Clear Sky Science · en
Development and multicenter validation of an explainable machine learning diagnostic criteria for pediatric abdominal sepsis
Why this matters for sick children
When a child shows up at the hospital with severe belly pain and infection, doctors have to decide very quickly who is in real danger. If abdominal sepsis – a life‑threatening infection in the gut area – is missed or recognized too late, children can slip into organ failure, and treatment may no longer work. This study describes a new computer‑based tool, built from real‑world hospital data, that helps doctors spot abdominal sepsis in children earlier and more reliably, using blood tests and vital signs they already collect every day.
The hidden threat inside the belly
Sepsis is one of the leading causes of death in children worldwide, and infections that start in the abdomen are among the most dangerous forms. Current sepsis “rules” and scoring systems were largely created for adults and focus heavily on lung and heart problems. By the time those signs look bad in a child, damage in the abdomen, liver, or intestines may already be severe. Existing pediatric tools also struggle to pick up abdominal sepsis early enough to guide timely surgery or aggressive treatment. The authors argue that children with suspected abdominal disease need a diagnosis tool tailored specifically to this kind of infection.
Turning routine tests into a smart alarm
The research team gathered electronic medical records from more than 22,000 children treated at a large children’s hospital in China between 2019 and 2023, focusing on 6,566 patients with abdominal problems such as appendicitis or intestinal blockage. Within this group, specialists carefully reviewed charts, imaging, operations, medications, and follow‑up notes to decide which children truly had pediatric abdominal sepsis (PAS). They used an “active learning” approach: a small sample was labeled by three experienced doctors, a preliminary model was trained, and that model then suggested new, uncertain cases for the doctors to re‑examine, repeatedly refining the dataset and reducing disagreements.
Nine simple signals with strong power
From dozens of lab values and vital signs measured during the first 24 hours of admission, the researchers searched for the combination that best separated sepsis from other abdominal illnesses. They ended up with nine everyday measurements: heart rate; white blood cell count; absolute neutrophil count; a liver‑related enzyme called γ‑glutamyl transferase; another liver enzyme (AST); a ratio of two blood proteins (albumin and globulin); prealbumin; calcium level; and a sensitive inflammation marker known as high‑sensitivity C‑reactive protein. None of these tests are exotic – they are part of routine care – but together they form a powerful pattern. Using these nine markers, several machine‑learning methods were compared, and a random‑forest model delivered the most reliable performance.
A tool that works across many hospitals
The final model, named ABSeD (Abdominal Sepsis Diagnosis), correctly distinguished PAS from other abdominal diseases with high accuracy. In the original hospital’s data, its performance was excellent, and it held up well in internal validation. To see if it would generalize beyond a single center, the team then built an online platform and prospectively collected data from seven additional hospitals in Zhejiang Province in early 2025. Among 308 children who had clear follow‑up or surgical confirmation, ABSeD again showed strong results, accurately flagging most children with abdominal sepsis and maintaining high precision – meaning that when it warned of sepsis, it was usually right. The system also shows how each of the nine markers influences the model’s judgment, giving doctors a transparent view rather than a mysterious “black box.”
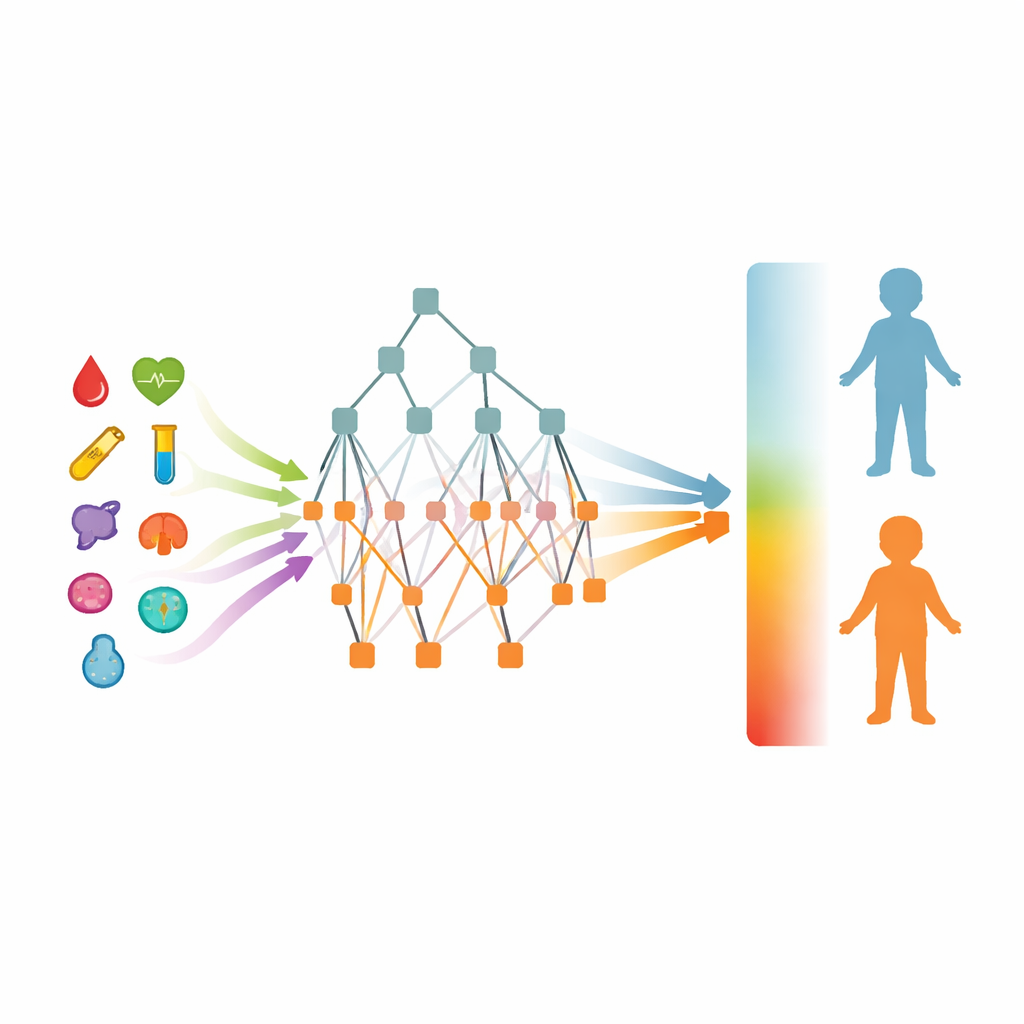
From research model to bedside helper
To make their work usable in everyday practice, the authors created a web‑based interface where clinicians enter a child’s age, basic information, and nine lab values. The tool returns a risk score and a clear visual breakdown of which measurements drove the result, helping doctors decide whether to escalate care, order imaging, or proceed to surgery. The study emphasizes both the promise and the limits of the model: it is meant for children who already have suspected abdominal disease, not for universal screening, and it has so far been tested only within one region and ethnic background. Even so, the ABSeD tool shows how carefully built and explainable artificial intelligence can turn ordinary lab tests into an early‑warning system, potentially saving children’s lives by catching deadly abdominal sepsis before it is too late.
Citation: Cao, S., Cai, D., Zhang, S. et al. Development and multicenter validation of an explainable machine learning diagnostic criteria for pediatric abdominal sepsis. npj Digit. Med. 9, 312 (2026). https://doi.org/10.1038/s41746-026-02500-0
Keywords: pediatric sepsis, abdominal infection, machine learning, early diagnosis, clinical decision support