Clear Sky Science · en
Automated OCT-tailored and same-visit biomarker-targeted microperimetry in geographic atrophy
Why this matters for aging eyes
As people live longer, more of us develop age-related eye diseases that quietly nibble away at central vision. One of the most feared is geographic atrophy, a late stage of macular degeneration for which new drugs have only recently become available. Yet regulators still question whether current tests truly capture how these treatments help patients see. This study introduces a smarter, automated way to measure vision loss right where the retina is actually sick, potentially reshaping how future therapies are evaluated in the clinic and in trials.
The problem with current vision tests
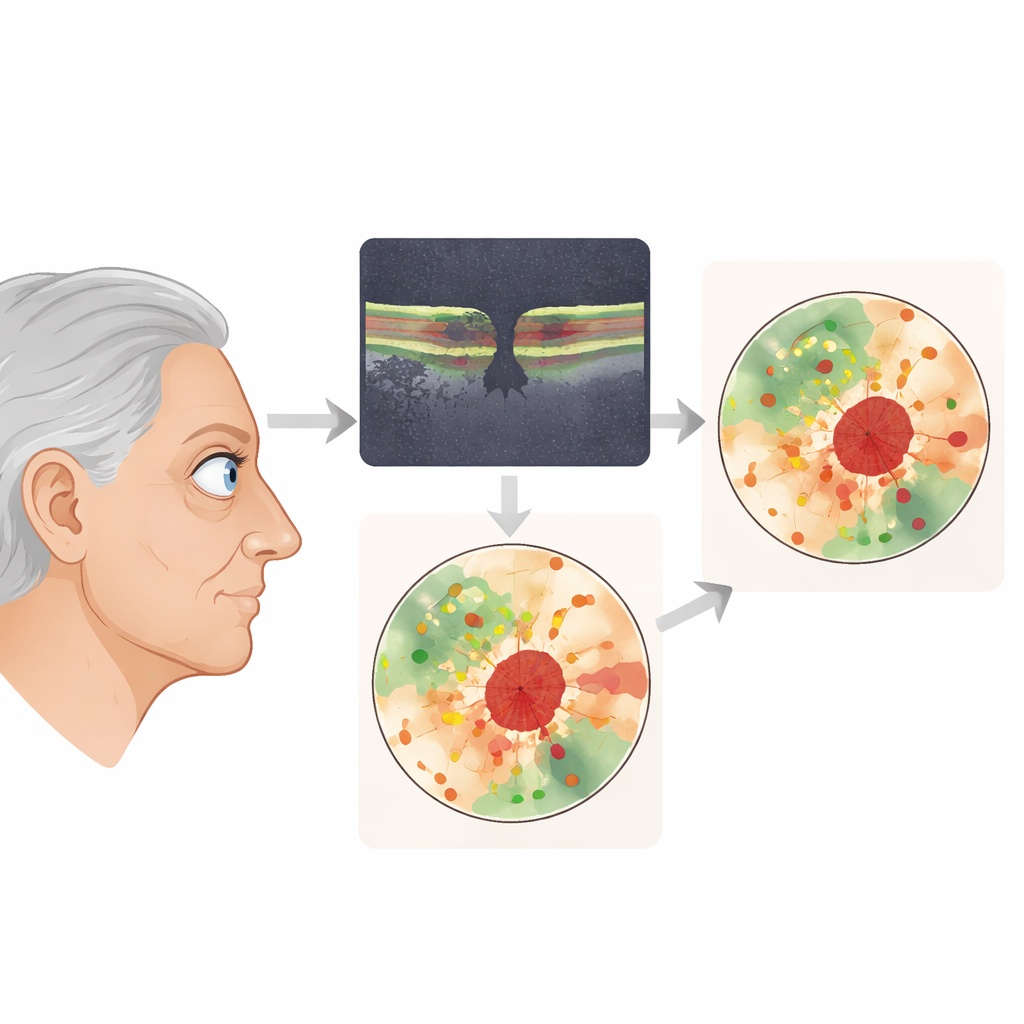
Geographic atrophy slowly erodes the light-sensing cells and the support layer beneath them in the central retina. Today’s drug trials mainly track how far these dead patches spread on imaging, while standard eye charts and similar tests often look surprisingly normal until very late in the disease. That mismatch has already had real-world consequences: a major treatment was turned down by a European regulator because the structural benefits were not matched by clear functional gains. Doctors urgently need tests that pick up early, patchy changes in seeing, not just end-stage blind spots.
A new way to aim the light flashes
The researchers focused on microperimetry, a test that projects tiny spots of light onto precise locations on the retina and records how bright each spot must be to be seen. Traditionally, the device uses a fixed grid of locations that ignores each patient’s unique pattern of damage. In this study, patients first had a detailed three-dimensional scan of the retina using optical coherence tomography. Certified artificial-intelligence software then automatically mapped two key zones: areas where the light-sensing layer was thinned or missing, and areas where both that layer and its support sheet were gone. A rule-based computer program used these maps to design a custom set of 40 test locations for each eye, packing more points into the “at-risk” ring of partial damage and fewer into fully dead or completely healthy regions.
Testing vision exactly where the damage lies
In 61 eyes from 44 older adults with geographic atrophy, the team generated and used these custom patterns during a single clinic visit. They confirmed that the device was actually stimulating the intended spots: on average, measured locations were within about 40 micrometers of where the algorithm had planned, and nearly all points fell within the correct tissue type once built-in safety margins were applied. When they compared light sensitivity across retinal zones, a clear gradient emerged. Areas that still looked structurally intact had the best sensitivity, the ring of partial damage showed intermediate loss, and regions of complete atrophy were worst, though not always completely blind. At the level of whole eyes, larger areas of damage—especially the earlier, partially damaged zones—were linked to lower average sensitivity even after accounting for age and distance from the center of vision.
What this could mean for future treatments
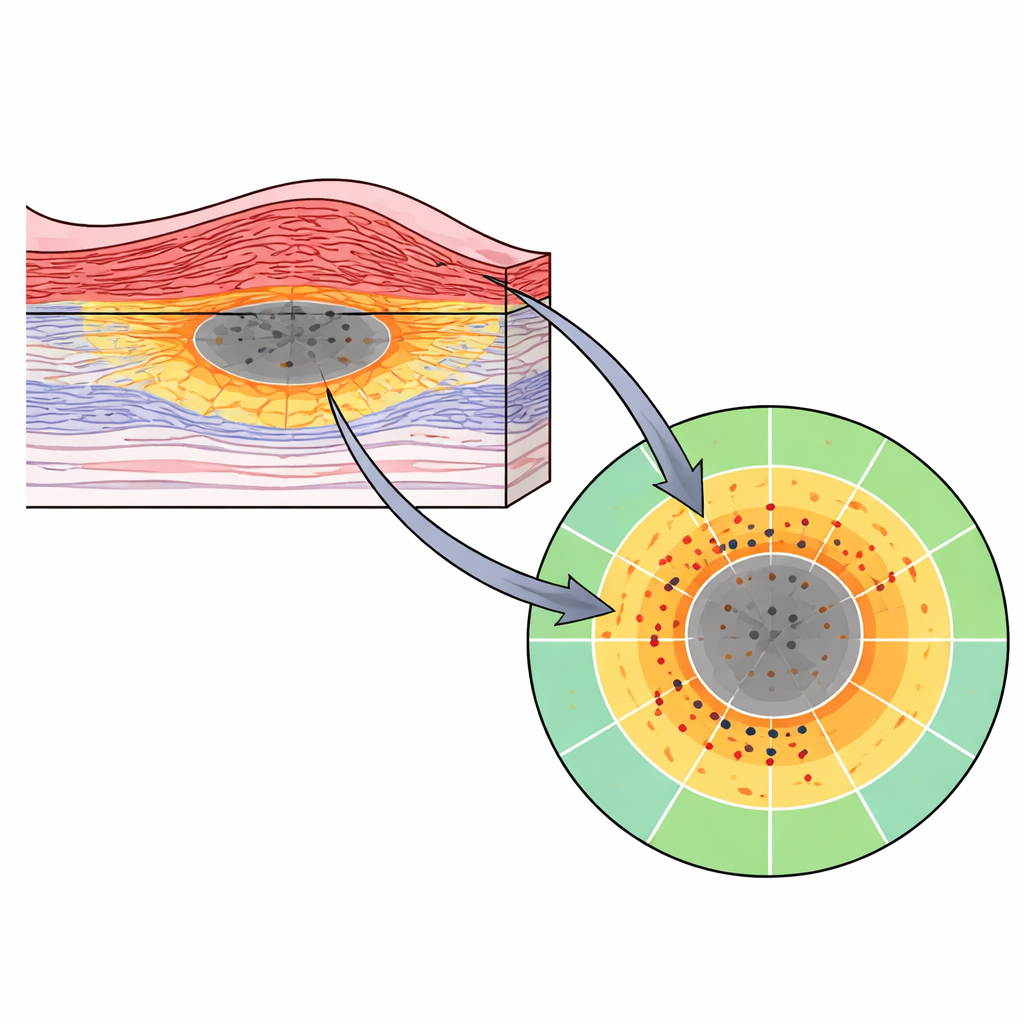
Because the custom patterns concentrate test spots in regions where function is changing fastest, they may capture subtle declines or treatment benefits that uniform grids and eye charts miss. The entire workflow—from scanning to automated mapping to tailored testing—can be completed within one appointment using commercially available tools and web-based software. The authors argue that this patient-specific, biomarker-guided map of structure and function could serve as a more sensitive outcome measure in drug trials, and could help clinicians follow disease activity in everyday practice.
Take-home message for patients and clinicians
This proof-of-concept study shows that it is feasible to automatically “aim” vision testing at the most vulnerable parts of the retina in geographic atrophy, using a combination of modern imaging, artificial intelligence, and smart test design. By aligning what doctors see on scans with how patients see in daily life, this approach may bridge the gap between structural and functional measures. If confirmed in longer-term and larger studies, such tailored testing could become an important tool for judging whether new treatments truly protect sight, not just retinal anatomy.
Citation: Tratnig-Frankl, M., Kuchernig, L., Birner, K. et al. Automated OCT-tailored and same-visit biomarker-targeted microperimetry in geographic atrophy. Sci Rep 16, 10830 (2026). https://doi.org/10.1038/s41598-026-45253-2
Keywords: geographic atrophy, age-related macular degeneration, microperimetry, retinal imaging, vision testing