Clear Sky Science · en
The role and possible mechanism of intestinal fungi in the progression of chronic liver diseases
Hidden partners in gut health
Most people have heard that gut bacteria can affect everything from digestion to mood. Far fewer know that another cast of tiny residents—fungi—also live in our intestines and may quietly shape the fate of our liver. This review article explores how these often‑ignored gut fungi change in different chronic liver diseases and how their products can either protect the liver or drive it toward scarring and cancer. Understanding this relationship could open up new ways to diagnose, prevent, and treat some of the world’s deadliest liver conditions.
The small community with big influence
Although fungi make up only a tiny fraction of the gut microbiome, they are genetically diverse and interact closely with our immune and metabolic systems. In healthy people, a balanced mix of fungal groups lives along the digestive tract, with different species favoring different regions and niches, such as the gut lining versus the open lumen. Diet, medications, geography, and lifestyle all shape this community. Because so many of these factors also change in liver disease, the authors stress that careful study design is needed to tease apart what fungi are truly doing, rather than simply reflecting illness or treatment.
When balance breaks in liver disease
Across several chronic liver diseases—alcohol‑related liver disease, fatty liver linked to metabolic problems, autoimmune bile‑duct disease, cirrhosis, and liver cancer—a common theme emerges: helpful fungi decline while potentially harmful ones bloom. In people who drink heavily, species such as Candida albicans often expand while friendly yeasts like Saccharomyces shrink, and these shifts track with disease severity and survival. Similar patterns of fungal imbalance appear in metabolic dysfunction–associated steatotic liver disease, where certain molds and yeasts correlate with liver fat, scarring, and inflammation. In autoimmune bile‑duct disorders and cirrhosis, increases in Candida and related species are linked with worse infections, earlier need for transplantation, and higher death rates. Even in liver cancer, the mix of gut fungi shifts toward Candida and Malassezia, while protective species fade.
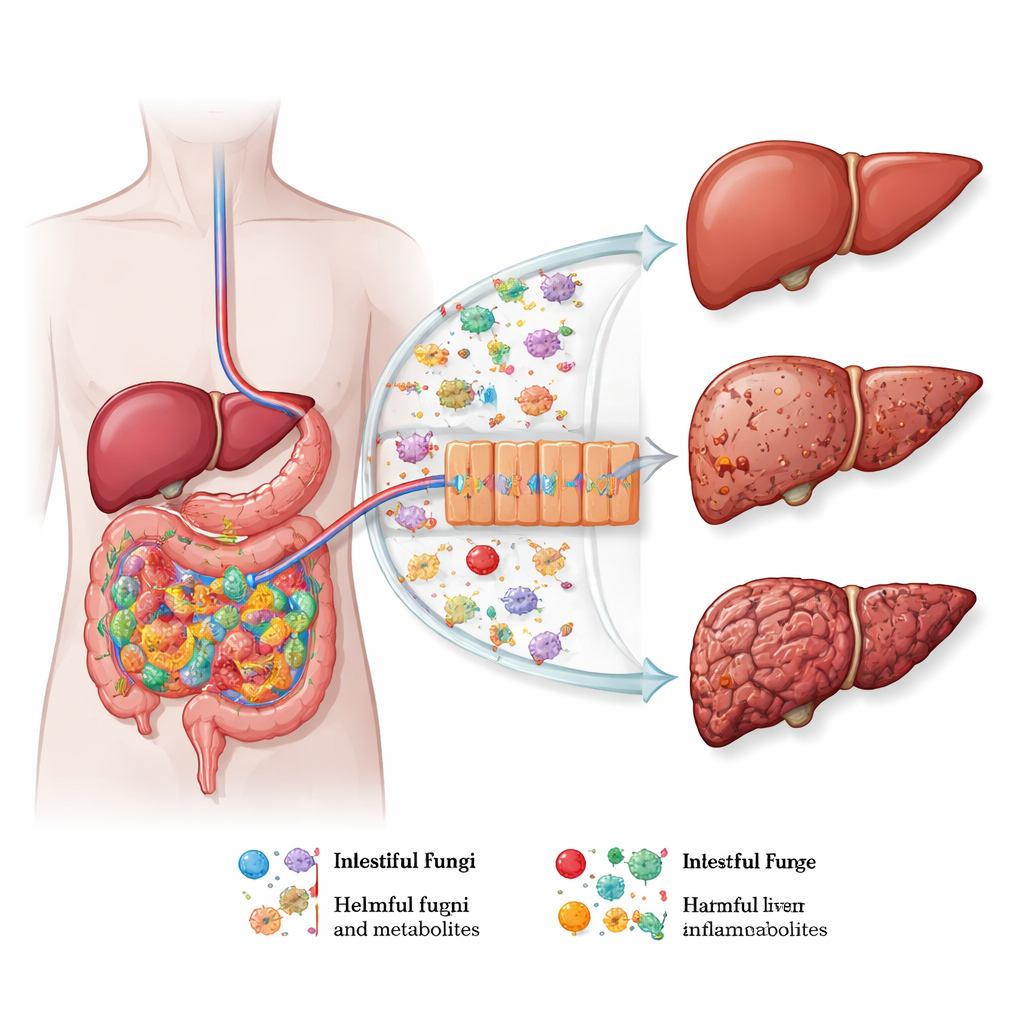
How gut fungi talk to the liver
The review outlines several routes by which intestinal fungi can influence liver health. When the gut barrier is weakened—by alcohol, fatty diets, or inflammation—fungal cells and fragments can slip into the bloodstream draining to the liver. There, specialized immune sensors on liver cells recognize fungal sugars such as beta‑glucans or other cell‑wall components and switch on inflammatory signaling pathways. Fungal toxins like candidalysin, produced by Candida albicans, can directly kill liver cells, while fungal fats, alcohol, prostaglandins, and carcinogens such as aflatoxin worsen fat buildup, scarring, or cancer risk. These signals also shape the activity of immune cells that promote a specific type of inflammation associated with tissue damage and fibrosis.
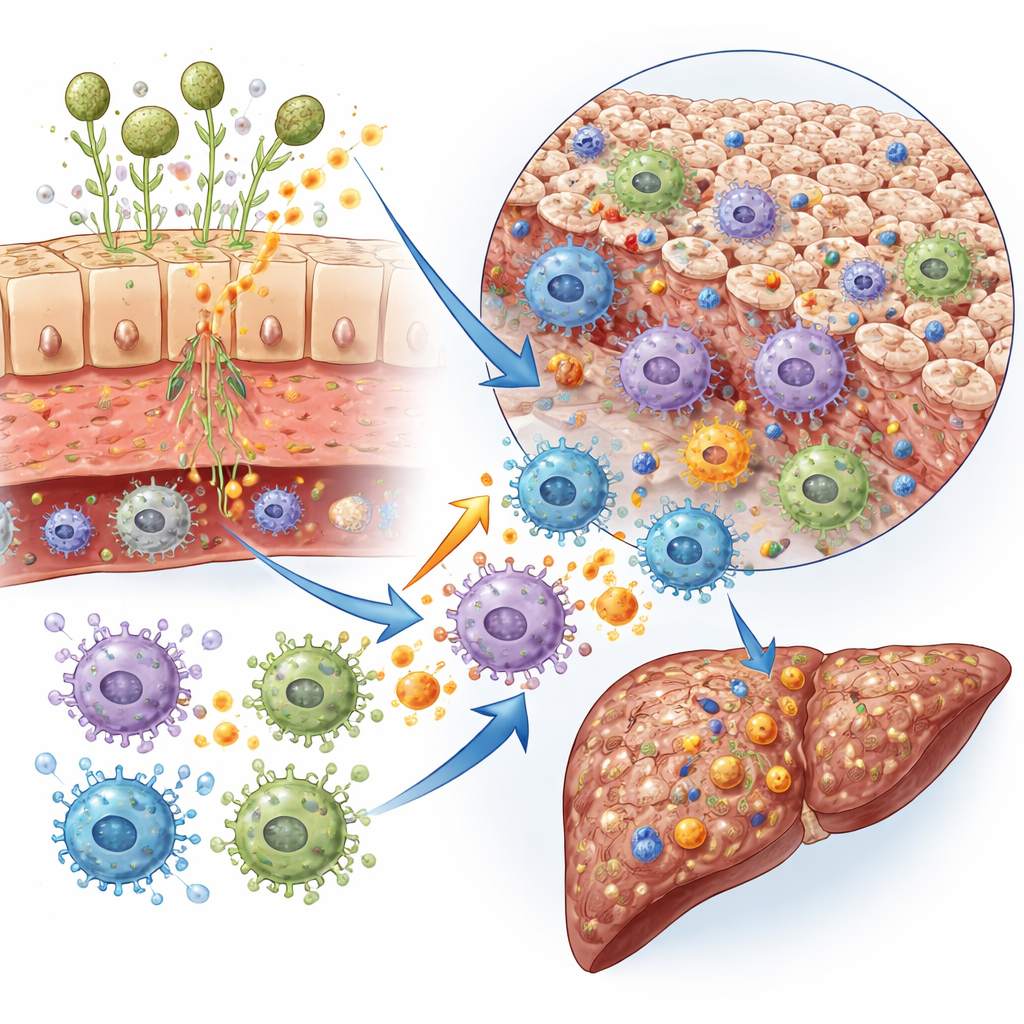
Fungal teamwork and future treatments
Gut fungi do not act alone. They form tight alliances and rivalries with gut bacteria, exchanging metabolites that can either fuel fungal growth or keep it in check. Some bacteria help tame aggressive fungi, while certain fungi can shield or support harmful bacteria. Because of this web of interactions, therapies that reshape the fungal community—such as probiotics, antifungal drugs, fecal microbiota transplants, or diet changes—may influence liver disease in complex ways. Early animal and small human studies suggest that specific probiotic yeasts, targeted antifungals, or carefully chosen microbiome donors can ease liver inflammation and fat accumulation, but they also reveal risks like drug toxicity or dangerous infections if the balance swings too far.
Why this matters for patients
The authors conclude that gut fungi are not mere bystanders in liver disease but active players that can either speed damage or offer protection. A recurring villain is Candida albicans and its toxin candidalysin, which appears across multiple liver conditions and is closely tied to poor outcomes, making it an attractive target for future drugs or antibodies. Yet the field is still young: many studies are small, use differing methods, and do not fully control for diet, medications, or immune status. To turn fungal signatures into reliable tests or treatments, large, long‑term studies are needed, along with new tools that can track how fungi, bacteria, and viruses interact over time. If successful, this work could add a powerful new lever—our gut mycobiome—to the prevention and treatment of chronic liver disease.
Citation: Hu, Y., Yang, Y., Wang, S. et al. The role and possible mechanism of intestinal fungi in the progression of chronic liver diseases. npj Biofilms Microbiomes 12, 86 (2026). https://doi.org/10.1038/s41522-026-00961-5
Keywords: gut fungi, chronic liver disease, Candida albicans, microbiome, alcohol and fatty liver