Clear Sky Science · en
Hypoxia or tobacco-smoke exposure induce region-specific microvascular remodeling in the brain
When Lung Disease Reaches the Brain
Chronic lung diseases such as COPD are usually thought of as problems of breathing and coughing. But the lungs are the body’s gateway for oxygen, and when they fail, many other organs can quietly suffer. This study explores how long‑lasting low oxygen or cigarette‑smoke damage in the lungs can reshape the brain’s tiniest blood vessels in specific regions, potentially helping to explain why people with severe lung disease often develop memory problems and are more prone to brain complications, including metastases from lung cancer.
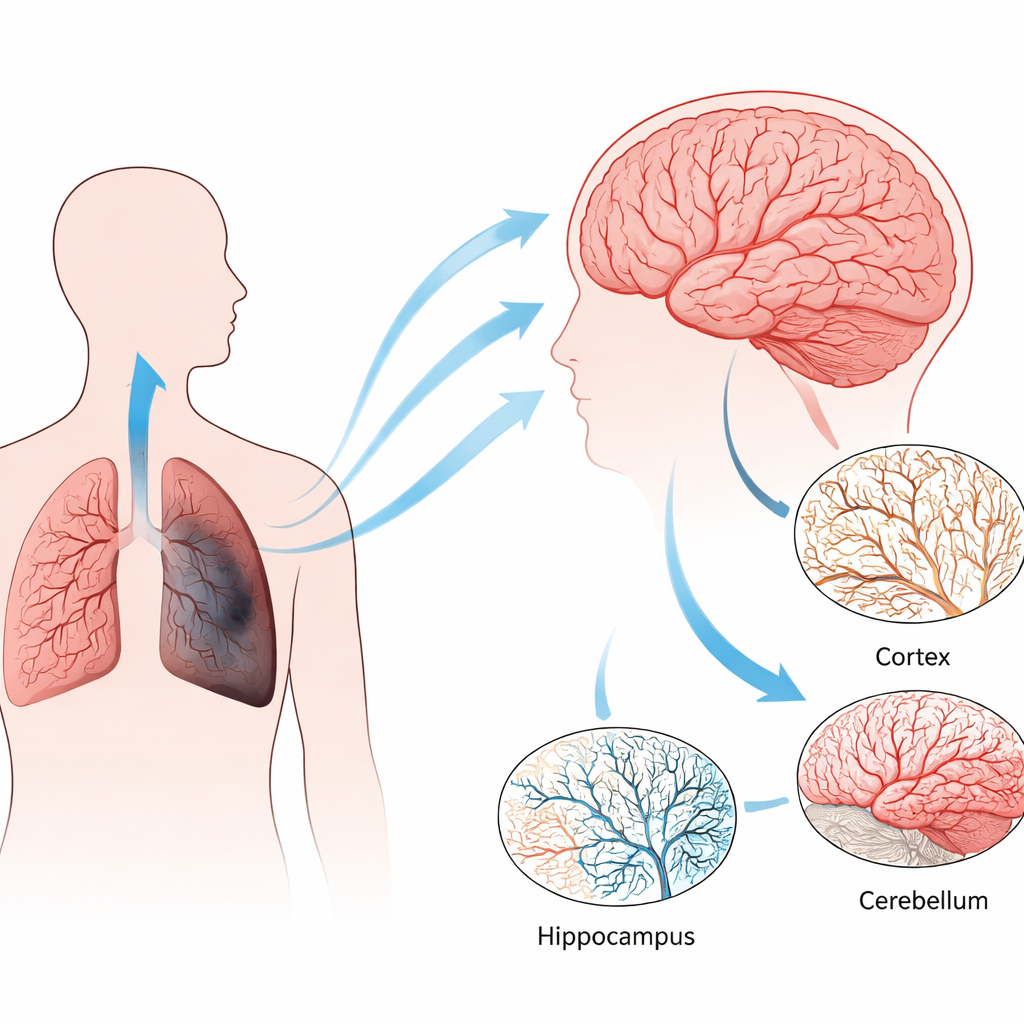
Three Ways to Stress the Lungs
The researchers used three mouse models that mimic different long‑term stresses seen in human lung disease. In one, animals were kept in mildly low oxygen, reflecting chronic hypoxia that develops when damaged lungs can no longer load enough oxygen into the blood. In the other two, mice inhaled cigarette smoke for months. A shorter exposure produced pulmonary hypertension, a dangerous rise in blood pressure in the lung’s vessels, while a longer exposure caused both pulmonary hypertension and emphysema, the classic loss of air sacs in COPD. These models allowed the team to separate the effects of low oxygen from those of smoke‑driven inflammation and damage.
Tiny Vessels, Big Regional Differences
The team then examined how the brain’s capillary network responded in key regions: the cortex (involved in thought), the hippocampus (crucial for memory), the brainstem and the cerebellum. Using fluorescent markers to label blood vessel lining cells on thin tissue slices, they measured how much area was occupied by vessels. Mild chronic hypoxia and the smoke model with emphysema both led to denser networks of tiny vessels in several regions, particularly in the hippocampus and cerebellum. In sharp contrast, the smoke model with only pulmonary hypertension showed a loss of microvessels, especially in the cortex and hippocampus. Three‑dimensional imaging of cleared, thicker brain slices confirmed these patterns, highlighting the hippocampus as the most sensitive area.
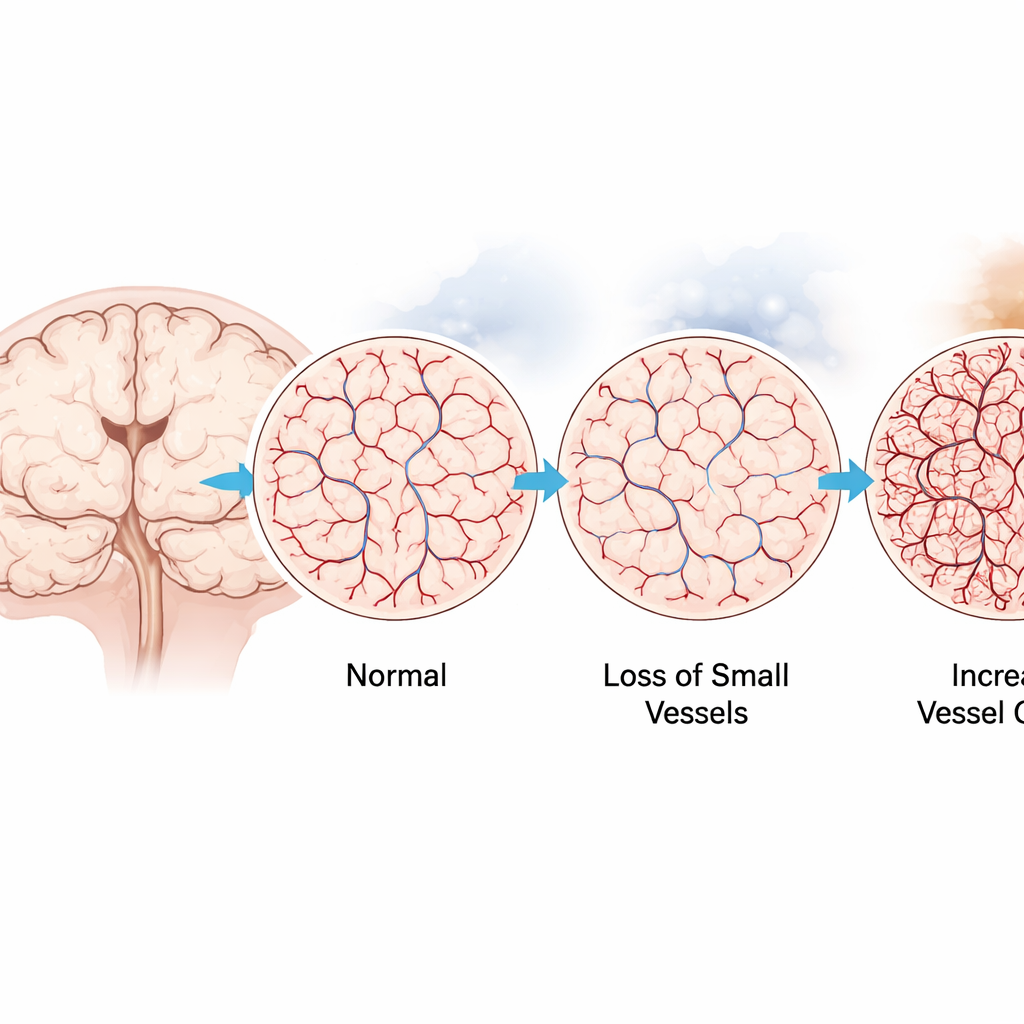
Immune Cells and Leakiness Under the Microscope
Because the brain’s resident immune cells, microglia, are known to help shape blood vessels, the researchers asked whether their numbers or spacing changed alongside the vessels. Surprisingly, they found no major shifts in microglial density or distribution at the time points studied, suggesting that any immune‑driven remodeling is either brief or too subtle for standard counting methods. They also looked for signs that the blood–brain barrier was leaking by tracking fibrinogen, a blood protein that normally stays inside vessels and rises in systemic inflammation. In both two‑ and three‑dimensional images, fibrinogen largely remained confined within vessels, pointing to remodeled but largely sealed capillary networks rather than overt breakdown.
Signals in the Blood and in the Brain
To probe the chemical signals behind these structural changes, the team measured fibrinogen and the enzyme MMP‑9 in blood plasma and brain tissue. In smoke‑exposed mice, circulating fibrinogen was higher, echoing findings in people with COPD, but this did not translate into clear accumulation inside the brain. In the low‑oxygen model, systemic fibrinogen stayed relatively stable, yet brain tissue showed higher fibrinogen levels, consistent with local deposition within growing vessels rather than leakage into brain tissue. MMP‑9, mostly present in its inactive form, was elevated in the blood during chronic hypoxia, while its natural blocker TIMP‑1 did not change, hinting that any role for this enzyme in reshaping brain vessels is likely controlled at specific sites rather than across the whole circulation.
Why These Changes Matter
Taken together, the experiments reveal that chronic lung problems can remodel the brain’s microcirculation in region‑specific ways that depend on the type and duration of stress. Some conditions thin out the capillary bed, while others promote extra vessel growth, with the hippocampus emerging as a key hotspot. Although this work was done in mice and does not directly track tumors, it supports the idea that long‑term lung disease can quietly prepare the brain’s landscape—through altered blood flow, vessel structure and inflammatory cues—in ways that might influence cognition and even how easily cancer cells can take hold. Understanding these hidden lung–brain connections could eventually guide strategies to protect vulnerable brain regions in people living with chronic lung disease.
Citation: Salik Demirtas, N., Loku, E., Porschen, Y. et al. Hypoxia or tobacco-smoke exposure induce region-specific microvascular remodeling in the brain. Sci Rep 16, 12722 (2026). https://doi.org/10.1038/s41598-026-45975-3
Keywords: COPD, brain blood vessels, chronic hypoxia, tobacco smoke, lung–brain axis