Clear Sky Science · en
Interaction between high-sensitivity C-reactive protein and mean platelet volume for 1-year major adverse cardiovascular events in stable coronary artery disease
Why this heart study matters
Many people live for years with “stable” coronary artery disease, in which the heart’s arteries are narrowed but not acutely blocked. Even on modern medications, they still face a steady risk of heart attack, stroke, or sudden worsening of chest pain. This study asks a practical question with real-world implications: can two simple blood tests, already available in most hospitals, be combined to pinpoint which of these patients are at especially high risk in the coming year?
Two simple clues in the blood
The researchers focused on two markers. The first, high‑sensitivity C‑reactive protein (hs‑CRP), reflects low‑grade inflammation in the body. The second, mean platelet volume (MPV), captures the average size of platelets, the tiny blood cells that help form clots. Larger platelets tend to be more active and more likely to contribute to clots that can block an artery. Instead of looking at each marker separately, the team asked whether having both high inflammation and large platelets together marked out a particularly vulnerable group of patients.
How the study was done
The study analyzed 1,463 adults with stable coronary artery disease treated at five medical centers in China. All had at least one coronary artery narrowed by half or more but were not in the midst of a heart attack. At the start, each person had blood drawn to measure hs‑CRP and MPV. The researchers then sorted patients into four groups: both markers low, only hs‑CRP high, only MPV high, or both markers high. Over the next year, they tracked major heart‑related events, including cardiovascular death, heart attack, stroke, urgent procedures to reopen arteries, and hospitalizations for unstable chest pain. 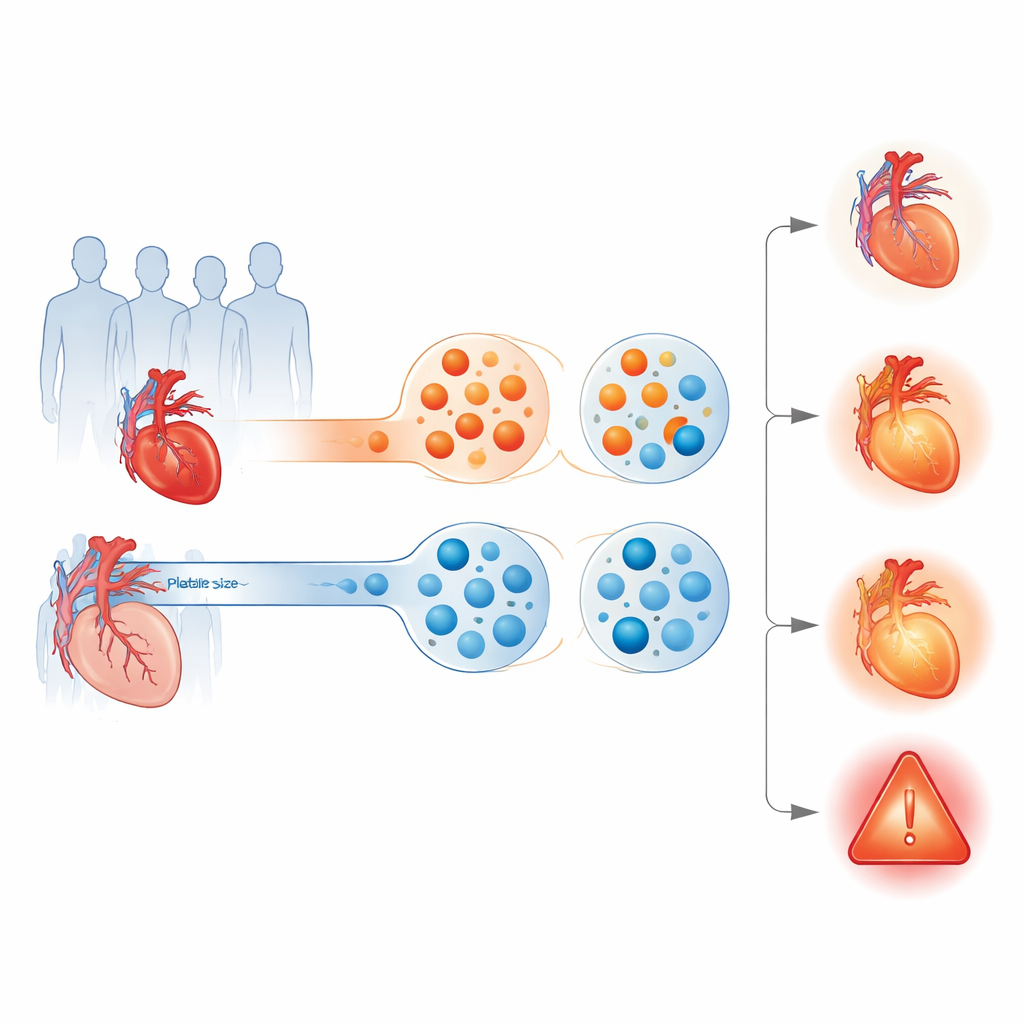
What the researchers found
Across the whole group, just under 5% of patients experienced a major event within one year. But this risk was not evenly distributed. Patients with both low inflammation and smaller platelets had about a 4% event rate. Those with only high hs‑CRP or only high MPV looked surprisingly similar, with event rates again around 4%. The standout group was the relatively small subset in whom both markers were elevated: roughly 10% of them suffered a serious heart‑related problem within a year. After accounting for age, sex, blood pressure, diabetes, kidney function, and other factors, having both markers high was linked to more than double the odds of a major event compared with having both low.
Inflammation and clotting working together
To dig deeper, the researchers examined whether the combined effect of inflammation and large platelets was greater than what would be expected if you simply added their separate risks. Statistical tests suggested a real “interaction”: when high hs‑CRP and high MPV coexisted, the excess risk was more than the sum of their individual contributions. Importantly, this high‑risk group did not simply have more extensive artery blockages or worse cholesterol histories than others, and the link held up even after considering white blood cell counts, statin use, prior heart attacks, and various alternative definitions. The pattern was similar whether patients were on one or two antiplatelet drugs. 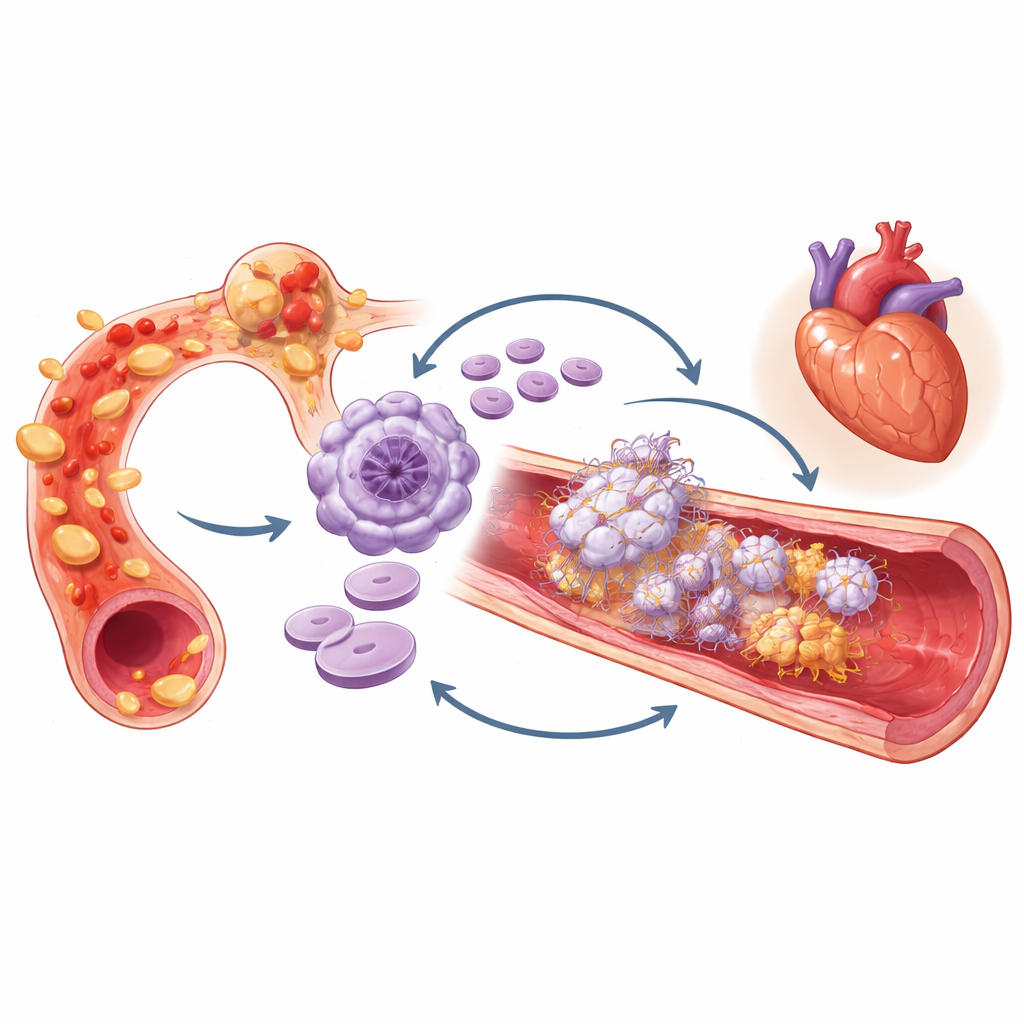
What might be happening inside the arteries
The authors interpret their findings through the lens of “immunothrombosis,” the close crosstalk between inflammation and clot formation. Long‑lasting inflammation may stimulate the bone marrow to produce larger, more reactive platelets. These platelets, in turn, can stick to immune cells and the vessel wall, release inflammatory signals, and help weave sticky webs of material that trap more cells and proteins, promoting clot growth. In this picture, high hs‑CRP and high MPV together signal a self‑reinforcing loop in which inflamed blood and overactive platelets amplify each other, nudging a seemingly “stable” artery toward an abrupt blockage.
What it means for patients and doctors
For people living with stable coronary artery disease, the study’s message is both cautionary and hopeful. It suggests that two routine, inexpensive blood measurements—hs‑CRP and MPV—can help single out a subgroup whose short‑term risk of heart attack or related events is considerably higher than average. At the same time, patients with only one elevated marker did not show extra risk over a one‑year horizon, hinting that treatment intensification might be most usefully reserved for those with both markers high. The authors argue that, if future research confirms these results and tests targeted therapies, this simple two‑marker profile could become a practical tool to guide more personalized prevention strategies in everyday cardiology care.
Citation: Hu, L., Peng, J., Meng, Y. et al. Interaction between high-sensitivity C-reactive protein and mean platelet volume for 1-year major adverse cardiovascular events in stable coronary artery disease. Sci Rep 16, 10702 (2026). https://doi.org/10.1038/s41598-026-46587-7
Keywords: coronary artery disease, C-reactive protein, platelets, cardiovascular risk, inflammation