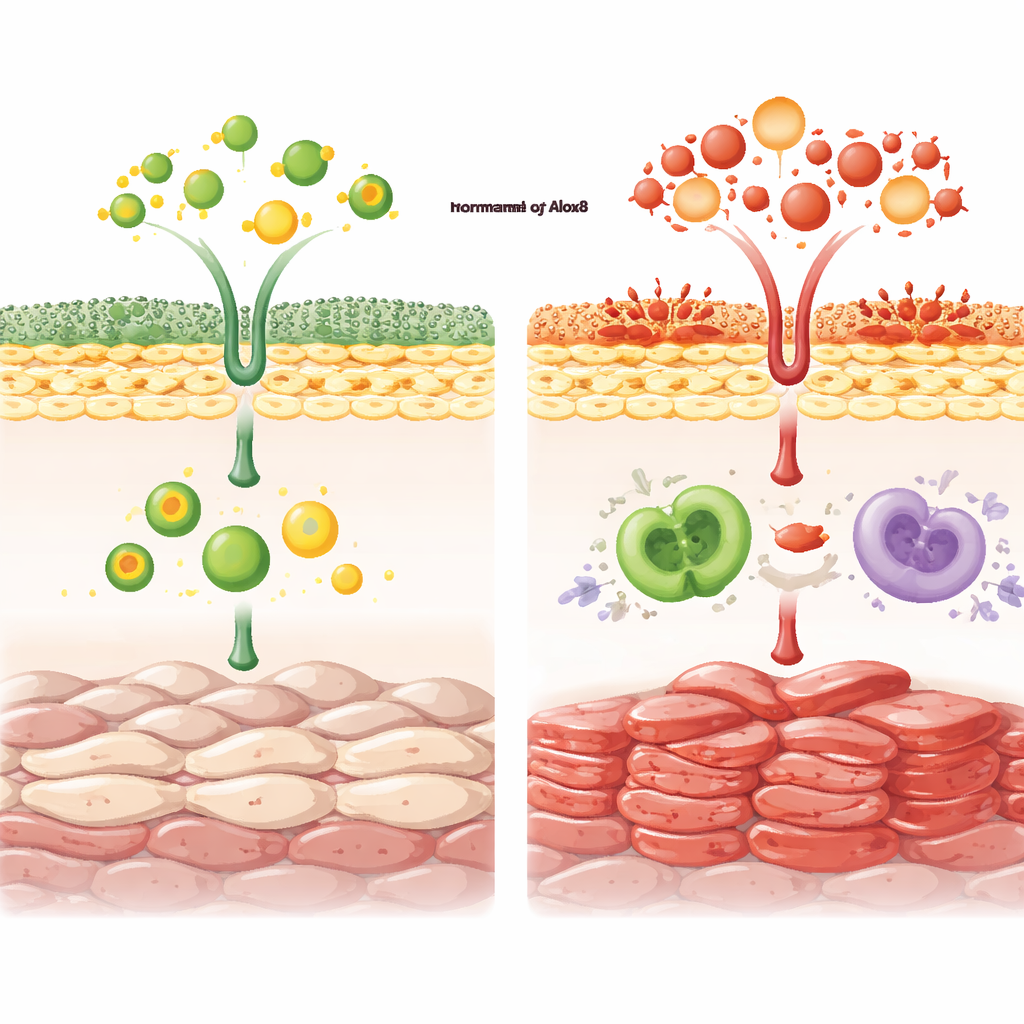
Oxidized fats: not always the villains
One intriguing finding concerned 4-hydroxynonenal, a marker of lipid peroxidation often associated with oxidative stress and cell death. In normal mice, imiquimod increased this oxidized lipid in the epidermis, but this rise was blunted in Alox8 knockouts. Despite having less of this damage marker, the knockout animals had worse disease, suggesting that some forms of controlled lipid oxidation may actually support the removal of damaged cells and help resolve inflammation. The loss of Alox8 seems to disrupt this delicate balance, reducing programmed cell death while favoring proliferation and chronic immune activation.
What this means for understanding psoriasis
Taken together, the work paints Alox8 as part of an internal braking system that helps mouse skin recover from inflammatory insults. Without this enzyme, specific lipid messengers fall, the broader lipid environment becomes disordered, and signaling through prostaglandins and T cell cytokines becomes exaggerated. The result is thicker, more inflamed skin that takes longer to calm down. While mice are not humans, and the chemistry of Alox8 and its human relative ALOX15B is not identical, the study strengthens the idea that fine-tuning lipid metabolism in the skin could be a powerful strategy to prevent or shorten psoriasis flares, and suggests that boosting the activity or products of this pathway might one day form the basis of new, locally acting treatments.
Citation: Palmer, M.A., Kirchhoff, R., Hahnefeld, L. et al. Alox8 knockout exacerbates imiquimod-induced psoriasis-like inflammation. Cell Death Dis 17, 390 (2026). https://doi.org/10.1038/s41419-026-08727-9
Keywords: psoriasis, skin inflammation, lipid mediators, immune cells, prostaglandins