Clear Sky Science · en
An integrated drug repositioning analysis identifies rosiglitazone as a treatment for sarcopenia
Why this study matters for healthy aging
As people live longer, many struggle with sarcopenia, an age-related loss of muscle strength and mass that makes everyday tasks—like climbing stairs or carrying groceries—harder and more dangerous. There are no approved medicines specifically for this condition, and exercise, while helpful, is often difficult for the frailest older adults. This study explores whether an existing diabetes drug, rosiglitazone, could be repurposed to help aging muscles stay stronger for longer by acting through a newly highlighted "gut–muscle–metabolism" connection.
Finding a new use for an old medicine
The researchers began at the computer rather than the clinic. They first assembled a detailed picture of the biology behind sarcopenia by combining large human genetic studies of grip strength and limb muscle mass with an automated search of thousands of scientific papers and disease databases. From this work they pulled out hundreds of genes and grouped them into a muscle-focused network that highlights key processes involved in muscle maintenance, inflammation, hormones, and energy use. They then overlaid information about existing approved drugs and their known targets to see which medicines sit closest to this sarcopenia network, a sign they might influence the disease pathways.
From big data to a promising drug
Using this network map, the team calculated a proximity score between each drug’s gene footprint and the sarcopenia gene module. Eighteen drugs stood out as being strongly connected. To narrow these down, they applied a genetic technique called Mendelian randomization, which tests whether changing the activity of a drug’s target genes is likely to cause changes in traits such as grip strength. This second line of evidence pointed in particular to gene targets whose reduced activity was linked to better muscle strength and mass. Rosiglitazone, a diabetes drug that acts on the PPARG/RXRA family of regulators, emerged as one of the most promising candidates because its known actions aligned with the direction of genetic effects that favored stronger muscles.
Testing rosiglitazone in aging muscles
To move beyond predictions, the researchers tested rosiglitazone in naturally aged male mice, a widely used stand-in for human sarcopenia. Over five months, mice fed a rosiglitazone-containing diet gained less body weight but maintained similar food intake. More importantly, treated mice ran farther on a treadmill, tolerated the effort for longer, and received fewer electric shocks before tiring. They also stayed on a rotating rod longer, squeezed harder in grip tests, and had heavier hindlimb muscles with larger muscle fibers, without changing the balance between slow and fast fiber types. Together, these experiments show that long-term, low-dose rosiglitazone can boost muscle performance and size in older animals.
A gut–muscle–metabolism axis comes into focus
To understand how rosiglitazone exerts these effects, the team profiled the animals’ muscles and gut bacteria in depth. In muscle tissue, the drug switched on the growth-promoting Igf1–Pi3k–Akt pathway, while dialing down genes that drive muscle breakdown, such as Atrogin-1 and MuRF1. Metabolite profiling revealed shifts in amino acids and other small molecules linked to protein digestion, amino acid metabolism, and fatigue resistance, including higher levels of threonine, methionine, certain antioxidants, and signaling lipids. At the same time, analysis of gut microbes showed that rosiglitazone reshaped intestinal communities, reducing some Firmicutes groups while enriching families such as Clostridiaceae and the genus Clostridium, which are known to produce beneficial short-chain fatty acids. Genetic analyses in humans suggested that higher levels of these bacteria are causally associated with stronger grip. Correlation analyses in mice tied these microbes to higher Igf1 levels, favorable metabolites, and better physical performance, supporting a coordinated gut–microbe–muscle pathway.
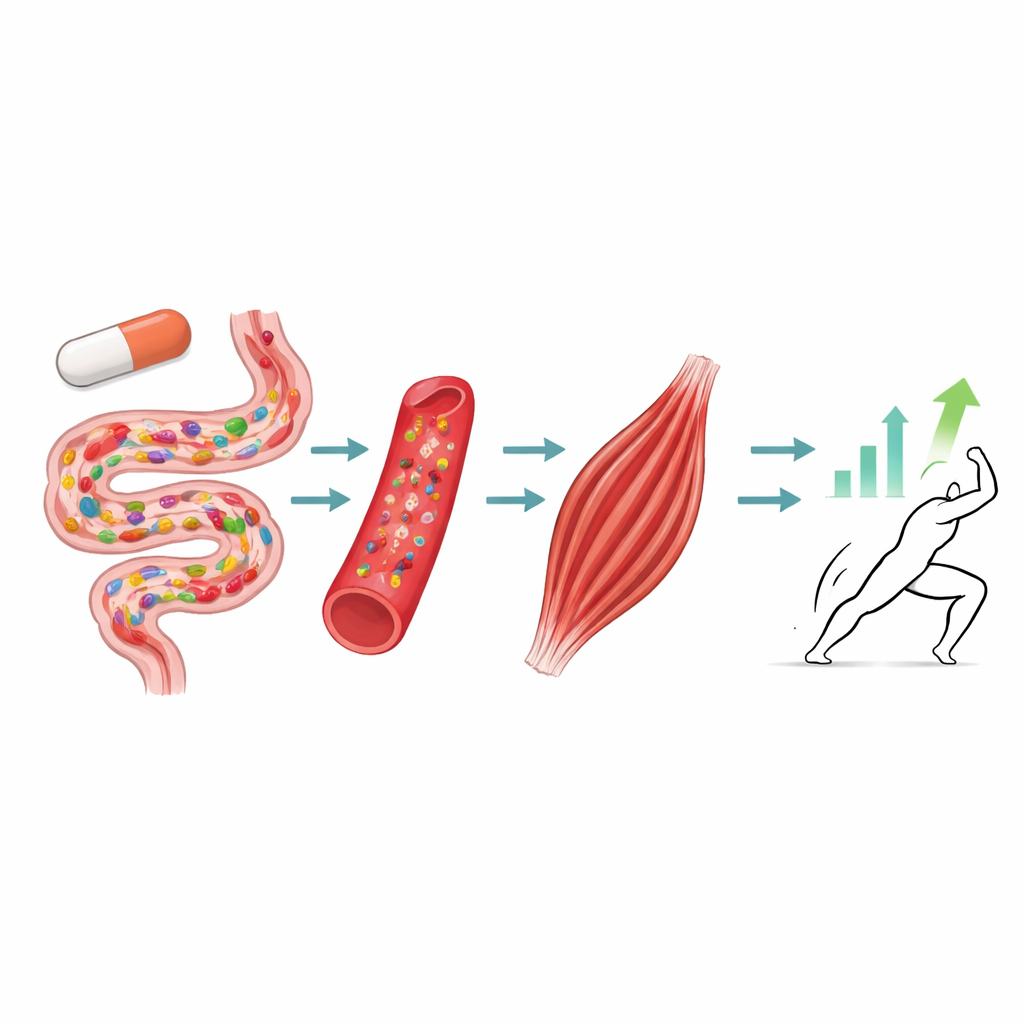
What this could mean for older adults
Taken together, the results suggest that rosiglitazone may help counter age-related muscle decline by tuning the gut microbiota, reshaping muscle gene activity, and improving protein and energy metabolism, ultimately leading to stronger, more resilient muscles. The drug is not without risks—it has been linked to heart failure, fluid retention, and increased fracture risk in some patients—so it cannot yet be recommended as a treatment for sarcopenia. However, this integrated, multi-omics study shows how an existing medicine might be redirected to support muscle health and highlights the gut–muscle–metabolism axis as a promising target. Future clinical trials will be needed to balance potential benefits in muscle strength against known side effects and to determine whether similar improvements can be achieved safely in older people.
Citation: Liang, S., Liu, Y., Xiao, HM. et al. An integrated drug repositioning analysis identifies rosiglitazone as a treatment for sarcopenia. Commun Biol 9, 443 (2026). https://doi.org/10.1038/s42003-026-09595-x
Keywords: sarcopenia, drug repurposing, rosiglitazone, gut microbiome, muscle aging