Clear Sky Science · en
A perfused, parallelized blood brain barrier-tumor platform for compound permeation and efficacy investigations
Why treating brain tumors is so hard
Modern cancer drugs have improved survival for many patients, but brain tumors remain stubbornly difficult to treat. One major reason is the brain’s own security system, the blood brain barrier, which blocks most substances from entering the brain. This study describes a lab grown model that brings a realistic brain barrier and patient derived brain tumor tissue together on a miniature plastic platform, so scientists can better see which drugs actually reach tumors and how well they work once they arrive.
A tiny barrier that blocks big hopes
The blood brain barrier is a thin lining of cells that coats blood vessels in the brain and tightly controls what gets through from the bloodstream. While it protects our brains from toxins, it also keeps out many helpful medicines. This is especially problematic for children with diffuse midline glioma, an aggressive brainstem tumor with very poor survival. Existing flat cell cultures and even many three dimensional tumor models often leave out a realistic brain barrier, making drugs look more promising in the lab than they turn out to be in patients.
Building a brain barrier and tumor on a chip
To tackle this gap, the researchers built a palm sized plastic device that holds 32 miniature test units arranged like the wells of a standard lab plate. Each unit contains a narrow channel lined with human blood vessel cells, supported by brain support cells called astrocytes and pericytes embedded in a soft gel below. Together they form a compact model of the blood brain barrier. Directly underneath this barrier, the team created a tiny hanging droplet that can hold a single spherical clump of tumor cells, grown separately from cells donated by children with diffuse midline glioma. This droplet places the tumor very close to the artificial blood vessel, similar to its location in the brainstem.
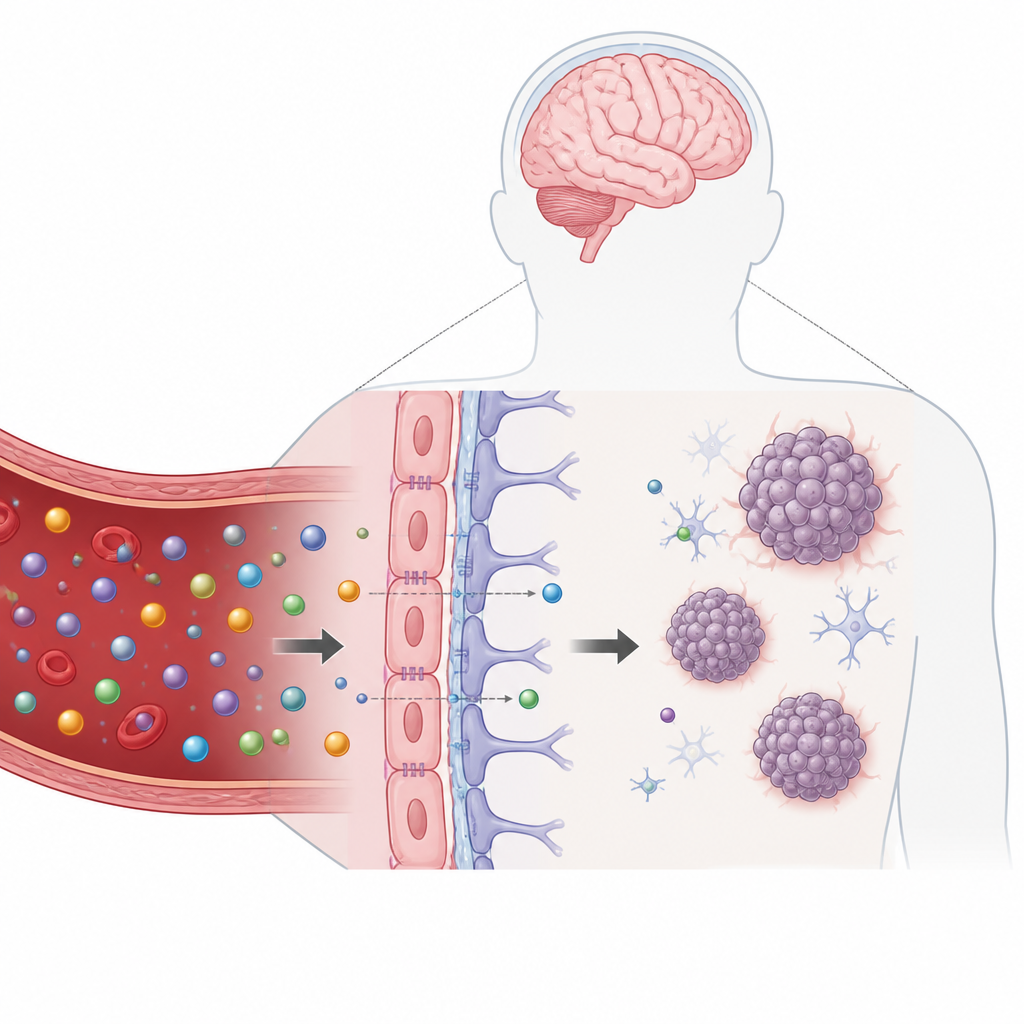
Simulating blood flow without pumps
In a living brain, vessel cells experience constant flow and gentle friction from the moving blood, which helps keep the barrier tight. To mimic this without bulky equipment, the team mounted their plate on a tilting stage inside a warm incubator. By slowly rocking the plate back and forth, they created gravity driven flow of nutrient liquid through each channel, bathing the vessel cells in realistic levels of shear stress. Computer simulations and measurements confirmed that flow and mechanical forces remained within the range expected in real brain vessels, and that the barrier stayed tight to small fluorescent test molecules.
Testing real cancer drugs in a realistic setting
With the platform established, the researchers tested four existing chemotherapy drugs that are already approved for other cancers: cisplatin, doxorubicin, homoharringtonine, and docetaxel. First, they exposed brain tumor spheroids and blood brain barrier spheroids in regular plates to a wide range of doses, finding how much of each drug killed half the cells. This helped them select doses that were harmful to the tumor cells but less damaging to the barrier itself. They then flowed these doses through the upper channel of the chip, allowing drugs to cross the barrier and reach the tumor only if they could permeate through the tight cell layer.
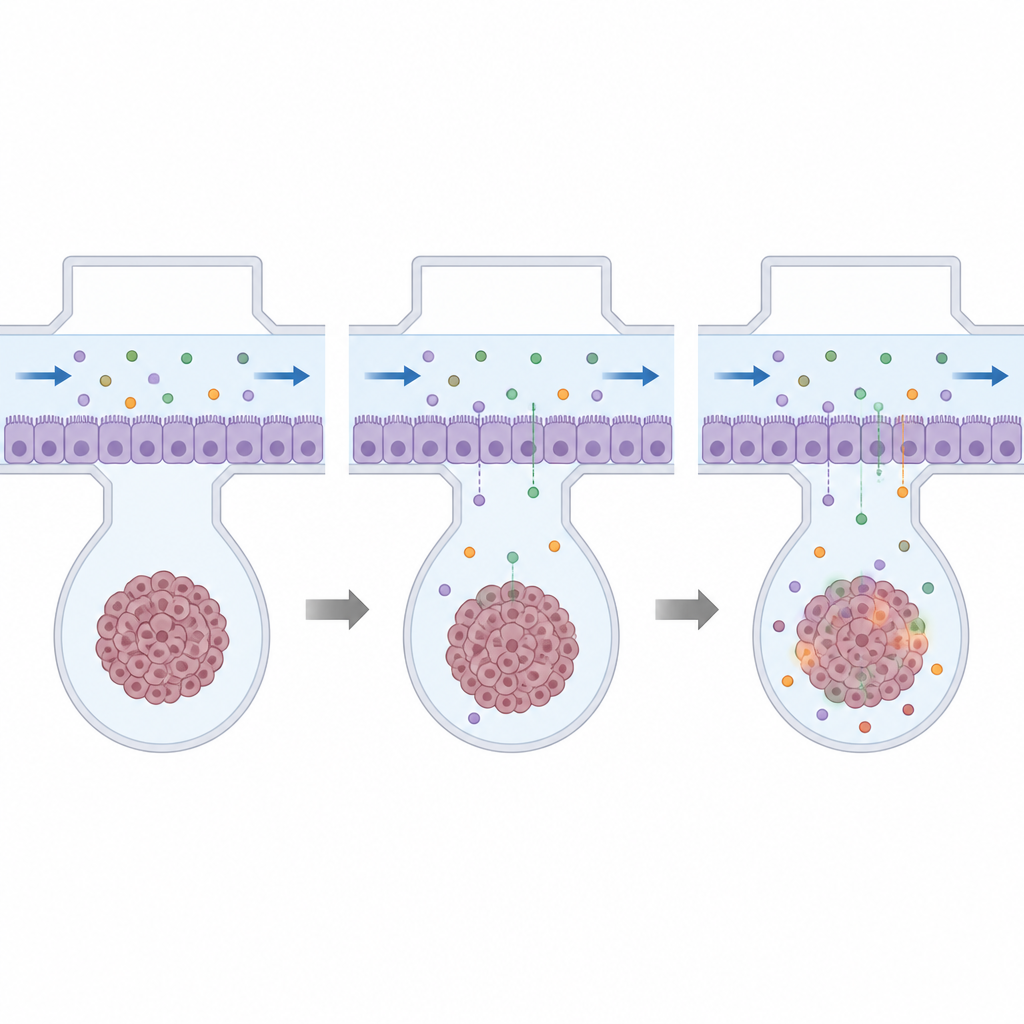
What the new platform reveals
The results showed that even when drugs were clearly toxic to tumor cells in standard dishes, the presence of an intact brain barrier on the chip sharply reduced their impact. Tumor spheroids behind the barrier lost far fewer cells than those directly bathed in drug solution, highlighting how strongly the barrier limits real drug exposure. Some drugs, such as doxorubicin and homoharringtonine, also made the barrier leakier at doses far below those that killed the barrier cells, allowing more drug to pass but also signaling potential harm to healthy brain tissue. Importantly, tumors from different patients responded differently, underlining the need for personalized testing.
Bringing personalized brain tumor testing closer
To a non specialist, the key message is that it is not enough for a cancer drug to kill tumor cells in a dish; it must also cross the brain’s protective wall without causing too much damage. This study introduces a practical, scalable tool that brings a realistic brain barrier and patient derived tumor tissue together in one miniaturized system. Because each test unit uses only a few hundred tumor cells, such platforms could one day test panels of drugs and doses on a child’s own cells before treatment, helping doctors choose options that are both more effective and safer for the brain.
Citation: Wei, W., Stano, M., Kritzer, B. et al. A perfused, parallelized blood brain barrier-tumor platform for compound permeation and efficacy investigations. Microsyst Nanoeng 12, 175 (2026). https://doi.org/10.1038/s41378-026-01268-3
Keywords: blood brain barrier, diffuse midline glioma, organ on chip, brain tumor drugs, microfluidic platform