Clear Sky Science · en
Diagnosing and defining MASLD in people living with chronic hepatitis B
Why this matters for everyday health
Two of the fastest-growing threats to liver health worldwide are a long-lasting viral infection called chronic hepatitis B and a common condition linked to weight, blood sugar, and cholesterol problems, now termed metabolic dysfunction-associated steatotic liver disease (MASLD). This review explores what happens when these two problems occur in the same person, why diagnosis is difficult, and how better tests and fairer access to care could prevent many cases of cirrhosis, liver cancer, and early death.
Two liver problems on a collision course
Chronic hepatitis B affects hundreds of millions of people and can silently damage the liver over decades, leading to scarring, cirrhosis, and liver cancer. At the same time, rising rates of obesity and diabetes have fueled an explosion of MASLD, in which fat builds up inside liver cells and can progress to inflammation and scarring. These trends increasingly overlap in regions such as Africa, the Eastern Mediterranean, and the western Pacific, where hepatitis B is common and metabolic diseases are rapidly increasing. The authors argue that this “critical nexus” will reshape the global pattern of liver disease and demands coordinated attention.
New names, shifting definitions, same patients
Until recently, fatty liver disease was often described using terms that referenced alcohol or carried stigma. In 2023, experts agreed on new language: MASLD for fat in the liver plus at least one heart–metabolism risk factor (for example high blood pressure, diabetes, abnormal blood fats, or obesity), and MASH for cases where there is both fat and active inflammation or scarring. In parallel, chronic hepatitis B care is moving toward simpler, more practical definitions focused on who needs treatment most. However, changing terminology, older studies using outdated labels, and inconsistent testing methods have made it hard to compare data and to see clearly how MASLD alters outcomes for people living with hepatitis B.
What the evidence shows so far
The review pulls together 12 systematic reviews covering 178 studies of people with both conditions. Overall, about one-third of people with chronic hepatitis B also have steatotic liver disease. Yet the reported effects of MASLD on scarring, liver cancer, and response to antiviral drugs are surprisingly mixed: some analyses find worse outcomes, others see no difference, and a few even suggest certain forms of fat in the liver might be protective. One consistent, intriguing signal is that people with MASLD appear more likely to lose hepatitis B surface antigen, a milestone sometimes called a “functional cure.” Possible explanations include death of fat-laden infected cells, changes in how viral proteins are released, and extra inflammation that may help the immune system clear infected cells, but these ideas remain speculative.
Tools for looking inside the liver without a needle
Liver biopsy—removing a small tissue sample with a needle—remains the traditional gold standard for judging how much fat and scarring is present, but it is invasive, costly, and samples only a tiny part of the organ. The field is rapidly turning to non-invasive tests: ultrasound-based devices that estimate liver stiffness and fat content, advanced magnetic resonance scans, and blood-based scores assembled from routine lab tests like liver enzymes and platelet counts. The review shows that many of these tools perform reasonably well in hepatitis B plus MASLD, but important details, such as the best cut-off values, often differ from those established in people without viral infection. In some cases, fat in the liver can make stiffness readings look worse than they are; in others, chronic hepatitis B itself shifts the thresholds at which fat or fibrosis should be called abnormal.
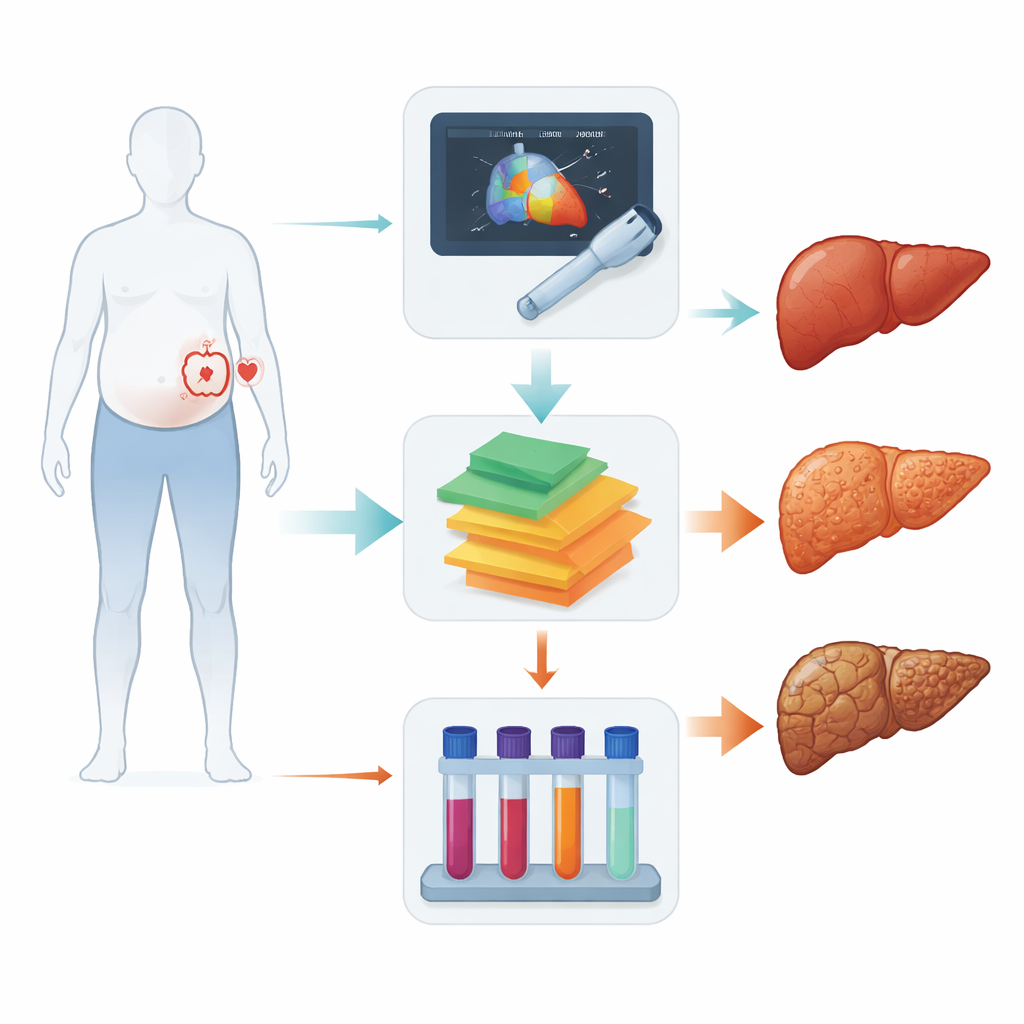
Matching tests and care to local realities
High-tech imaging such as magnetic resonance elastography is highly accurate but far too expensive and scarce for routine use in most settings where hepatitis B is common. The authors therefore emphasize practical strategies: in well-resourced clinics, pairing simple ultrasound-based stiffness and fat measurements with selected blood scores to identify people at highest risk of advanced scarring; and in resource-limited areas, relying more heavily on inexpensive scores derived from common blood tests, while acknowledging their imperfections. They sketch an example algorithm showing how a viral hepatitis clinic might screen people for metabolic risk factors, look for signs of liver fat and scarring, and decide who needs lifestyle support, closer monitoring, or specialist referral.
Bringing fairness and future therapies into focus
Beyond diagnostics, the paper highlights deep global inequities. Regions with the heaviest dual burden of hepatitis B and metabolic disease often have the weakest access to imaging devices, laboratory infrastructure, and new medicines. Meanwhile, the treatment landscape is changing quickly: guidelines are starting to treat MASLD itself as a reason to start hepatitis B antivirals earlier, and powerful new drugs for obesity and fatty liver are coming to market. To ensure these advances benefit everyone, the authors call for more inclusive research that reflects diverse populations, clearer and harmonized test thresholds, and investment in integrated care models that address viral infection, metabolism, and cardiovascular risk together.
What this means for patients and the public
For someone living with chronic hepatitis B, the message is that everyday health factors—weight, blood sugar, blood pressure, and cholesterol—matter as much to the liver as the virus itself. When these risks pile up, they can accelerate scarring and complications, but they are also treatable through lifestyle changes and, increasingly, medications. The authors conclude that the most effective path forward is not a single miracle test or drug, but a coordinated effort: clear definitions, reliable and affordable tools to measure liver damage, and health systems that can act on those findings fairly across the globe.
Citation: Martyn, E., Arenas-Pinto, A., Gilson, R. et al. Diagnosing and defining MASLD in people living with chronic hepatitis B. Commun Med 6, 273 (2026). https://doi.org/10.1038/s43856-026-01383-2
Keywords: chronic hepatitis B, MASLD, fatty liver, non-invasive liver tests, global liver health