Clear Sky Science · en
Periodontitis induces skeletal muscle atrophy by increasing circulating levels of activin A.
Why your gums might matter to your muscles
Most people think of gum disease as a problem limited to the mouth—sore, bleeding gums and maybe loose teeth. This study suggests something far more surprising: chronic gum infection, known as periodontitis, can quietly weaken your muscles throughout the body. By tracing a chemical signal that travels from inflamed gums into the bloodstream and on to muscle tissue, the researchers reveal a hidden link between oral health and the strength needed for everyday activities like walking, climbing stairs, or simply getting out of a chair.
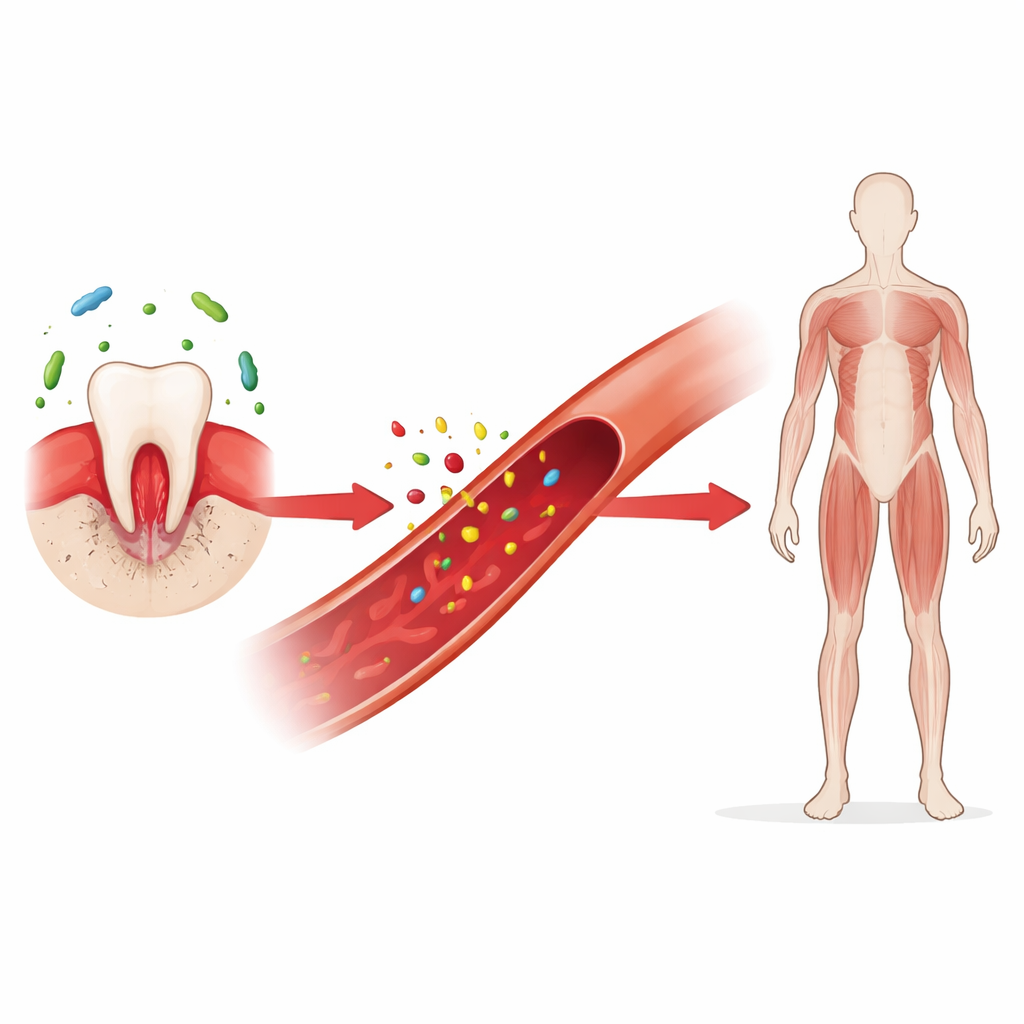
From sore gums to body-wide changes
To explore this connection, scientists used a well-established mouse model of periodontitis in which a tiny thread is tied around a tooth, encouraging bacterial overgrowth and gum inflammation. Within just two weeks, the animals showed clear loss of both muscle and bone mass, even though their food intake and fat mass stayed normal. This meant the animals were not simply eating less; something about the gum disease itself was driving tissue loss. Muscle weights fell, individual muscle fibers became thinner, and grip strength declined. At the same time, the spongy, inner portions of bones weakened, making them more fragile during mechanical testing.
A hidden messenger in inflamed gums
The researchers then hunted for substances produced in diseased gums that could circulate through the blood and trigger muscle wasting. By analyzing gene activity in gum tissue, they pinpointed one standout candidate: activin A, a protein already known to cause muscle shrinkage in conditions such as cancer-related wasting. In mice with periodontitis, the gene for activin A was turned on strongly in several gum cell types—fibroblasts that build connective tissue, surface epithelial cells lining the mouth, and immune cells that flood into the inflamed area, as well as bone-resorbing cells near the tooth socket. Blood tests showed that levels of activin A in the circulation rose rapidly after gum disease was induced, peaking while inflammation and bone loss were most active.
How a gum signal shrinks muscle
Rising activin A in the blood is only part of the story; it must also act on muscle. The team showed that when activin A increased, signaling pathways inside muscles switched on, including a molecular switch called SMAD3 and genes that tag muscle proteins for breakdown. To prove that gum-derived activin A alone was enough to cause damage, the scientists used a harmless virus to make gum cells overproduce activin A, without adding other inflammatory triggers. The extra activin A flowed into the bloodstream, activated its receptors on muscle fibers, and led to marked loss of muscle mass and fiber size, confirming that the mouth could drive muscle atrophy through this single messenger.
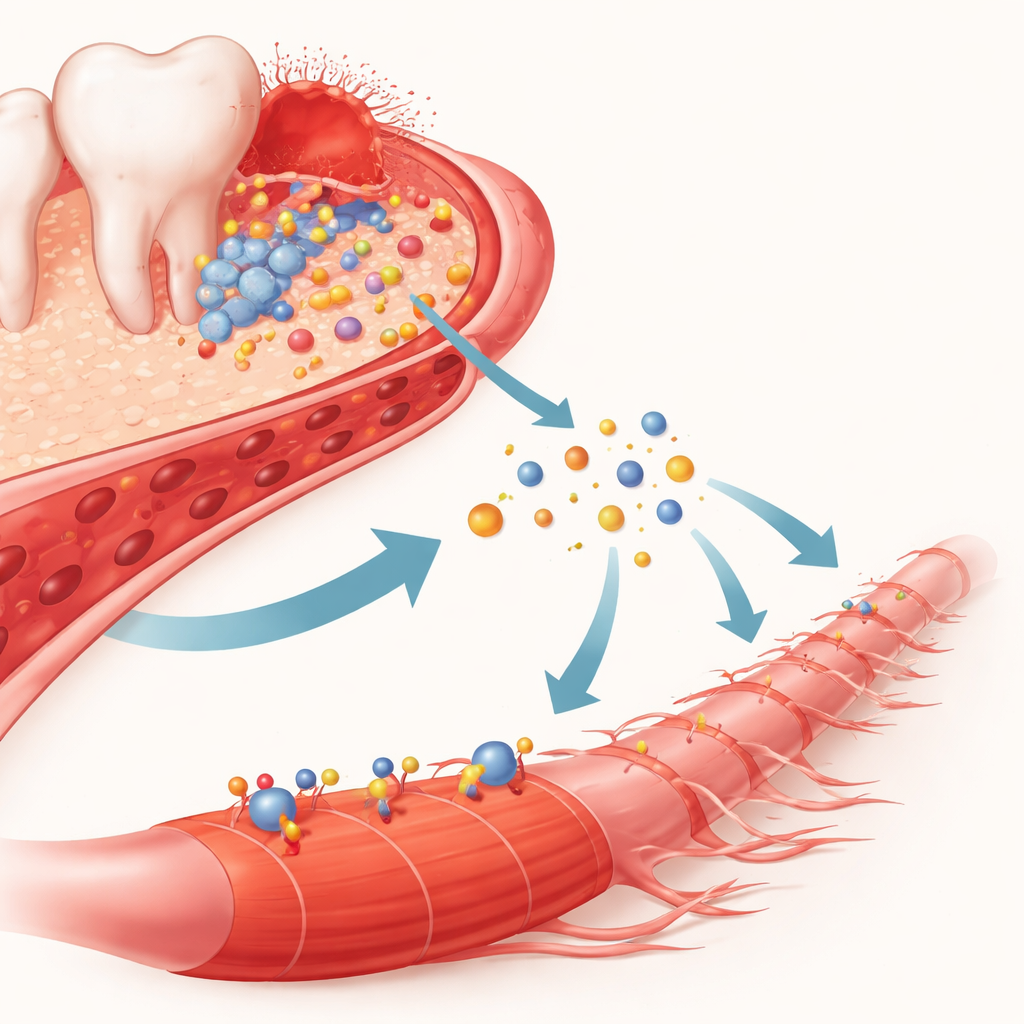
Turning down the signal to protect muscle
If activin A is the culprit, blocking it should spare muscle. The researchers tested two strategies. First, they injected a small interfering RNA—essentially a targeted "off switch" for the activin A gene—directly into the diseased gums of mice with periodontitis. This local treatment sharply reduced activin A levels in the blood during the active phase of disease and largely restored muscle mass, fiber diameter, and grip strength, even though the gum disease and associated bone loss continued. Second, they used genetically engineered mice whose muscles are naturally shielded from activin A by an internal inhibitor called follistatin. These protected animals did not lose muscle strength or size when periodontitis was induced, underscoring that activin A signaling in muscle is the crucial link between gum disease and systemic muscle wasting.
Evidence in people and what it means
The team also looked at human data to see whether this mechanism might matter outside the lab. In gum tissue samples from people with periodontitis, the gene for activin A was strongly elevated, especially in the same types of cells highlighted in the mouse work. Blood tests showed higher activin A levels in patients with significant bone loss around their teeth than in healthy volunteers. National survey data further revealed that older adults with periodontitis tended to have weaker handgrip strength, a simple measure of overall muscle function. Taken together, these findings suggest that chronic gum inflammation may be an underappreciated contributor to age-related muscle loss and frailty.
Why keeping gums healthy could protect your strength
In everyday terms, this study proposes a chain reaction: ongoing gum disease encourages certain cells in the mouth to pump out activin A; this protein then enters the bloodstream, travels to muscles throughout the body, and nudges them toward breakdown and weakness. Importantly, the work also hints at practical solutions. Standard dental care to prevent or treat periodontitis may do more than save teeth—it might help preserve muscle strength as we age. In the future, targeted treatments that dampen activin A production in diseased gums, without affecting the rest of the body, could offer a new way to shield vulnerable older adults from muscle loss linked to chronic oral infection.
Citation: Shim, W., Suh, J., Kim, H.K. et al. Periodontitis induces skeletal muscle atrophy by increasing circulating levels of activin A.. Nat Commun 17, 4063 (2026). https://doi.org/10.1038/s41467-026-72766-1
Keywords: periodontitis, muscle atrophy, activin A, oral-systemic health, sarcopenia