Clear Sky Science · en
CSF1 regulates inflammation and apoptosis in intervertebral disc degeneration
Why Back Pain Starts Deep Inside the Spine
Low back pain is one of the most common reasons people visit a doctor or miss work. Much of that pain traces back to wear and tear in the soft cushions between the bones of the spine, called intervertebral discs. This study asks a surprisingly simple question with big implications: is there a single signaling molecule in the body that helps drive both inflammation and cell death inside these discs, and could it become a target for earlier diagnosis or gentler treatments?
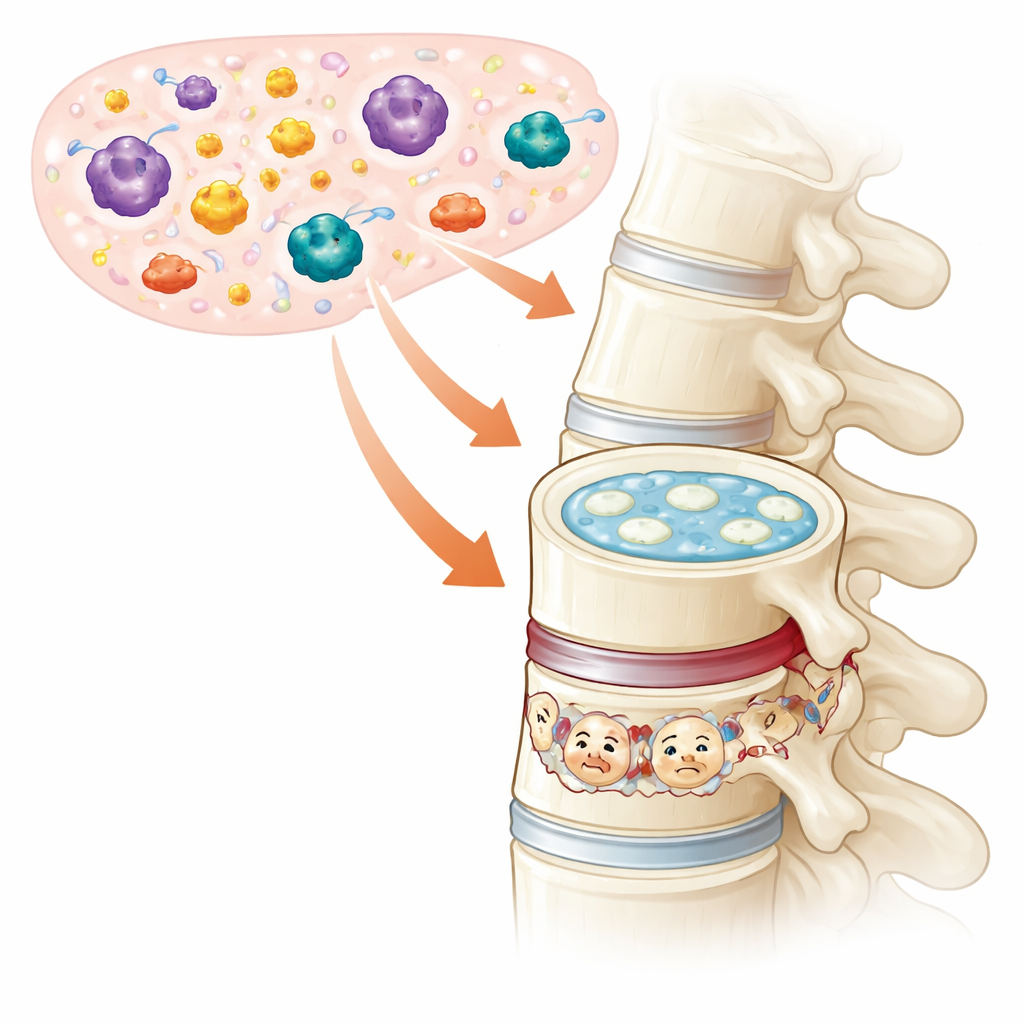
A Closer Look at the Spine’s Shock Absorbers
Intervertebral discs act as flexible pads between neighboring vertebrae, allowing us to bend, twist, and absorb the forces of daily life. At their core sits a gel-like center packed with specialized cells that maintain a springy mix of collagen and other matrix materials. When these cells falter, the disc dehydrates, thins, and may bulge or tear, a process known as intervertebral disc degeneration. People with advanced degeneration often live with chronic pain and limited movement, yet current therapies mainly focus on relieving symptoms rather than stopping or reversing the underlying damage.
Hunting for Trouble-Making Genes in Human Data
The researchers began by digging into existing genetic data from people with and without degenerated discs. They analyzed two large datasets of gene activity—essentially, which genes are turned up or down in diseased versus healthy tissue and blood. From thousands of genes that changed, they focused on 52 that shifted in the same direction across both datasets. Among these shared genes, one called CSF1 stood out. CSF1 is known to influence immune cells and tissue repair elsewhere in the body, so its strong signal in disc degeneration suggested it might be an important coordinator of inflammation and cell survival inside the spine.
How One Signal Can Fan the Flames Inside the Disc
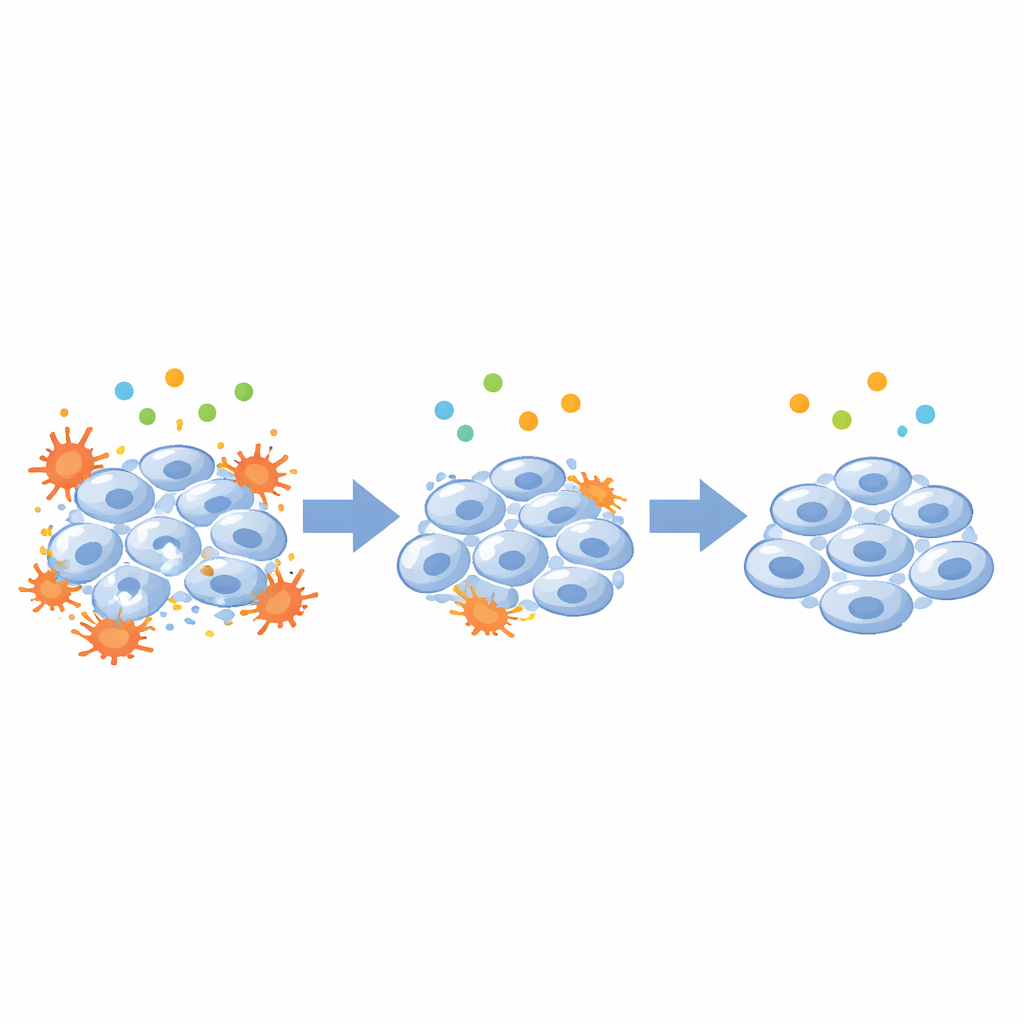
To test CSF1’s role more directly, the team turned to disc cells grown in the lab. They exposed nucleus pulposus cells—the key cells in the disc’s center—to an inflammatory trigger and watched CSF1 levels rise alongside classic inflammatory markers and increased cell death. Next they used genetic tools to dial CSF1 down inside these cells. When CSF1 was silenced, inflammatory proteins dropped, and the balance of cell death and survival shifted in a protective direction: proteins that promote survival increased, while those linked to self‑destruction decreased. In parallel, computer-based analyses of immune cell patterns suggested that higher CSF1 is tied to shifts in many types of immune cells, hinting that this one signal may help orchestrate a broader inflammatory environment in degenerating discs.
Clues from the Blood: A Possible Warning Signal
Because drawing samples directly from discs is invasive, a blood-based indicator would be far more practical in the clinic. The scientists therefore measured CSF1 levels in the blood of patients with varying degrees of disc degeneration and in healthy volunteers. They found that people with more severe degeneration had higher CSF1 levels in their blood, and that CSF1 tended to climb as disease severity increased. These findings raise the possibility that CSF1 could serve as a convenient biomarker—something a simple blood test might track to flag early disc damage or monitor how well treatments are working.
What This Means for Future Back Pain Care
Taken together, the results suggest that CSF1 is more than a bystander: it appears to help drive inflammation and cell loss in spinal discs while also reflecting disease severity in the bloodstream. For patients, this opens two promising avenues. First, CSF1 or its signaling partners might become targets for new drugs designed to calm harmful inflammation inside discs without resorting to major surgery. Second, blood tests based on CSF1 could one day help identify people at risk before irreversible damage sets in. More work, including animal studies and larger patient groups, will be needed to confirm these possibilities, but this study lays important groundwork for turning a molecular signal into better tools for diagnosing and treating low back pain.
Citation: Zhang, F., Wu, W., Yuan, Y. et al. CSF1 regulates inflammation and apoptosis in intervertebral disc degeneration. Sci Rep 16, 10566 (2026). https://doi.org/10.1038/s41598-026-44984-6
Keywords: intervertebral disc degeneration, low back pain, CSF1, spinal inflammation, biomarkers