Clear Sky Science · en
Agreement and potential for arithmetic adjustment of anterior segment measurements across IOLMaster 700, Pentacam HR, and Sirius
Why eye scan differences matter
When people prepare for cataract or vision correction surgery, surgeons rely on detailed scans of the front of the eye to choose and size artificial lenses. Even tiny mismatches between scanners can nudge results away from the sharp vision patients expect. This study asks a practical question: when three popular eye imaging machines give slightly different numbers, which differences truly matter, and can simple math bring some of those readings into line?
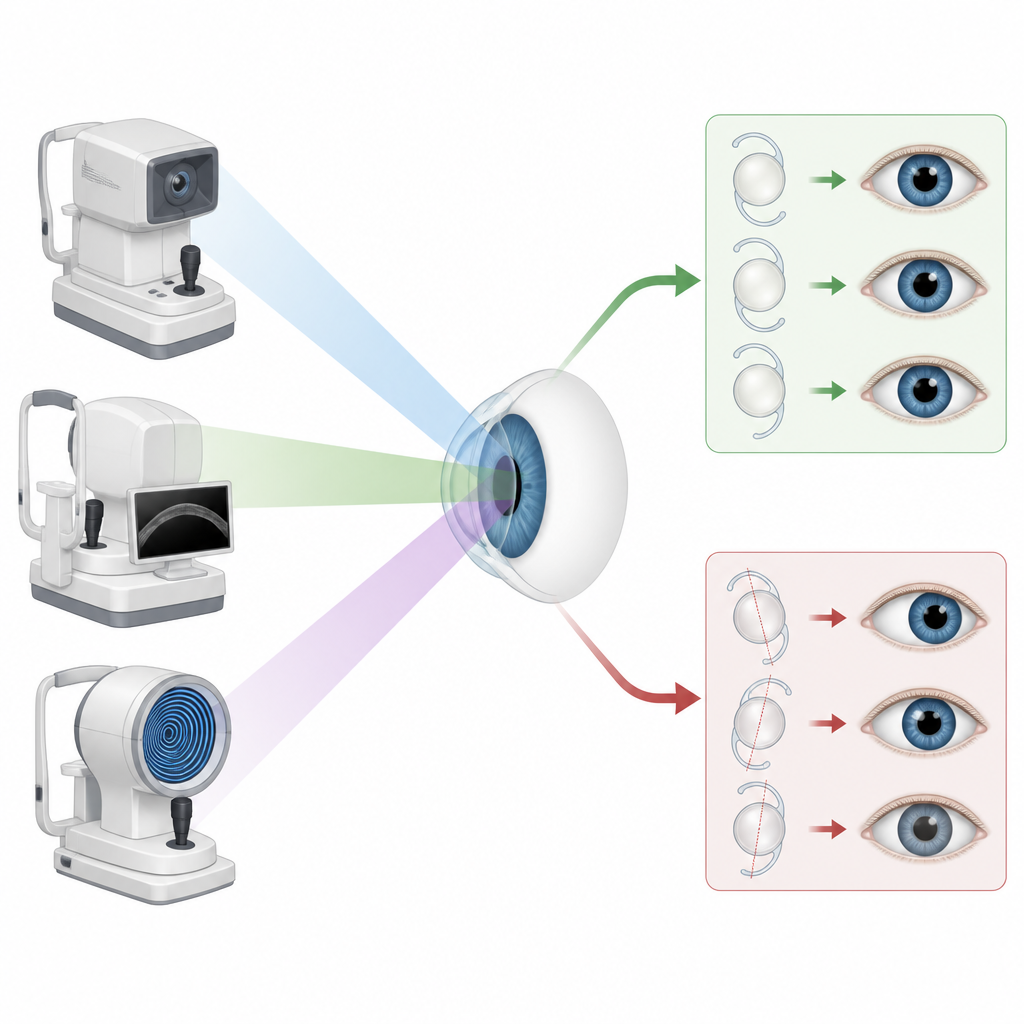
Three machines, one eye
The researchers focused on three widely used devices that measure the clear front window of the eye, the cornea, and nearby structures. One uses a swept light beam to build cross-sectional pictures, while the other two rely on rotating cameras and special rings of light. All three report key values that guide surgery planning, such as how steeply the cornea curves, how thick it is, how deep the front chamber of the eye is, and the horizontal “white-to-white” distance across the visible colored part of the eye. The team examined 111 healthy eyes, all from people being assessed for laser vision correction, and recorded the same measurements on each device under tightly controlled conditions.
Checking if numbers agree
To see how well the machines matched, the authors compared both the overall spread of values and how closely readings for each individual eye lined up across devices. They used statistical tools that distinguish between random scatter and a fixed, repeatable shift. A small fixed shift may be less worrisome than wide scatter, because it opens the door to a simple correction: if one device always reads a little lower or higher than another, a constant amount can be added or subtracted to bring its numbers closer into step.
What matched and what did not
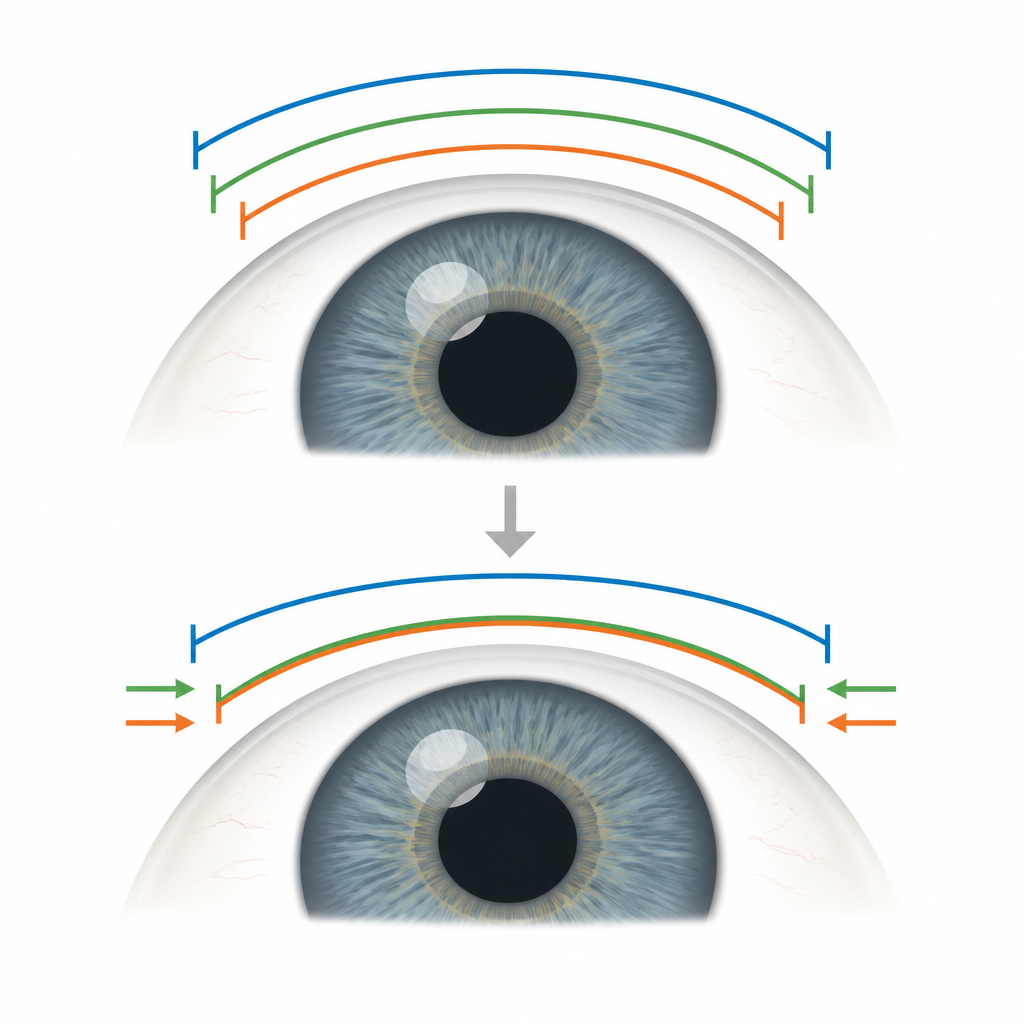
Most measurements showed excellent agreement. The thickness of the central cornea and the depth of the front chamber were very similar from one machine to the next, with differences so small that they would change lens power choices by less than a quarter of a diopter, a commonly used threshold for clinical relevance. Corneal curvature values were also strongly correlated, but the spread of differences was wide enough that swapping these readings between devices for an individual eye could shift the final lens choice in a meaningful way. The largest trouble spot was the white-to-white distance, a measure often used to select the size of certain implantable lenses that sit in front of the natural lens.
When a simple shift helps
For the white-to-white distance, the three machines did not agree well at first glance. However, a closer look revealed that two of them tended to differ by a nearly constant amount across the full range of eyes. This pattern suggests a systematic offset rather than random noise. By adding a fixed correction of about a third of a millimeter to one device’s readings, the agreement between those two systems jumped to an excellent level, even though the third machine still behaved differently. In other words, for these two scanners, a simple arithmetic tweak could make their white-to-white values practically interchangeable, while such a fix did not work for the third.
What this means for patients
For people undergoing cataract or implantable lens surgery, this study offers a reassuring message with a cautionary note. Surgeons can generally trust measurements of corneal thickness and front chamber depth from any of these three machines for choosing lens power, because their differences are small enough to have little impact on vision outcomes. By contrast, corneal curvature numbers and the horizontal white-to-white measurement, especially when switching between certain devices, should not be mixed freely from one scan to another for the same eye. In some cases a simple, well-tested adjustment may help, but doctors still need to treat each device’s numbers with awareness of its built-in biases rather than assuming all scanners speak exactly the same language.
Citation: Doostparast, A., Semnani, F., Ghandhari, M. et al. Agreement and potential for arithmetic adjustment of anterior segment measurements across IOLMaster 700, Pentacam HR, and Sirius. Sci Rep 16, 15121 (2026). https://doi.org/10.1038/s41598-026-42204-9
Keywords: cataract surgery, corneal measurements, ocular biometry, implantable lenses, device comparison