Clear Sky Science · en
Who is benefiting from the dramatic decline in U.S. cancer mortality? Place-based evidence of disparities in rates of improvement
Why Where You Live Matters for Cancer Deaths
Across the United States, deaths from cancer have dropped dramatically over the past few decades, sparing millions of families from heartbreak. But this positive national story hides an uncomfortable truth: not every community has shared in the progress. This study looks beyond national averages to ask a simple, human question with big consequences: which kinds of places are truly benefiting from the decline in cancer deaths, and which are being left behind?
A Turning Point in the Cancer Fight
In 1991, U.S. cancer death rates reached a high point and then began to fall. By 2019, the age-adjusted cancer death rate had dropped by about one-third compared with 1991 levels, largely due to better tobacco control, screening, and treatment. Using detailed records from nearly 21.4 million cancer deaths between 1981 and 2019, the researchers tracked how cancer mortality changed over time in 2,954 counties—nearly the entire country. Instead of just counting deaths, they focused on how quickly death rates improved in each county, offering a clearer picture of who is gaining ground and who is stuck.
How the Team Measured Local Change
The study grouped yearly data into three-year periods to smooth out random swings, especially in small counties. For each county, the authors calculated how much its cancer death rate fell—or failed to fall—relative to the early 1980s. They then linked those changes to basic features of each county: income levels, how urban or rural it is, racial makeup, and education. Using both traditional statistical models and spatial mapping tools, they examined not only overall relationships but also how these patterns varied region by region across the map of the United States.
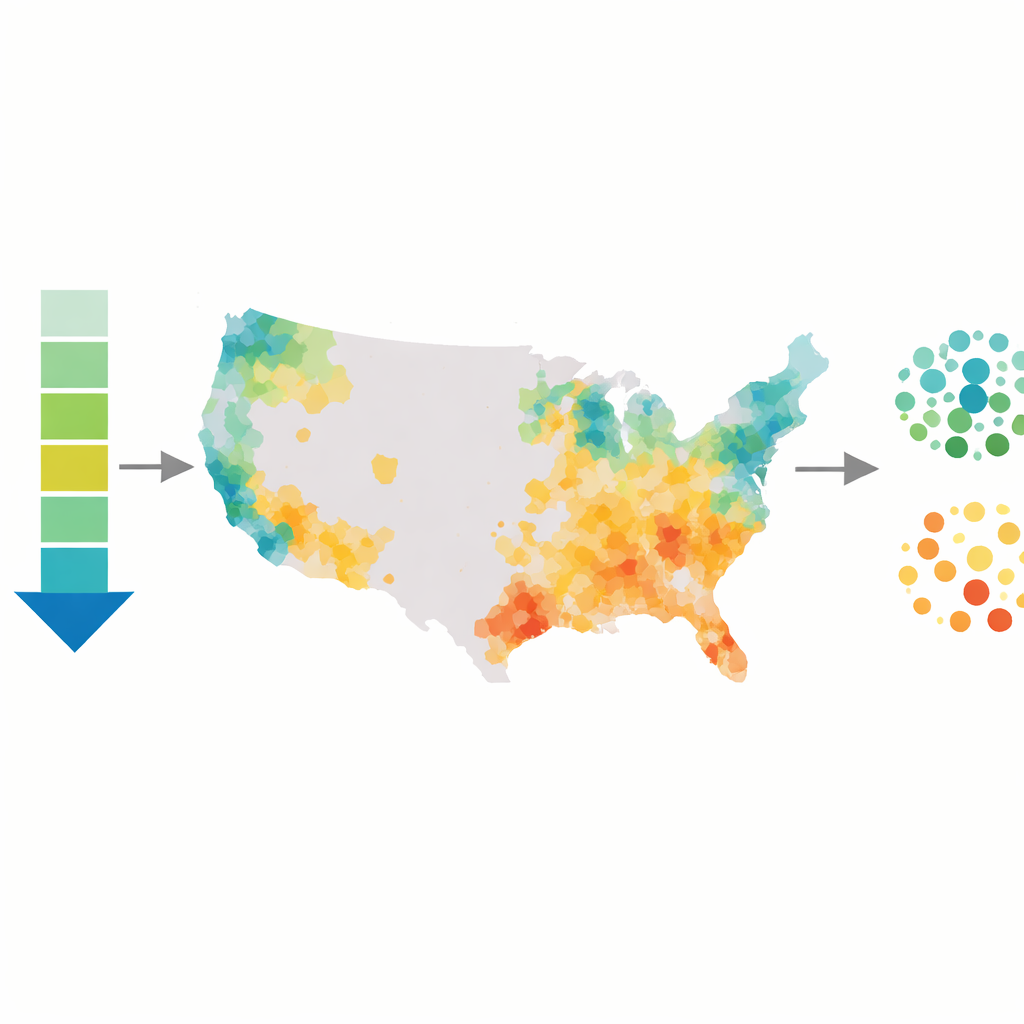
Coastal Cities Pull Ahead, the Heartland Lags
The maps and models reveal striking geographic divides. Most counties saw some reduction in cancer deaths, but 460 counties did not improve at all, and almost all of these actually saw cancer mortality rise. Counties with the biggest improvements were clustered along the Atlantic, Gulf, and Pacific coasts and around major metropolitan areas such as the Boston–New York–Washington corridor, South Florida, coastal California, Denver, and Phoenix. In contrast, many counties in the central United States formed large blocks of weak or no improvement, highlighting an emerging coastal-versus-inland split in the benefits of cancer progress.
The Power of Income and City Life
When the authors examined county characteristics, income and urban status stood out. Higher-income counties, which together held about 10% of the U.S. population in each income band, were the first to see cancer death rates turn downward and experienced the steepest declines over time. The lowest-income group had ten times as many counties with no improvement, much higher death rates by 2017–2019, and only about one-seventh the pace of improvement compared with the richest group. Urban counties also did better than rural ones, and together with income they explained a growing share of the differences in improvement as the decades passed. Education showed a modest link, while the share of Black residents had a smaller and slightly negative association once income, education, and urban–rural status were taken into account.
Local Social Conditions Shape Outcomes
More advanced mapping analysis showed that these social factors do not work the same way everywhere. For example, income had especially strong ties to cancer mortality improvement in Appalachia and the eastern interior, while the influence of urban residence was strongest in New England, the North Central states, the southern border states, and Florida. In many regions where most Black Americans live, the race effect on improvement itself was close to zero after accounting for other local conditions, suggesting that broader social and economic environments are key drivers of who benefits from better prevention and treatment.
What This Means for Communities and Policy
The study concludes that the United States has made real progress against cancer, but that progress has not been shared equally. Big cities and higher-income counties have reaped the greatest gains, while many rural and poorer areas have seen slower improvement—or none at all. For the public, this means that a falling national cancer death rate does not guarantee that one’s own community is improving. For policymakers and health leaders, the findings underscore the need for place-based strategies that bring proven measures—like tobacco control, screening, and high-quality treatment—into the communities that have been left behind. Without a deliberate effort to spread these benefits, advances in cancer care may continue to widen the gap between more advantaged and less advantaged parts of the country.
Citation: Cosby, A.G., Lebakula, V., Bergene, K. et al. Who is benefiting from the dramatic decline in U.S. cancer mortality? Place-based evidence of disparities in rates of improvement. Br J Cancer 134, 1468–1478 (2026). https://doi.org/10.1038/s41416-026-03339-8
Keywords: cancer mortality, health disparities, rural urban gap, social determinants, county-level analysis