Clear Sky Science · en
Clinical performance of ASCL1/LHX8 DNA methylation on first-void urine to screen for cervical cancer
Why a Simple Urine Test Could Change Cervical Cancer Screening
Cervical cancer can often be prevented or caught early, but many women skip regular screening because it requires a pelvic exam at a clinic. This study explores a different approach: using a small amount of urine collected at home to look for the virus that causes most cervical cancers and for tiny chemical changes in DNA that signal serious disease. If reliable, this kind of test could make screening more comfortable, convenient, and accessible, especially for people who rarely see a doctor.
A New Way to Use a Home Urine Sample
The researchers focused on “first-void” urine, the very first part of the urine stream, which is richest in cells and DNA shed from the genital tract. Women at home used a special device that captures this portion and preserves the DNA so it can be shipped to a lab. In total, 454 women took part, including healthy volunteers and patients already known to have a range of cervical changes from mild abnormalities to cancer. From each urine sample, the team ran two types of tests: one to detect high-risk human papillomavirus (HPV), the virus responsible for most cervical cancers, and another to measure chemical tags called methyl groups on two human genes, ASCL1 and LHX8.
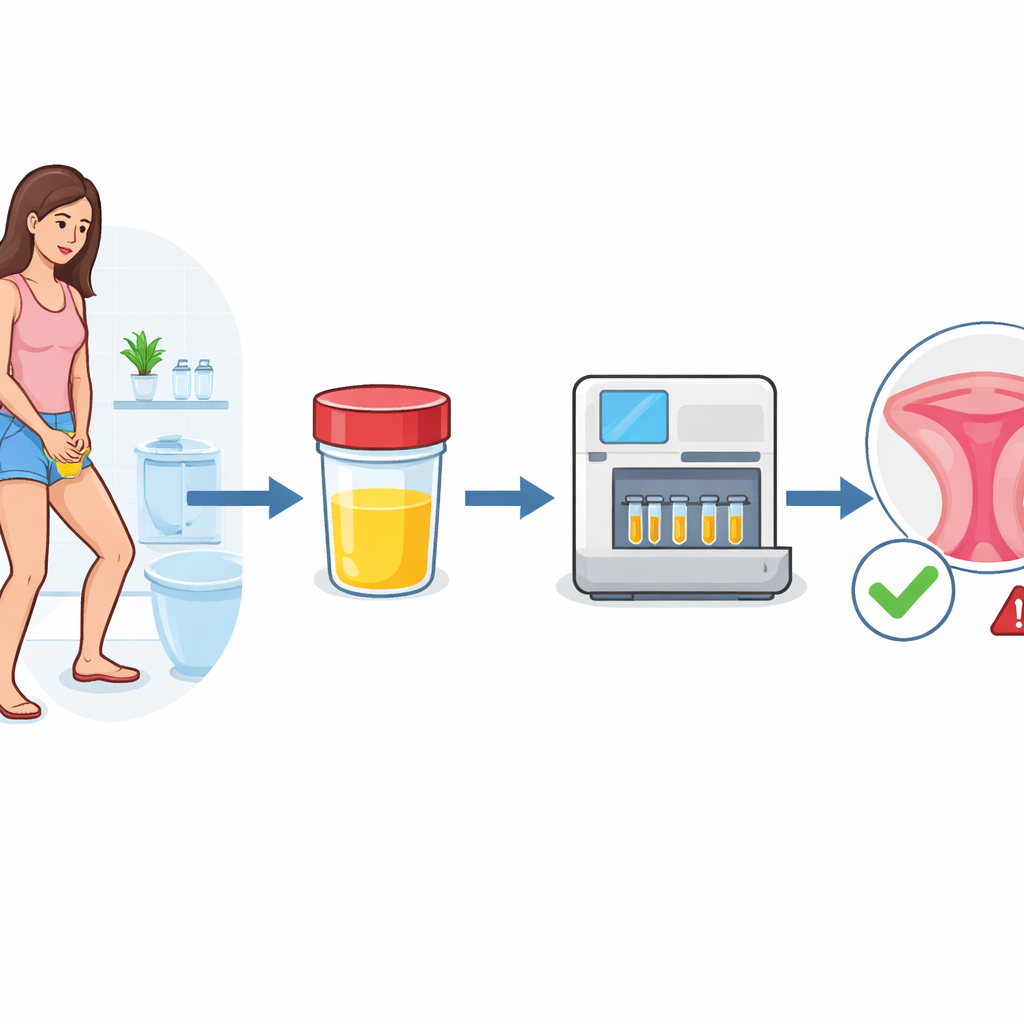
Reading Cancer Risk from DNA Tags
Methylation is a natural chemical modification that cells place on DNA to control which genes are active. In many cancers, methylation patterns shift in characteristic ways. Earlier work suggested that methylation of ASCL1 and LHX8 increases as cervical cells move from harmless HPV infection toward high-grade precancer and cancer. In this study, the team confirmed that in urine samples: methylation levels of both genes rose steadily with disease severity. Women with cancer had the highest methylation, followed by those with severe precancerous changes; women with no or only mild abnormalities had much lower levels. This pattern held even though the overall amount of human DNA in the urine was similar between groups, indicating that the signal reflects disease, not just DNA quantity.
How Well the Urine Test Finds Serious Disease
To judge how well the methylation test works, the researchers split the women into a training group and a separate validation group. They used the first group to define a cut-off value for a positive methylation result that would incorrectly flag only about 20–30% of women without serious disease. They then checked performance in the second group. At the chosen threshold, the methylation test correctly identified 73% of women with severe precancer or cancer, while correctly reassuring about 82% of women without important disease. It detected nearly all cancers; only one rare tumor type, known to be unrelated to HPV, was missed. In comparison, HPV testing in urine was more sensitive for severe precancer overall but less specific, meaning it generated more false alarms among women who did not need treatment.
Using Methylation as a Smart Follow-Up Test
Because many HPV infections clear on their own, a key challenge is deciding which HPV-positive women truly need further exams such as colposcopy. The team therefore tested methylation specifically in women whose urine was already positive for high-risk HPV. In this group, methylation of ASCL1/LHX8 picked up three-quarters of the serious lesions and all cancers, while still avoiding many unnecessary referrals. Another common follow-up method, checking whether the HPV type is one of the highest risk variants (types 16 or 18), caught a similar share of severe lesions but missed several cancers and was less specific. When the researchers combined both pieces of information—methylation status plus HPV type—they could detect 85% of severe precancers and all cancers, although this broader net also meant more women without dangerous disease would be sent on for further testing.
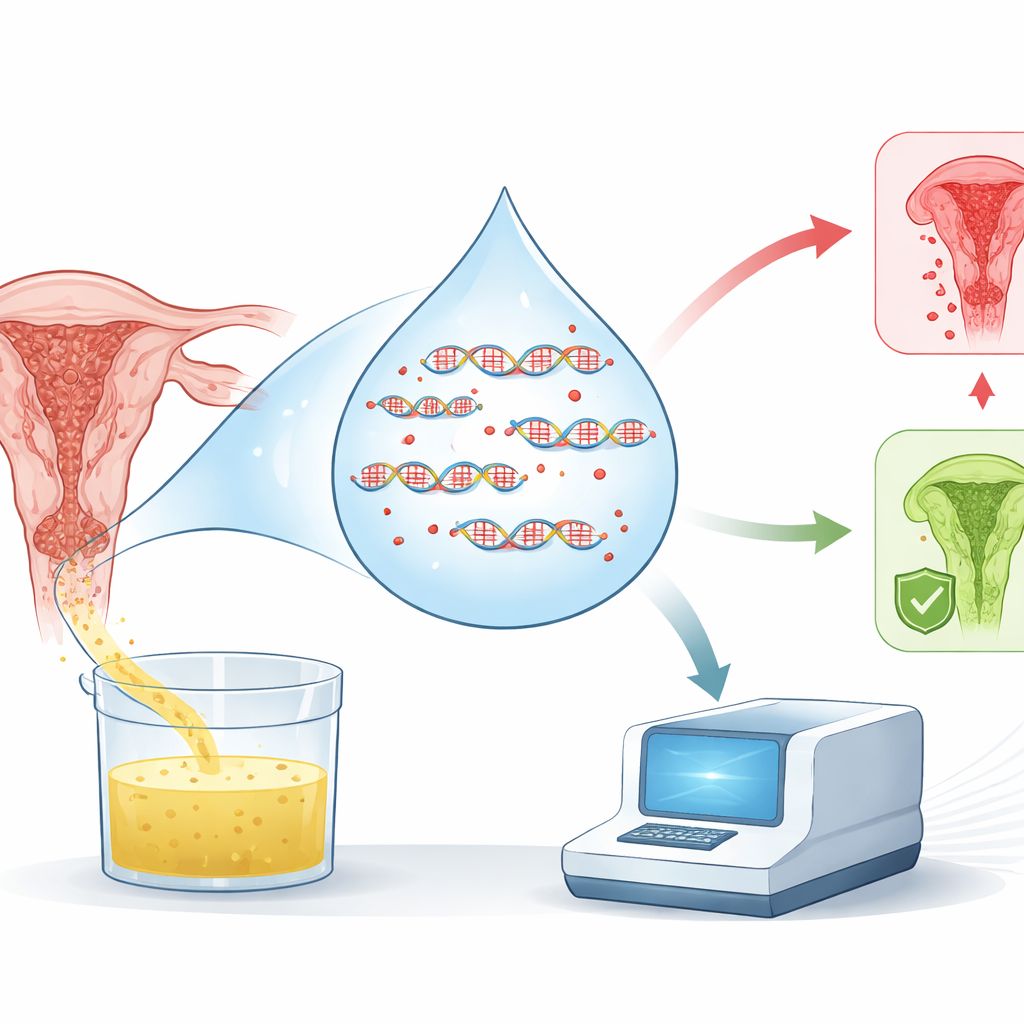
What This Could Mean for Future Screening
The study shows that a fully molecular approach—HPV testing plus DNA methylation analysis, both done on a single at-home urine sample—can identify nearly all cancers and most severe precancers without requiring a clinic-based pelvic exam or Pap smear. While this work was carried out in women already referred for evaluation, the results suggest that such a test could one day support large-scale, mail-out screening programs. If confirmed in broader screening studies, first-void urine testing with methylation-based follow-up could make cervical cancer prevention simpler, less invasive, and more reachable for women who are currently missed by standard programs.
Citation: Van Keer, S., van den Helder, R., Téblick, L. et al. Clinical performance of ASCL1/LHX8 DNA methylation on first-void urine to screen for cervical cancer. Commun Med 6, 248 (2026). https://doi.org/10.1038/s43856-026-01512-x
Keywords: cervical cancer screening, HPV, urine self-sampling, DNA methylation, ASCL1 LHX8 test