Clear Sky Science · en
Radiomorphometric and texture-based mandibular bone assessment in type 2 diabetes mellitus: correlation with vitamin D, osteocalcin, and glycemic control—an analytical cross-sectional study
Why your dentist might spot more than cavities
Type 2 diabetes is usually managed by physicians, yet it quietly changes the skeleton too. This study asks a surprising question with everyday consequences: can a routine dental panoramic X‑ray of the lower jaw reveal early signs that diabetes is weakening bone, long before a major fracture occurs? By linking blood tests with detailed measurements taken from jaw images, the researchers explore whether the dentist’s chair could double as a checkpoint for overall bone health in people with diabetes.
Looking at the jaw as a window into the body
The team focused on the mandible, the lower jawbone, because it is commonly imaged when planning fillings, extractions, or implants. They enrolled 132 adults over age 35 and divided them into four equal groups: healthy men, healthy women, men with type 2 diabetes, and women with type 2 diabetes. Everyone had a panoramic radiograph taken, the wide X‑ray that shows both jaws in a single curved image. At the same visit, blood samples were collected to measure vitamin D and osteocalcin, a protein made by bone‑forming cells that is linked to both bone strength and blood sugar control.
From simple measurements to fine‑grained patterns
On each X‑ray, dentists used established indices that describe the visible thickness and shape of the lower jaw’s outer shell, or cortex. These include the Mental Index (a direct thickness measurement) and two versions of the Panoramic Mandibular Index, which relate cortical thickness to jaw height, as well as a grading scale called the Mandibular Cortical Index that classifies the cortex as smooth, mildly eroded, or severely porous. The researchers also examined the inner sponge‑like bone. They selected small square regions in different jaw areas and ran them through computer processing to calculate fractal dimension, a measure of how complex the internal lattice is, and to perform “strut” and texture analyses that capture how well the tiny bony struts are connected and how uniform the image appears.
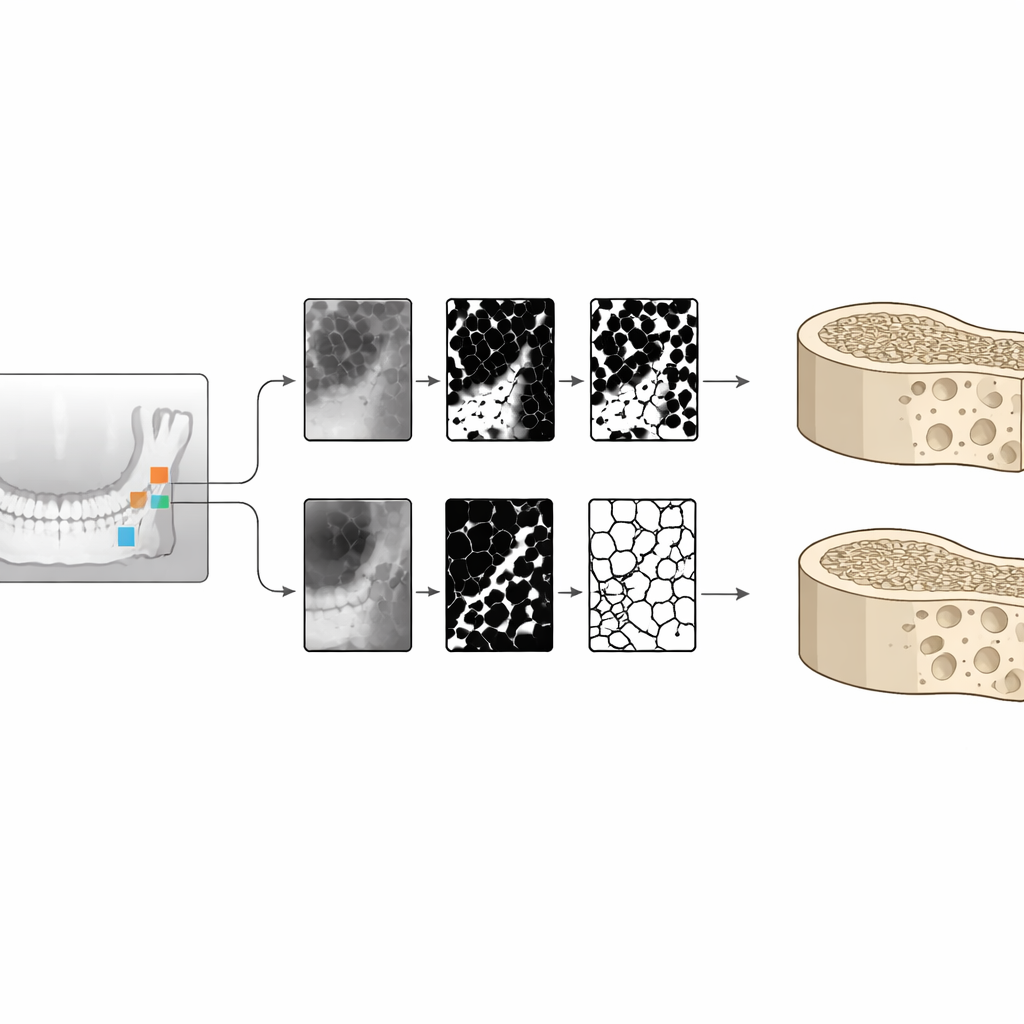
What was different in people with diabetes
Across almost all basic jaw measurements, people with type 2 diabetes showed signs of poorer bone quality than those without diabetes, even though the groups were similar in age. Diabetic participants had thinner jaw cortices and more porous‑looking outer borders, reflected in lower Mental and Panoramic Mandibular indices and higher cortical erosion grades. These changes were most striking in men with diabetes, who also showed more deterioration in the internal lattice of the jawbone. Blood tests revealed that people with diabetes tended to have lower levels of vitamin D and osteocalcin. However, once the data were adjusted for age, sex, and blood sugar levels, osteocalcin was linked more tightly to long‑term glucose control (HbA1c) than to the mere presence or absence of diabetes, suggesting that how well diabetes is managed matters for bone metabolism.
Advanced image features versus practical tools
The sophisticated computer‑derived texture measures did detect some differences between groups, particularly in diabetic men, but they added little beyond the simpler thickness and shape indices once all factors were considered together. Many of these advanced variables were so closely related to each other that they offered overlapping information. In contrast, the straightforward radiomorphometric indices—cortical thickness measurements and the three‑level cortex grading—proved to be robust, reproducible, and strongly associated with diabetes status, independent of age, sex, and blood sugar control. This means that ordinary panoramic images, interpreted with relatively simple tools, can already reveal much about how diabetes is affecting the jawbone.
What this means for everyday dental care
The study concludes that type 2 diabetes is linked to a meaningful loss of jawbone quality, both in the dense outer shell and in the inner sponge‑like structure, and that these changes can be detected on routine dental X‑rays. Because dentists frequently obtain panoramic images for treatment planning, these radiographs could serve as an “opportunistic” screening tool to flag patients whose bones may be at risk, prompting further medical evaluation. While the gold‑standard bone scan (DEXA) remains essential for diagnosis, the authors argue that simple measurements made on dental images are practical, low‑cost clues to hidden skeletal problems in people with diabetes, and deserve further testing in long‑term studies.
Citation: Benjamin Rajasekar, A., Krithika, C.L., Ganesan, A. et al. Radiomorphometric and texture-based mandibular bone assessment in type 2 diabetes mellitus: correlation with vitamin D, osteocalcin, and glycemic control—an analytical cross-sectional study. Sci Rep 16, 11523 (2026). https://doi.org/10.1038/s41598-026-41522-2
Keywords: type 2 diabetes, jawbone density, dental X-rays, osteoporosis risk, vitamin D and osteocalcin