Clear Sky Science · en
Nuclear protein 1 is a cell death regulator in primary human airway epithelial cells and reduced in idiopathic pulmonary fibrosis
Why this lung study matters
Idiopathic pulmonary fibrosis is a deadly lung disease where scar tissue gradually stiffens the lungs, making every breath harder. Many patients have a history of smoking, but scientists still struggle to understand how smoke and vulnerable airway cells team up to damage the lung. This study looks closely at a little-known stress protein inside airway cells, asking whether it helps those cells survive harm and whether its loss might leave lungs more fragile in people with fibrosis.
The lung’s frontline defenders
The airways are lined by a thin, busy sheet of cells that act as both shield and cleaning crew. Some cells grow hair-like structures that sweep mucus and dust out of the lungs, while others secrete mucus or repair damage. Because cigarette smoke is the first thing these cells encounter, the authors used fully matured human airway cells grown in the lab to see how they respond to long-term smoke exposure. They measured thousands of proteins inside the cells and used computer tools to spot which stress pathways were changing together, hoping to uncover new players in smoke-related injury.
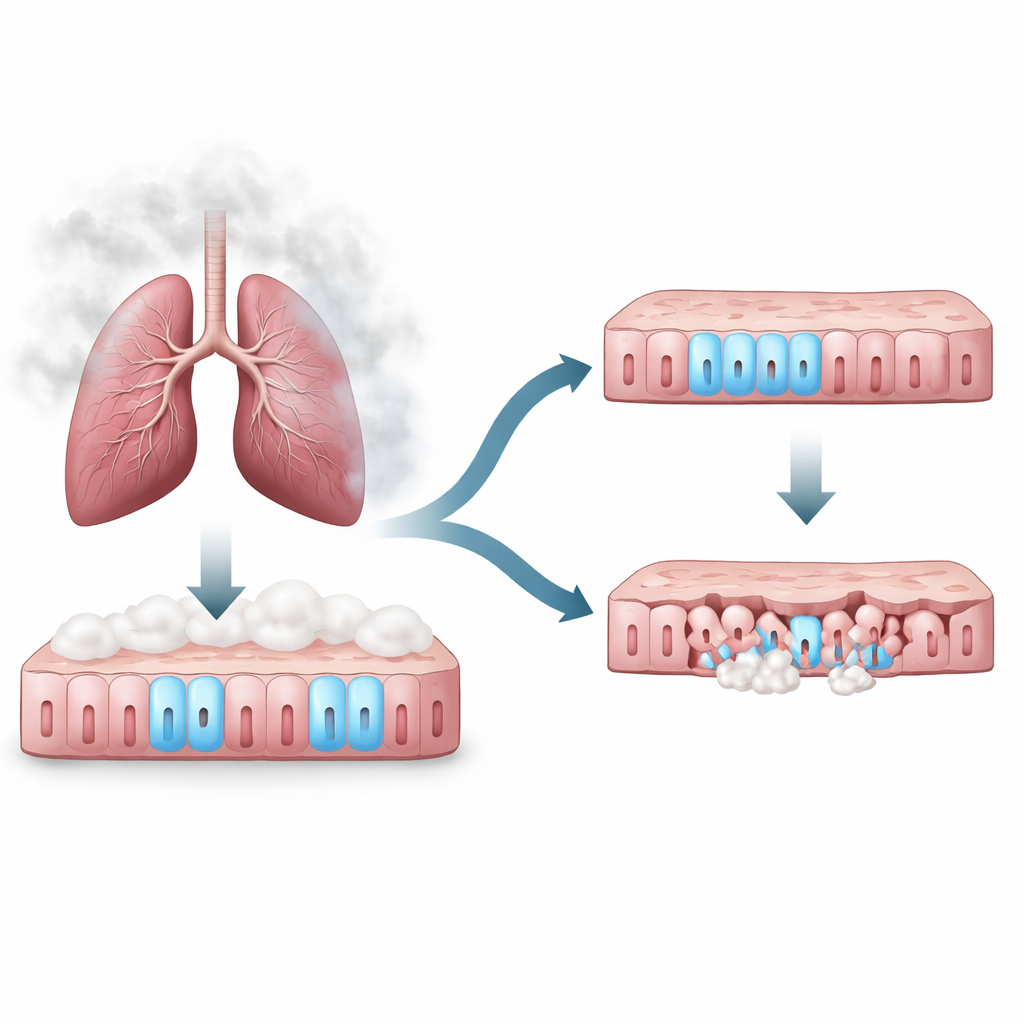
A stress protein that quietly protects
The protein that stood out was nuclear protein 1, or NUPR1, a stress response factor previously linked mostly to cancer and pancreatic disease. Computer analysis suggested that smoke should switch NUPR1 on, helping airway cells cope with damage. But when the team checked directly, they found that cigarette smoke did not reliably increase NUPR1 levels or change where it sat inside the cell. Instead, experiments with a drug that blocks NUPR1 from entering the nucleus showed that the protein itself is strongly protective. When NUPR1 was blocked, more airway cells died and the normally tight barrier between them began to leak and fall apart, even without smoke.
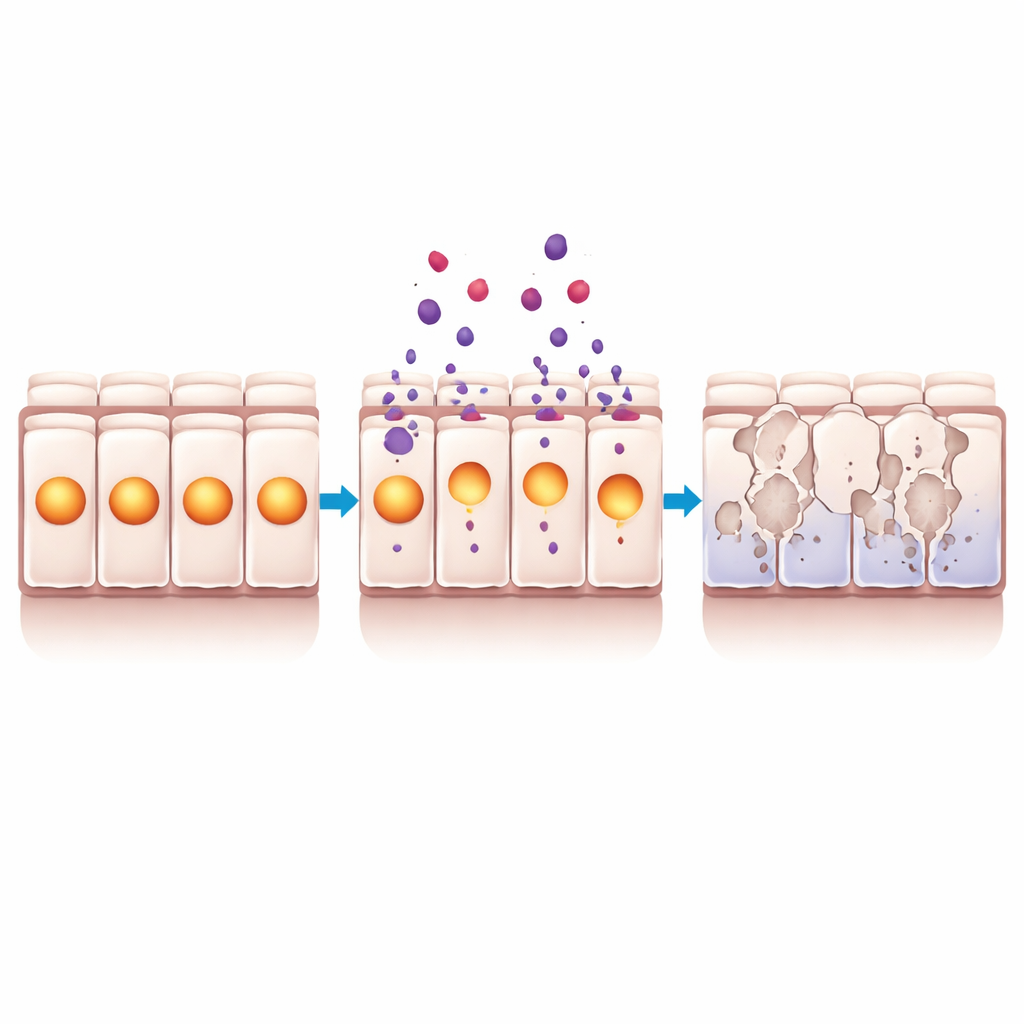
How cells die when protection is lost
Cell death can follow different routes, and earlier work had suggested that losing NUPR1 might trigger a special form of iron-driven damage called ferroptosis. To test this, the researchers measured genes and markers tied to ferroptosis, as well as general oxidative damage, in airway cells treated with the NUPR1 blocker. While some gene signals shifted, there was no convincing sign of the characteristic lipid damage that defines ferroptosis. Instead, proteins associated with classic programmed cell death rose, and the share of living cells fell. These findings point to NUPR1 acting mainly as a shield against apoptosis in airway cells, helping them weather stress without immediately self-destructing.
Fragile airways in fibrotic lungs
The team then turned to lung tissue and cells from people with idiopathic pulmonary fibrosis. Single-cell data and fluorescent staining of patient lungs showed that NUPR1 levels were lower overall, including in airway lining cells, and appeared especially reduced in current smokers. When the scientists grew airway cells taken from people with fibrosis, those cultures formed an epithelium with fewer ciliated cells and more mucus-producing cells than cultures from control donors, mirroring changes seen in diseased lungs. Strikingly, these fibrosis-derived cells were more sensitive to NUPR1 blockade: they lost barrier function and died at lower drug doses, suggesting that they depend heavily on whatever NUPR1 protection remains.
What this means for future care
Put simply, this study suggests that NUPR1 acts as a built-in survival factor that helps airway cells stay alive and keep the lung surface sealed. Cigarette smoke did not clearly boost this safeguard in lab-grown cells, yet patient data hinted that long-term smoking and fibrosis are linked to lower NUPR1 levels in the lung. Losing that protection may leave airway cells in fibrotic lungs easier to injure and quicker to die, potentially feeding the cycle of scarring. The results also raise a caution flag for cancer drugs that try to shut down NUPR1: while that approach may weaken tumors, it could also harm already stressed airway cells, especially in people with underlying lung fibrosis.
Citation: Zöller, M., Mastalerz, M., Dick, E. et al. Nuclear protein 1 is a cell death regulator in primary human airway epithelial cells and reduced in idiopathic pulmonary fibrosis. Sci Rep 16, 14728 (2026). https://doi.org/10.1038/s41598-026-51510-1
Keywords: idiopathic pulmonary fibrosis, airway epithelium, cigarette smoke, cell death, NUPR1