Clear Sky Science · en
3D imaging contribution in pediatric surgical oncology: a multi-stakeholder assessment study
Seeing Inside the Body in Three Dimensions
When a child needs surgery for a tumor deep in the pelvis, families and doctors face decisions that are both urgent and frightening. Yet the medical images used to guide these operations usually appear as flat black‑and‑white slices that can be hard to interpret—even for surgeons, and especially for parents. This study explores whether lifelike three‑dimensional (3D) models built from MRI scans can make pelvic tumors and surrounding organs easier for everyone to understand, from families in the clinic to senior surgeons in the operating room.
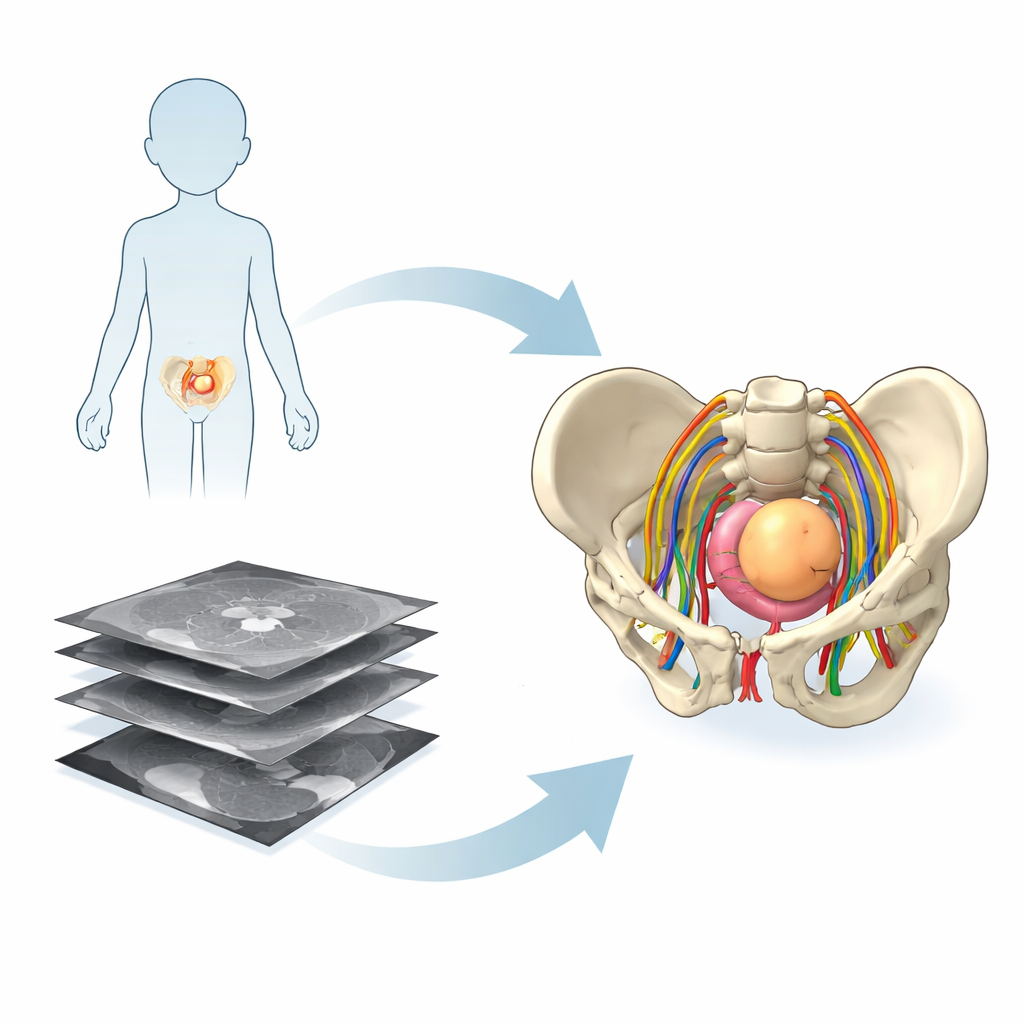
From Flat Slices to 3D Models
Traditional scans such as MRI show the body as a stack of thin two‑dimensional images. Radiologists are trained to mentally assemble these slices into a 3D picture, but this mental “puzzle‑building” is demanding, particularly in the crowded anatomy of a child’s pelvis where nerves, blood vessels, bladder, rectum, bones, and tumor all compete for space. The research team in France used advanced image‑processing and artificial‑intelligence tools to turn standard MRI and a special nerve‑mapping sequence into patient‑specific 3D models. These models included not only bones and organs, but also the delicate nerve fibers that are crucial for preserving bladder, bowel, and leg function after surgery.
Voices from Patients, Trainees, and Experts
To understand how useful these 3D models might be in real life, the investigators surveyed three groups across France: adults without medical training, surgical trainees and a few non‑surgical doctors, and experienced pediatric surgeons. All participants watched short video presentations of five real cases of pelvic tumors in children. Each case was shown twice—first with conventional 2D MRI images and then with 3D reconstructions, or vice versa in random order. After each format, viewers rated how well they felt they understood the anatomy, the surgical goals and risks, and, for non‑experts, how reassured or anxious the images made them feel.
Clearer Pictures, Better Understanding
Across all three groups, self‑reported understanding improved markedly when 3D images were used. People without medical training moved from mid‑range scores with 2D scans to near‑top scores with 3D models, especially for grasping what the disease was, what surgeons planned to do, and what complications might arise. Importantly, seeing more detail did not increase their anxiety; instead, they reported feeling more reassured. Trainees also reported clearer views of key structures—vessels, nerves, and tumor borders—and a stronger sense of how the operation would proceed. Senior surgeons, who already scored highly with 2D images, still reported meaningful gains in planning operations, judging risks, picturing the anatomy before and during surgery, and talking with families about what to expect.
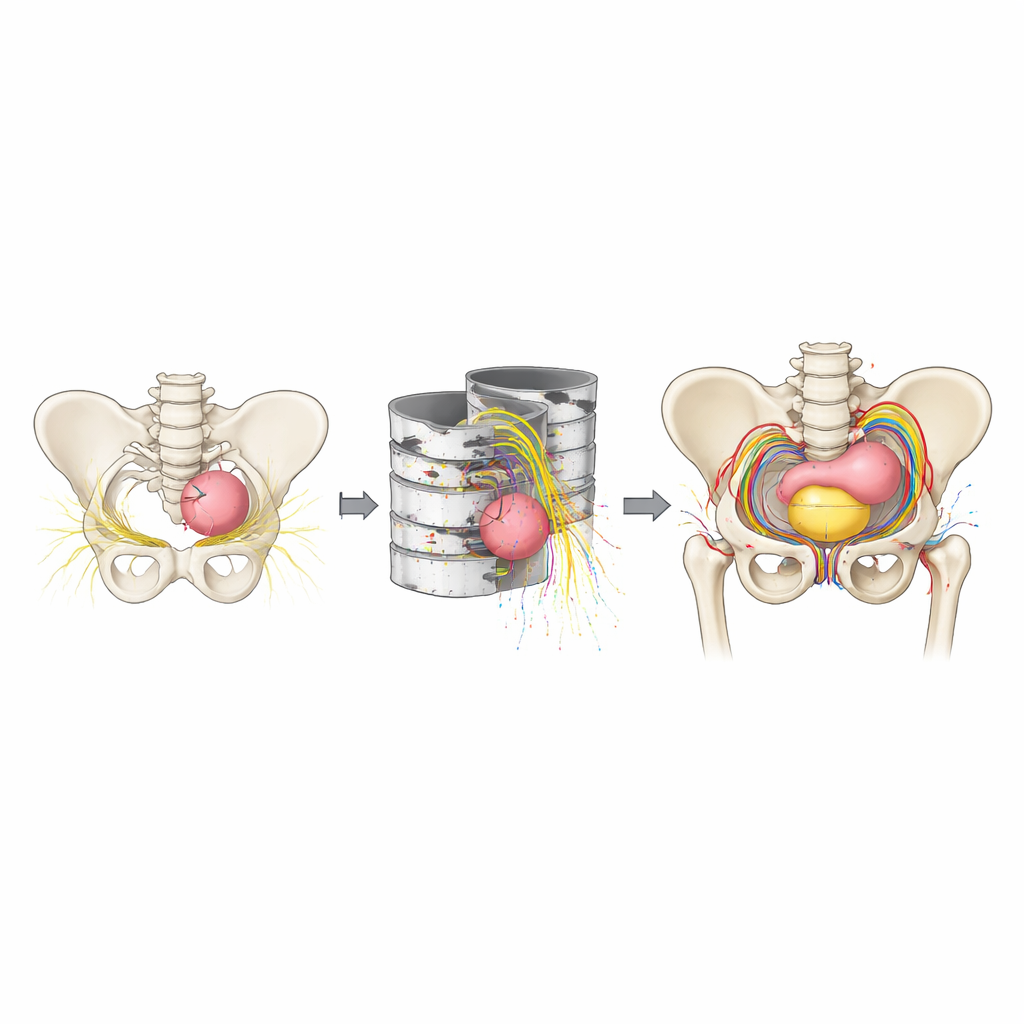
Leveling the Field in the Operating Room
An intriguing pattern emerged when the researchers compared groups. With 2D imaging alone, trainees and senior surgeons reported similar confidence in recognizing pelvic anatomy, even though real‑world experience differs greatly between them. With 3D models, scores for all three groups—from laypeople to experts—rose and converged toward similarly high levels. The authors suggest that 3D visualization may act as a kind of “common language,” shrinking the gap between novices and experts and making conversations among families, trainees, and surgeons more grounded in a shared mental picture of the child’s anatomy. Surgeons also expressed strong willingness to learn and adopt this technology, especially as newer automated tools have lowered the time and cost of generating such models.
What This Means for Children and Their Families
The study shows that people perceive 3D models of pediatric pelvic tumors as clearer and more helpful than standard flat images for understanding anatomy, planning surgery, and communicating risks and goals. However, the authors stress that these results are based on questionnaires, not on hard clinical outcomes: the study did not measure whether operations were actually safer, faster, or more precise. Future research will need to test whether using 3D imaging changes complication rates, nerve preservation, or recovery, and whether the added expense is justified. For now, the work offers encouraging evidence that turning complex scans into intuitive 3D pictures could make difficult conversations and delicate operations a little more understandable—and perhaps, in time, a little safer—for children with pelvic tumors.
Citation: Pio, L., Kassir, R., La Barbera, G. et al. 3D imaging contribution in pediatric surgical oncology: a multi-stakeholder assessment study. Sci Rep 16, 14264 (2026). https://doi.org/10.1038/s41598-026-44543-z
Keywords: 3D medical imaging, pediatric cancer surgery, pelvic tumors, surgical planning, patient education