Clear Sky Science · en
Mesenchymal stem cell derived exosomes and injectable platelet-rich fibrin enhance SDFT healing in a donkey tendonitis model
Why Healing Torn Tendons Matters
Tendon injuries are a leading cause of lost training time and early retirement in racehorses and working equids, and similar problems affect human athletes. Once damaged, tendons tend to heal with stiff scar tissue rather than restoring their original springiness, making re‑injury likely. This study explores a new way to help injured tendons in donkeys heal more like healthy tissue, using two natural blood‑ and cell‑based products that may one day benefit horses and perhaps even people.
A Closer Look at Donkey Leg Injuries
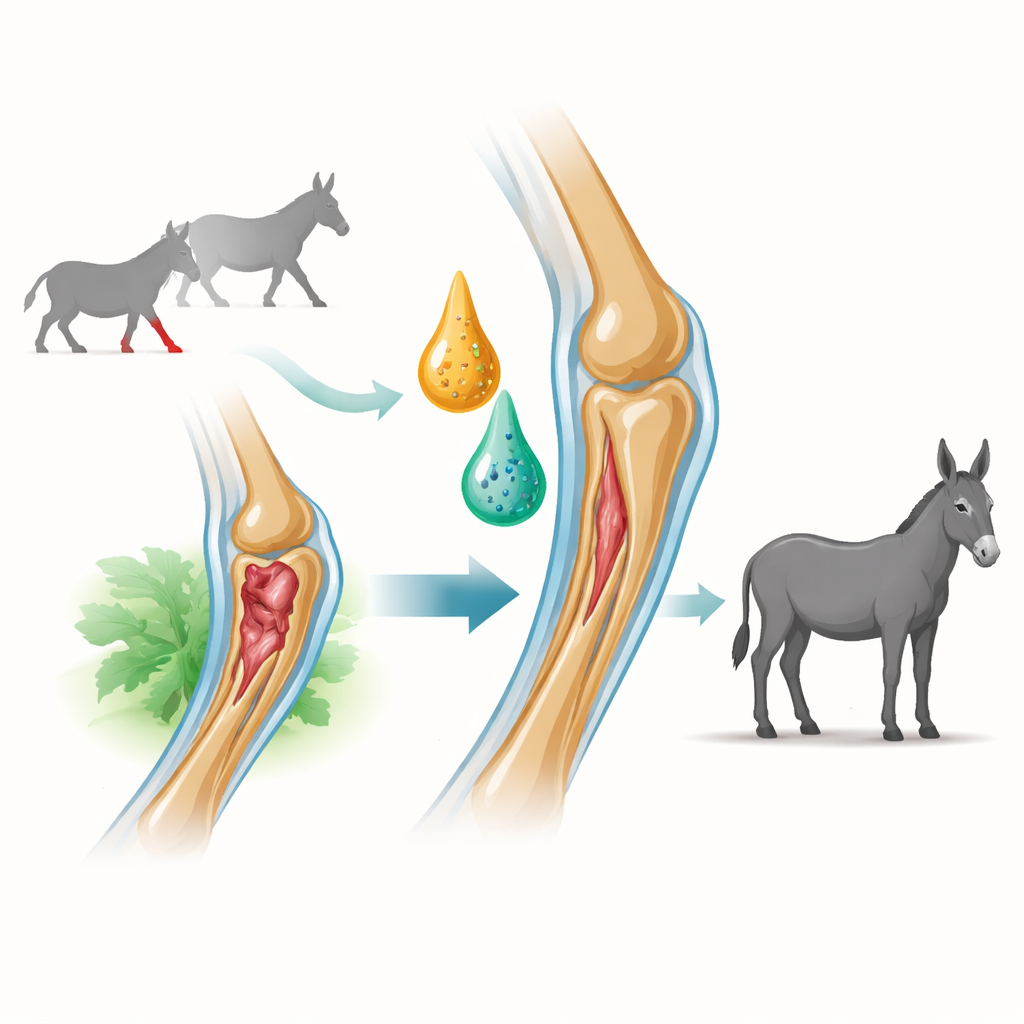
The research focused on the superficial digital flexor tendon, a cord‑like structure that helps support the weight of the body and stores energy during movement. In sport horses this tendon is a frequent site of strain. To mimic this problem in a controlled way, the scientists created small, standardized injuries in the front leg tendons of donkeys using an enzyme that weakens the tissue. This model reproduces the pain, swelling, and microscopic damage seen in real‑world tendonitis, but allows careful, side‑by‑side testing of new treatments.
Two Natural Boosts for Repair
The team tested an injectable form of platelet‑rich fibrin (I‑PRF) and tiny packets released by stem cells, known as exosomes. I‑PRF is made from the animal’s own blood and contains platelets trapped in a soft fibrin network that slowly releases growth factors over about two weeks. Exosomes were prepared from bone‑marrow‑derived stem cells; these nanoscale vesicles carry signaling molecules that can calm inflammation and guide local cells toward rebuilding tissue. Donkeys were randomly assigned to receive saline (placebo), I‑PRF alone, or a mixture of I‑PRF and exosomes injected directly into the injured tendon one week after damage.
Tracking Healing From Surface to Strength
Over 20 weeks, the researchers monitored recovery using several complementary methods. Clinicians scored lameness, pain, and how well each animal bore weight on the injured limb. Ultrasound scans measured the size of the damaged core, how reflective the tendon looked, and how well the internal fibers lined up. At set time points, some tendons were examined under the microscope to assess fiber organization, blood vessel growth, and types of collagen present. Finally, at the end of the study, tendon strips were stretched until they broke to measure how much force and stretch they could withstand compared with normal tissue.
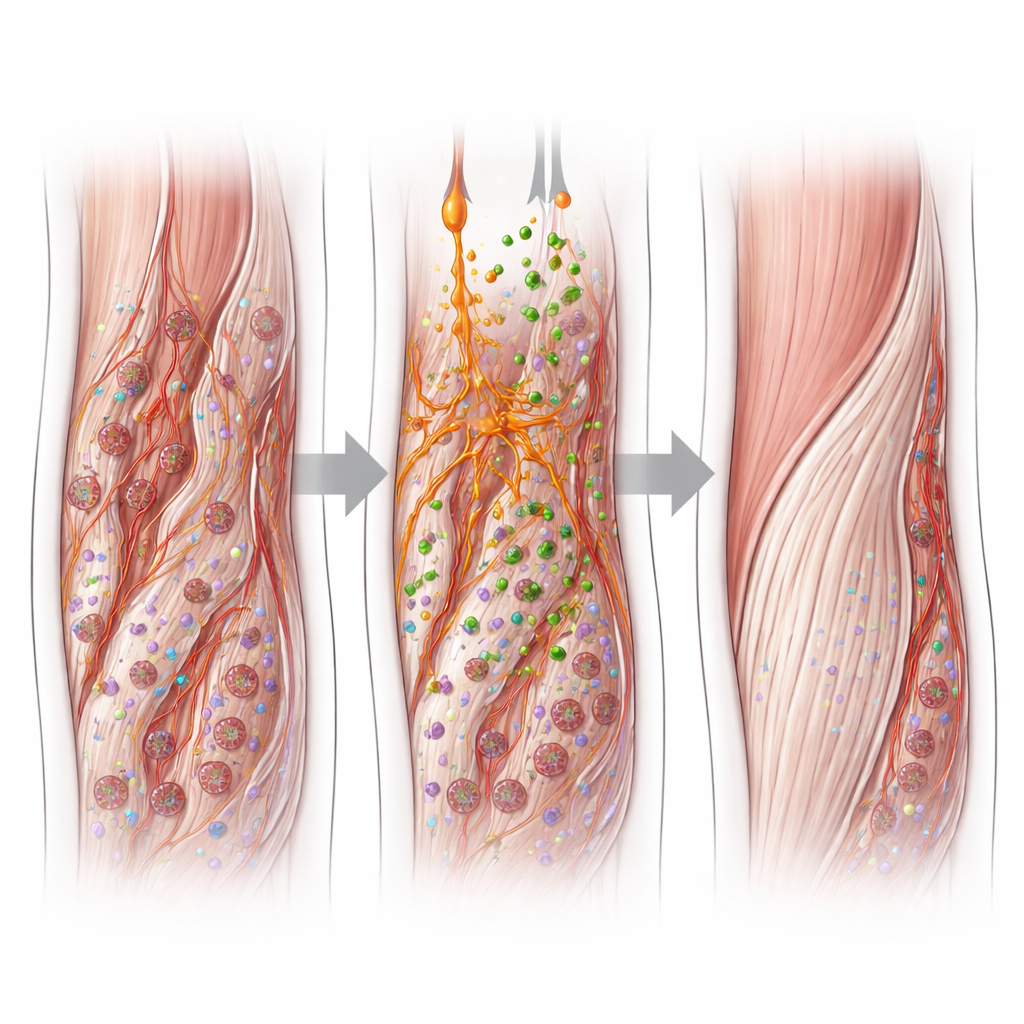
What the Treatments Changed Inside the Tendon
All groups improved over time, but the pattern and quality of healing differed. Tendons treated with the combination of I‑PRF and exosomes showed the fastest reduction in the size of the core lesion on ultrasound and earlier return toward a more uniform, nearly normal appearance. Under the microscope, these tendons had better‑aligned fibers, fewer abnormal blood vessels, and a more balanced cell density. Importantly, they contained more collagen type I—the strong, rope‑like form found in healthy tendon—and less collagen type III, which is associated with weaker scar tissue. I‑PRF alone produced intermediate benefits, while the saline group tended to develop harder, nodular areas with disorganized fibers and a higher proportion of scar‑like collagen.
From Microscopic Changes to Real‑World Strength
Mechanical testing revealed that, although none of the injured tendons fully matched the strength of uninjured ones by 20 weeks, those treated with I‑PRF plus exosomes endured the greatest stress before failing and could stretch more before tearing. Donkeys in this group also showed near‑normal tendon shape on palpation and more even weight‑bearing at rest. Combined, these findings suggest that pairing a long‑acting platelet‑rich scaffold with stem‑cell‑derived exosomes can guide tendon repair away from brittle scarring and toward a more functional rebuild. The authors caution that longer studies in naturally occurring injuries are needed, but the work points toward a promising biologic strategy to help high‑risk tendons in equine and possibly human athletes heal stronger and last longer.
Citation: Najeb, M., Samy, A., Rizk, A. et al. Mesenchymal stem cell derived exosomes and injectable platelet-rich fibrin enhance SDFT healing in a donkey tendonitis model. Sci Rep 16, 12013 (2026). https://doi.org/10.1038/s41598-026-44967-7
Keywords: tendon healing, platelet-rich fibrin, stem cell exosomes, equine sports medicine, regenerative therapy