Clear Sky Science · en
Proteomic analysis identifies distinct signaling pathways in lumbar intervertebral disc degeneration between type-2 diabetic and non-diabetic patients
Why your back and blood sugar are connected
Low back pain is one of the leading reasons people miss work, and worn out spinal discs are often to blame. This study asks a question that matters to millions living with type 2 diabetes: does diabetes change the way the soft cushions between the bones of the spine break down, and if so, how? By zooming in on thousands of proteins inside these discs, the researchers uncover distinct molecular patterns that differ between people with and without diabetes, offering clues to why back problems may be worse or earlier in life for some patients.
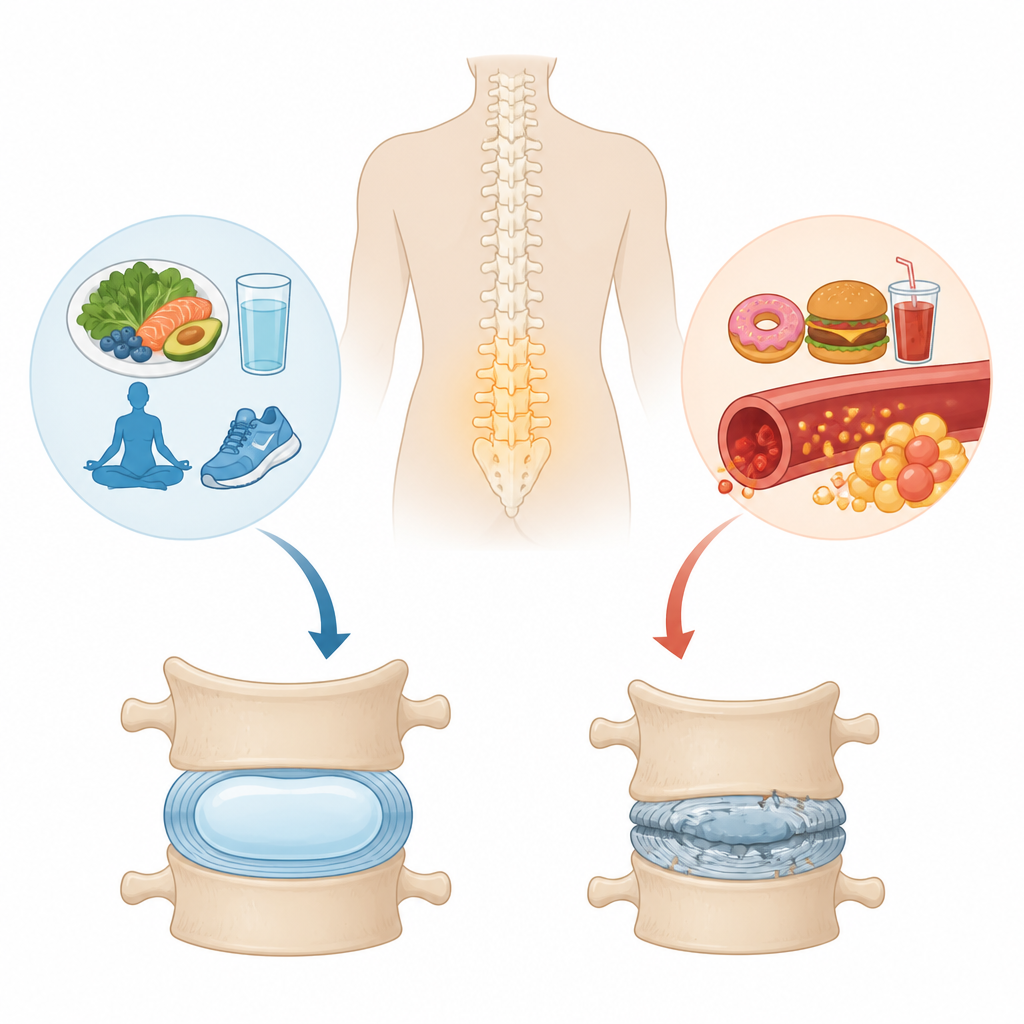
The cushions that keep us moving
Between each bone in the spine sits a small, jelly like pad called an intervertebral disc. Its center, the nucleus pulposus, is rich in water holding proteins that act like a shock absorber. Over time, or after injury, this structure can wear down, a process known as disc degeneration, which is closely linked to chronic low back pain. Type 2 diabetes, a long term disorder tied to high blood sugar and low grade inflammation, has been linked in large population studies to a higher risk of disc problems, but until now scientists had not directly compared the detailed protein makeup of discs from diabetic and non diabetic patients.
Reading the protein fingerprint of spinal discs
The team collected tissue from the center of lumbar discs removed during surgery from nine adults with severe disc disease, five with type 2 diabetes and four without. Using a technique called quantitative proteomics, they measured the levels of nearly 3,900 different proteins in these samples. When they compared the two groups, they found that 221 proteins were noticeably higher and 233 were lower in discs from people with diabetes. Computer based analyses showed that discs from diabetic patients had a clearly distinct protein pattern from those of non diabetic patients, confirming that diabetes is associated with a different internal environment in these damaged cushions.
How diabetes shifts disc energy use and structure
A key difference lay in how disc cells handle energy. In diabetic discs, many proteins linked to the cell’s power plants, the mitochondria, were increased, and entire pathways involved in burning fuel and producing energy were more active. This pattern points to higher oxidative stress, a state where reactive molecules can damage cells and their surroundings. At the same time, proteins that help build and organize the disc’s supporting gel and fibers were often reduced in diabetic discs. Important structural components, such as the large proteoglycan versican, and several molecules found in the space between cells, were lower, suggesting that the cushioning fabric of the disc is more fragile in the presence of diabetes.
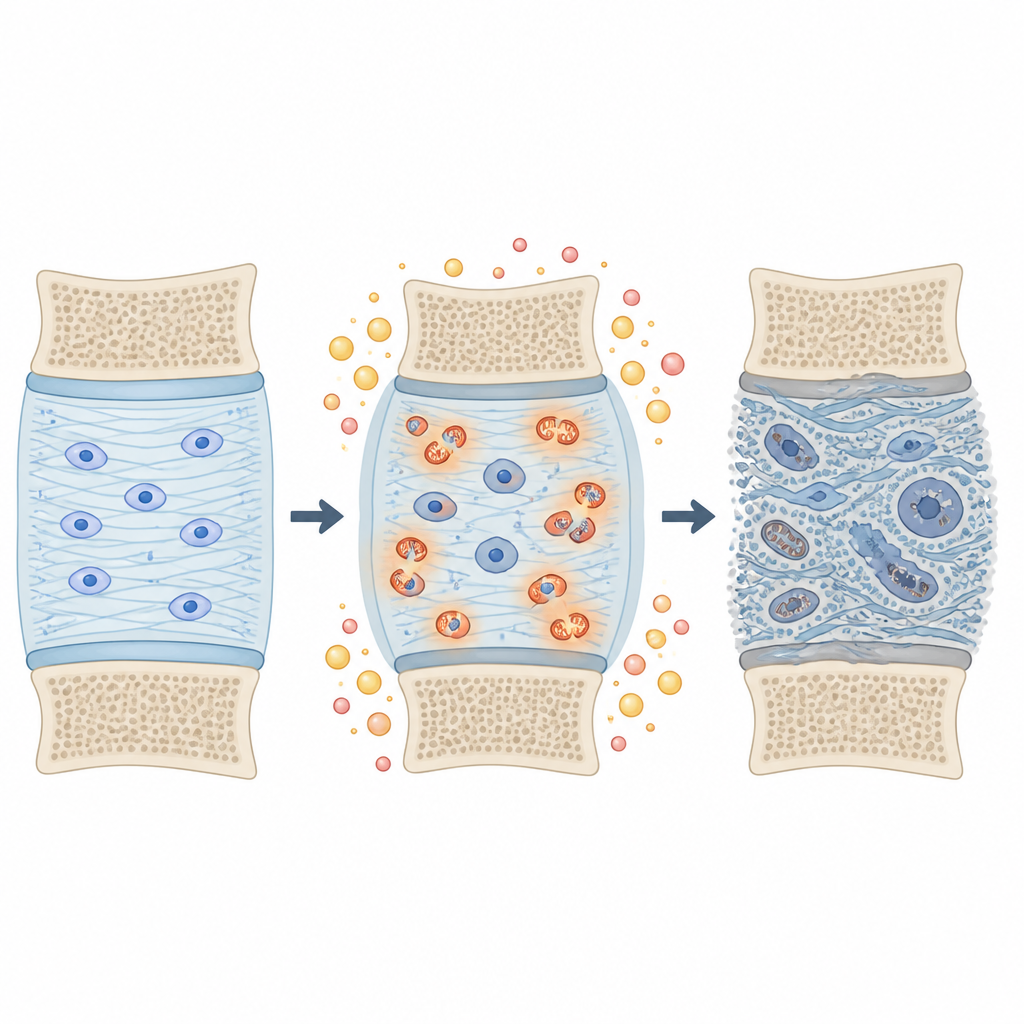
Chemical tweaks to the disc’s scaffolding
The researchers also looked at a subtle chemical change called proline hydroxylation, which is especially common in collagen, the main fibrous protein of connective tissues. They found more than two thousand of these modified sites across 230 proteins, many of them in collagens and other outside the cell components. In diabetic discs, some of these modifications on collagens were increased, forming a tightly connected network of altered proteins. This pattern is consistent with an environment under oxidative stress, where the disc’s scaffolding is chemically tweaked in ways that could stiffen or weaken it, and make it more prone to cracking or tearing under everyday loads.
What this means for patients and future care
Taken together, the findings suggest that type 2 diabetes does not simply speed up ordinary wear and tear in spinal discs; it reshapes the disc’s inner chemistry in specific ways. Diabetic discs show signs of overworked energy systems, higher oxidative stress, and deeper damage to the cushioning matrix than discs from non diabetic patients. While this small study cannot prove cause and effect, it provides a detailed map of candidate proteins and pathways that may one day guide blood tests, imaging markers, or targeted treatments. For people with diabetes and back pain, the work reinforces the idea that controlling metabolic health could be an important part of protecting the spine, while researchers now have a sharper molecular starting point for designing future therapies.
Citation: Moinuddin, F.M., Zhong, J., Astudillo Potes, M.D. et al. Proteomic analysis identifies distinct signaling pathways in lumbar intervertebral disc degeneration between type-2 diabetic and non-diabetic patients. Sci Rep 16, 15151 (2026). https://doi.org/10.1038/s41598-026-44970-y
Keywords: low back pain, intervertebral disc, type 2 diabetes, proteomics, oxidative stress