Clear Sky Science · en
Disrupted temperature-sleep coupling mechanism in a Dravet syndrome mouse model
Why Body Heat and Sleep Matter in This Disease
Parents of children with Dravet syndrome often struggle with two constant worries: dangerous seizures and restless nights. Alongside epilepsy, many children with this condition have trouble keeping a stable body temperature and getting good-quality sleep. This study uses a mouse version of Dravet syndrome to uncover a hidden link between body temperature and sleep, and points to a small but powerful brain region that may help explain these everyday challenges.
How a Rare Epilepsy Affects the Whole Body
Dravet syndrome is caused by faults in a gene that helps brain cells generate electrical signals. While it is best known for severe, hard-to-treat seizures, people with Dravet also commonly experience problems with heart rate, breathing, temperature control, and sleep. The researchers worked with mice carrying a disease-causing mutation in the same gene, creating a model that mirrors many features seen in patients. They set out not to study seizures, but to understand why these mice, like children with Dravet, have trouble both keeping warm and sleeping soundly.
Colder Bodies and Poor Sleep Preparation
When the team measured body temperature in young mice, they found that Dravet mice ran cooler than their healthy littermates. Both groups were exposed to a gently warmed environment and then brought back to room temperature. Even though both types of mice warmed up to similar levels, the Dravet mice cooled down more and ended up with a lower temperature after returning to normal conditions. The mice were also given nesting material overnight, a simple test of a natural behavior that helps animals get ready for sleep and stay warm. Healthy mice built snug, elaborate nests; most Dravet mice built poor nests or none at all, suggesting a reduced ability or drive to carry out this basic sleep-preparation behavior. 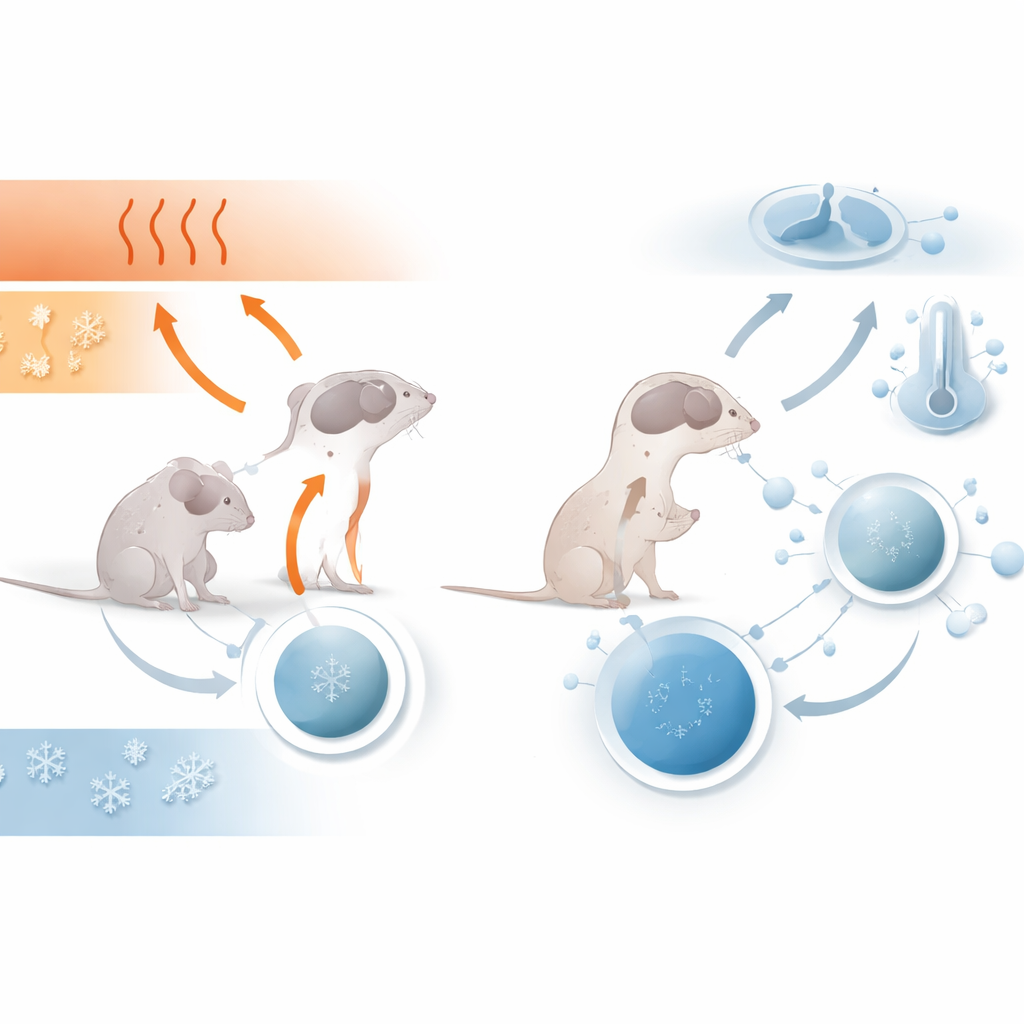
When Sleep Fails to Cool the Body
In healthy animals, drifting from wakefulness into non–rapid eye movement (NREM) sleep is usually paired with a small but important drop in core temperature and a rise in slow, rhythmic brain waves known as delta activity. Using brain recordings and tiny temperature probes, the researchers watched this transition closely. In typical mice, the onset of NREM sleep brought a clear surge in delta waves and a noticeable cooling of the body. In Dravet mice, however, delta activity during NREM barely rose above waking levels, and body temperature stayed largely unchanged during the same transitions. This pattern held true when the scientists recorded directly from the front part of the hypothalamus, a deep brain region known to coordinate both sleep and temperature control: healthy mice showed strong delta changes and cooling at sleep onset, while Dravet mice did not.
Warmth That Helps Some Mice Sleep but Not Others
Ordinarily, a slightly warm environment encourages animals, including humans, to fall asleep more easily. To test this, the team gently warmed the surroundings of older mice while recording brain activity. Healthy mice responded as expected: in the warmer setting they spent more time in NREM sleep, while their slow brain waves strengthened. Dravet mice, in contrast, showed no such sleep-promoting effect of warmth, even though the warmer temperature did not trigger extra epileptic activity. The researchers then asked whether strengthening signals in the hypothalamus could fix this. Using a viral vector, they boosted production of the faulty sodium channel protein specifically in the front hypothalamus of Dravet mice. After this targeted gene delivery, warmth once again increased NREM sleep and enhanced delta activity, much like in healthy animals.
Switching Hypothalamic Neurons Back On
To further probe the role of this brain area, the scientists turned to a chemogenetic tool that lets them temporarily boost the activity of neurons with a designer drug. They infected hypothalamic neurons with a viral construct carrying an artificial receptor, then later activated it by injecting a compound that switches these cells into a more active state. In healthy mice, warming the environment promoted NREM sleep whether or not this drug was given. In Dravet mice, however, warmth alone still failed to encourage sleep. Only when the hypothalamic neurons were artificially activated did a warm environment increase NREM sleep and strengthen slow brain waves. This showed that simply making these neurons more excitable was enough to restore the missing temperature-induced sleep response.
What This Means for Families and Future Treatments
Taken together, the study reveals that in Dravet syndrome, the normal partnership between body cooling and sleep onset is broken, and that this breakdown is closely tied to altered activity in a specific hypothalamic hub. Dravet mice stay cooler at baseline, do not show the usual drop in temperature when they fall asleep, and do not become sleepier in a warm environment—unless hypothalamic neurons are helped to fire properly. While these experiments were done in mice, they suggest that targeting this brain region and its temperature–sleep circuitry might one day help manage sleep and thermal problems that burden patients and caregivers, offering relief beyond seizure control. 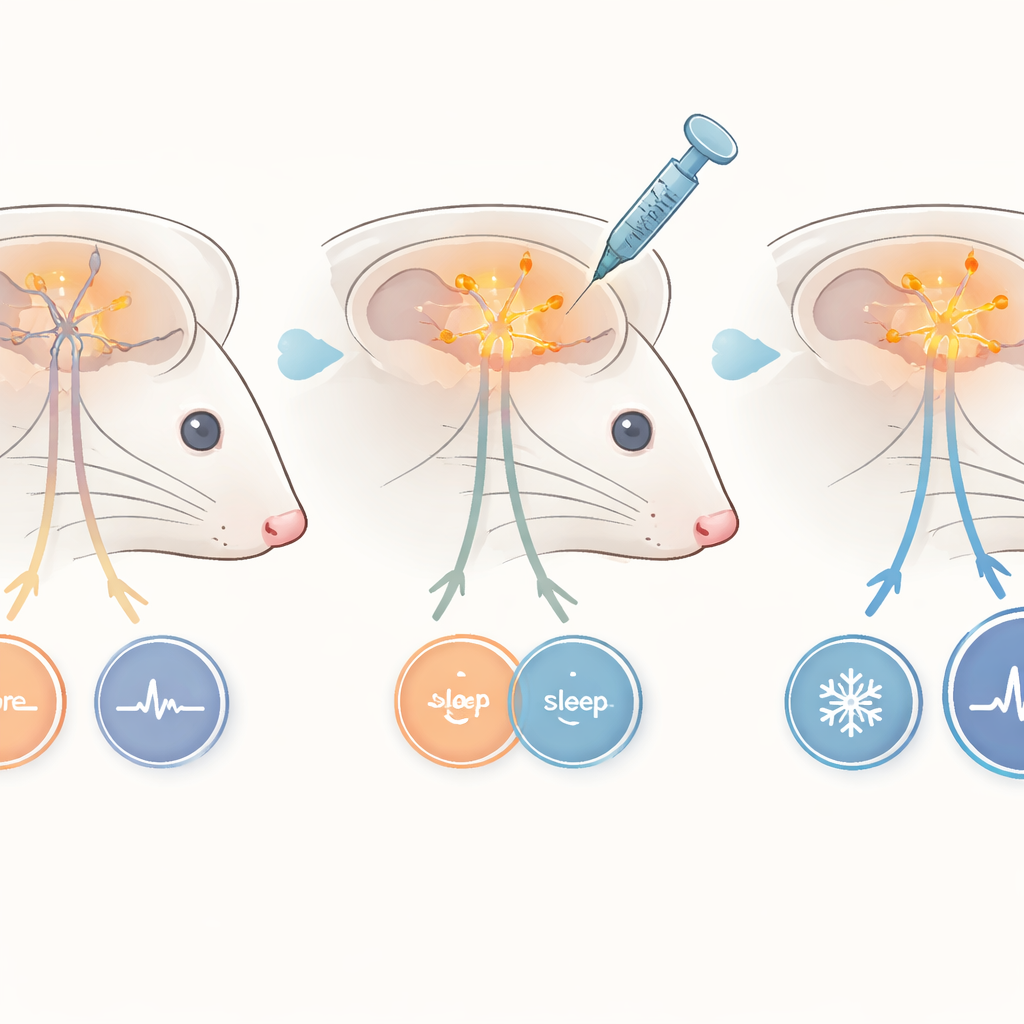
Citation: Fadila, S., Krivoshein, G., Majadly, H. et al. Disrupted temperature-sleep coupling mechanism in a Dravet syndrome mouse model. Nat Commun 17, 3232 (2026). https://doi.org/10.1038/s41467-026-69957-1
Keywords: Dravet syndrome, sleep, thermoregulation, hypothalamus, mouse model