Clear Sky Science · en
Cervical cancer screening coverage and care cascade in Tamil Nadu, India, based on a community-based cross-sectional survey
Why this study matters for women’s health
Cervical cancer is one of the few cancers that can often be prevented through regular screening, yet many women never get tested. This study looks at how well women in Tamil Nadu, a large state in southern India, are being reached by screening services and what happens after a woman gets a positive test. The findings highlight both encouraging signs and serious gaps that matter for any reader interested in how health systems protect women from preventable cancers.
Checking how many women are reached
The researchers carried out a state-wide health survey between December 2023 and March 2024, visiting households in all 38 districts of Tamil Nadu. Using a structured sampling method, they interviewed 4,184 women aged 30 to 69 years about whether they had ever been screened for cervical cancer, where they were tested, and what happened afterward. They also collected basic information such as age, education, marital status, place of residence, and history of conditions like high blood pressure and diabetes, and used statistical methods that account for the survey’s complex design.

How few women get screened
The survey showed that only about 10 percent of women had ever been screened for cervical cancer in their lifetime, even though national guidelines advise screening all women from age 30 onward. Tamil Nadu’s coverage is higher than the Indian national average, but still far below the World Health Organization’s target of screening at least 70 percent of women at key ages. Most screened women were tested within the past five years, and more than half used private health facilities rather than government clinics, especially in cities. Screening was more common among women aged 45 to 59 years, among those with schooling beyond eighth standard, and among women who already knew they had diabetes.
What happens after a positive test
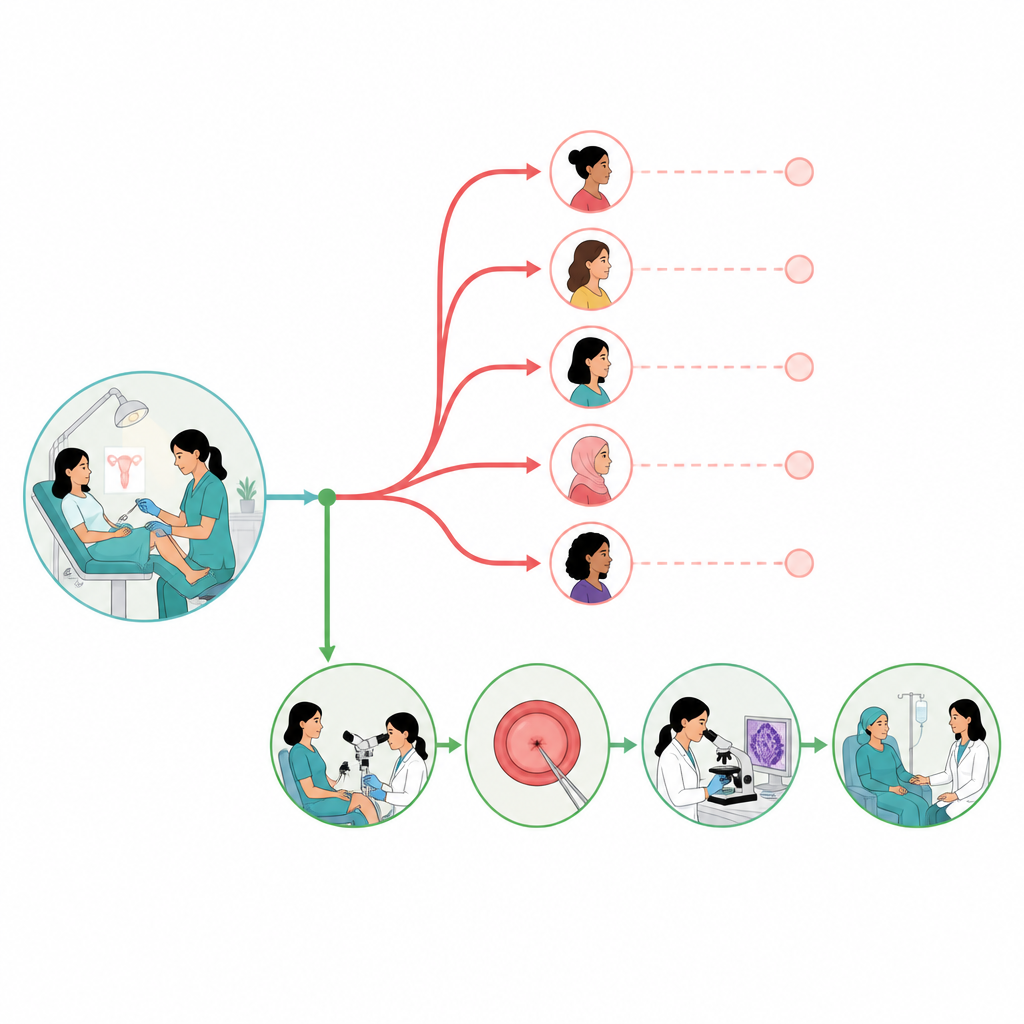
The study also traced what the authors call the “care cascade” the series of steps a woman should move through after a positive screening test. Among the 423 women who had ever been screened, 108 reported a positive result. Of these, a little over half said they were referred for a closer examination using a colposcope, and nearly all who were referred actually reached the referral center and completed the examination. Further along the pathway, some women had abnormal findings on this exam, some went on to have a tissue sample taken, and one woman in the survey reported being diagnosed with cervical cancer. By keeping the total number of screened women as the reference point, the researchers showed clearly how many were lost at each stage.
Why many women are missed
When asked why they had never been screened, nearly four out of five women said they did not feel the need because they felt healthy. Smaller groups said they did not know where to go or had no time. Among women who did get screened, most said it was because a health worker advised it or because it was part of a routine checkup. The authors also studied patterns across districts using maps and found only limited geographic clustering, suggesting that differences in local program implementation rather than broad regional trends may explain why some areas do better than others. Private clinics played a large role in providing screening, which raises challenges for tracking results and ensuring consistent quality because national programs mainly monitor government facilities.
Where the system is leaking
The biggest drop in the care pathway occurred at the point where women with a positive screening result should be referred for colposcopy. Many women reported that they were simply not advised or sent for this crucial follow-up, pointing to weaknesses in how health workers communicate and arrange referrals. Past research has linked clear, supportive conversations between providers and patients to better uptake of cancer screening, and this study reinforces that message. The authors also note likely obstacles such as travel distance, cost, time away from work, and family support, although these were not measured in detail here.
What this means going forward
For a lay reader, the main message is that Tamil Nadu’s health system is catching only a small fraction of women who could benefit from cervical cancer screening, and some of those who do test positive are not guided all the way to diagnosis and care. Improving awareness that screening is needed even when a woman feels well, strengthening advice and referral from health workers, and better involving private clinics in reporting and follow-up could help close these gaps. The study suggests that focused communication with younger women and those with little or no formal schooling, together with better training and support for providers, will be important steps toward making preventable cervical cancer deaths far less common.
Citation: Sakthivel, M., Ramalingam, A., Chadwick, J. et al. Cervical cancer screening coverage and care cascade in Tamil Nadu, India, based on a community-based cross-sectional survey. Sci Rep 16, 15131 (2026). https://doi.org/10.1038/s41598-026-45005-2
Keywords: cervical cancer screening, Tamil Nadu, women’s health, cancer prevention, care cascade