Clear Sky Science · en
A novel logarithmic spiral design for proximal interphalangeal joint arthroplasty
Why a new finger joint matters
Many people develop painful, stiff fingers as they age, especially in the middle joints that let us grip keys, type, or button a shirt. When these joints wear out, surgeons can either fuse the bones, which stops movement, or replace the joint with an artificial implant. Today’s implants often do not move like a healthy finger, leading to limited bend, discomfort, or device failure. This study introduces a new middle finger joint implant shaped around a graceful mathematical curve called a spiral, with the goal of making artificial joints move more like the real thing.
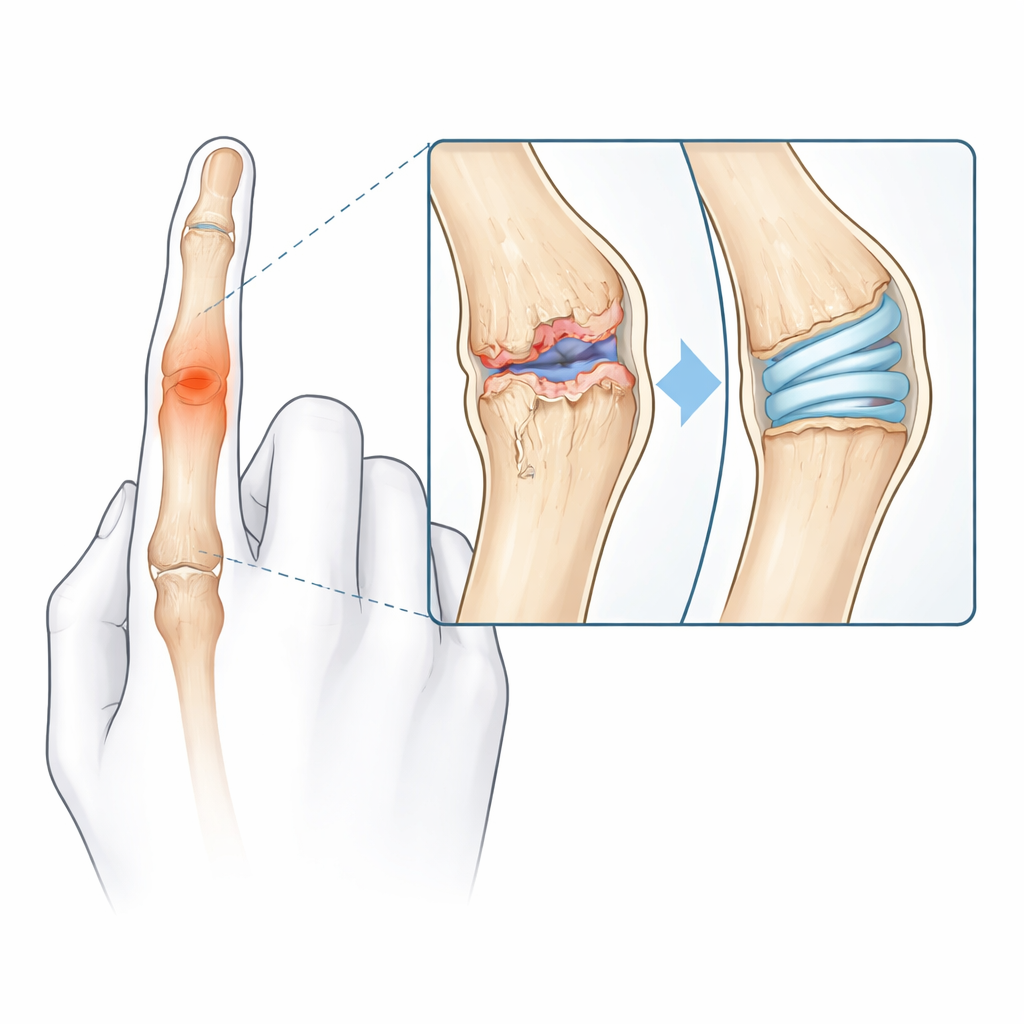
How healthy fingers really move
The middle joint of each finger—the proximal interphalangeal, or PIP, joint—does not work like a simple door hinge. As we bend a finger, the joint surfaces roll, slide, and subtly twist in three dimensions. The center of rotation actually shifts along a corkscrew-like path, and yet, despite all this complexity, the path traced by the fingertip as it curls in toward the palm follows a very regular spiral. Earlier implants treated the joint as a single fixed hinge with a circular shape, ignoring this natural spiral motion and the wide differences in finger shapes between people. That mismatch helps explain why many patients end up with stiff, unnatural-feeling joints after standard replacement surgery.
Designing a spiral-shaped joint
To better match nature, the research team carefully analyzed 3D scans of 100 healthy finger bones. From these, they created an average shape for the head of the finger bone and the base of its neighbor, paying attention to widths, corner curves, and the inner canal that holds the implant’s stem. They then reshaped the sliding surface of the new implant so that, in side view, it follows a logarithmic spiral—a specific kind of curve that keeps a constant angle as it winds inward. In practical terms, this gives the joint a single, stable center of rotation and ensures that the direction of forces across the joint stays consistent as the finger bends, while still tracing the same spiral path that a natural fingertip follows.
Testing the idea in virtual joints
Before turning to human tissue, the team tested how the spiral joint behaves in a computer model. They built detailed 3D models of the metal and plastic implant parts and simulated the joint moving from straight to fully bent under a gentle, realistic load. The analysis focused on two critical measures: how pressure is spread where the two parts meet, and how far apart the surfaces stay as they slide. Across the full bending range, the spiral design kept pressure spread fairly evenly and the gap between surfaces nearly constant. As the joint approached a deep bend of about 105 degrees, the curve of the spiral caused the sliding motion to slow down, acting like a natural brake that reduces sudden stress on the joint surfaces.
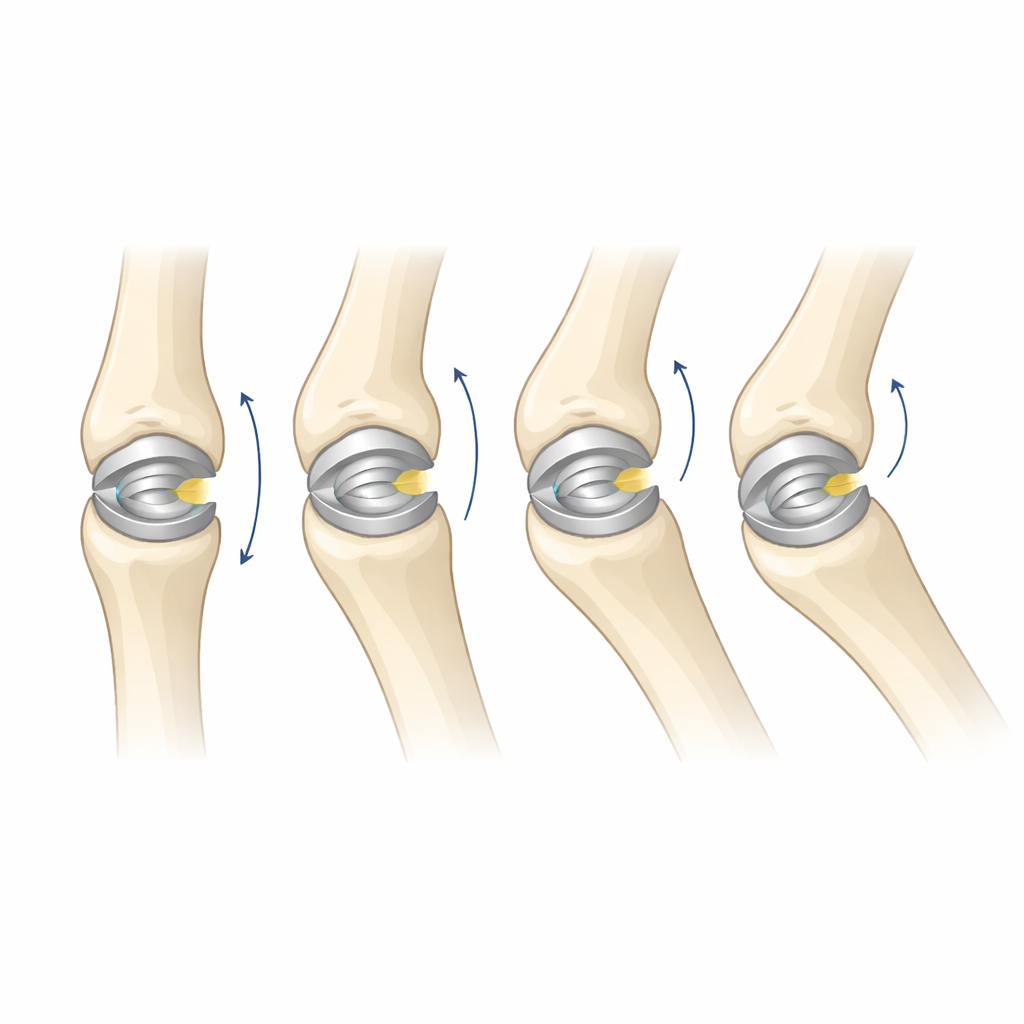
Trying the implant in real fingers
The researchers then implanted the device into preserved human fingers that retained lifelike softness and movement. Surgeons prepared the bones much like they would in real operations and inserted properly sized versions of the implant. When the flexor tendon was pulled with a controlled force to mimic muscle action, all treated joints bent more than 100 degrees—within the normal range for a living PIP joint—while fully straightening or nearly so. X‑ray movies showed that the contact point between the implant surfaces stayed in a central band as the joint moved, instead of wandering unpredictably. In a separate test using a thin pressure sensor between the parts, the overall force across the joint remained steady during most of the bending motion, supporting the computer prediction of smooth, stable contact.
What this could mean for patients
The study suggests that shaping a finger joint implant around a spiral, rather than a simple circle, may help the artificial joint glide more like a natural one. By keeping contact even and motion smooth throughout bending, the design could one day offer patients a greater range of movement, less wear on the device, and possibly longer-lasting pain relief. However, these results come from simulations and cadaver fingers, not living patients, and the work did not yet measure how surrounding ligaments and muscles adapt over time. Clinical trials and direct comparisons with existing implants will be needed before surgeons know whether this spiral-based joint truly improves daily function for people with painful, arthritic fingers.
Citation: Hirata, H., Kurimoto, S., Yoneda, H. et al. A novel logarithmic spiral design for proximal interphalangeal joint arthroplasty. Sci Rep 16, 13266 (2026). https://doi.org/10.1038/s41598-026-45687-8
Keywords: finger joint replacement, hand osteoarthritis, joint prosthesis design, biomechanics, logarithmic spiral implant