Clear Sky Science · en
Intra and inter-network functional connectivity among long-Covid patients with ongoing disease duration
Why lingering Covid symptoms matter for the brain
Many people who recover from COVID-19 continue to struggle with fatigue, brain fog and trouble concentrating for months or even years. These long-lasting problems, often grouped under the term long-Covid, raise a pressing question: what is happening inside the brain as time goes on? This study uses advanced brain scanning to examine how the brains of long-Covid patients with shorter versus longer illness duration differ, and whether those differences might reflect damage or the brain’s own attempts to cope and adapt.
Looking at the resting brain
Instead of asking people to perform tasks in a scanner, the researchers used resting-state functional MRI, which measures how different brain regions naturally “talk” to each other when a person is lying still with eyes closed. Patterns of synchronized activity across regions form large-scale networks involved in attention, memory, movement and daydreaming, among others. The team studied 39 adults with long-Covid who still had symptoms at least three months after infection. Using a data-driven method, they identified 17 such networks and then compared people whose symptoms had lasted roughly 9 months to those whose symptoms had persisted for almost 28 months.
Same symptoms, different brain wiring
Surprisingly, the two groups looked very similar outside the scanner. They did not differ in age, education, number of symptoms, performance on a broad range of thinking tests, or measures of mood and fatigue. The major difference was simply how long they had been ill and, relatedly, vaccination status: most of the short-duration group had been vaccinated before infection, whereas most in the long-duration group had not, a factor the authors note as an important limitation. Yet when the researchers examined brain connectivity, they found clear contrasts between the groups that did not show up in standard clinical measures.
Networks that grow stronger inside
Within several key networks, people with longer-lasting long-Covid showed stronger internal connections. These included networks that underlie focusing attention, selecting important information, guiding movement, processing visual input and supporting self-related thoughts. In other words, regions within each of these circuits were more tightly linked in the long-duration group. Because the two groups performed similarly on cognitive and psychological tests, the authors suggest that these changes might represent the brain’s way of stabilizing function under ongoing stress: by reinforcing communication inside essential circuits, the brain may preserve day-to-day abilities despite lingering illness.
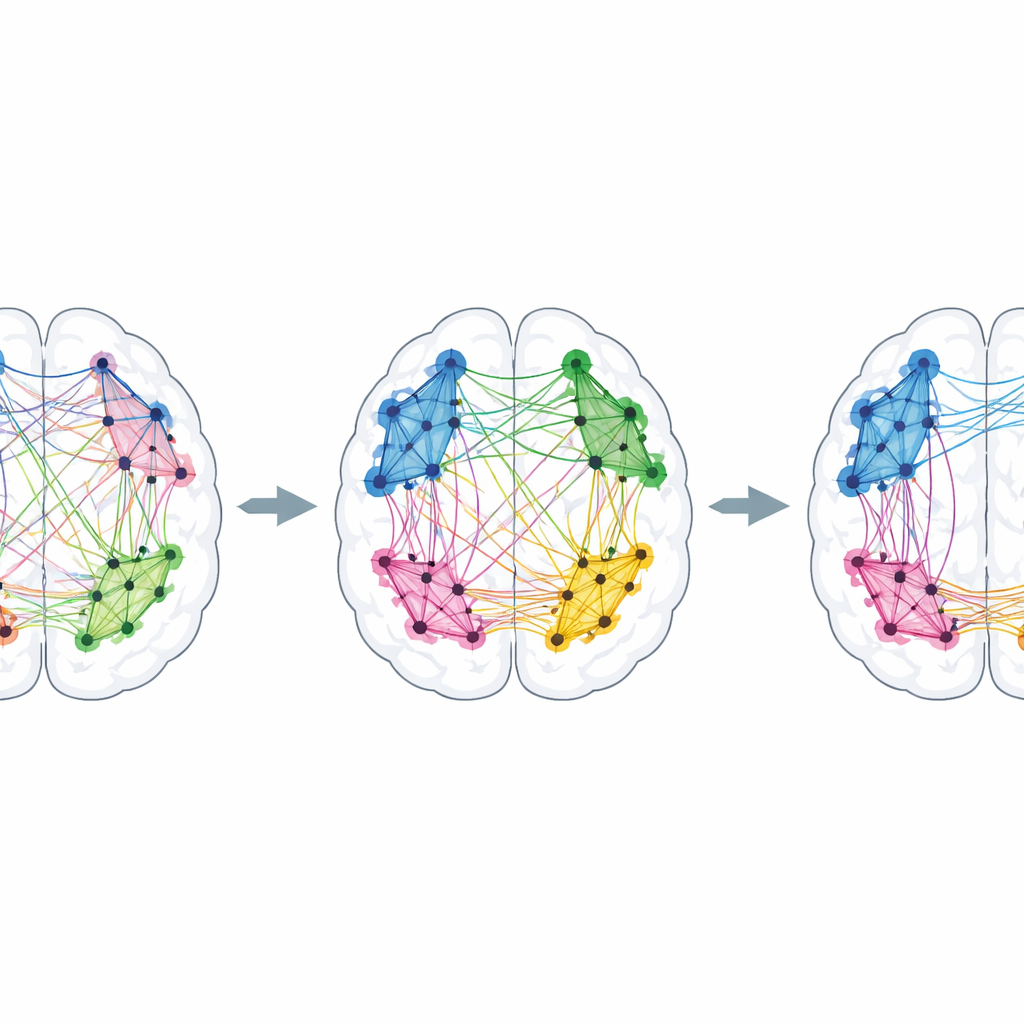
Networks that loosen their ties between each other
The picture looked different when the team examined how these networks interacted with one another. In those with longer disease duration, connections between several major systems were weaker, especially links involving the default mode network—a set of regions active during inward-focused thought—and networks that support goal-directed, outward-focused attention and control. Traditionally, such reduced cross-talk between networks has been seen as a sign of less efficient processing. But the authors note that in some situations, separating networks can actually help: when a person needs to focus, quieter communication from the daydreaming network can reduce interference and sharpen task performance.
What the findings may mean for people with long-Covid
Putting these pieces together, the study paints long-Covid not simply as ongoing damage, but as a condition in which the brain’s wiring gradually shifts. As months turn into years, networks important for thinking and everyday function appear to strengthen internally while their links to other systems relax. The authors interpret these patterns cautiously as possibly adaptive—changes that may help maintain stable thinking and daily functioning in the face of a prolonged illness. At the same time, they stress that the work is cross-sectional, lacks a healthy control group and is complicated by differences in vaccination, so it cannot prove whether these brain changes are ultimately helpful, harmful, or both. Still, the results highlight that even when symptoms and test scores look similar on the surface, the brains of long-Covid patients with different illness durations may be working in subtly different ways.
Citation: Leitner, M., Ropele, S., Fellner, M. et al. Intra and inter-network functional connectivity among long-Covid patients with ongoing disease duration. Sci Rep 16, 12811 (2026). https://doi.org/10.1038/s41598-026-42000-5
Keywords: long COVID, brain connectivity, resting-state fMRI, cognitive function, default mode network