Clear Sky Science · en
Impact of high relative dose intensity on effectiveness and treatment continuity of IO-TKI therapy in Japanese advanced renal cell carcinoma
Why this research matters for patients
Kidney cancer that has spread beyond the kidney is difficult to treat, but new drug combinations have improved survival. Doctors now often pair immune-based medicines, which help the body’s defenses attack tumors, with targeted drugs that block growth signals in cancer cells. This study asks a simple but crucial question for Japanese patients: is “more” of the targeted drug always better, or can very high dosing backfire by causing side effects that force people to stop treatment too soon?
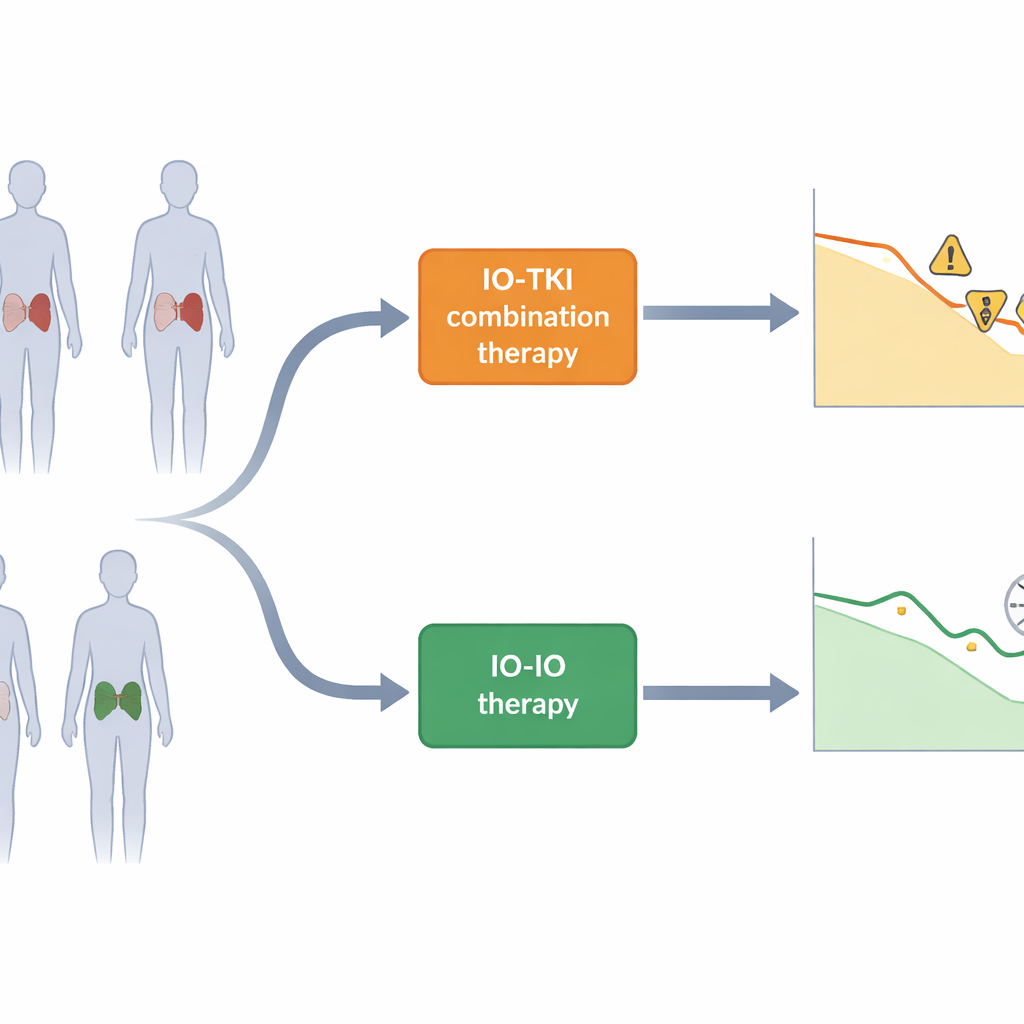
Two modern treatment paths
The researchers looked back at the records of 145 Japanese patients with advanced renal cell carcinoma who received modern first-line treatment at four hospitals. One group received a mix of immune therapy and a targeted tablet drug called a tyrosine kinase inhibitor (IO–TKI). The other group received a dual immune therapy without the tablet drug (IO–IO). Both approaches are now standard options worldwide. The team compared how well each strategy worked in everyday practice, focusing on how long patients lived without the cancer growing and how long they lived overall.
Short-term gain versus long-term balance
Patients given IO–TKI therapy had better short-term tumor control than those on IO–IO treatment. Their cancers were more likely to shrink or at least remain stable, and the period before the disease worsened tended to be longer. However, when the researchers looked at overall survival, the advantage disappeared: people in both treatment groups lived for a similar length of time. This suggested that the early benefits of the IO–TKI combinations might be offset by other factors over the long run, prompting the team to examine how dosing of the tablet drugs might be influencing outcomes.
When higher dose can hurt
The scientists focused on “relative dose intensity,” a measure of how close a patient’s actual tablet dosing stayed to the planned full dose over time. They divided IO–TKI patients into those who maintained a high dose (at least 80% of the planned level) and those whose dose was kept lower. Surprisingly, patients who stayed at the highest dose tended to have worse overall survival than those whose dose was reduced. High-dose patients also had their treatment stopped because of side effects sooner than those on more moderate dosing, even though both groups enjoyed similar periods before the cancer progressed. In other words, pushing the dose too hard seemed to raise the risk of serious problems without delivering extra long-term benefit.
Finding a “just right” dose range
To refine this picture, the team further split IO–TKI patients into three bands of dose intensity: below half of the planned dose, between half and four-fifths, and at least four-fifths. Patients in the middle band, who stayed between about 50% and 80% of the planned dose, tended to do best overall. They enjoyed good control of their cancer and could stay on treatment longer before side effects forced them to stop. Those below 50% may not have received enough medicine to control the disease well, while those at 80% or more were more likely to run into serious side effects that cut their therapy short.
What this means for patients and doctors
This study suggests that for Japanese patients receiving an IO–TKI combination for advanced kidney cancer, aiming for the very highest tablet dose may not be the safest or most effective strategy. Instead, carefully adjusting the dose so that it remains in a moderate range can help balance cancer control with manageable side effects, allowing people to stay on treatment longer. While larger, prospective studies are needed to confirm the exact “sweet spot,” the message for clinical practice is clear: thoughtful dose tuning, rather than simply maximizing the amount of drug, may give patients the best chance at longer, more tolerable survival.
Citation: Tasaki, Y., Hamamoto, S., Ikoma, H. et al. Impact of high relative dose intensity on effectiveness and treatment continuity of IO-TKI therapy in Japanese advanced renal cell carcinoma. Sci Rep 16, 13305 (2026). https://doi.org/10.1038/s41598-026-43607-4
Keywords: advanced kidney cancer, immunotherapy, targeted therapy, drug dosing, treatment side effects