Clear Sky Science · en
Emerging biomarkers and diagnostic tools for the early prediction of adverse prenatal outcomes
Why This Matters for Expectant Families
Pregnancy is often described as a time of joy and anticipation, but for many families it also carries a quiet undercurrent of worry. Complications such as premature birth, high blood pressure in pregnancy, or babies who are very small for their age can appear suddenly and have lifelong effects. This review article explores how tiny signals in blood, vaginal fluid, and even gut bacteria could help doctors spot these risks months earlier than is currently possible, opening the door to closer monitoring and simple, low-cost treatments that may save lives.

Hidden Dangers in Pregnancy
Worldwide, adverse pregnancy outcomes affect roughly one in five pregnancies and remain a leading cause of death in children under five, especially in disadvantaged communities. The review focuses on three of the most common problems: preterm birth (babies born before 37 weeks), pre-eclampsia (a dangerous rise in blood pressure during pregnancy), and small-for-gestational-age babies (very small babies for their stage of pregnancy). These conditions often share risk factors and can occur together, yet they are hard to predict early because many women show no obvious warning signs in the first half of pregnancy, when preventive treatments such as low-dose aspirin or vaginal progesterone work best.
Tiny Clues Floating in Blood
The authors describe how molecules circulating in a pregnant woman’s blood can serve as early warning beacons. Traditional protein tests, such as those that measure fetal fibronectin or certain placental hormones, are helpful mainly for short-term decisions late in pregnancy, like ruling out labour in the next week or two. They are less useful for universal early screening. Newer work instead tracks fragments of genetic material, including RNA and microRNAs, which rise or fall months before symptoms appear. For example, sets of microRNAs in the first trimester can signal an increased chance of preterm birth or growth restriction, while other RNA signatures hint at early-onset pre-eclampsia. Some of these markers, like the microRNA called miR-374a-5p, show up across several pregnancy complications, raising the possibility of a single blood test to flag general high risk.
The Role of Friendly and Unfriendly Microbes
Beyond blood, the review highlights the surprising influence of microbes living in the vagina and gut. In the vagina, a shift away from communities dominated by protective Lactobacillus bacteria toward more mixed, inflammatory species is linked to higher risk of preterm birth. New mass-spectrometry techniques can scan metabolic traces directly from a swab, rapidly capturing the chemical “fingerprints” of these communities without complex sequencing. In the gut, women who later develop pre-eclampsia often have fewer bacteria that produce short-chain fatty acids such as butyrate, which help maintain healthy blood vessels and reduce inflammation. Animal experiments even suggest that restoring these beneficial microbes or their by-products could ease symptoms, hinting at future probiotic or dietary approaches.
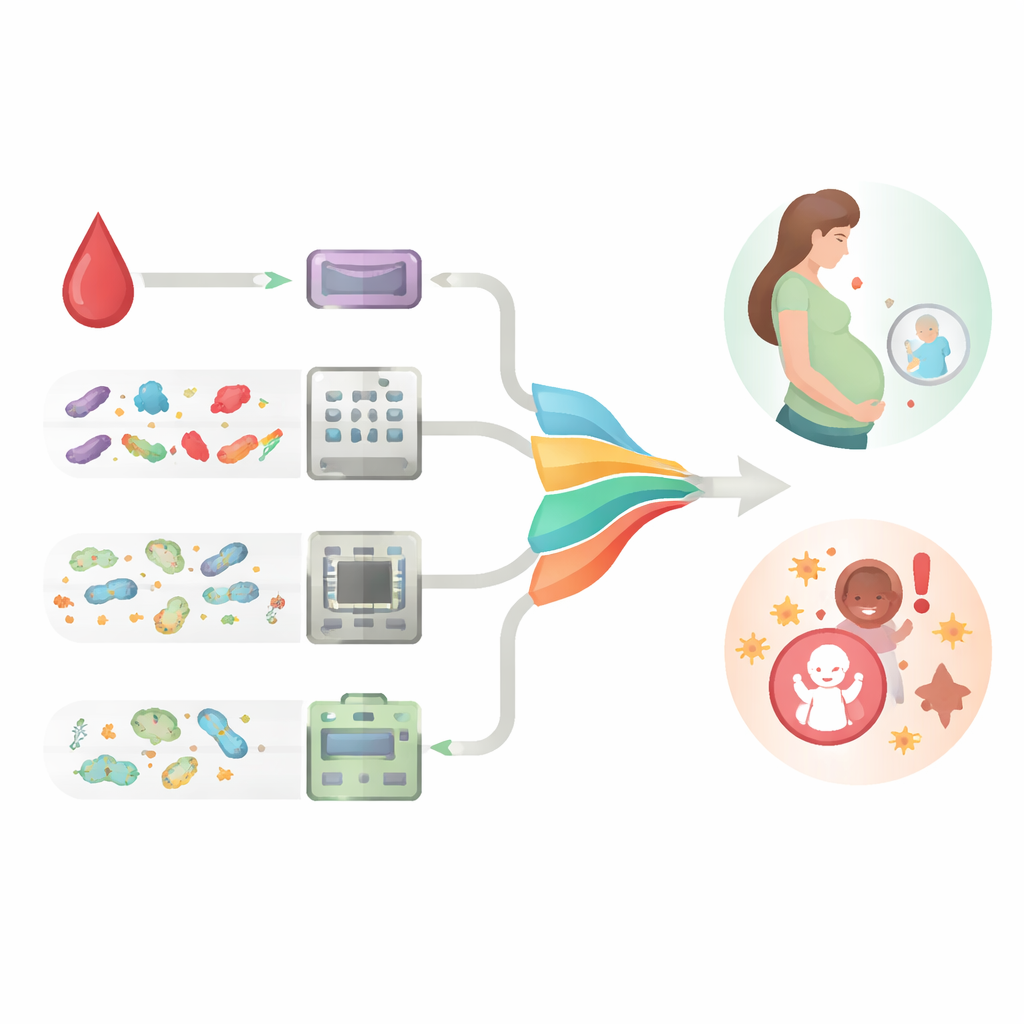
From Lab Bench to Bedside
Finding a promising biomarker is only half the story; turning it into a practical test is equally challenging. Current tools like PCR and sequencing are sensitive but slow, expensive, and ill-suited to busy clinics or low-resource settings. The authors survey emerging technologies designed for quick, low-cost use at the bedside, including paper-based lateral flow strips that can read microRNAs directly from a drop of plasma, optical biosensors for key placental proteins, and compact devices to profile microbes without full DNA analysis. They argue that the most powerful tests will likely combine several types of markers—proteins, genetic fragments, and microbial signals—together with routine clinical measurements, with artificial intelligence helping to sift through complex patterns.
What This Could Mean for Parents and Babies
In plain terms, the article concludes that we are moving toward a future where a simple, non-invasive test early in pregnancy could sort women into different risk groups long before trouble appears. Those at higher risk could receive closer follow-up, timely medications, or lifestyle support, while those at lower risk might avoid unnecessary interventions. Although many of the most exciting biomarkers still need to be validated in large, diverse populations, and standardized testing methods must be agreed upon, the direction is clear. By reading the body’s molecular “whispers” rather than waiting for loud clinical alarms, healthcare systems may soon be able to protect more mothers and babies from preventable harm.
Citation: Soler, M., Parke, B., Kim, S.H. et al. Emerging biomarkers and diagnostic tools for the early prediction of adverse prenatal outcomes. npj Womens Health 4, 20 (2026). https://doi.org/10.1038/s44294-026-00138-7
Keywords: pregnancy biomarkers, preterm birth, preeclampsia, prenatal screening, vaginal and gut microbiome