Clear Sky Science · en
Analysis of postmortem dermal extracts is an efficient illicit drug screening method supporting forensic medicine
Why a simple skin test after death matters
When someone dies unexpectedly, one of the most urgent questions is whether alcohol or drugs played a role. Today, answering that often means a full autopsy and intensive lab work on blood and organs—procedures that are slow, costly, and sometimes rejected for cultural or religious reasons. This study explores a surprisingly simple alternative: gently soaking the skin of the hands and feet with moistened filter paper after death and using that tiny amount of material to screen for a wide range of drugs and their breakdown products.
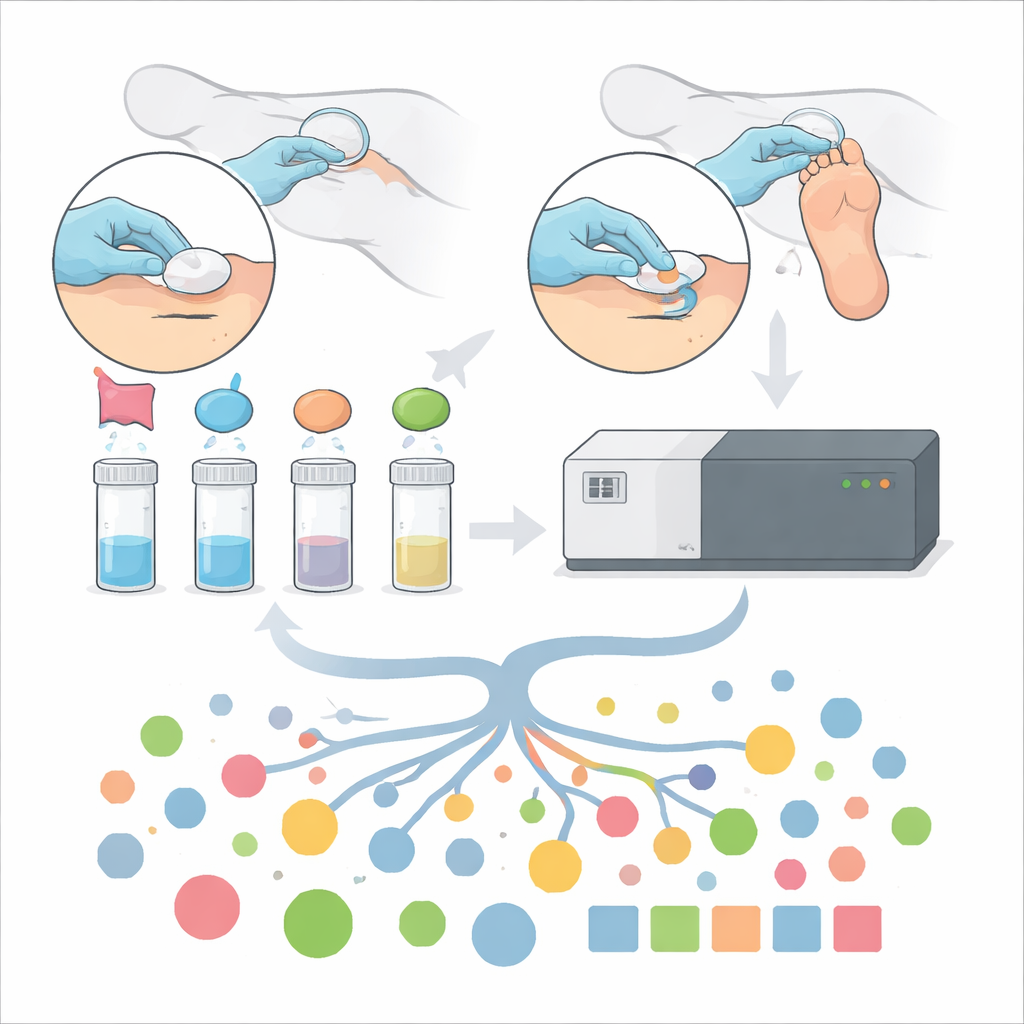
A new way to read chemical traces on the skin
The researchers built on earlier work showing that sweat from living people’s fingertips contains enough chemical information to monitor medicines and drugs. They asked whether a similar, non-invasive approach could work on deceased individuals, long after active sweating has stopped. In 93 people undergoing medicolegal autopsy, small circles of pre-wetted filter paper were pressed onto the palms and soles for five minutes, then stored and extracted with a simple water-based solution. Instead of focusing on a narrow list of compounds, the team used an untargeted high-resolution mass spectrometry method, which can scan broadly for hundreds of different small molecules in a single, rapid run.
How the skin test compared with standard toxicology
All of the bodies also underwent routine forensic toxicology, where blood, brain tissue, stomach contents, urine, and other materials were processed using a validated assay that targets more than 400 drugs and related compounds. By comparing these reports with the results from the skin-derived "dermal extracts," the scientists could see how well the new method performed. Out of 123 different therapeutic and illicit substances reported by the standard assay, 82—about two-thirds—were also found in dermal extracts. For a panel of 19 drugs often linked to illegal use, the skin method showed very high agreement: on average about 95% overlap for positive findings and 87% for negative findings, with the main exceptions being extremely potent, low-dose drugs like fentanyl that are harder to detect without a more specialized, targeted approach.
Seeing past surface contamination with drug breakdown products
One major concern with any surface-based test is contamination from the environment. Traces of cocaine, for example, are known to be present on everyday surfaces such as banknotes and public transport handrails. To separate true drug use from casual contact, the team looked not only for the parent drugs but also for "endogenous" metabolites—chemical breakdown products that are formed inside the body. For cocaine, they tracked an extended network of metabolites, including several that are not measured in standard toxicology. If a person’s skin sample showed a consistent pattern of multiple cocaine-related metabolites, the authors treated that as strong evidence of actual consumption rather than simple contamination. This strategy almost doubled the number of likely cocaine users identified, many of whom also had other drugs or alcohol present, suggesting real-world patterns of combined substance use.
Hints of a longer detection window in skin
In some cases, dermal extracts revealed signs of drug use even when the classical assay was negative. Heroin, for instance, breaks down quickly in blood and is often missed in routine screens; yet the researchers were able to detect heroin itself or its characteristic breakdown products, such as 6-acetylmorphine and morphine, in several skin samples. A similar pattern appeared for ketamine and its metabolites. The authors propose that drugs may be stored in the outer skin layers in a way that somewhat resembles hair, preserving evidence of recent or habitual use even days after death. Because bodies in this study were often examined more than a week after death, the persistence of drug-related molecules in the skin suggests that dermal extracts could offer a longer detection window than some traditional biological fluids, though more work is needed to pin down exact time scales.
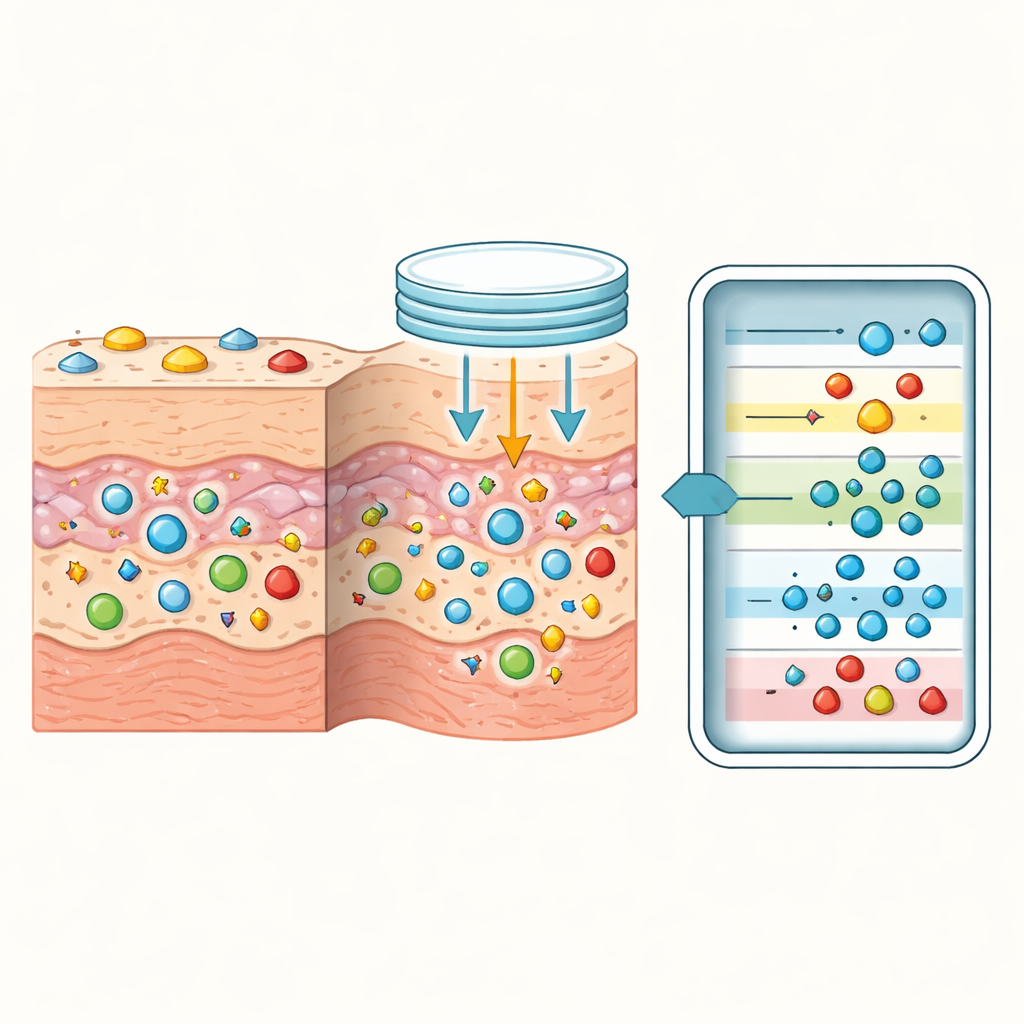
What this could mean for future forensic work
By combining skin-derived drug and metabolite profiles into a simple "drug score," the researchers found they could distinguish deaths linked to drug abuse from natural or accidental causes, even using only qualitative (presence-or-absence) data. Collecting dermal extracts is fast, inexpensive, and does not require an autopsy: in principle, first responders could perform the sampling at the scene, and laboratory analysis could deliver results within about half an hour from the time the sample arrives at the instrument. While the method does not yet replace full toxicology—especially for very low-level drugs, precise concentrations, or legal proceedings—it offers a powerful screening tool that could flag cases needing more exhaustive investigation. With further refinement, including targeted methods and statistical models, postmortem dermal extracts may become a routine, non-invasive way to uncover drug use and mixed-drug intoxication in forensic medicine.
Citation: Wasinger, D., Stolz, K., Wolf, M. et al. Analysis of postmortem dermal extracts is an efficient illicit drug screening method supporting forensic medicine. Sci Rep 16, 14183 (2026). https://doi.org/10.1038/s41598-026-45056-5
Keywords: forensic toxicology, postmortem drug testing, skin-based screening, drug metabolites, mass spectrometry