Clear Sky Science · en
Expert consensus on the management of third molar health
Why Wisdom Teeth Matter
Wisdom teeth sit at the crossroads of everyday experience and specialized dental care. Many people are told in their teens or twenties that their wisdom teeth should come out, often without a clear explanation of why or when this is truly necessary. This article brings together leading oral surgeons to create an expert playbook for managing wisdom teeth over a person’s lifetime, explaining how they develop, when they cause trouble, how they can be safely removed, and even how they can sometimes be reused to save other teeth.
How Wisdom Teeth Grow In
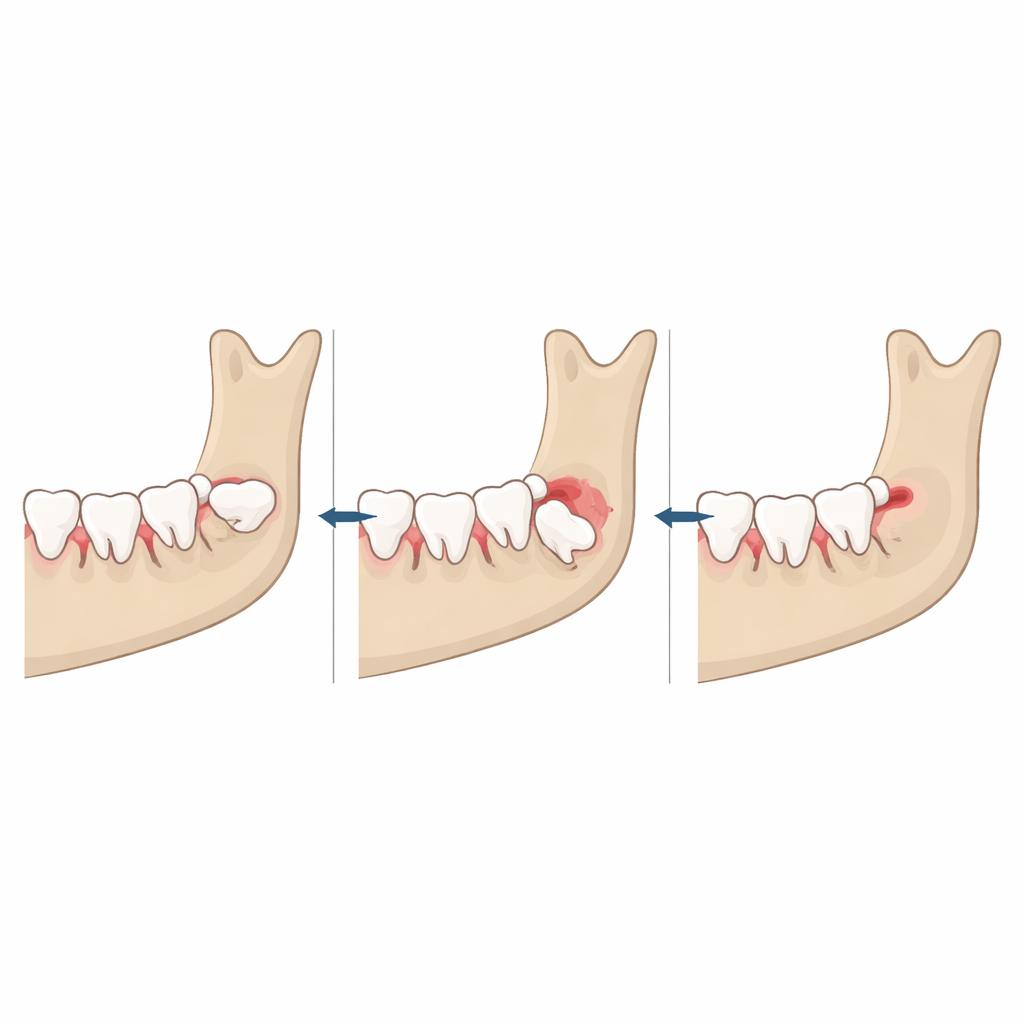
Wisdom teeth, or third molars, are the last permanent teeth to form and erupt, maturing well into a person’s twenties. Because they start developing later and farther back in the jaws, they often run out of room, tilt sideways, or remain buried in the bone. The paper describes a typical timeline: the early tooth bud appears in childhood, the crown forms through the teenage years, and the roots finish in late adolescence and early adulthood. Small differences in jaw size, growth pattern, sex, and ancestry strongly influence whether there is enough space for these teeth to emerge normally or whether they become “impacted” and trapped under gum or bone.
When Hidden Teeth Become a Problem
Impacted wisdom teeth are common and can quietly undermine oral health. Their awkward position makes them hard to clean, so bacteria collect around them and under the gum flap that partly covers them. This can trigger painful gum infections (pericoronitis), spread into the cheeks and neck spaces, or, in a minority of cases, progress to bone infection. The cramped contact point with the neighboring second molar often turns into a trap for food and plaque, raising the risk of cavities, deep gum pockets, and even loss of the healthy tooth in front. Pressure from a tilted wisdom tooth can also erode the root of the second molar or disturb the way the upper and lower teeth meet, sometimes aggravating jaw joint problems.
How Dentists Decide What to Do
The consensus stresses that no single rule fits everyone. Instead, dentists should combine a careful mouth examination with modern X‑ray methods to understand the exact position of each wisdom tooth and its relationship to nerves and the sinus. Simple mouth films and panoramic images are adequate for many cases, while three‑dimensional cone‑beam CT scans are reserved for tricky situations, such as roots close to the main jaw nerve or teeth bulging into the sinus. The authors review widely used classification systems that describe how deep and how tilted a tooth is, then refine them to better predict how difficult removal will be and what complications might occur. These tools help determine whether a tooth should be watched, taken out early, or managed with special techniques.
Modern Ways to Remove or Preserve Them
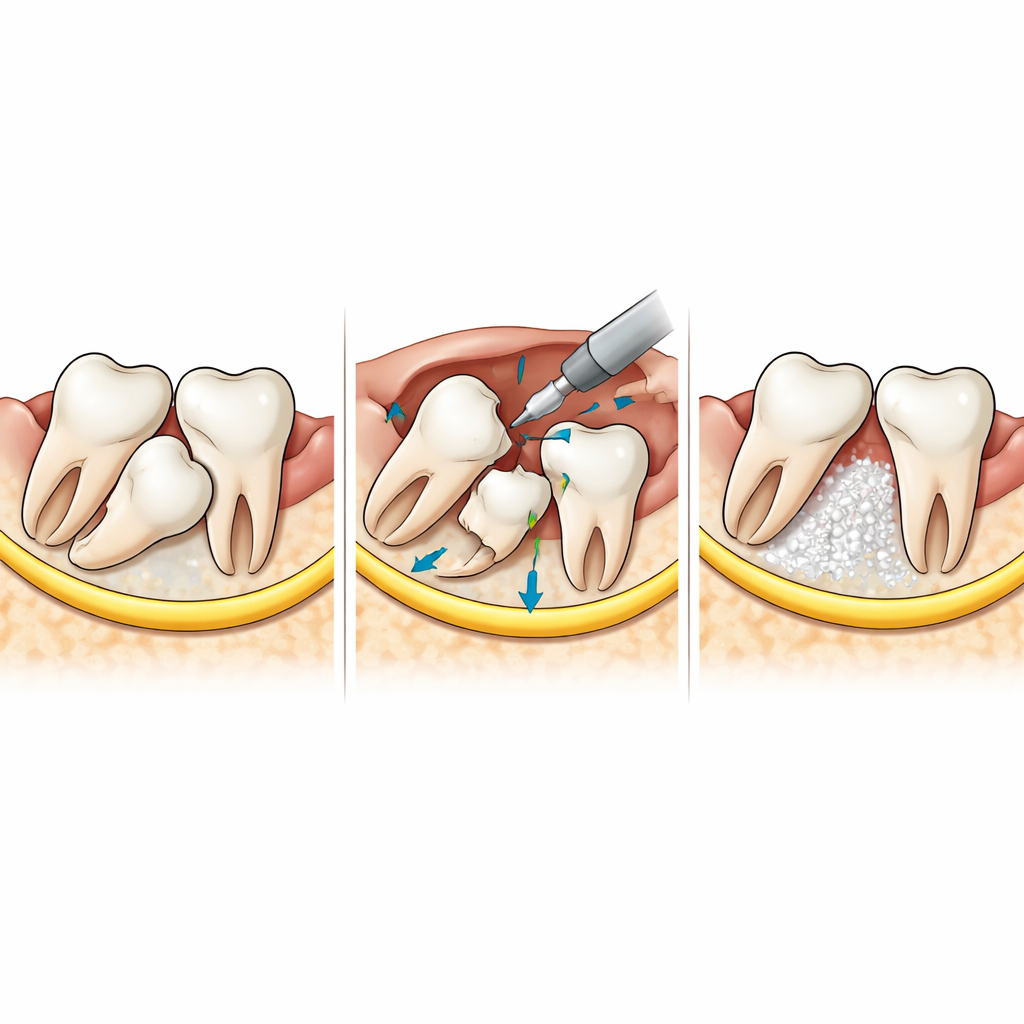
When removal is indicated—because of repeated infections, damage to the second molar, cysts or tumors, or planned braces or jaw surgery—the group recommends a step‑by‑step, minimally invasive surgical approach. This includes thoughtful incision design, gentle bone “window” creation, and cutting the tooth into pieces rather than removing it in one block, all to spare nearby structures like the jaw nerve and sinus. For deeply placed or high‑risk teeth, several newer strategies are highlighted: taking out the roots first while protecting the tooth in front, removing only the crown and leaving the roots when they are tightly wrapped around a nerve, or using orthodontic traction to slowly pull a tooth away from danger before extraction. Digital tools such as 3D planning, surgical guides, navigation systems, and even robots and endoscopes further improve accuracy and safety. The authors also discuss how to protect the bone behind the second molar with growth‑factor gels, bone substitutes, or replacing a bone window after surgery to encourage solid healing.
Turning a Problem Tooth into a Helpful One
Importantly, the paper argues that not all impacted wisdom teeth are liabilities. If a wisdom tooth is healthy and not causing trouble, it can sometimes be kept for future use. One option is autotransplantation—moving a wisdom tooth into the spot of a badly damaged first or second molar. With careful planning and gentle handling, success rates are high, allowing patients to keep a living, natural tooth instead of relying immediately on implants. Another option is to move the wisdom tooth forward with braces to fill a gap left by another molar, preserving chewing function and avoiding artificial replacements. These approaches require time and specialized skill but can make the most of teeth that would otherwise be discarded.
What This Means for Patients
For people wondering about their wisdom teeth, this expert consensus offers a reassuring message: decisions should be individualized, evidence‑based, and focused on preserving long‑term oral health. The article provides dentists with detailed guidance on when to monitor, when to intervene, and how to perform and follow up surgery as safely and gently as possible. For patients, it underscores the value of early evaluation, clear discussion of risks and options, and the possibility that a wisdom tooth can sometimes be part of the solution, not just the problem.
Citation: Sun, R., Xu, Y., Wu, Y. et al. Expert consensus on the management of third molar health. Int J Oral Sci 18, 36 (2026). https://doi.org/10.1038/s41368-025-00413-4
Keywords: wisdom teeth, third molar impaction, oral surgery, dental imaging, tooth autotransplantation