Clear Sky Science · en
Precision percutaneous coronary intervention
Making Heart Stent Procedures More Personal
Heart artery blockages are a leading cause of heart attacks and chest pain, and millions of people each year receive a stent through a procedure called percutaneous coronary intervention (PCI). This review article explains how PCI is shifting from a one-size-fits-all treatment to a more tailored, “precision” approach. By blending advanced imaging, smart computer tools, genetics, and careful planning before and after the procedure, doctors aim to make stent treatments safer, more effective, and more comfortable for each individual patient.
Looking at the Whole Patient Before the Procedure
Traditional PCI often began once a blockage was seen on an angiogram. Precision PCI starts earlier, by asking: who really needs a stent, and how should their procedure be prepared? The authors describe how modern heart CT scans combined with computer models can estimate how much a narrowing actually restricts blood flow, sometimes avoiding invasive tests. Artificial intelligence (AI) systems trained on thousands of images can highlight worrisome plaques or calcium deposits and help map out which segments of artery should be treated. At the same time, doctors individualize basic steps like fasting rules and blood thinner management instead of following rigid routines. For example, some studies show that many patients can safely eat before low‑risk catheterization, and continuing certain blood thinners right through the procedure may reduce hospital stays without extra bleeding.
Fine-Tuning What Happens in the Cath Lab
During PCI itself, precision care means shaping every decision to the patient’s anatomy, heart function, and risk profile. Sedation is adjusted to balance comfort with safety and to avoid drugs that interfere with vital anti‑clot medicines. Whenever possible, doctors use an artery in the wrist rather than the groin, guided by ultrasound and supported by tailored “cocktails” to prevent vessel spasm and clots. For people with weak hearts or very complex blockages, the team may choose from several mechanical support devices to assist circulation during the procedure, weighing the benefits and complications of balloon pumps, small heart pumps, or full heart–lung support. In patients who have had an artificial aortic valve placed, special catheters and imaging are selected to safely reach the coronary arteries through or around the valve frame.
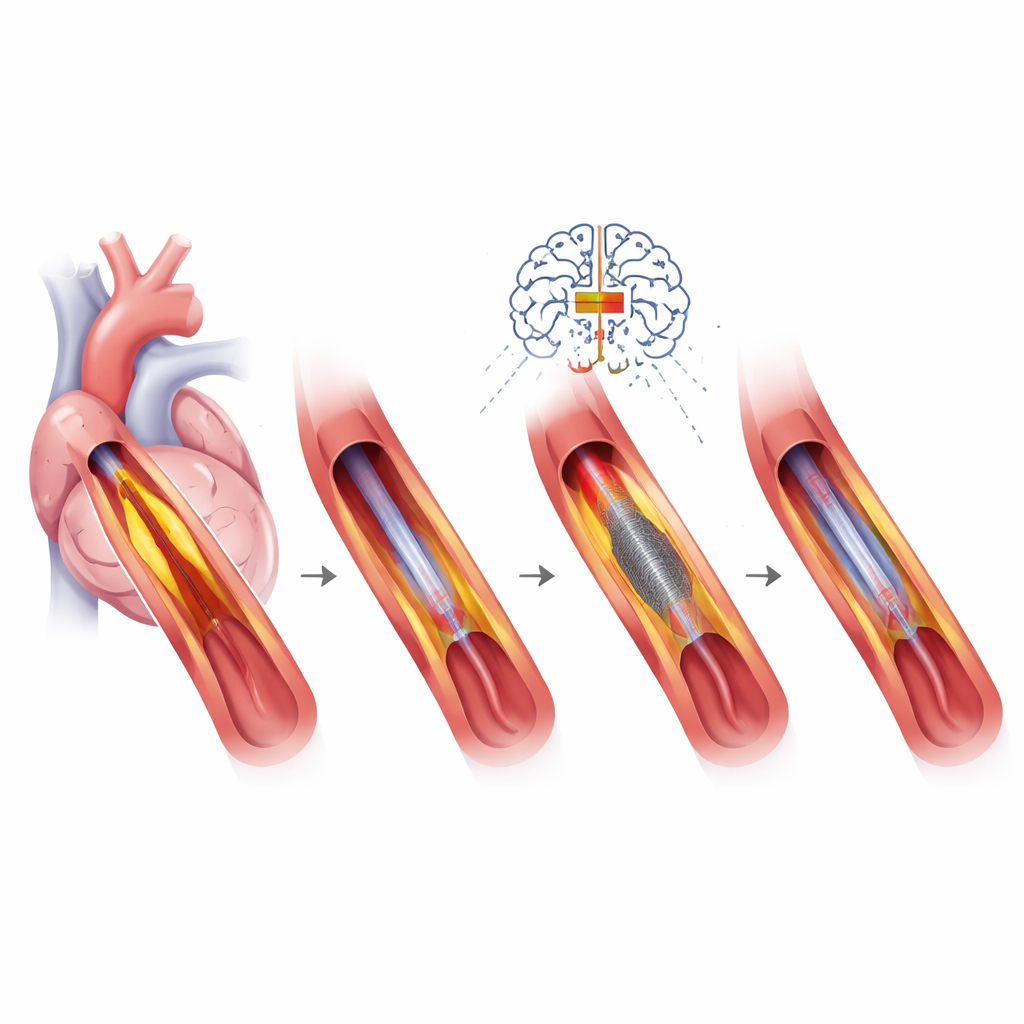
Seeing Inside the Artery and Choosing the Right Tools
A cornerstone of precision PCI is high‑resolution imaging from inside the artery, using ultrasound or light‑based cameras. These tools reveal how long and how calcified a blockage is, how well a stent expands, and why a previous stent may have failed. That information guides the choice among several plaque‑modifying tools, such as tiny sanding devices or balloons that crack calcium with sound waves before a new stent is placed. Stent designs themselves have become more refined—with thinner metal struts, specialized coatings, or even temporary “scaffolds”—and are matched to the patient’s bleeding risk, vessel size, and lesion complexity. For some situations, especially small vessels or patients at high risk for bleeding, drug‑coated balloons that leave no metal behind may be favored.
Medicines, Recovery, and Genetic Clues
Precision PCI continues after the stent is in place. The article reviews how blood thinners during and after the procedure can be selected and dosed based on kidney function, overall bleeding risk, and even genetics. Some people carry gene variants that make standard drugs like clopidogrel less effective, putting them at higher risk of clots; for these patients, testing can support a switch to stronger medications, while others can safely stay on less intensive therapy and avoid extra bleeding. After the procedure, careful management of the wrist access site helps keep the artery open while minimizing bruising. Many stable patients can now go home the same day, improving comfort and lowering costs, as long as clear follow‑up plans are in place. Routine stress testing is reserved for higher‑risk cases rather than being used automatically.
The Road Toward Smarter, Fairer Heart Care
In plain terms, this article concludes that the future of stent procedures lies in doing the right amount of treatment for the right person at the right time. That means combining detailed imaging, computer guidance, and genetic information with thoughtful choices about access routes, devices, and medicines across the entire journey—before, during, and after PCI. The authors also stress that cost, training, and access to technology remain major hurdles, and that not every hospital can yet offer the full “precision” package. With further research, better digital infrastructure, and more equitable funding, they envision catheterization labs where stent procedures are not just routine repairs, but highly individualized interventions that improve outcomes while reducing complications and unnecessary care.
Citation: Wilson, T.M., Munaf, U., Shaikh, N. et al. Precision percutaneous coronary intervention. npj Cardiovasc Health 3, 10 (2026). https://doi.org/10.1038/s44325-026-00111-y
Keywords: precision cardiology, coronary stents, intravascular imaging, artificial intelligence in PCI, personalized antiplatelet therapy