Clear Sky Science · en
Excessive pyroptosis mediates the exacerbation of pneumonia caused by low-lethality influenza virus and secondary MRSA co-infection
When Flu and Bacteria Team Up
Most winters, we think of seasonal flu as a short lived illness. But when flu joins forces with certain drug resistant bacteria, a routine infection can spiral into life threatening pneumonia. This study uses mice to explore why a mild strain of influenza A virus, when followed by infection with methicillin resistant Staphylococcus aureus (MRSA), can cause such severe lung damage and what this might mean for future treatments.
A Dangerous Double Hit to the Lungs
The researchers built a co infection model in mice by first giving them a low dose of influenza A virus and then, three days later, exposing them to MRSA. On their own, these mild infections caused limited illness. Together, they produced pneumonia that was worse than either a high dose of flu or a high dose of MRSA alone. The co infected mice lost more body weight, had higher lung weight relative to body size and showed intense inflammation in lung tissue sections, including collapsed air sacs, heavy immune cell invasion and bleeding. Interestingly, the amount of flu virus in the lungs did not rise much during co infection, but the MRSA levels did, suggesting that the earlier flu infection weakened the lungs’ ability to clear bacteria.
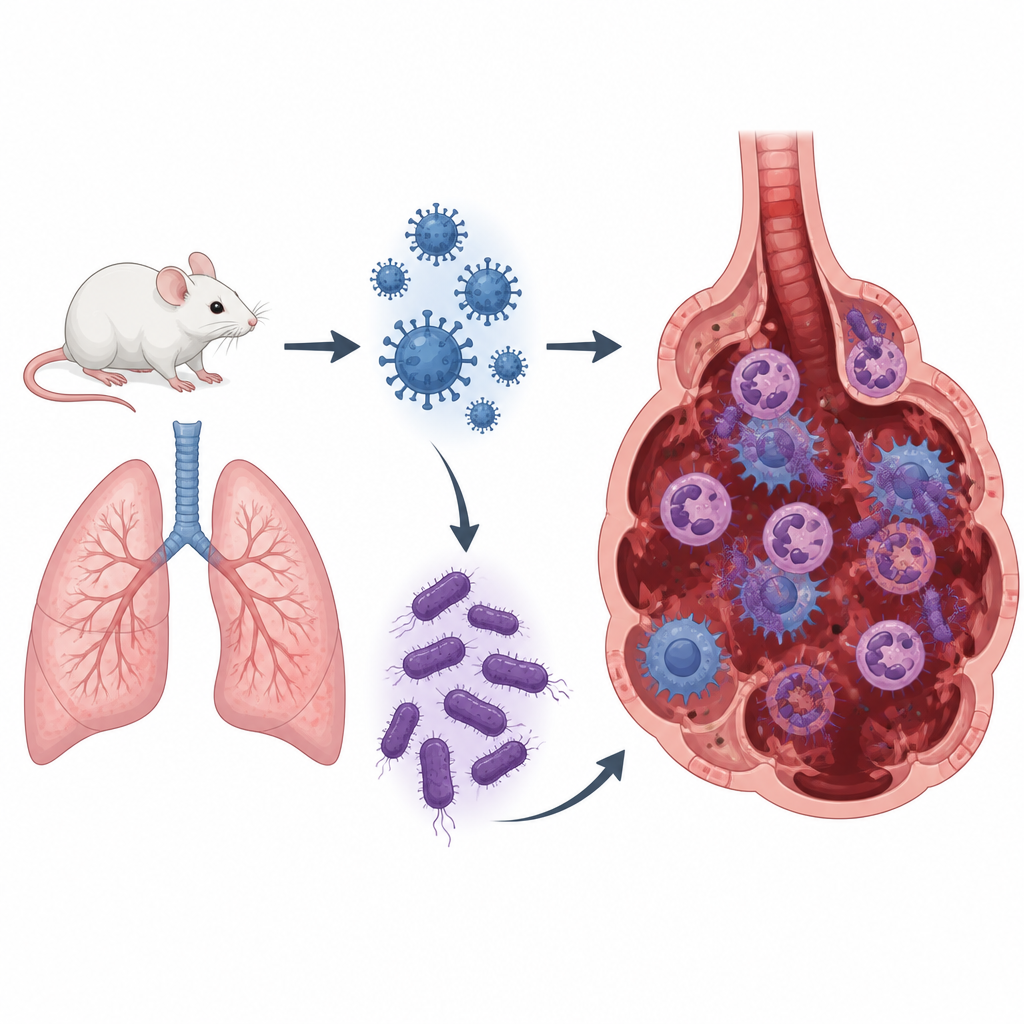
Standard Drugs Cannot Fully Calm the Storm
Because doctors usually treat such patients with an antiviral for flu and antibiotics for bacteria, the team tested this approach in their mice. They gave oseltamivir, a common flu drug, together with linezolid, an antibiotic used against MRSA, after symptoms appeared. While this treatment attacked both virus and bacterium, the mice still showed serious lung injury. Their lung index values stayed high, tissue damage was obvious and key signaling molecules of inflammation remained elevated. These findings suggest that once the inflammatory storm has started, simply removing the germs is not enough to restore lung health.
Cells that Self Destruct and Fuel Inflammation
To understand what was driving this runaway damage, the scientists examined which genes were switched on in infected lungs. They found strong activation of pathways linked to a fiery form of cell death called pyroptosis. In this process, immune cells such as macrophages activate a protein called caspase 1, which cuts another protein, gasdermin D, into a fragment that punches holes in the cell membrane. The dying cell then spills inflammatory molecules that can injure surrounding tissue. In the co infected mice, genes and proteins related to this pathway, including gasdermin D and interleukin 1β, were sharply increased. Microscopy and cell culture experiments showed that lung macrophages, the resident cleanup cells of the air sacs, were undergoing this pore forming death in large numbers during co infection.
Blocking Harmful Cell Death to Protect the Lung
The team then asked whether stopping pyroptosis could soften the impact of co infection. They used disulfiram, an old drug better known for treating alcohol dependence, which can block gasdermin D pores. When given directly into the nose of co infected mice, disulfiram reduced visible lung damage, lowered levels of inflammatory molecules and helped restore the population of tissue resident macrophages. Bacterial counts in the lungs also fell, suggesting that preserving macrophage function improved bacterial clearance. Finally, when disulfiram was added to the standard mix of oseltamivir and linezolid, lung injury and inflammation decreased more than with antiviral and antibiotic treatment alone.
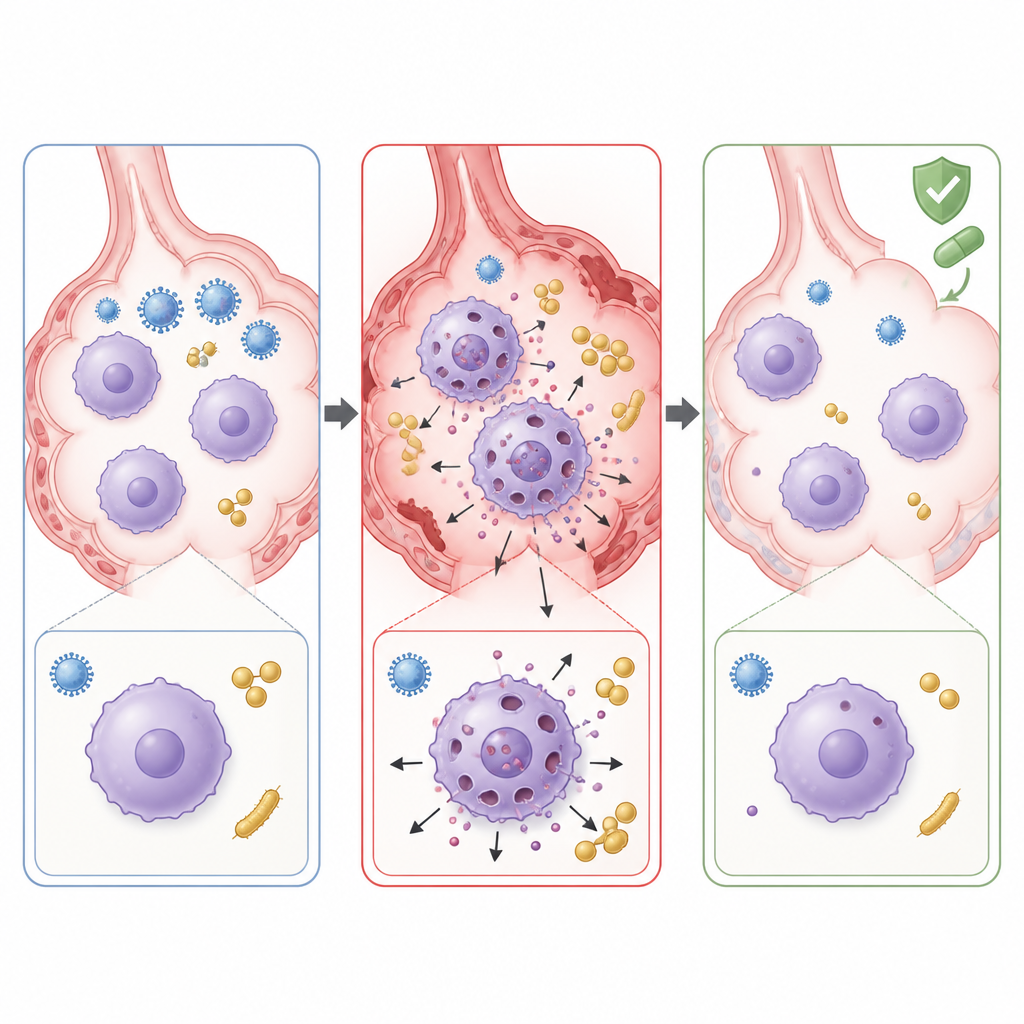
What This Means for Treating Severe Pneumonia
This work suggests that in flu MRSA co infection, part of the danger comes not only from the microbes themselves but from friendly fire, as macrophages die in a highly inflammatory way and damage lung tissue. Standard drugs that target virus and bacteria may not fully protect patients once this self destructive process is underway. By blocking gasdermin D and dampening pyroptosis, drugs like disulfiram could one day serve as add ons to existing therapies, helping to calm lung inflammation, preserve helpful immune cells and improve outcomes in severe pneumonia caused by mixed infections.
Citation: Tian, ZC., Liu, Y., Niu, YJ. et al. Excessive pyroptosis mediates the exacerbation of pneumonia caused by low-lethality influenza virus and secondary MRSA co-infection. Cell Death Discov. 12, 216 (2026). https://doi.org/10.1038/s41420-026-03031-z
Keywords: influenza, MRSA coinfection, pneumonia, macrophage pyroptosis, lung inflammation