Clear Sky Science · en
CCR7 immune cell receptor expression in inflammatory breast cancer
Why this study matters
Inflammatory breast cancer is one of the rarest yet most aggressive forms of breast cancer. It tends to spread early through the skin’s tiny lymph vessels, leading to rapid breast swelling and redness. This study asks a simple but important question: is a specific "homing" switch on cells, called CCR7, helping inflammatory breast cancer cells find and invade these lymph channels and nearby lymph nodes? If so, that switch could become a new bullseye for future targeted therapies.
A dangerous pattern of spread
Unlike more familiar breast cancers that usually form a distinct lump, inflammatory breast cancer often appears as a painful, swollen, and discolored breast. Under the microscope, the skin’s lymph channels are packed with clusters of tumor cells. Because these vessels connect directly to lymph nodes and the wider body, understanding what draws cancer cells into this network is crucial for understanding why this disease spreads so quickly and is harder to cure.
The cell “homing” switch CCR7
CCR7 is a receptor normally found on certain immune cells, helping them travel through lymph vessels to lymph nodes, where immune responses are coordinated. It acts like a lock that recognizes chemical “keys” released in lymphatic tissues. Previous research in other cancers suggested that when tumor cells start using this same lock-and-key system, they can more easily migrate into lymph vessels and seed distant sites. However, CCR7’s role in inflammatory breast cancer had not been carefully mapped out before this study.
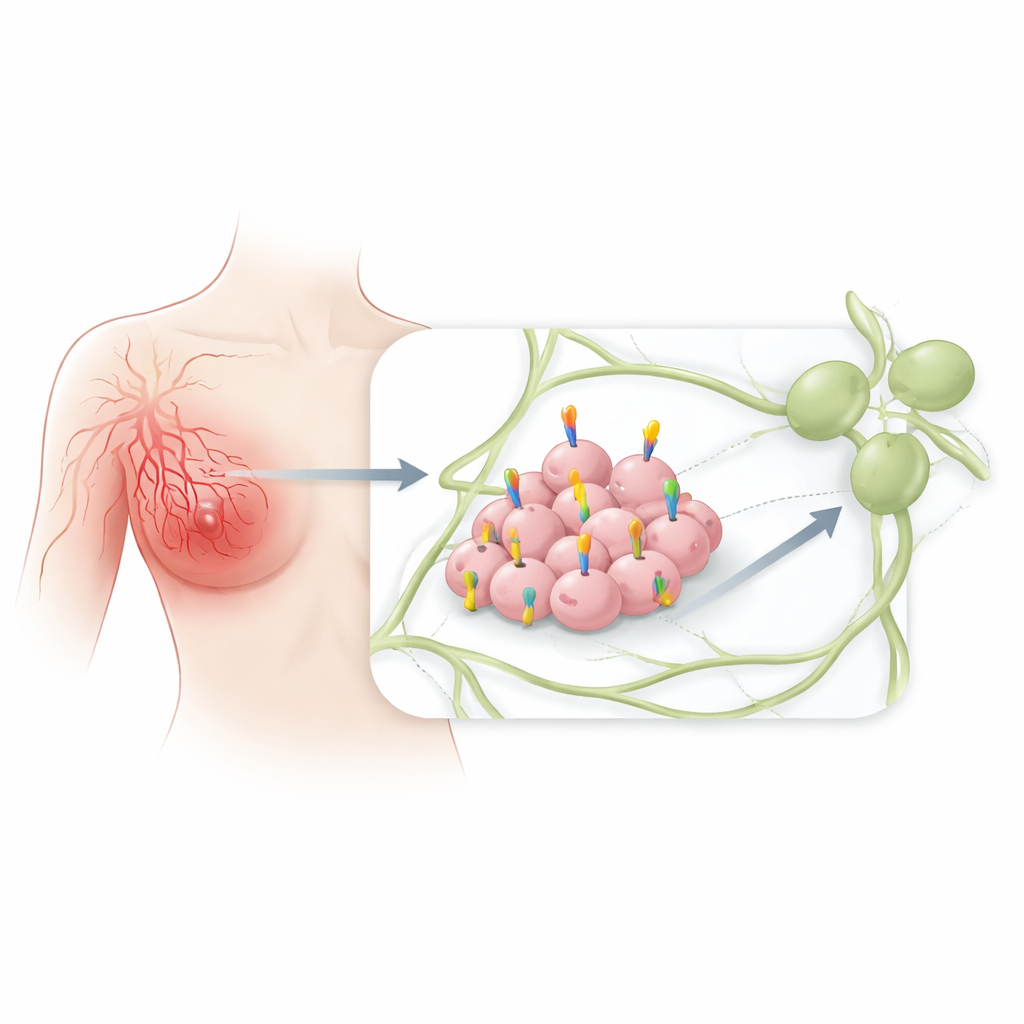
Tracking CCR7 in models and patient samples
The researchers first looked at experimental models. In mice whose breast tissue had been primed by a high-fat diet and changes in breastfeeding patterns—conditions that increased inflammation and lymphatic activity—they found higher levels of CCR7-related signals in the mammary gland. They then examined breast cancer cell lines in the lab and found that both inflammatory and non-inflammatory breast cancer cells made CCR7 protein, suggesting this receptor is widely available to tumor cells. Next, using a large international database of tumor gene profiles, they compared 137 inflammatory breast cancers with 252 non-inflammatory cases. CCR7 gene activity was significantly higher in inflammatory tumors, and so was activity of its main chemical partner, CCL21, which is abundant in lymphatic cells.
Which tumors show the strongest signal
Not all inflammatory breast cancers are the same. When the team grouped tumors by common clinical markers, CCR7 gene activity was especially high in those lacking estrogen receptors and in those that fell into HER2-positive or basal-like categories—subtypes already known to have worse outcomes. CCL21, the main partner signal for CCR7, also tended to be higher in HER2-positive tumors. However, when the scientists looked at survival data across the large dataset, they did not find a simple link between higher CCR7 or CCL21 gene levels and overall survival, hinting that how and where the protein is used on the cell surface may matter more than gene levels alone.
Seeing CCR7 directly in tumor tissue
To test what this looks like in real tumors, the researchers stained tissue microarrays made from inflammatory breast cancer mastectomy samples. Nearly every sample with enough tumor tissue showed CCR7 on the cancer cells, most often as a strong, continuous ring along the cell surface. Many tumors had nearly all of their cells stained. This widespread presence supports the idea that CCR7 is part of the basic toolkit of inflammatory breast cancer cells, even if small patient numbers limited the ability to tie staining patterns to patient outcomes such as recurrence or survival.
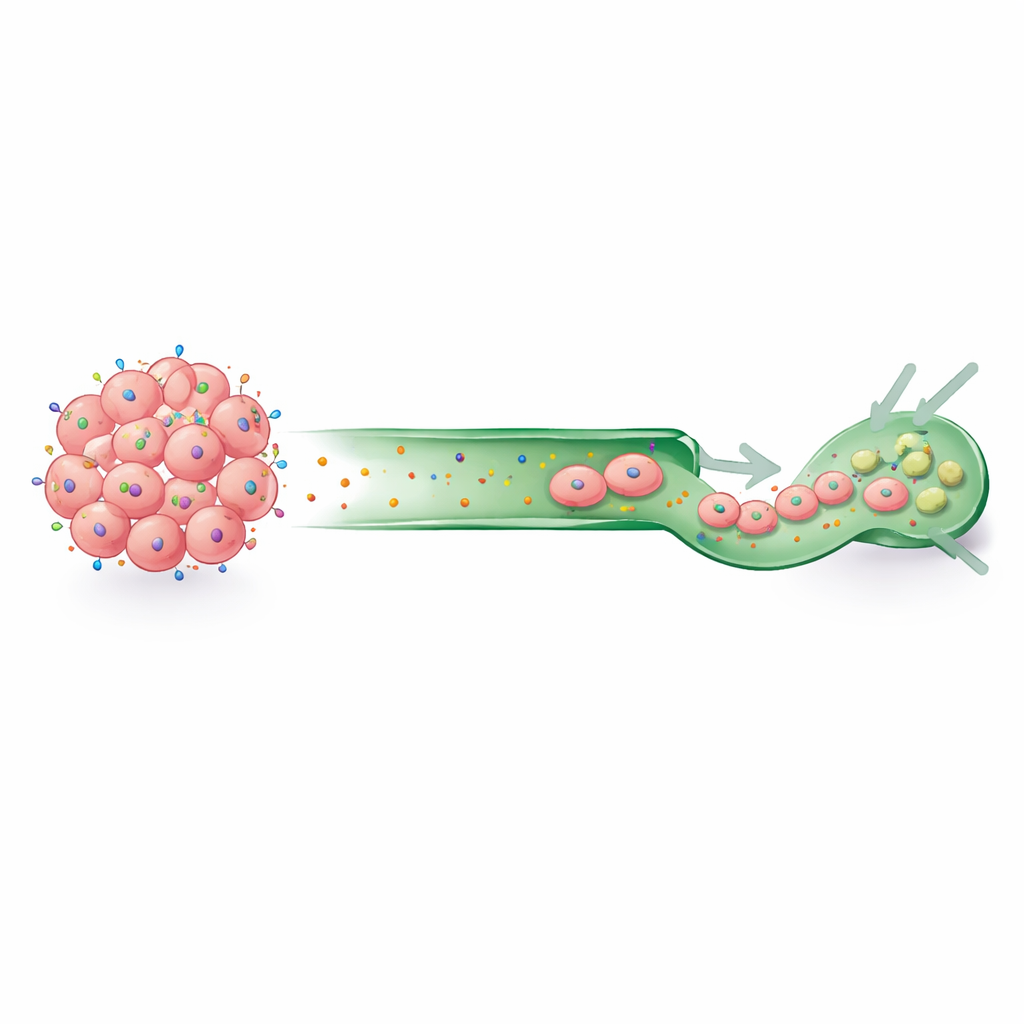
What this means for future treatments
Taken together, the findings paint CCR7 as both common and particularly active at the gene level in inflammatory breast cancer, especially in harder-to-treat subtypes. Its partnership with CCL21 and its known role in lymph vessel homing suggest it may help cancer cells invade and travel through lymph channels. The study highlights CCR7 as a promising candidate for targeted therapies, such as antibody–drug conjugates that deliver toxic payloads directly to CCR7-bearing cells. While more work is needed in larger patient groups to confirm how CCR7 influences spread and outcomes, this research lays the groundwork for turning a key driver of lymphatic invasion into a potential therapeutic vulnerability.
Citation: Chen, J.H., Balema, W., Krishnamurthy, S. et al. CCR7 immune cell receptor expression in inflammatory breast cancer. Sci Rep 16, 13513 (2026). https://doi.org/10.1038/s41598-026-43437-4
Keywords: inflammatory breast cancer, CCR7, lymphatic spread, HER2-positive breast cancer, targeted therapy