Clear Sky Science · en
Toward robust automated cardiovascular arrhythmia detection using self-supervised learning and 1-dimensional vision transformers
Why smarter heart monitors matter
Heart disease is the world’s leading killer, and doctors now record hundreds of millions of heart tracings, or ECGs, every year. These squiggly lines can reveal dangerous rhythm problems, but having experts review each one by hand is impossible. This paper explores how modern artificial intelligence can learn directly from huge collections of ECGs—most of them never labeled by a human—to recognize abnormal rhythms more accurately, more reliably, and fast enough for real-time monitoring on everyday devices.
Learning from oceans of unlabeled heartbeats
Traditional computer systems for reading ECGs need many carefully labeled examples and still struggle when confronted with noisy, real-world data. The authors instead tap into a massive resource that hospitals and wearable devices already generate: millions of raw ECG recordings that have never been annotated. They design a way for an AI model to teach itself the patterns of normal and abnormal heart activity by predicting missing pieces of the signal, a training style known as self-supervised learning. By first mastering the general “language” of heartbeats from 8.2 million unlabeled recordings, the system can later be fine-tuned with a much smaller set of expert-labeled cases to identify many different rhythm problems.
Turning heartbeat lines into patches the model can understand
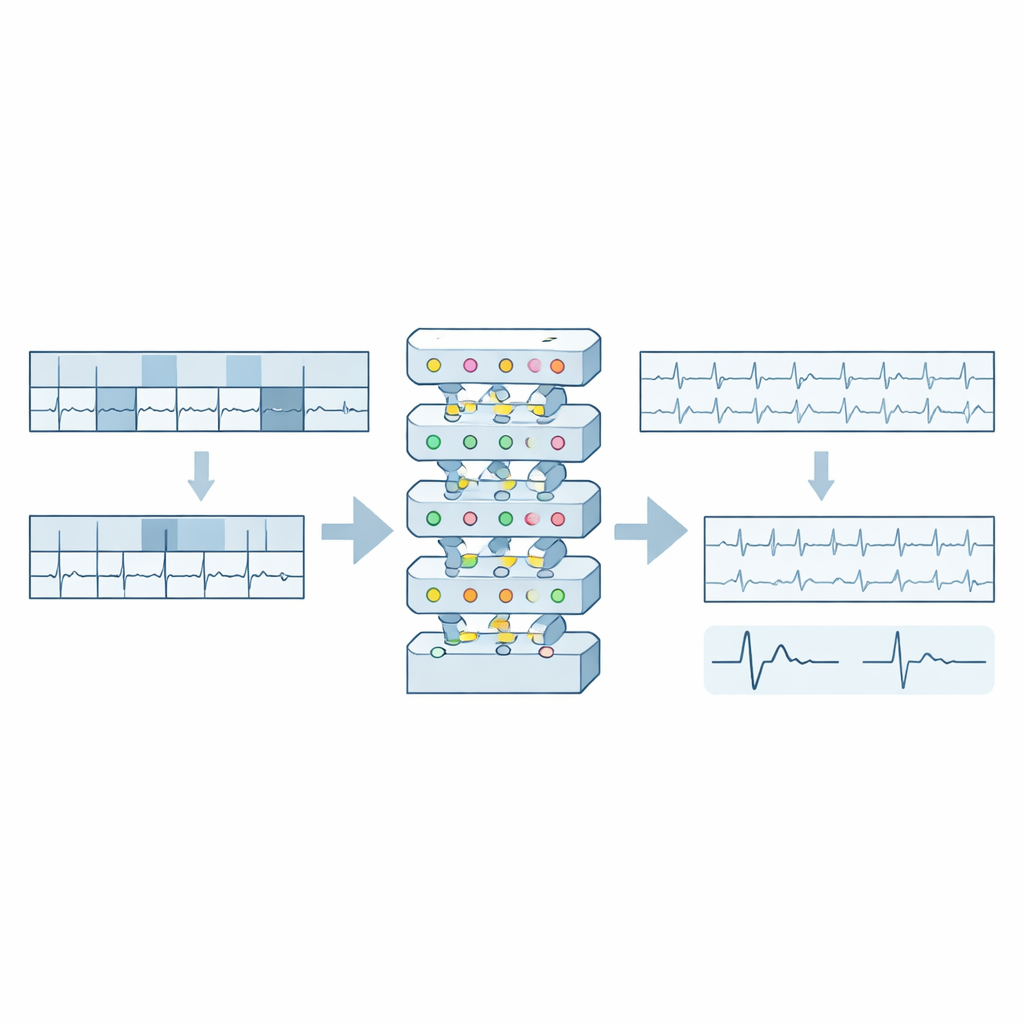
Most earlier approaches converted ECG signals into pictures and then used image-based systems, which waste space and blur fine details. This work keeps the data in its natural one-dimensional form. The authors introduce PatchECG, a model that slices each 10-second ECG into small, half‑second “patches” along each lead, then hides about 40% of them. The model’s training task is to reconstruct the missing patches from the remaining context, forcing it to learn how waves and rhythms unfold over time. This strategy preserves subtle changes in the ECG that are crucial for diagnosis, such as tiny shifts in the segments associated with heart attacks, while avoiding the information loss that comes from squeezing signals into low‑resolution images.
Outperforming established methods with less computing
After self-training on unlabeled data, PatchECG is fine‑tuned for several real diagnostic tasks: recognizing dozens of rhythm and structural problems in a widely used benchmark dataset, combining multiple public datasets into the largest labeled ECG collection to date, and spotting a dangerous type of heart attack called STEMI. Across these tests, PatchECG matches or surpasses strong existing systems, including sophisticated recurrent networks and image-based transformers, while using about one‑fifth of the computing time of a leading rival. The model is particularly impressive in how consistent its predictions are across different patient groups and datasets, with much tighter uncertainty ranges than older approaches. This stability is important for building trust in tools that might eventually guide urgent treatment decisions.
Handling messy data and imbalanced conditions
Real ECG datasets are far from perfect: some diagnoses are rare, many labels are uncertain or even wrong, and recordings are often contaminated by movement and electrical noise. The authors show that their self‑supervised training makes PatchECG more robust to these problems. When they analyze performance by diagnosis, they find that classes with lower expert confidence in the labels tend to be harder for the model as well, suggesting the tool could help flag questionable entries for human review. They also experiment with modern fine‑tuning techniques that update only small parts of the network and augment the data at test time. Together, these steps deliver a modest but meaningful boost—more than 2 percentage points in key accuracy measures—without inflating the computational cost.
What this means for future heart care
In simple terms, this study shows that a carefully designed one‑dimensional AI model can learn the rhythms of the heart from millions of unlabeled ECGs, then apply that knowledge to detect dangerous problems quickly and efficiently. By avoiding the detour through images, PatchECG keeps more medically relevant detail and runs faster, making it a strong candidate for use in continuous monitoring systems, from hospital beds to smartwatches. While clinical trials are still needed before deployment, the work lays a foundation for more reliable, scalable, and broadly accessible automated ECG analysis that could help catch life‑threatening arrhythmias before they become fatal.
Citation: Chatterjee, M., Chan, A.D.C. & Komeili, M. Toward robust automated cardiovascular arrhythmia detection using self-supervised learning and 1-dimensional vision transformers. Sci Rep 16, 11793 (2026). https://doi.org/10.1038/s41598-026-41549-5
Keywords: electrocardiogram, arrhythmia detection, self-supervised learning, transformer models, medical AI