Clear Sky Science · en
Lysine attenuates acute lung injury by restoring α-tubulin acetylation and ciliary activity
Why this matters for lung health
Severe lung injury can turn a bad infection or toxic exposure into a life‑threatening crisis, leaving patients dependent on machines to breathe and, if they survive, at risk of lasting scarring. This study explores a surprisingly simple helper: the common amino acid lysine. The researchers show that lysine can help injured lungs repair themselves in animal models by supporting tiny hair‑like structures on airway cells and stabilizing the barrier that keeps the air sacs intact.
When lung repair goes off course
Acute lung injury and its severe form, acute respiratory distress syndrome, arise from major insults such as viral pneumonia, toxic chemicals like paraquat, radiation, or chemotherapy. In these conditions, the delicate lining of the air sacs is damaged, fluid and inflammatory cells flood in, and some patients progress to permanent scarring called pulmonary fibrosis. The lung’s main repair cells, known as type II alveolar cells, can either regenerate the normal air‑sac surface or drift into scar‑forming states. The authors used human samples and animal models of paraquat poisoning, a well‑known cause of catastrophic lung damage, to understand what tips this balance toward healing or fibrosis.
A hidden energy shortage in injured lung cells
By mining single‑cell RNA sequencing data from patients and measuring blood metabolites, the team found that the lung’s epithelial cells undergo a profound metabolic shift during severe injury. Mitochondrial pathways that normally generate energy are pushed to their limits, and cells start heavily consuming amino acids, especially lysine. In both patients and mice, blood levels of lysine and several other essential amino acids dropped, suggesting they were being burned as backup fuel. At the same time, genes involved in breaking down lysine into acetyl‑CoA, a central metabolic building block, were ramped up. This pointed to lysine metabolism as a key “salvage” route helping exhausted cells keep going when sugar and fat pathways falter.
Lysine helps damaged lungs bounce back
To test whether this metabolic clue could be turned into therapy, the researchers supplemented lysine in mice and non‑human primates with paraquat‑induced lung injury. The results were striking: in mice, survival improved from none of the untreated animals to nearly two‑thirds of those given lysine. Lungs from supplemented animals showed less collagen deposition and thickening of tissue, indicating less fibrosis, and classic microscopic signs of alveolitis were markedly reduced. Gene‑expression profiles, wildly disturbed by paraquat, moved back toward normal under lysine treatment. Markers of the key epithelial cell types that form the air‑blood barrier, particularly type II and type I alveolar cells, rebounded. At the same time, immune cell recruitment and systemic inflammatory markers diminished, consistent with secondary benefit from better preservation of the epithelial barrier.
Tiny cellular “brushes” and calcium control
Digging deeper, the authors discovered that lysine’s main action was structural as much as metabolic. Paraquat injury reduced important epithelial adhesion proteins such as E‑cadherin and ZO‑1, loosening the seal between neighboring cells, and it blunted the growth and function of primary cilia—microscopic protrusions that sense the cell’s environment. Lysine supplementation restored acetylation of α‑tubulin, a modification required to build stable cilia, and brought ciliary numbers and length back toward normal. These revived cilia helped reposition a calcium channel protein, TRPC1, away from the flat cell surface and toward the cilium. As a result, harmful calcium influx into the cell dropped, downstream calcium‑sensitive signaling quieted, and E‑cadherin and ZO‑1 levels recovered, helping cells retain their organized, epithelial identity instead of sliding into scar‑like states. Notably, cilia were most prominent on a subset of type II alveolar cells, suggesting lysine particularly supports these crucial progenitors.
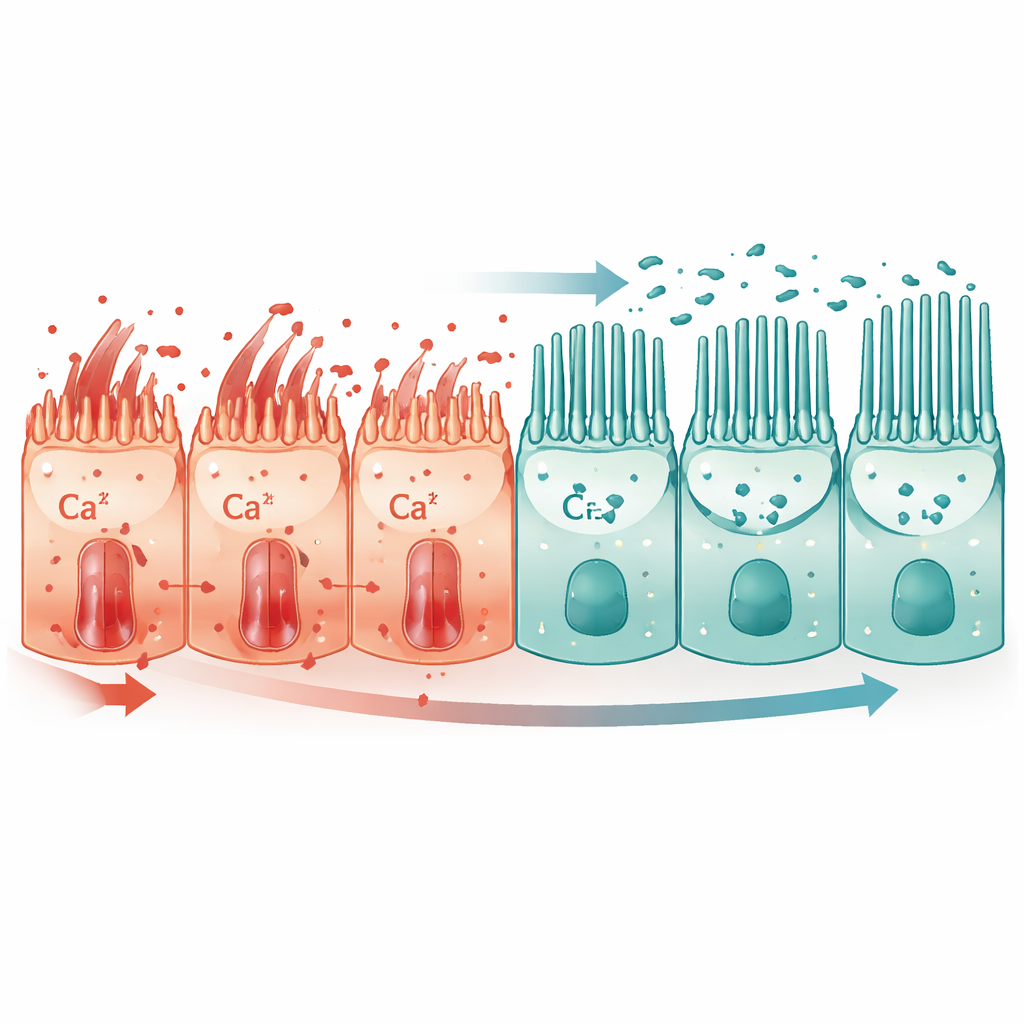
Blood calcium as a warning sign
The study also looked outward, into the bloodstream. In patients with paraquat poisoning, serum calcium levels were significantly lower than in healthy volunteers and fell further as blood paraquat levels and kidney injury worsened. In both mice and primates, paraquat depressed blood calcium, while lysine treatment partially restored it. Together with the cell‑level data, this points to disturbed calcium handling as a central feature of severe lung injury and positions lysine’s normalization of calcium flows as a key part of its protective effect.
What this could mean for patients
In everyday terms, the authors propose that lysine acts like a dual‑purpose support: it refuels stressed lung cells with the metabolic ingredient acetyl‑CoA and uses that fuel to shore up the microscopic scaffolding that holds cells together and powers their cilia. By restoring these tiny “brushes” and tightening cell junctions, lysine helps calm runaway calcium signals that would otherwise push cells toward scarring. Because lysine is already used clinically and showed benefits in multiple animal models, the work suggests that carefully designed trials could test it as a safe add‑on treatment for acute lung injury and perhaps for preventing subsequent fibrosis.
Citation: Yang, W., Meng, X., Zhu, Y. et al. Lysine attenuates acute lung injury by restoring α-tubulin acetylation and ciliary activity. Cell Death Discov. 12, 150 (2026). https://doi.org/10.1038/s41420-026-03025-x
Keywords: acute lung injury, lysine, alveolar epithelial cells, cilia, calcium signaling