Clear Sky Science · en
Exercise pressor reflex in Amyotrophic lateral sclerosis patients
Why gentle movement still matters
Amyotrophic lateral sclerosis (ALS) gradually robs people of their ability to move, speak, and breathe on their own. For patients in the most advanced stages, even simple voluntary exercise is no longer possible, and families and clinicians often wonder whether any kind of physical therapy can still benefit the body. This study asks a basic but important question: when caregivers move the limbs of people with late-stage ALS, does the body still react in ways that support the heart and blood vessels? The answer sheds light on how much of the nervous system remains functional, even when muscles can no longer obey the brain’s commands.
Understanding the body’s built-in exercise response
In healthy people, any physical activity, from climbing stairs to squeezing a handgrip, triggers a rise in heart rate and blood pressure. Part of this response comes from sensors inside the muscles that detect stretching and movement and send signals through nerves to the brainstem, which then boosts circulation. This automatic loop is sometimes called a “pressor reflex.” In ALS, the nerve cells that move muscles slowly die, but there has been debate about whether the sensory and automatic (autonomic) parts of the nervous system stay intact, especially in people who are already on ventilators and can barely move. If these systems still work, even passive movements provided by a therapist might help maintain blood flow and possibly provide other health benefits.
How the researchers tested gentle stretching
The researchers studied nine people with late-stage ALS, aged 55 to 92, all using mechanical ventilators and receiving tube feeding. Because they could not exercise on their own, the team focused on two kinds of passive movement: brief static stretching of one forearm and a short session of leg pedaling on a motorized device, where the machine moved the legs for the patient. For stretching, therapists bent the wrist to a level just below each person’s pain threshold and held it for one minute. Throughout these sessions, the team continuously measured beat-to-beat blood pressure from a finger sensor and calculated heart rate and average arterial pressure. When the finger method did not work well, they added traditional arm cuff readings around rest, movement, and recovery.
What happened inside the circulation
During gentle forearm stretching below the pain threshold, patients showed clear increases in heart rate and in all major blood pressure measures compared with rest. Average arterial pressure rose by about 10 millimeters of mercury, a change similar in size to what has been reported in young healthy volunteers undergoing the same type of stretching. These changes faded back toward baseline during the recovery period. In contrast, passive leg pedaling, even though it lasted three minutes, did not produce significant shifts in heart rate or blood pressure. This pattern—stronger responses to arm stretching than to leg movement—also echoes findings in healthy participants, suggesting that the basic reflex pathways in the forearm muscles of these ALS patients are still operating much as they do in people without the disease.
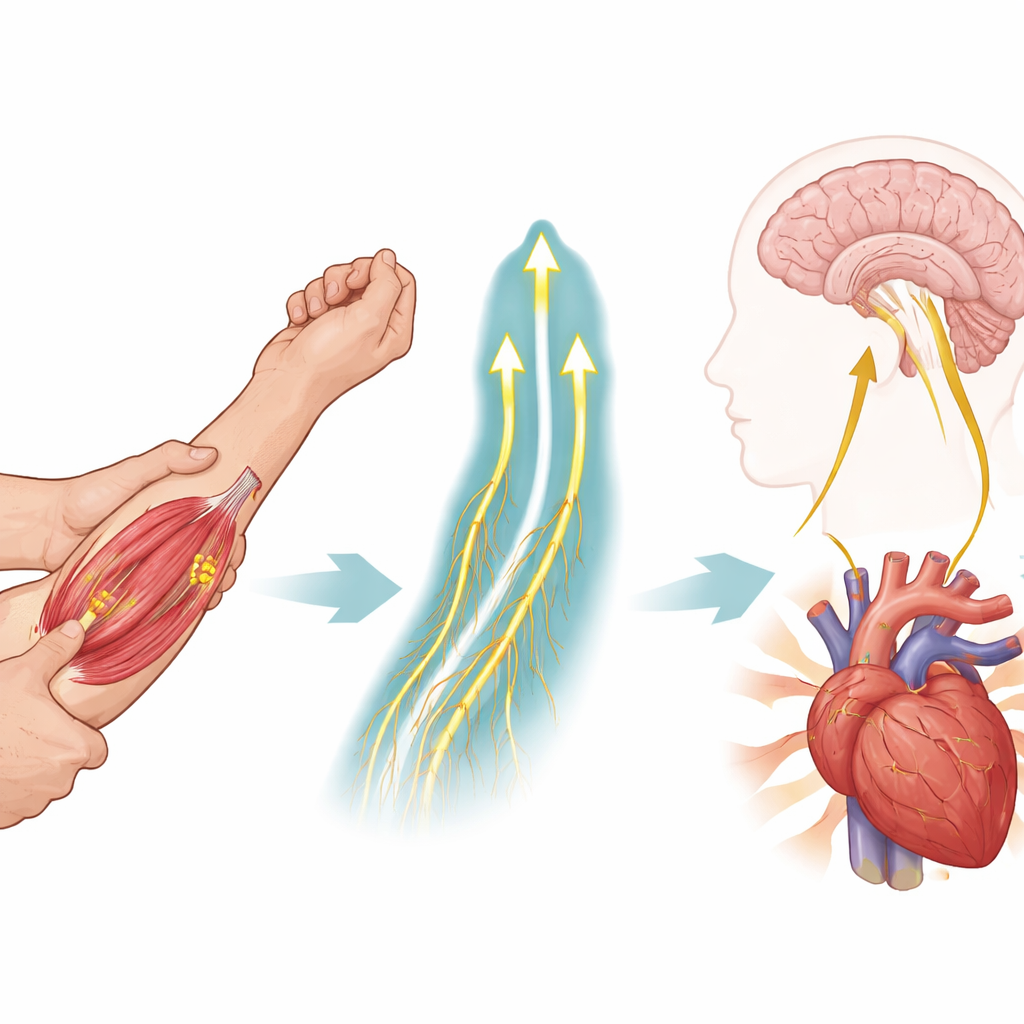
What this reveals about the remaining nerves
The results indicate that the nerve fibers that sense mechanical changes in muscle, and the autonomic circuits that control blood vessel tightening, are at least partly preserved in late-stage ALS. Despite severe muscle wasting and almost no voluntary movement, the patients’ bodies could still detect a simple stretch of the forearm and translate it into a boost in blood pressure. The researchers note that this does not mean all automatic functions are normal in ALS; other studies show disruptions in different parts of the autonomic system. However, it does point to a specific reflex arc—from muscle sensors through the spinal cord and brainstem to the blood vessels—that appears to remain functional even after many years of disease.
Why this matters for care and comfort
For families and clinicians caring for people with advanced ALS, these findings offer a measure of reassurance. Even when a person can no longer move or breathe without machines, gentle passive stretching can still “speak” to the body’s internal control systems and trigger a healthy circulatory response. While this small study cannot prove long-term benefits or replace other therapies, it supports the idea that carefully guided passive exercise is more than just joint maintenance—it taps into surviving nerve pathways that help keep the heart and blood vessels responsive. In other words, the nervous system in ALS may be more resilient in certain respects than the outward loss of movement suggests.
Citation: Saeki, Y., Nakamura, N. & Hayashi, N. Exercise pressor reflex in Amyotrophic lateral sclerosis patients. Sci Rep 16, 12804 (2026). https://doi.org/10.1038/s41598-026-43367-1
Keywords: amyotrophic lateral sclerosis, passive exercise, blood pressure, autonomic nervous system, mechanoreflex