Clear Sky Science · en
DUSP6 promotes motility, invasion, and tumorigenicity of thyroid cancer cells via IL8-induced neutrophil extracellular traps
Why this thyroid cancer study matters
Thyroid cancer is usually highly treatable, but a fraction of tumors become aggressive, spread to other parts of the body, and stop responding well to standard therapies. This study looks under the microscope at how certain molecules in and around the tumor help cancer cells move, invade, and grow. By uncovering this hidden support system, the researchers point to new weak spots that future drugs might target to keep thyroid cancer from spreading.
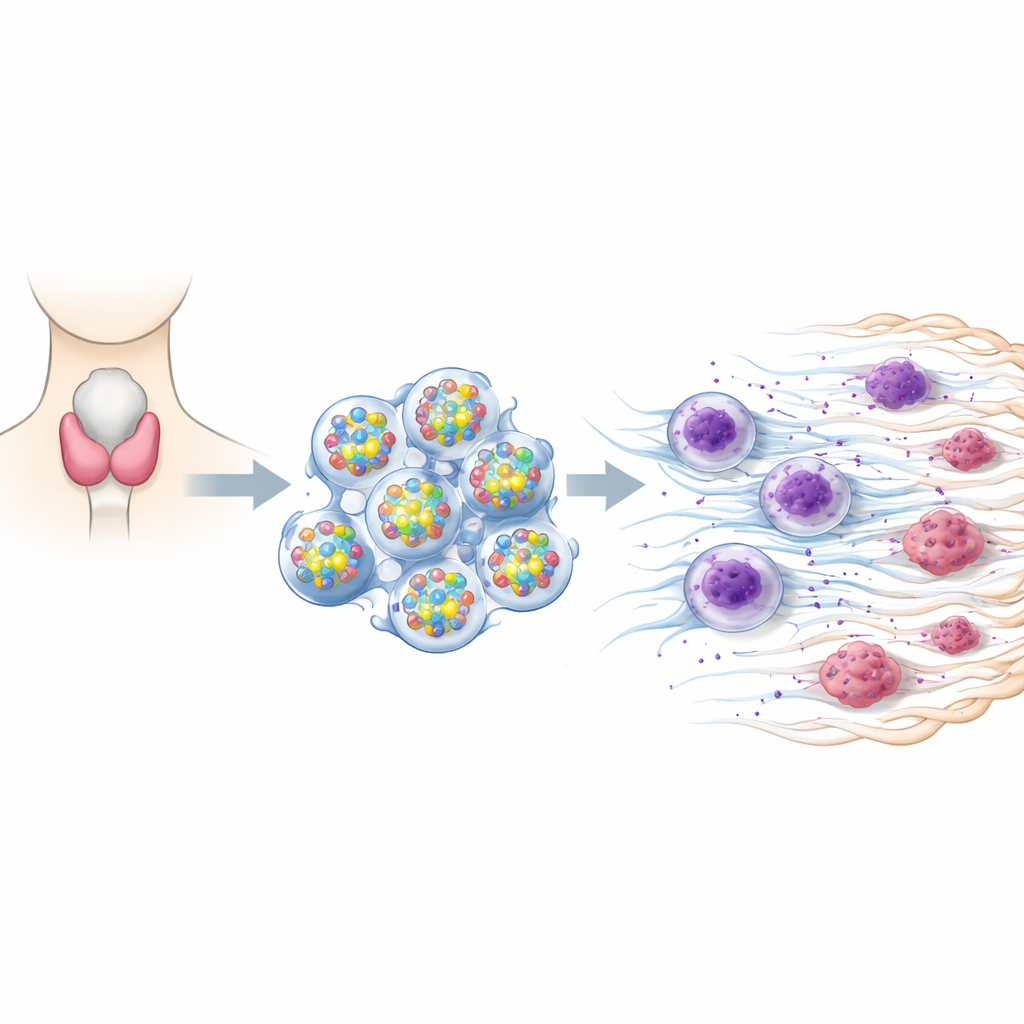
A signaling switch that goes into overdrive
The team focused on a protein called DUSP6, which acts like a switch inside cells that can tune growth signals up or down. Using patient samples from papillary thyroid carcinoma, the most common form of thyroid cancer, they compared tumor tissue with nearby healthy thyroid tissue. They found that tumors carried much higher levels of DUSP6. Importantly, the amount of DUSP6 in each patient’s tumor rose and fell in step with two other markers: IL-8, a molecule that attracts immune cells, and PAD4, a marker linked to special webs released by immune cells. This pattern suggested that DUSP6 might be helping to create an environment that favors tumor spread.
Pushing cancer cells to grow, move, and invade
To see what DUSP6 actually does inside thyroid cancer cells, the researchers used two human thyroid cancer cell lines grown in the lab. They artificially boosted DUSP6 in some cells and silenced it in others. When DUSP6 was turned up, cancer cells multiplied faster, moved more quickly across a surface, and more easily invaded through a gel that mimics tissue. These cells were also less likely to undergo programmed cell death. When DUSP6 was dialed down, the opposite happened: growth slowed, movement and invasion dropped, and more cells died. At the same time, DUSP6 changed the balance of proteins on the cell surface, nudging cells toward a looser, more mobile state that is commonly seen when cancers metastasize. The boosted cells also produced more IL-8, linking this internal switch to a powerful signal that can influence the surrounding immune system.
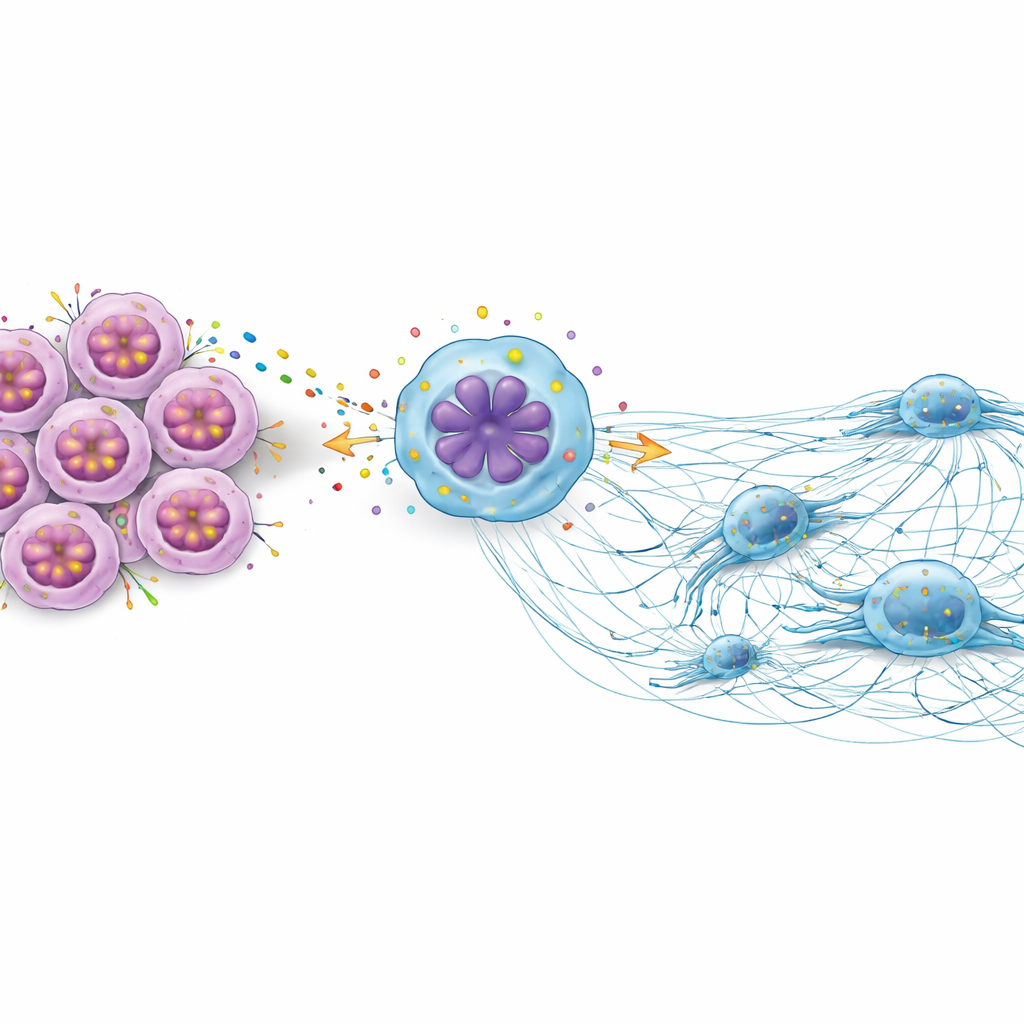
Immune cell webs that help cancer spread
The study then turned to a lesser-known player in cancer: neutrophil extracellular traps, or NETs. These are sticky, web-like structures made of DNA and proteins that certain white blood cells release. Although they normally help trap invading microbes, NETs can also create tracks along which cancer cells can travel. In laboratory dishes, when thyroid cancer cells were exposed to NETs, they became even more mobile and invasive. However, when DUSP6 or IL-8 was knocked down, this NET-driven boost in movement and invasion was significantly reduced. In other words, DUSP6 and IL-8 made tumor cells more responsive to these harmful webs.
How tumor signals reshape nearby immune cells
To dig deeper into the chain of events, the researchers studied neutrophils, the very immune cells that form NETs. When they increased DUSP6 levels in these cells, markers of NET formation went up; when they lowered DUSP6 or blocked IL-8, those markers went down. Additional staining experiments confirmed that DNA-based webs and associated proteins were more abundant when DUSP6 was high and IL-8 signaling was intact. These findings suggest a loop in which thyroid cancer cells with elevated DUSP6 produce more IL-8, which in turn encourages neutrophils to spin out more NETs—creating a physical and chemical environment that helps cancer cells move and invade.
Slowing tumor growth in animals
The team tested the real-world impact of this pathway in mice. They implanted thyroid cancer cells under the skin of mice and used genetic tools to reduce DUSP6 in some of the tumors. Tumors with lower DUSP6 grew more slowly and ended up smaller and lighter than those in control animals. Under the microscope, these tumors were less densely packed with cancer cells and showed protein patterns consistent with a less invasive state. Tumor tissue from these mice also had reduced levels of IL-8 and NET-related markers, echoing the cell-culture findings and supporting the idea that DUSP6 drives a pro-metastatic environment.
What this means for future thyroid cancer treatment
Put simply, the study shows that a protein switch inside thyroid cancer cells, DUSP6, helps tumors spread by turning up IL-8, which then prompts immune cells to cast sticky NETs that cancer cells can exploit. Blocking DUSP6, IL-8, or NET formation disrupted this chain and slowed tumor growth in experiments. While more work is needed, including in-depth animal studies and eventual clinical trials, these results highlight a promising trio of targets that could one day help keep aggressive thyroid cancers from invading and metastasizing.
Citation: Xiao, W., Luo, L., Yang, Y. et al. DUSP6 promotes motility, invasion, and tumorigenicity of thyroid cancer cells via IL8-induced neutrophil extracellular traps. Sci Rep 16, 12575 (2026). https://doi.org/10.1038/s41598-026-43233-0
Keywords: thyroid cancer, DUSP6, interleukin-8, neutrophil extracellular traps, metastasis