Clear Sky Science · en
Identification of common spontaneous brain activity alterations across psychiatric disorders
Why this matters for mental health
Many different mental health conditions, such as depression, bipolar disorder, schizophrenia, anxiety, obsessive compulsive disorder, and posttraumatic stress disorder, can look very different on the surface. Yet people with these diagnoses often share similar problems with mood, thinking, and motivation. This study asks a basic question that matters for patients, families, and clinicians alike: do these disorders also share a common signature in the resting brain, and if so, what might that reveal about causes and treatments that cut across labels?

A quiet brain is never truly at rest
Our brains are active even when we lie still with eyes closed, and this baseline activity can be measured with resting state functional MRI. One widely used measure, called the amplitude of low frequency fluctuation, tracks how strongly local brain areas pulse over time. The authors gathered data from 210 previous studies, covering more than ten thousand patients and over eleven thousand healthy volunteers. By combining these results, they searched for brain regions that consistently differed between patients and healthy people, no matter which psychiatric diagnosis the patients carried.
Shared hot spots and quiet zones
The meta analysis revealed a striking pattern. Across disorders, several regions involved in thinking and emotion showed stronger spontaneous activity in patients than in healthy volunteers. These “hot spots” included parts of the frontal lobes that support planning and self control, the insula that helps integrate body signals and feelings, the cingulate and medial frontal areas linked to motivation and emotion regulation, the amygdala that detects threat and fear, and the striatum that processes reward and habits. In contrast, brain areas that control voluntary movement and bodily sensations, located along the central strip of the brain, tended to show weaker baseline activity in patients.
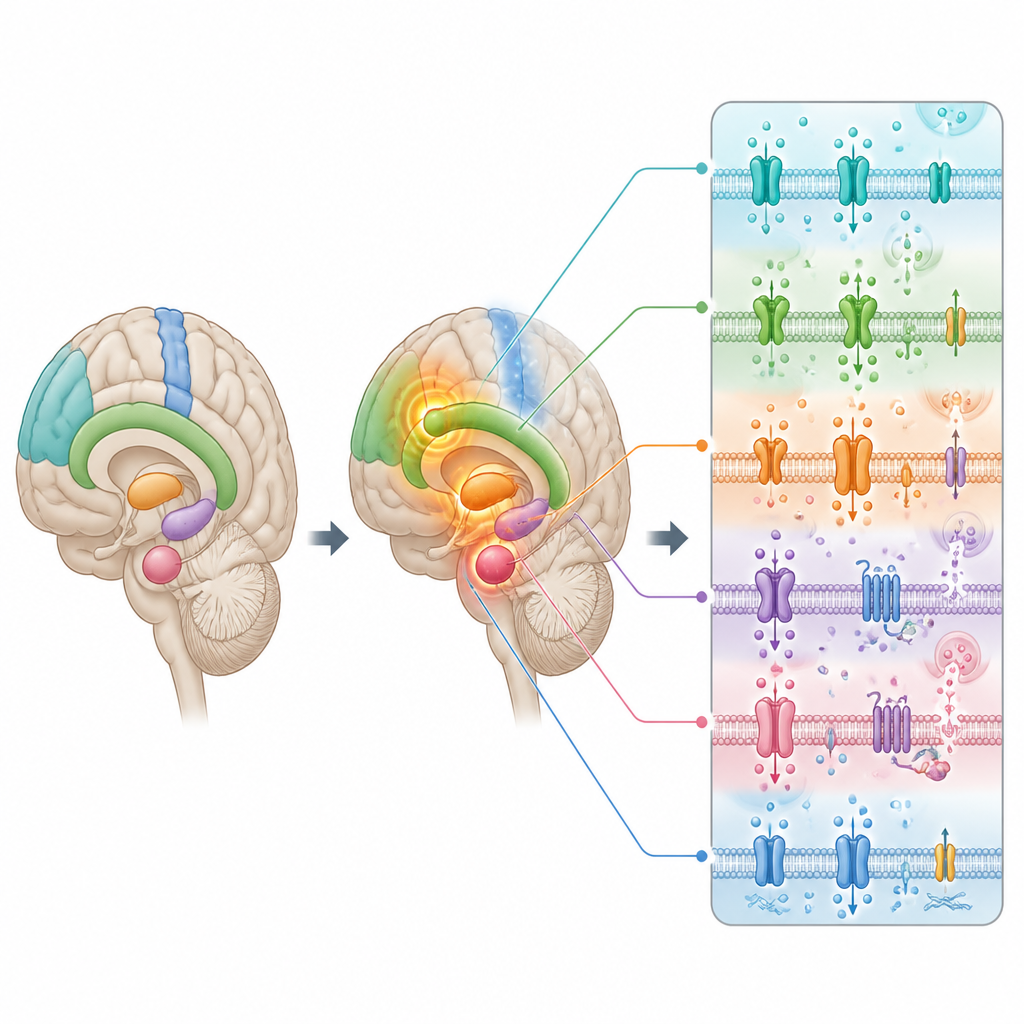
Changes in brain wiring and chemistry
To understand whether these functional shifts ride on deeper physical changes, the researchers also pooled results from studies of cortical thickness, a measure of how thick the brain’s outer sheet of cells is. They found that some of the same frontal and insula regions with unusually strong activity were also thinner across disorders, hinting that the brain might be working harder in damaged areas to compensate. The team then compared the altered activity map with large databases of gene activity in the human brain and with maps of chemical messenger systems, such as dopamine and serotonin, built from PET scans.
Linking symptoms to genes and brain chemicals
The regions that behaved differently in patients were enriched for genes involved in moving charged particles across cell membranes and operating ion channels, basic components that let nerve cells fire. These same regions lined up with several transmitter systems, including dopamine, serotonin, noradrenaline, opioid, and acetylcholine, all well known to influence mood, motivation, and anxiety. When the authors compared their brain map with patterns from many task based imaging studies, they found the strongest overlap with mental functions related to reward, mood, and fear. In other words, the very circuits that look disrupted at rest are the ones people rely on to feel pleasure, stay balanced emotionally, and manage threat.
What this means for understanding mental illness
Put together, the findings suggest that many major psychiatric diagnoses share a common “neural fingerprint” at rest, centered on frontal and insula regions, deep emotion and reward hubs, and motor and sensory areas. The altered activity seems tied to both subtle physical thinning of brain tissue and to shifts in the genes and chemical messengers that let nerve cells communicate. For a lay reader, the key message is that conditions like depression, schizophrenia, and anxiety may be different expressions of partly shared brain circuit and molecular disruptions, rather than entirely separate brain diseases. Recognizing these overlaps could guide therapies that target common brain pathways instead of single diagnostic boxes, while also explaining why people across diagnoses can struggle with similar problems in mood, motivation, and movement.
Citation: Guo, Z., Tang, X., Xiao, S. et al. Identification of common spontaneous brain activity alterations across psychiatric disorders. Transl Psychiatry 16, 244 (2026). https://doi.org/10.1038/s41398-026-03986-8
Keywords: resting-state fMRI, psychiatric disorders, brain networks, neurotransmitters, emotion and reward