Clear Sky Science · en
Hematological and immune cell changes in complete blood count before and after hemodialysis
Why this matters for people on dialysis
Hemodialysis keeps people with severe kidney disease alive by cleaning their blood several times a week. But the treatment itself can quietly change their blood and immune cells in ways that affect fatigue, infection risk, and long term health. This study looks closely at simple blood tests taken before and after a single dialysis session to reveal what is really happening inside the bloodstream of these patients.
Looking at blood as a window into health
The researchers focused on the complete blood count, a routine test that measures red blood cells, white blood cells, and platelets. These numbers reflect how well the body carries oxygen, fights infection, and repairs blood vessels. By comparing results from 107 adults immediately before and immediately after one dialysis session, they hoped to see short term shifts that might not be obvious during regular clinic visits. The group included both men and women of different ages whose kidney failure was mainly caused by high blood pressure, often combined with diabetes.
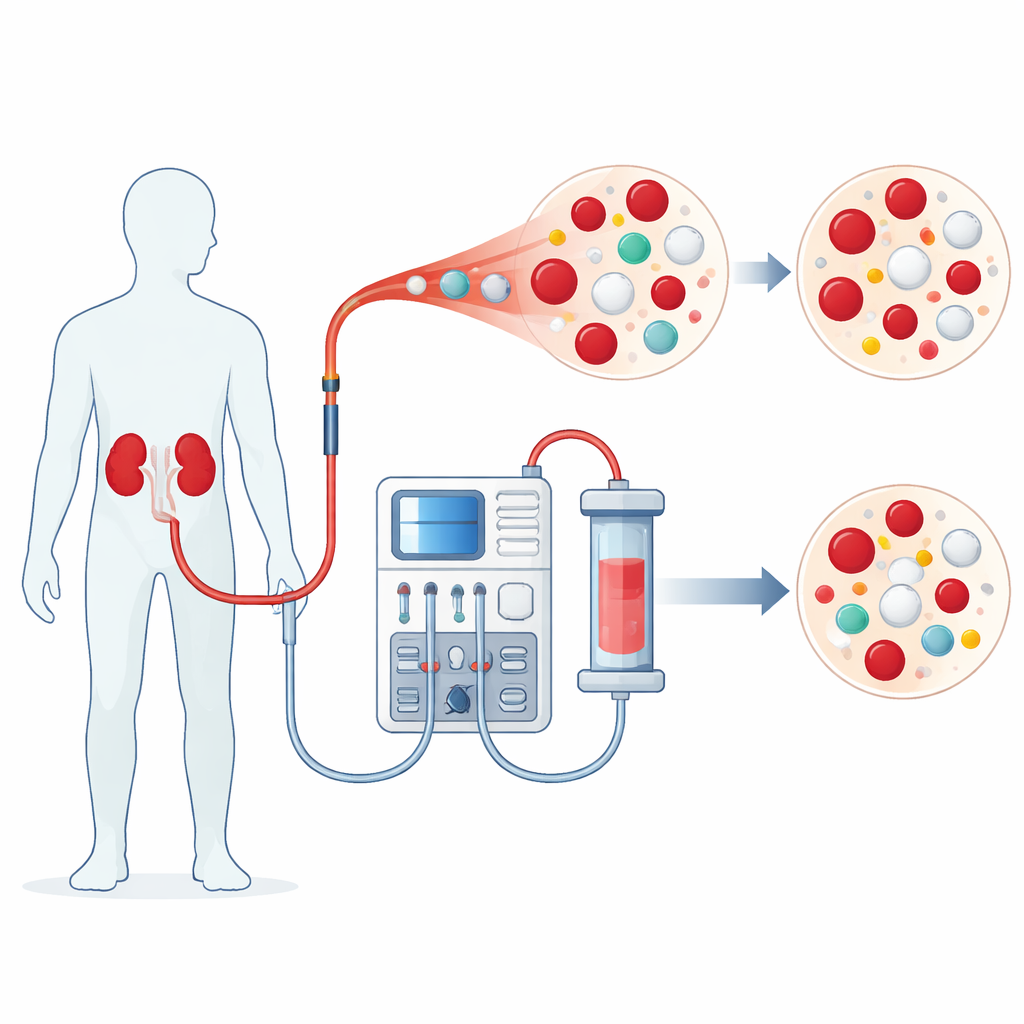
Differences between men and women
Before dialysis even began, men and women showed distinct patterns in their blood results. Anemia, a shortage of healthy red blood cells that can cause weakness and breathlessness, was very common overall but especially frequent in men. Women, on the other hand, had higher counts of certain white blood cells called lymphocytes and monocytes. These cells help coordinate immune responses and clean up damaged material, and their higher levels in women likely reflect known effects of sex hormones and genes on immunity. These baseline differences suggest that men and women may not respond to dialysis or infections in exactly the same way and may need slightly different treatment targets.
What one dialysis session does to blood cells
When the team compared blood tests taken just before and just after dialysis, they saw a clear drop in nearly all major blood cell measures. Levels of red blood cells, hemoglobin, and related indices all fell, which points toward ongoing damage or loss of red cells during treatment and may contribute to the stubborn anemia many patients face. White blood cells also declined, including key defenders such as neutrophils, lymphocytes, and monocytes. This pattern supports the idea that the dialysis circuit and filters place mechanical and chemical stress on blood cells, causing some to break apart or be temporarily trapped in blood vessels.
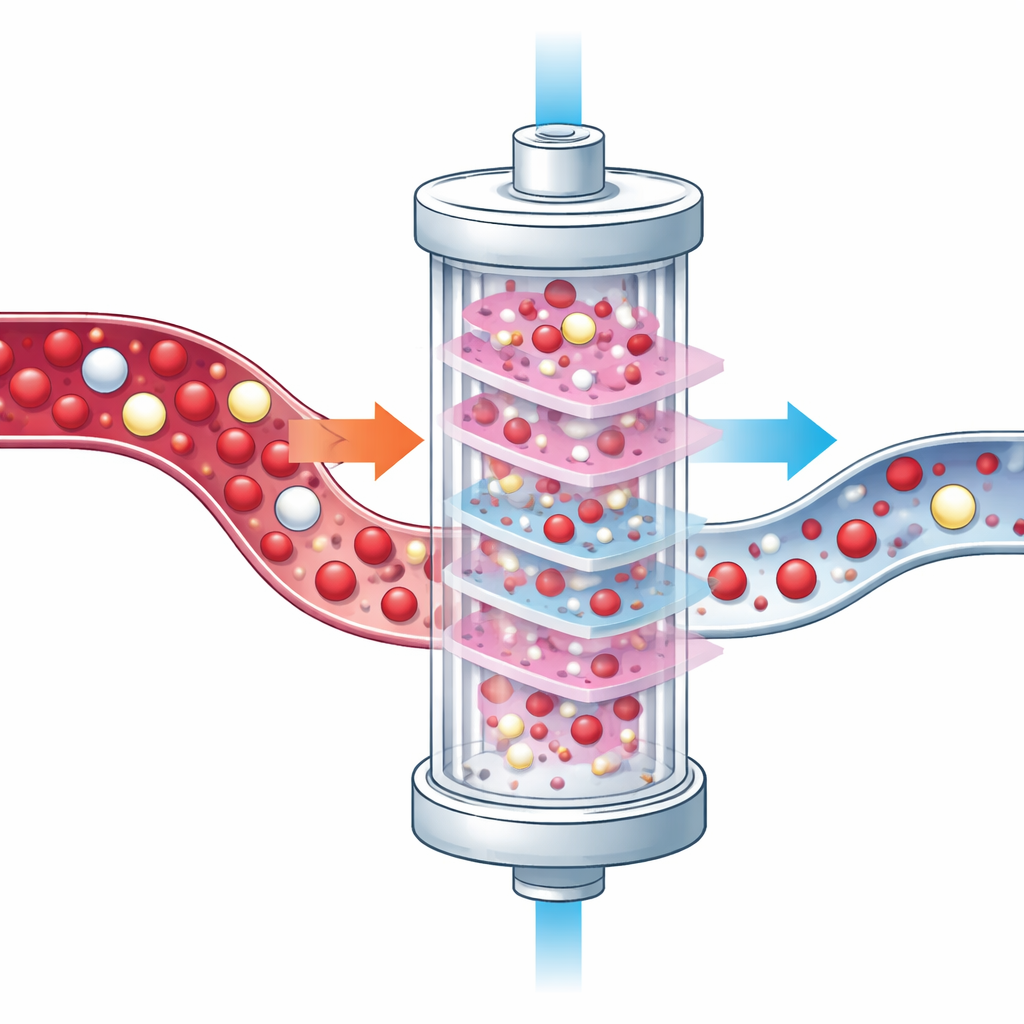
Hidden shifts in the immune system
Beyond simple rises and falls in cell counts, the study examined how different cell types move together. Before dialysis, total white blood cell numbers were strongly linked to their main subgroups, suggesting a coordinated immune system. After dialysis, those links weakened, except between lymphocytes and monocytes, hinting that neutrophils are especially disrupted by the process. The researchers also compared patients whose kidney failure was due only to high blood pressure with those who had both high blood pressure and diabetes. People with high blood pressure alone showed larger changes in their white blood cell counts, while those with diabetes seemed to have a blunted response, consistent with the known immune problems that accompany long standing high blood sugar.
What this means for patient care
To a layperson, the key message is that dialysis is more than a blood washing machine. Each session not only clears waste but also removes or stresses red and white blood cells, deepening anemia and weakening immune defenses, at least in the short term. These effects differ by sex and by other health problems such as diabetes or high blood pressure. The authors conclude that routine blood counts before and after dialysis could be used more thoughtfully as low cost markers to spot emerging immune suppression or worsening anemia. Tailoring dialysis settings and anemia treatment to each person’s age, sex, and medical background may help reduce infections, improve energy levels, and ultimately support better quality of life for people living with chronic kidney disease.
Citation: Alsayb, M.A., Makhdoom, H.Q. & Mahallawi, W.H. Hematological and immune cell changes in complete blood count before and after hemodialysis. Sci Rep 16, 14724 (2026). https://doi.org/10.1038/s41598-026-45584-0
Keywords: hemodialysis, chronic kidney disease, immune cells, anemia, complete blood count