Clear Sky Science · en
Varying patterns of association between cortical large-scale networks and subthalamic nucleus activity in Parkinson’s disease
Why this brain study matters
Parkinson’s disease is best known for its shaking and slowness of movement, but beneath these symptoms lies a problem of faulty communication in the brain. Doctors can already listen in on deep brain activity during surgery, yet they would prefer to read these signals from the outside, using non-invasive methods like brain scans. This study asks a simple but powerful question: can patterns of activity measured from the surface of the brain reveal what is happening deep inside a tiny region called the subthalamic nucleus, which plays a key role in Parkinson’s disease?
Looking at deep and surface brain signals together
The researchers recorded brain activity from 27 people with Parkinson’s disease who had recently received deep brain stimulation electrodes. While the patients sat quietly with eyes open, the team measured two kinds of signals at the same time: magnetoencephalography (MEG), which detects fast activity from across the outer brain surface, and local field potentials from the subthalamic nucleus deep inside the brain. Each person was tested both after stopping their Parkinson’s medication and again after taking their usual dose of a fast-acting drug. This design let the team see how brain communication patterns changed with and without medication.
Hidden networks that flicker in and out
Instead of treating the outer brain as one uniform area, the scientists used a mathematical method called a hidden Markov model to uncover networks of regions that tend to become active together for short bursts of time. These networks, previously mapped in healthy people, include a “sensorimotor” network involved in movement and a “default mode” network linked to inward-focused thought. By sliding through the recordings millisecond by millisecond, the model identified when each network was most active and how much time each person’s brain spent in these different patterns.
Deep brain rhythms tied to specific networks
When the team compared these network bursts with activity in the subthalamic nucleus, clear links emerged. During activations of the sensorimotor network, the subthalamic nucleus showed stronger rhythmic activity in the beta range, a frequency band already known to be exaggerated in Parkinson’s disease and associated with brief “beta bursts.” These periods also showed tighter synchrony between the subthalamic nucleus and a movement-related region called the supplementary motor area. The default mode network told a different story: its activations were paired with lower-frequency rhythms in the subthalamic nucleus and increased synchrony at slower speeds, suggesting a distinct functional state that may relate more to non-motor aspects of the disease.
Medication effects depend on brain state
The researchers then examined how Parkinson’s medication altered these deep rhythms. On average, medication reduced beta activity in the subthalamic nucleus, in line with earlier studies. But when they looked through the lens of the large-scale networks, a more nuanced picture appeared. The strongest medication-related reductions in beta power occurred during network states that did not show especially strong coupling between the subthalamic nucleus and motor areas. In contrast, the sensorimotor and default mode networks, where deep and surface areas communicated most tightly, were less clearly affected. An independent dataset from another research group largely confirmed the core finding that particular networks are linked to distinct deep brain rhythm patterns, even though the medication effects were weaker there.
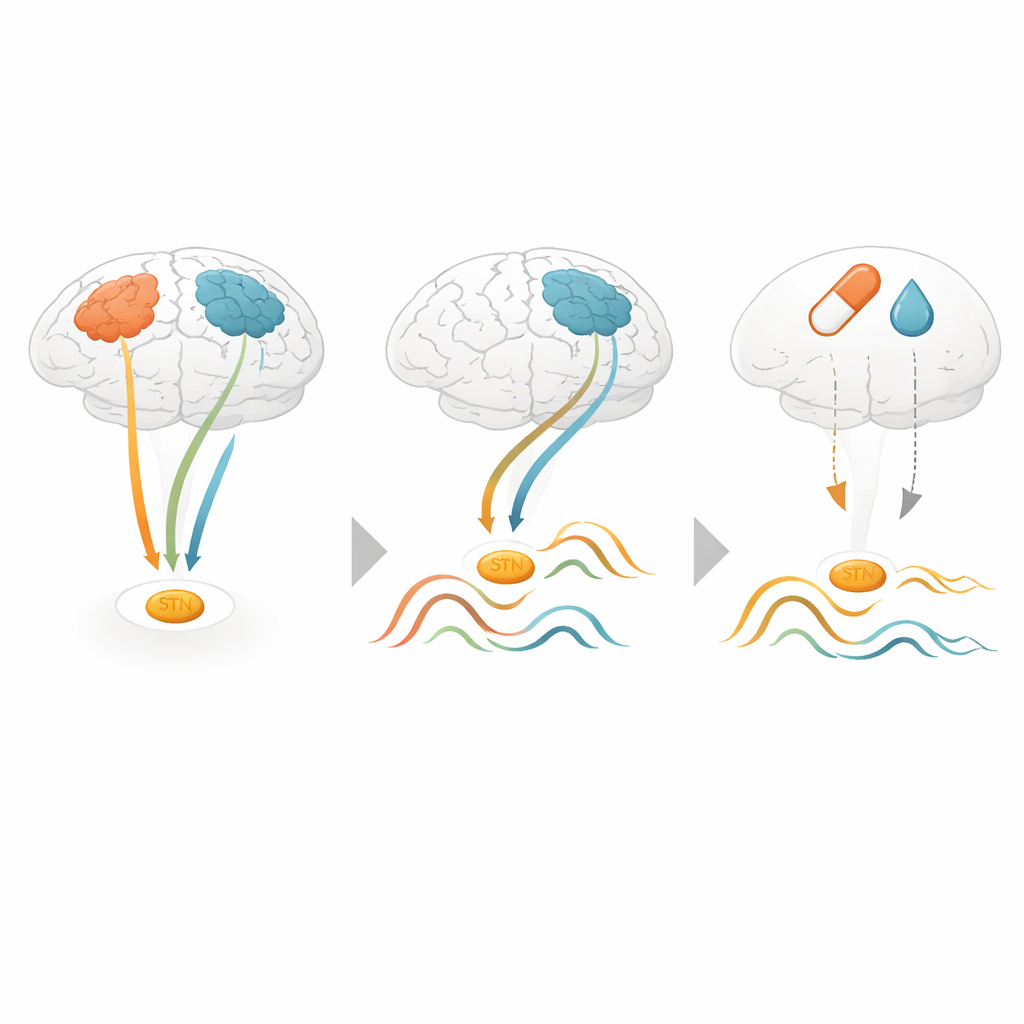
What this means for future treatment
For a lay reader, the key message is that the brain does not sit in one constant Parkinson’s state. Instead, it flips between different large-scale patterns, and each pattern lines up with a particular “mood” of the deep structure targeted by surgery and drugs. Because these patterns can be detected non-invasively from the brain surface, they could eventually serve as external markers to guide diagnosis, monitor disease progression, or trigger adaptive deep brain stimulation only when harmful rhythms appear. In this way, reading the language of brain networks may open new windows into the hidden workings of Parkinson’s disease and help clinicians tailor treatments to the brain’s moment-to-moment needs.
Citation: Kohl, O., Gohil, C., Sure, M. et al. Varying patterns of association between cortical large-scale networks and subthalamic nucleus activity in Parkinson’s disease. npj Parkinsons Dis. 12, 106 (2026). https://doi.org/10.1038/s41531-026-01372-1
Keywords: Parkinson’s disease, brain networks, deep brain stimulation, beta rhythms, magnetoencephalography